Cyclothymic Disorder as an Overlooked Mood Condition
When most people think of mood disorders, two conditions typically come to mind: major depression and bipolar disorder.

Key Takeaways
- Increased energy and activity levels
- Elevated or irritable mood
- Decreased need for sleep without feeling tired
- Racing thoughts and rapid speech
- Increased confidence or grandiose ideas
Introduction
When most people think of mood disorders, two conditions typically come to mind: major depression and bipolar disorder. Yet there exists a third cyclical mood condition that remains largely unrecognized, even among mental health professionals. Cyclothymic disorder as an overlooked mood condition affects countless individuals who experience chronic emotional highs and lows without meeting the full criteria for manic or depressive episodes. These persistent mood fluctuations create real distress and functional impairment, yet the condition frequently goes undiagnosed or misunderstood. This article examines what cyclothymic disorder is, why it remains underrecognized in clinical practice, and how understanding this condition can help those experiencing unexplained emotional volatility find appropriate support.
Understanding Cyclothymic Disorder in the Context of Mood Disorders
The Diagnostic and Statistical Manual of Mental Disorders categorizes multiple distinct mood disorders, each with specific diagnostic criteria and patterns. Within this classification system, three conditions stand out as cyclical mood disorders characterized by predictable patterns of emotional fluctuation: Major Depressive Disorder, Bipolar Disorder, and Cyclothymic Disorder.
Major Depressive Disorder represents one of the most commonly recognized cyclical mood conditions, involving substantial unpredictable ups and downs in mood states. Bipolar Disorder features cyclical patterns with significant mood fluctuations between distinct poles of emotional experience. Cyclothymic disorder occupies a distinct position among these conditions, characterized by chronic emotional instability without the severity that defines full manic or major depressive episodes.
Clinical research suggests that cyclothymic disorder involves persistent mood fluctuations over extended periods, typically requiring symptoms to persist for at least two years in adults. The emotional highs associated with this condition resemble hypomanic states—elevated mood, increased energy, reduced need for sleep—but don't meet the full intensity or duration criteria for hypomania. Similarly, the low periods involve depressive symptoms such as low energy, sadness, and difficulty concentrating, without reaching the threshold for a major depressive episode.
This middle ground between normal mood variation and more severe mood disorders contributes to why cyclothymic disorder as an overlooked mood condition continues to be underdiagnosed in clinical settings.
Why Cyclothymic Disorder Remains Underrecognized
Several factors contribute to the lack of awareness surrounding this condition among both mental health professionals and the general public. Understanding these barriers helps explain why so many individuals with cyclothymic patterns struggle to receive accurate diagnosis and appropriate treatment.
Diagnostic overshadowing: When patients present with mood symptoms, clinicians often focus on the more familiar categories of unipolar depression or bipolar disorder. The chronic, less severe nature of cyclothymic fluctuations may not immediately suggest a distinct diagnostic category, leading to misdiagnosis or dismissal of symptoms as personality traits rather than a treatable condition.
Training gaps: Many mental health training programs emphasize the major mood disorders while spending less time on the less common presentations. This creates a knowledge gap where practitioners may be familiar with cyclothymic disorder in theory but don't readily recognize it in clinical practice.
Patient presentation: Individuals with cyclothymic disorder often don't seek help during hypomanic periods, when they may feel productive and positive. They're more likely to present during depressive phases, which can lead clinicians to focus on depressive symptoms without recognizing the broader pattern of mood cycling.
Symptom normalization: Because the mood swings are chronic and less extreme than those in bipolar disorder, many people with cyclothymic patterns assume their emotional variability is simply part of their personality. They may describe themselves as "moody" or "intense" without recognizing that their experience represents a diagnosable pattern.
Overlapping presentations: Cyclothymic disorder shares features with several other conditions, including borderline personality disorder, attention-deficit/hyperactivity disorder, and anxiety disorders. This overlap can complicate diagnosis, particularly when multiple conditions coexist.
The consequences of this underrecognition are significant. Without accurate diagnosis, individuals may receive treatments that don't address the cyclical nature of their symptoms, or they may go without support entirely, attributing their struggles to personal failings rather than a recognized mood condition.
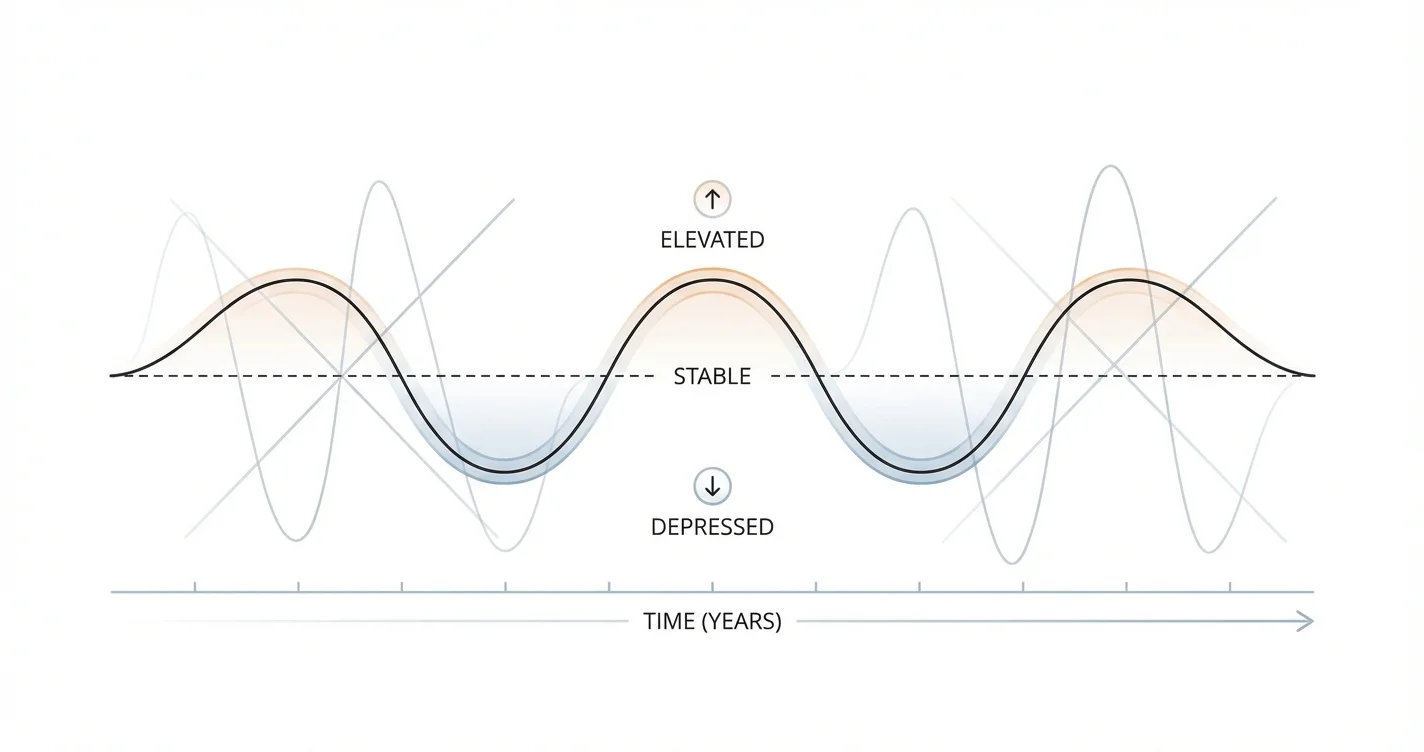
Recognizing the Pattern: What Cyclothymic Disorder Looks Like
Understanding the characteristic presentation of cyclothymic disorder helps distinguish it from normal mood variation and other mood conditions. The pattern involves numerous periods of hypomanic and depressive symptoms alternating over time, with relatively brief intervals of stable mood.
During hypomanic periods, individuals may experience:
- Increased energy and activity levels
- Elevated or irritable mood
- Decreased need for sleep without feeling tired
- Racing thoughts and rapid speech
- Increased confidence or grandiose ideas
- Impulsive decision-making or increased risk-taking
- Greater sociability and talkativeness
During depressive periods, symptoms may include:
- Low energy and fatigue
- Feelings of sadness, emptiness, or hopelessness
- Loss of interest in previously enjoyable activities
- Difficulty concentrating or making decisions
- Changes in appetite or sleep patterns
- Feelings of worthlessness or excessive guilt
- Social withdrawal
The key distinguishing feature is that these mood states don't meet the full criteria for major depressive or hypomanic episodes in terms of severity, number of symptoms, or duration. The fluctuations are more frequent and the symptoms less intense than in bipolar disorder, yet more persistent and disruptive than typical mood variation.
This chronic pattern creates significant challenges in daily functioning. Relationships may suffer due to unpredictable mood changes. Work performance can fluctuate with mood states. Planning for the future becomes difficult when emotional states feel unreliable. For those seeking support, tools like Lovon.app can provide on-demand emotional processing during both highs and lows, helping individuals identify patterns and develop coping strategies between professional appointments.
The Impact of Living with Unrecognized Cyclothymic Disorder
When cyclothymic disorder as an overlooked mood condition goes undiagnosed, the consequences extend beyond the mood symptoms themselves. The chronic nature of the condition means individuals spend years navigating emotional instability without understanding its source or having appropriate strategies to manage it.
Relationship challenges: Frequent mood changes can strain personal relationships. Partners, friends, and family members may struggle to understand the unpredictability, sometimes interpreting mood shifts as reactions to their behavior rather than manifestations of an underlying condition. The person with cyclothymic disorder may feel misunderstood or criticized for their emotional variability.
Career and academic difficulties: The fluctuating energy levels and mood states can create inconsistent performance patterns. During hypomanic periods, individuals may take on excessive commitments or make impulsive professional decisions. During depressive phases, following through becomes challenging, potentially leading to a pattern of incomplete projects and unrealized potential.
Self-perception issues: Without a diagnostic framework to understand their experience, many individuals internalize their struggles. They may view themselves as inherently unstable, unreliable, or flawed. This self-perception can contribute to shame and reluctance to seek help, creating a cycle that perpetuates the lack of recognition.
Risk of progression: Research suggests that cyclothymic disorder may increase the risk of eventually developing bipolar I or II disorder, particularly if left untreated. Some studies indicate that approximately 15-50% of individuals with cyclothymic disorder may later meet criteria for a bipolar diagnosis, though individual variation is significant and progression is not inevitable.
Comorbid conditions: The chronic stress of managing unexplained mood fluctuations may contribute to the development of additional conditions, including anxiety disorders, substance use issues, and sleep disorders. These comorbid presentations can further complicate diagnosis and treatment.
Understanding these impacts underscores the importance of improving recognition and diagnosis of this condition among mental health professionals and the general public.
Diagnosis and Treatment Approaches
Accurate diagnosis of cyclothymic disorder requires comprehensive assessment by a qualified mental health professional. The evaluation typically involves detailed history-taking to establish the pattern and duration of mood symptoms, ruling out other potential causes such as medical conditions or substance use, and differentiating cyclothymic disorder from other mood and personality conditions.
Mood tracking: Systematic monitoring of mood patterns over time provides valuable diagnostic information. Individuals may be asked to maintain daily mood logs noting energy levels, sleep duration, mood quality, and behaviors. This longitudinal perspective helps clinicians identify the cyclical pattern characteristic of the condition.
Treatment modalities: Several approaches may help manage cyclothymic symptoms:
-
Psychotherapy: Cognitive-behavioral therapy and interpersonal therapy can help individuals recognize mood patterns, develop coping strategies, and address relationship challenges. Dialectical behavior therapy techniques may help with emotional regulation.
-
Mood stabilization: In some cases, healthcare providers may discuss medication options that help reduce the amplitude of mood swings. The decision to use medication should be made collaboratively with a psychiatrist who specializes in mood disorders.
-
Lifestyle interventions: Maintaining regular sleep schedules, avoiding substances that affect mood, engaging in regular physical activity, and managing stress can all support mood stability. These interventions are often most effective when combined with professional treatment.
-
Relationship education: Helping partners and family members understand the condition can reduce relationship strain and improve support networks.
Ongoing support: Between professional appointments, accessible resources can provide valuable support. Platforms like Lovon.app offer on-demand opportunities to process emotional experiences, identify triggers, and work through relationship challenges that arise from mood fluctuations. This type of support complements professional treatment by providing immediate assistance during difficult moments.
However, it's important to note that self-help strategies and digital tools are supplements to, not replacements for, professional mental health care. Cyclothymic disorder is a recognized clinical condition that responds best to coordinated treatment approaches.
When to Seek Professional Help
If you recognize patterns of cyclothymic disorder in your own experience, several signs indicate that professional evaluation would be beneficial:
- Mood fluctuations are affecting your relationships, work performance, or daily functioning
- You've noticed a pattern of emotional highs and lows lasting for months or years
- Family members or friends have expressed concern about your mood changes
- You're struggling to maintain consistency in important areas of your life
- Previous treatments for depression or anxiety haven't adequately addressed your symptoms
- You're experiencing impulsive behaviors during high-mood periods that create negative consequences
Mental health professionals who can provide appropriate evaluation and treatment include psychiatrists, psychologists, and licensed therapists with experience in mood disorders. When seeking care, specifically mentioning your observation of cyclical mood patterns can help guide the assessment process.
For those already in treatment for other conditions, raising the possibility of cyclothymic disorder with your current provider can prompt a reevaluation of your diagnosis and treatment plan. Many individuals discover this diagnosis after years of treatment for other conditions, finally finding an explanation that fits their experience.
Conclusion
Cyclothymic disorder as an overlooked mood condition represents a significant gap in mental health awareness and practice. This chronic pattern of emotional highs and lows affects numerous individuals who often go years without accurate diagnosis or appropriate support. The condition occupies a distinct position among cyclical mood disorders—less severe than bipolar disorder but more persistent and disruptive than normal mood variation.
Improving recognition of cyclothymic disorder requires both professional education and public awareness. Mental health practitioners benefit from heightened attention to cyclical patterns that don't meet full criteria for bipolar disorder. Individuals experiencing unexplained emotional volatility benefit from knowing that their experience has a name, represents a recognized condition, and responds to treatment approaches.
If you recognize these patterns in your own experience, seeking comprehensive evaluation from a qualified mental health professional represents an important step toward understanding and managing your symptoms. With appropriate diagnosis and treatment, individuals with cyclothymic disorder can develop effective strategies for managing mood fluctuations, improving relationships, and achieving greater stability in their daily lives.
Disclaimer: This is general information, not medical advice or diagnosis. If symptoms are severe, affecting your daily life, or you're having thoughts of self-harm — seek professional help. In the US: call or text 988 (Suicide & Crisis Lifeline). For immediate danger: 911 or local emergency services.
How AI Support Helps You Heal
AI emotional support isn't about replacing human connection — it's about filling the gaps. The moments when you need to talk at 2 AM, when you don't want to burden your friends again, or when you simply need someone to listen without judgment.
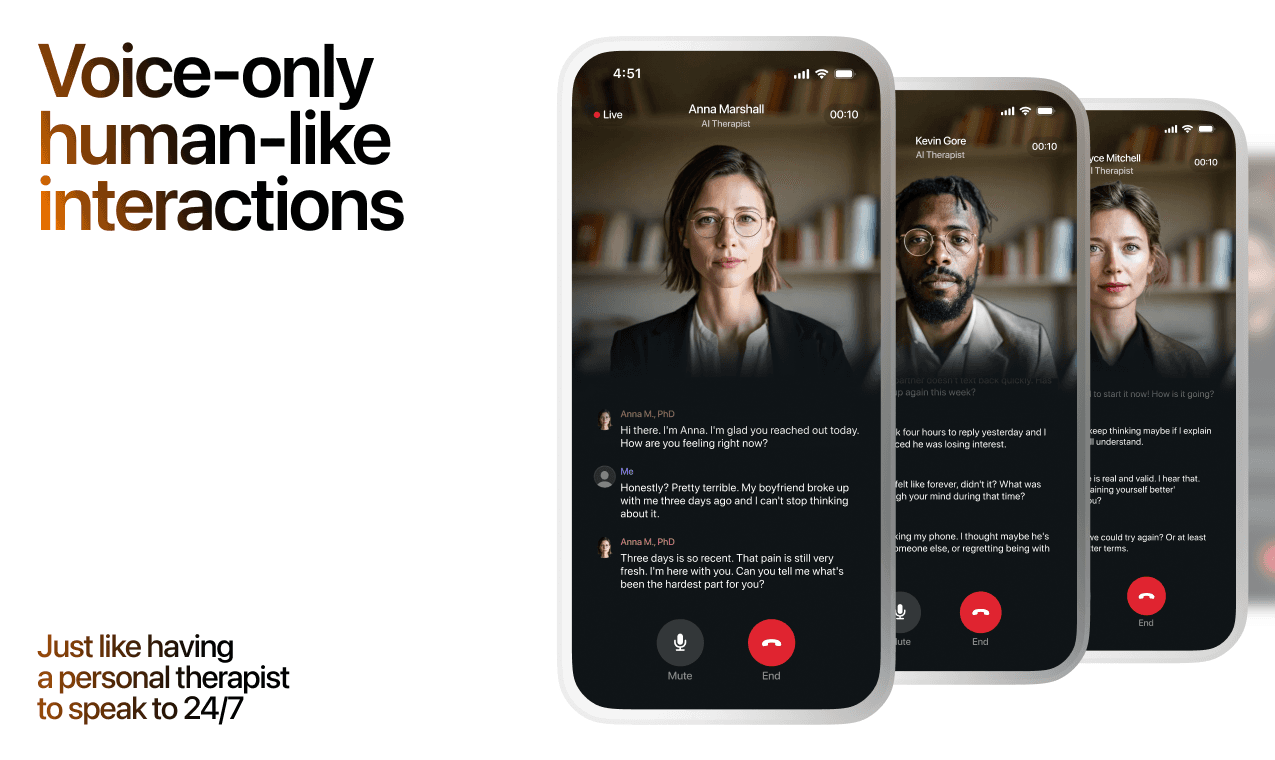
Here's what happens in a typical Lovon session:
You share what's on your mind
There's no script, no intake form, no waiting room. You speak or type whatever you're feeling — in your own words, at your own pace.
Lovon validates and explores
Using frameworks from CBT (Cognitive Behavioral Therapy) and motivational interviewing, Lovon acknowledges your feelings first, then gently helps you explore them. No dismissive "just move on" advice.
You build coping skills together
Lovon doesn't just listen — it actively works with you on evidence-based techniques: thought reframing, urge surfing, behavioral experiments, and more.
What a Session with Lovon Looks Like
When to Seek Professional Help
AI support is a valuable tool, but it's not a replacement for professional care. Please consider reaching out to a licensed therapist if you experience any of the following:
- Persistent thoughts of self-harm or suicide
- Inability to perform daily activities (work, eating, sleeping) for more than 2 weeks
- Turning to alcohol or substances to cope
- Intense anger or desire to harm your ex-partner
- Complete emotional numbness that doesn't improve over time
Crisis Resources (US): If you're in immediate danger, call 988 (Suicide & Crisis Lifeline) or text HOME to 741741 (Crisis Text Line). Available 24/7, free, and confidential.
Outside the US? Find a crisis line in your country
Ready to Start?
Your healing journey can begin right now
1 free conversation. No credit card. No judgment. Just a safe space to process what you're going through.
Frequently Asked Questions
Is AI therapy a replacement for a real therapist?
Is my conversation with Lovon AI private?
How is Lovon different from ChatGPT for emotional support?
Can I use Lovon if I'm already seeing a therapist?
Can I try Lovon for free?
About the Author
The Lovon Editorial Team
Mental Health & Wellness Content Team
The Lovon Editorial Team develops mental health and wellness content designed to make psychological concepts accessible and actionable. Our goal is to bridge the gap between clinical research and everyday life - helping you understand why your mind works the way it does and what you can do about it....
Similar Articles
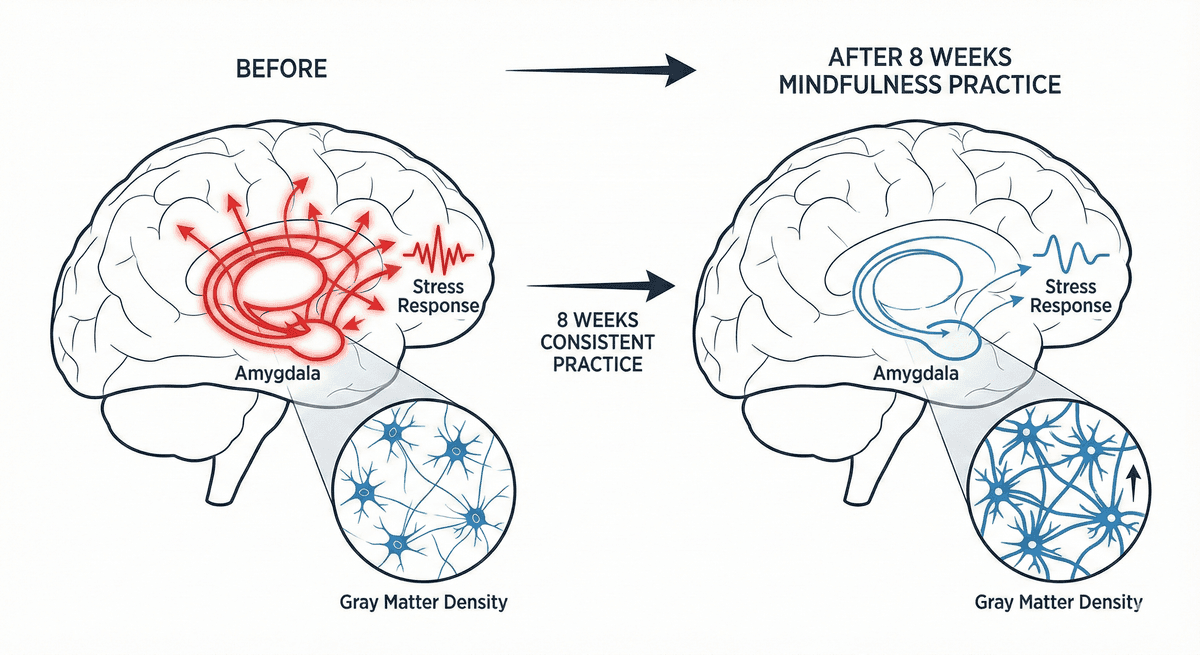
Amygdala Reactivity Reduction: Gray Matter Changes After Eight Weeks of Mindfulness Practice
Discover how eight weeks of mindfulness practice reshapes the brain, reducing amygdala reactivity and building lasting neural resilience.
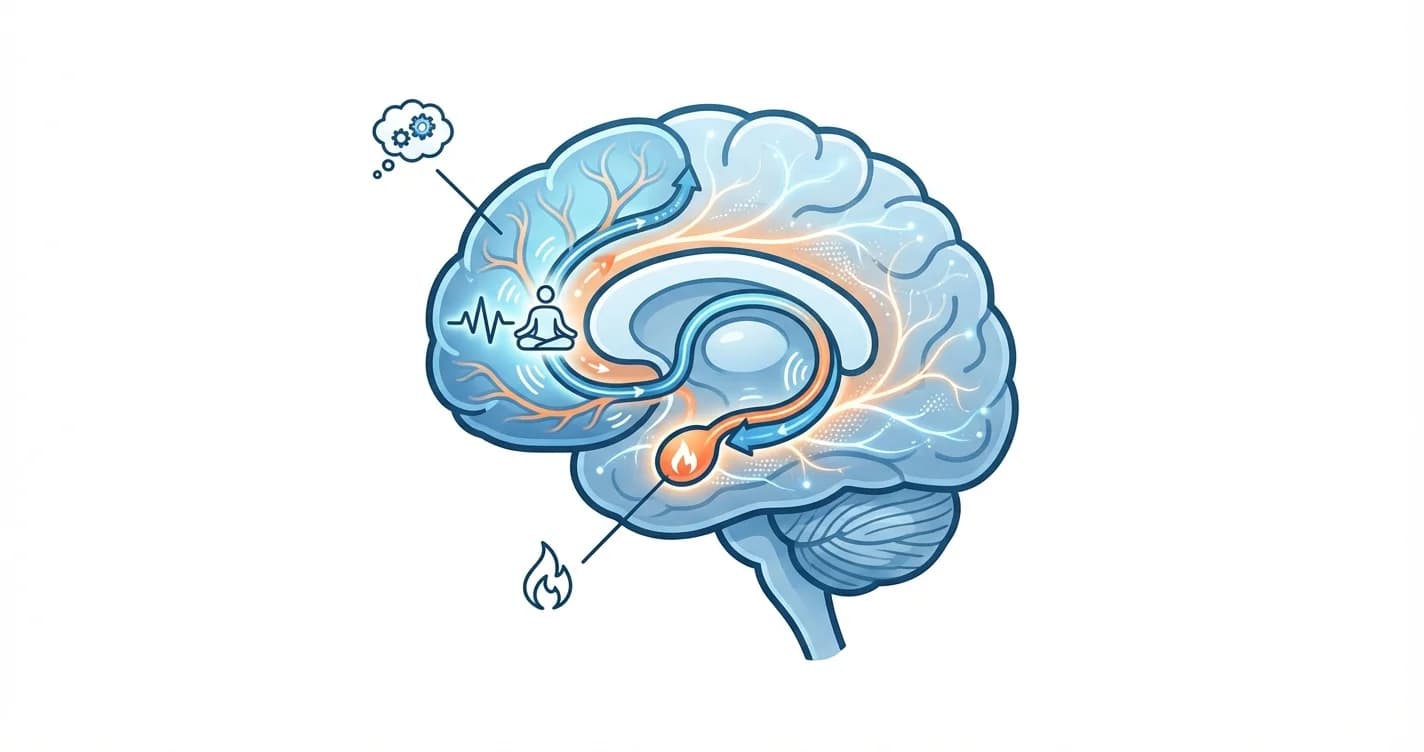
Amygdala and Prefrontal Cortex Connection: Training Emotional Regulation Through Mindfulness
How mindfulness practices reshape neural pathways to strengthen emotional control and reduce reactivity
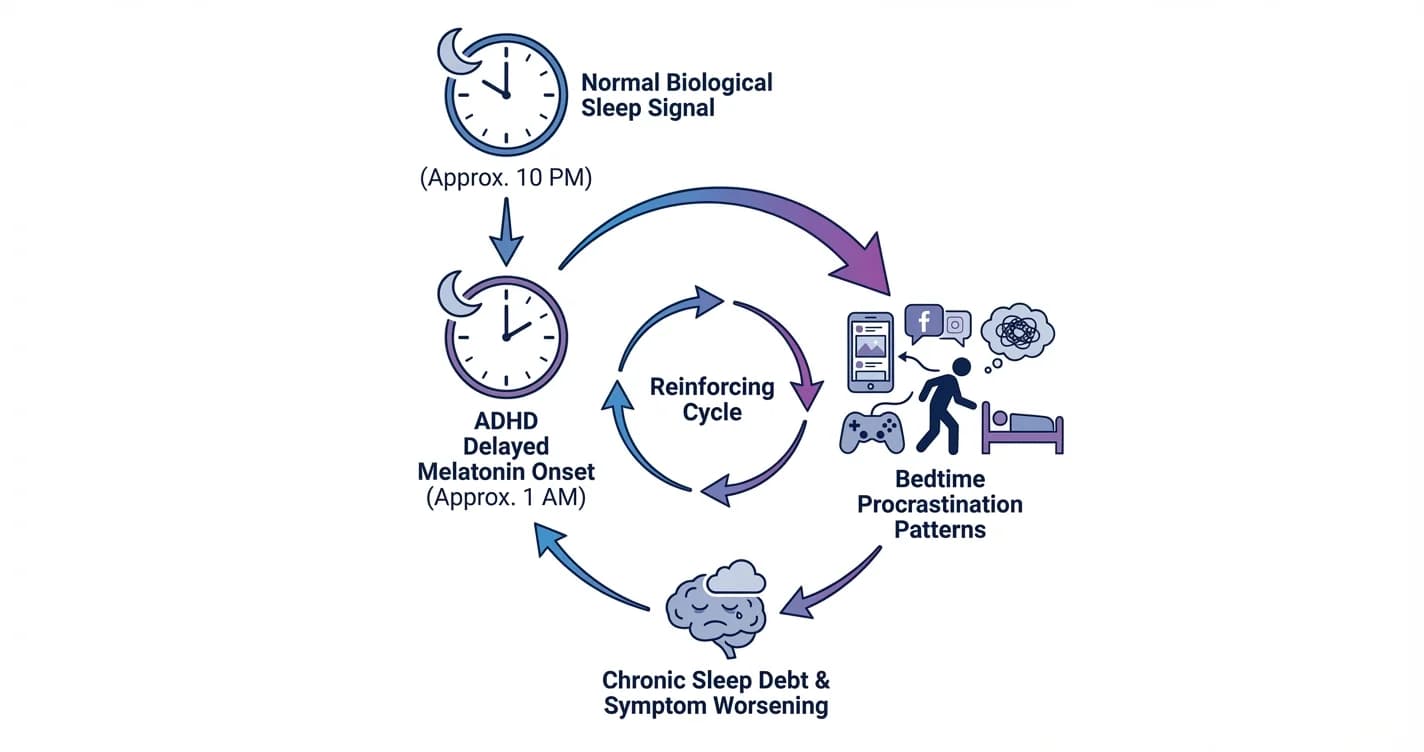
ADHD Sleep Cycle Disruption: Melatonin Delay and Bedtime Procrastination Patterns
Understanding how attention regulation difficulties interfere with natural sleep timing and the nightly wind-down process
Disclaimer: This article is for informational purposes only and does not constitute medical advice, diagnosis, or treatment. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition. If you are in crisis or think you may have an emergency, call 988 (Suicide & Crisis Lifeline) or go to the nearest emergency room. Outside the US? Find a crisis line in your country.