Major Depressive Disorder vs Persistent Depressive Disorder
When struggling with prolonged sadness or emotional difficulty, understanding what you're experiencing can feel overwhelming.

Key Takeaways
- Persistent sad, empty, or hopeless mood most of the day, nearly every day
- Markedly diminished interest or pleasure in activities once enjoyed
- Significant changes in appetite or weight
- Sleep disturbances (insomnia or excessive sleeping)
- Psychomotor agitation or retardation observable by others
Introduction
When struggling with prolonged sadness or emotional difficulty, understanding what you're experiencing can feel overwhelming. Major Depressive Disorder vs Persistent Depressive Disorder represents one of the most clinically significant distinctions in mood disorders, yet many people—and even some mental health professionals—conflate these two conditions. While both involve depressive symptoms, they differ fundamentally in their duration, intensity, and the pattern of mood fluctuations they produce. According to the Diagnostic and Statistical Manual of Mental Disorders (DSM), these represent two distinct categories within the broader spectrum of mood disorders, each requiring different recognition and treatment approaches. This article examines the core differences between these conditions based on current diagnostic criteria and clinical insights, helping you understand which pattern may align with your experiences.
Understanding Major Depressive Disorder
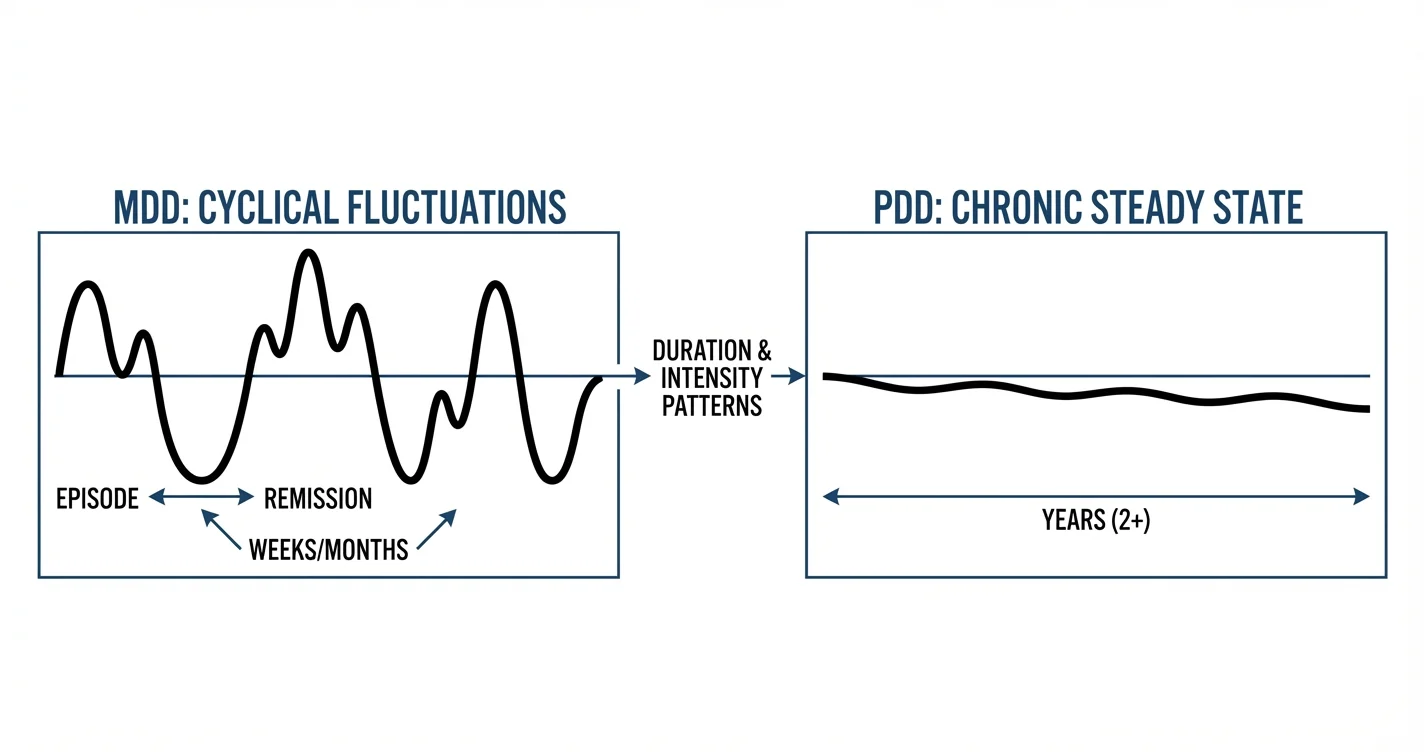
Major Depressive Disorder (MDD) is characterized by its cyclical nature, featuring substantial and often unpredictable mood fluctuations. Unlike the steady low mood of other depressive conditions, MDD involves episodes—periods of intense depressive symptoms that emerge, persist for weeks or months, and eventually remit, either with treatment or sometimes spontaneously.
During a major depressive episode, individuals typically experience a combination of symptoms that significantly impair daily functioning:
- Persistent sad, empty, or hopeless mood most of the day, nearly every day
- Markedly diminished interest or pleasure in activities once enjoyed
- Significant changes in appetite or weight
- Sleep disturbances (insomnia or excessive sleeping)
- Psychomotor agitation or retardation observable by others
- Fatigue or loss of energy
- Feelings of worthlessness or excessive guilt
- Difficulty concentrating or making decisions
- Recurrent thoughts of death or suicidal ideation
What distinguishes MDD as a cyclical mood disorder is that these episodes have a clear beginning and end. Between episodes, individuals may return to their baseline functioning, experiencing periods of relatively normal mood. The unpredictability of when episodes will occur and how long they'll last creates particular challenges for those managing this condition. Research indicates that without treatment, major depressive episodes typically last several months, though duration varies considerably between individuals.
Defining Persistent Depressive Disorder
Persistent Depressive Disorder (PDD), previously known as dysthymia, presents a markedly different pattern. Rather than discrete episodes with clear beginnings and ends, PDD involves a chronic, fairly constant state of low mood with minimal fluctuations. Mental health professionals describe this as a steady baseline of sadness that persists for extended periods—at least two years in adults.
The experience of PDD differs from Major Depressive Disorder vs Persistent Depressive Disorder primarily in its consistency and duration rather than acute severity. Individuals with PDD describe feeling as though they've "always been this way" or that sadness has become their default emotional state. The symptoms may be somewhat less intense than those experienced during a major depressive episode, but their relentless presence creates cumulative impairment over time.
Clinical characteristics of Persistent Depressive Disorder include:
- Depressed mood most of the day, more days than not, for at least two years
- Presence of two or more additional symptoms: poor appetite or overeating, insomnia or hypersomnia, low energy, low self-esteem, poor concentration or difficulty making decisions, feelings of hopelessness
- Symptoms cause significant distress or functional impairment
- The person has not been without symptoms for more than two months at a time during the two-year period
The chronic nature of PDD often leads individuals to normalize their experience, viewing depression as part of their personality rather than a treatable condition. This presents unique challenges for recognition and treatment initiation, as the gradual onset and persistent nature may not trigger the same urgency as the more dramatic episodes characteristic of MDD.
Major Depressive Disorder vs Persistent Depressive Disorder: Core Distinctions
The fundamental difference between these conditions lies in their temporal patterns and mood trajectories. Major Depressive Disorder operates in cycles—periods of severe depression alternating with periods of remission or normal mood. Persistent Depressive Disorder maintains a steady, chronic low mood without the dramatic shifts seen in MDD.
Duration and Onset
MDD episodes have defined durations, typically lasting weeks to months if untreated. The onset can be relatively sudden, with individuals able to identify when their mood significantly changed. PDD requires at least two years of persistent symptoms in adults (one year in children and adolescents), with symptoms present more days than not throughout this period.
Intensity and Fluctuation
During acute episodes, MDD often produces more severe symptoms that profoundly disrupt functioning—individuals may be unable to work, maintain relationships, or perform basic self-care. PDD symptoms may be less acutely severe but their constant presence creates sustained impairment. As clinical experts note, PDD involves minimal mood fluctuations, maintaining a fairly constant sadness, whereas MDD involves substantial unpredictable ups and downs.
Functional Impact
Both conditions significantly affect quality of life, but differently. MDD's episodic nature may allow for periods of recovery and normal functioning between episodes, though repeated episodes can lead to progressive impairment. PDD's chronic nature means individuals rarely experience relief, leading to long-term effects on self-concept, relationships, and life trajectory. Many people with PDD struggle to remember what "normal" mood feels like.
Comorbidity Patterns
It's important to recognize that these conditions can coexist. When someone with Persistent Depressive Disorder experiences a major depressive episode superimposed on their chronic low mood, this is sometimes referred to as "double depression." This pattern underscores that Major Depressive Disorder vs Persistent Depressive Disorder represents a spectrum rather than completely separate conditions.
Therapeutic Approaches for MDD vs PDD
While both conditions respond to similar treatment modalities, the approach and focus differ based on the specific pattern present. Understanding whether you're experiencing MDD or PDD helps clinicians tailor interventions to your particular needs.
Psychotherapy Considerations
For Major Depressive Disorder, therapy often focuses on managing acute episodes, identifying triggers, developing crisis plans, and preventing relapse. Cognitive-behavioral therapy (CBT) has substantial research support for treating MDD, helping individuals recognize and modify thought patterns that contribute to depressive episodes. Interpersonal therapy (IPT) addresses relationship patterns and role transitions that may precipitate episodes.
For Persistent Depressive Disorder, therapeutic work typically addresses the chronic, entrenched nature of symptoms. This may involve longer-term therapy to modify deeply held beliefs about self and world, gradually building experiences that challenge the persistent negative mood state. Some therapists use approaches specifically designed for chronic depression, acknowledging that the steady nature of PDD requires different strategies than episodic MDD.
Tools like Lovon.app can provide on-demand support for processing emotional patterns and preparing for therapeutic work, particularly useful when working through the day-to-day challenges that both conditions present. However, these resources complement rather than replace professional treatment.
Medication Approaches
Research suggests that both MDD and PDD may respond to similar medication classes, though response rates and optimal treatment duration can differ. For MDD, medications may be used during acute episodes and continued to prevent recurrence. For PDD, given the chronic nature, longer-term medication management is often recommended.
When considering MDD vs PDD therapy, the consistent, chronic nature of PDD sometimes requires extended treatment trials to observe benefit, whereas MDD episodes may show more rapid response. Always work with a prescriber who can evaluate your specific situation, monitor response, and adjust treatment as needed.
Lifestyle and Self-Management
Both conditions benefit from lifestyle interventions, though their implementation differs. For MDD, establishing routines that provide early warning of emerging episodes and intensifying self-care during high-risk periods can help. For PDD, the challenge lies in maintaining consistent engagement with beneficial activities despite chronic low motivation. Strategies that may help include:
- Structured daily routines that don't rely on motivation or mood
- Regular physical activity, which research associates with improvements in depressive symptoms
- Social connection, even when it feels difficult
- Sleep hygiene practices
- Mindfulness or acceptance-based approaches that address the relationship with persistent low mood
Recognizing Which Pattern You're Experiencing
Distinguishing between Major Depressive Disorder vs Persistent Depressive Disorder in your own experience requires reflection on the timeline and pattern of your symptoms. Consider these questions:
Timeline Assessment: Can you identify specific periods when your depression was significantly worse, with beginnings and ends to these episodes? Or has your low mood been fairly constant for years, without clear periods of normal mood?
Intensity Variation: Do you experience dramatic shifts in your depression severity, or does it maintain a relatively consistent (though unpleasant) level?
Baseline Mood: Can you remember extended periods (several months or more) in recent years when you felt "normal" or like yourself? Or has depression become what feels like your default state?
Functional Patterns: Have there been times when depression completely prevented you from functioning, followed by recovery periods? Or do you manage to continue functioning despite constant low mood, perhaps leading others to underestimate your struggle?
These reflections can inform conversations with mental health professionals, though formal diagnosis requires clinical evaluation. The DSM criteria that clinicians use involve specific symptom counts, duration thresholds, and assessments of functional impairment that require professional judgment.
It's worth noting that mood disorders exist within a broader classification system that includes several other conditions. The DSM contains six different mood disorder categories (or seven if counting Bipolar 1 and 2 separately), including less commonly discussed conditions like Cyclothymic Disorder—which involves chronic emotional highs and lows without full manic or depressive episodes. Comprehensive evaluation ensures that your treatment addresses the specific pattern you're experiencing rather than assuming all persistent sadness fits the same category.
When to Seek Professional Help
If you recognize patterns consistent with either Major Depressive Disorder or Persistent Depressive Disorder, professional evaluation is important. Specific indicators that professional help is needed include:
- Depressive symptoms persisting for two weeks or longer
- Significant difficulty fulfilling work, school, or family responsibilities
- Withdrawal from relationships and activities
- Changes in sleep, appetite, or energy that affect daily functioning
- Difficulty concentrating or making decisions
- Thoughts of death, dying, or self-harm
- Use of alcohol or substances to manage mood
- Feelings that life isn't worth living
Mental health professionals who can help include licensed therapists, psychologists, psychiatrists, and counselors specializing in mood disorders. Many people benefit from a combination of therapy and medication management, which may involve seeing both a therapist and a prescriber.
For those seeking immediate support or help between professional appointments, resources like Lovon.app provide accessible options for processing emotions and working through difficult moments. These tools can help you articulate your experiences and prepare for conversations with treatment providers.
Conclusion
Understanding Major Depressive Disorder vs Persistent Depressive Disorder provides crucial insight into the specific pattern of depression you may be experiencing. While both conditions involve depressive symptoms and significantly affect quality of life, they differ fundamentally in their temporal patterns—MDD involves cyclical episodes with substantial mood fluctuations, while PDD presents as chronic, fairly constant low mood with minimal variation. Recognizing these distinctions helps ensure you receive treatment approaches tailored to your specific needs rather than a one-size-fits-all intervention. Whether you're experiencing the dramatic ups and downs of Major Depressive Disorder or the steady low mood of Persistent Depressive Disorder, effective treatments exist and recovery is possible. The first step involves acknowledging your experience, seeking proper evaluation, and engaging with treatment approaches that address your particular pattern of symptoms. If you're struggling with persistent sadness or depressive episodes, reach out to a mental health professional who can provide comprehensive assessment and evidence-based treatment.
Disclaimer: This is general information, not medical advice or diagnosis. If symptoms are severe, affecting your daily life, or you're having thoughts of self-harm—seek professional help. In the US: call or text 988 (Suicide & Crisis Lifeline). For immediate danger: 911 or local emergency services.
How AI Support Helps You Heal
AI emotional support isn't about replacing human connection — it's about filling the gaps. The moments when you need to talk at 2 AM, when you don't want to burden your friends again, or when you simply need someone to listen without judgment.
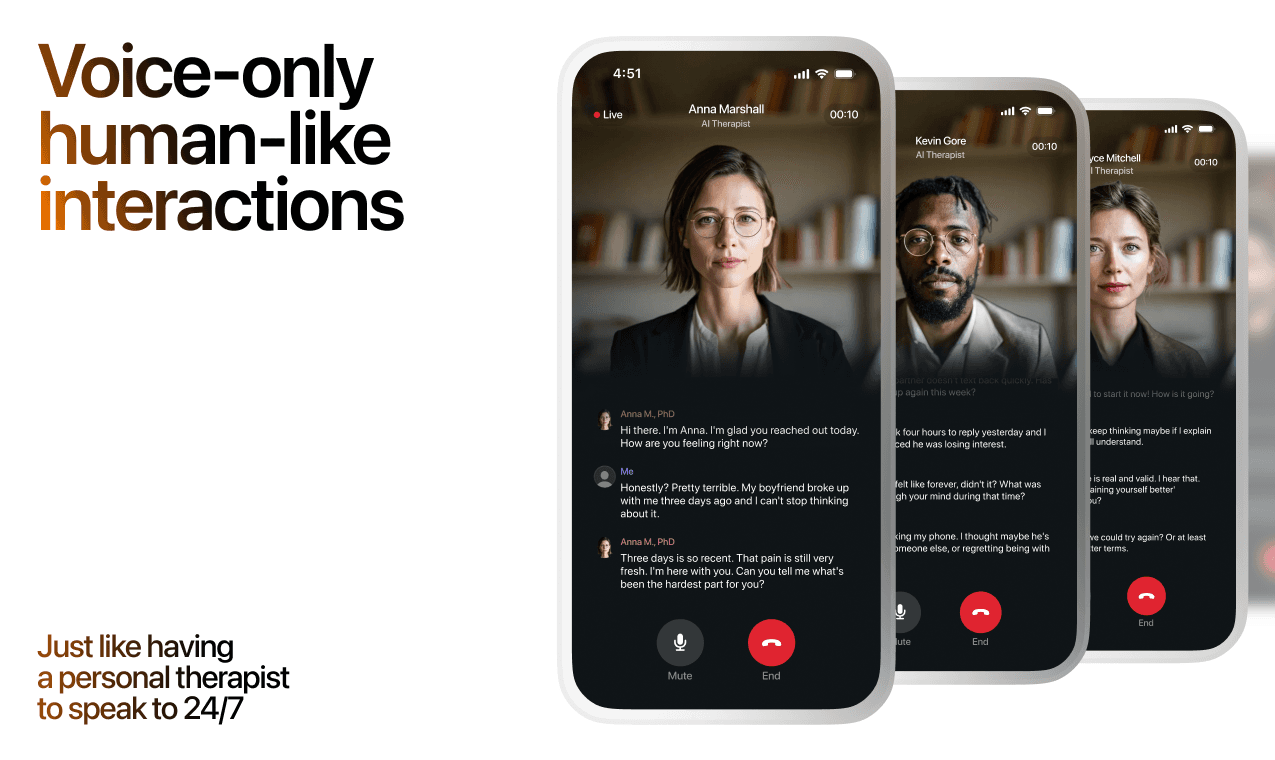
Here's what happens in a typical Lovon session:
You share what's on your mind
There's no script, no intake form, no waiting room. You speak or type whatever you're feeling — in your own words, at your own pace.
Lovon validates and explores
Using frameworks from CBT (Cognitive Behavioral Therapy) and motivational interviewing, Lovon acknowledges your feelings first, then gently helps you explore them. No dismissive "just move on" advice.
You build coping skills together
Lovon doesn't just listen — it actively works with you on evidence-based techniques: thought reframing, urge surfing, behavioral experiments, and more.
What a Session with Lovon Looks Like
When to Seek Professional Help
AI support is a valuable tool, but it's not a replacement for professional care. Please consider reaching out to a licensed therapist if you experience any of the following:
- Persistent thoughts of self-harm or suicide
- Inability to perform daily activities (work, eating, sleeping) for more than 2 weeks
- Turning to alcohol or substances to cope
- Intense anger or desire to harm your ex-partner
- Complete emotional numbness that doesn't improve over time
Crisis Resources (US): If you're in immediate danger, call 988 (Suicide & Crisis Lifeline) or text HOME to 741741 (Crisis Text Line). Available 24/7, free, and confidential.
Outside the US? Find a crisis line in your country
Ready to Start?
Your healing journey can begin right now
1 free conversation. No credit card. No judgment. Just a safe space to process what you're going through.
Frequently Asked Questions
Is AI therapy a replacement for a real therapist?
Is my conversation with Lovon AI private?
How is Lovon different from ChatGPT for emotional support?
Can I use Lovon if I'm already seeing a therapist?
Can I try Lovon for free?
About the Author
The Lovon Editorial Team
Mental Health & Wellness Content Team
The Lovon Editorial Team develops mental health and wellness content designed to make psychological concepts accessible and actionable. Our goal is to bridge the gap between clinical research and everyday life - helping you understand why your mind works the way it does and what you can do about it....
Similar Articles
Amygdala and Prefrontal Cortex Connection: Training Emotional Regulation Through Mindfulness
How mindfulness practices reshape neural pathways to strengthen emotional control and reduce reactivity
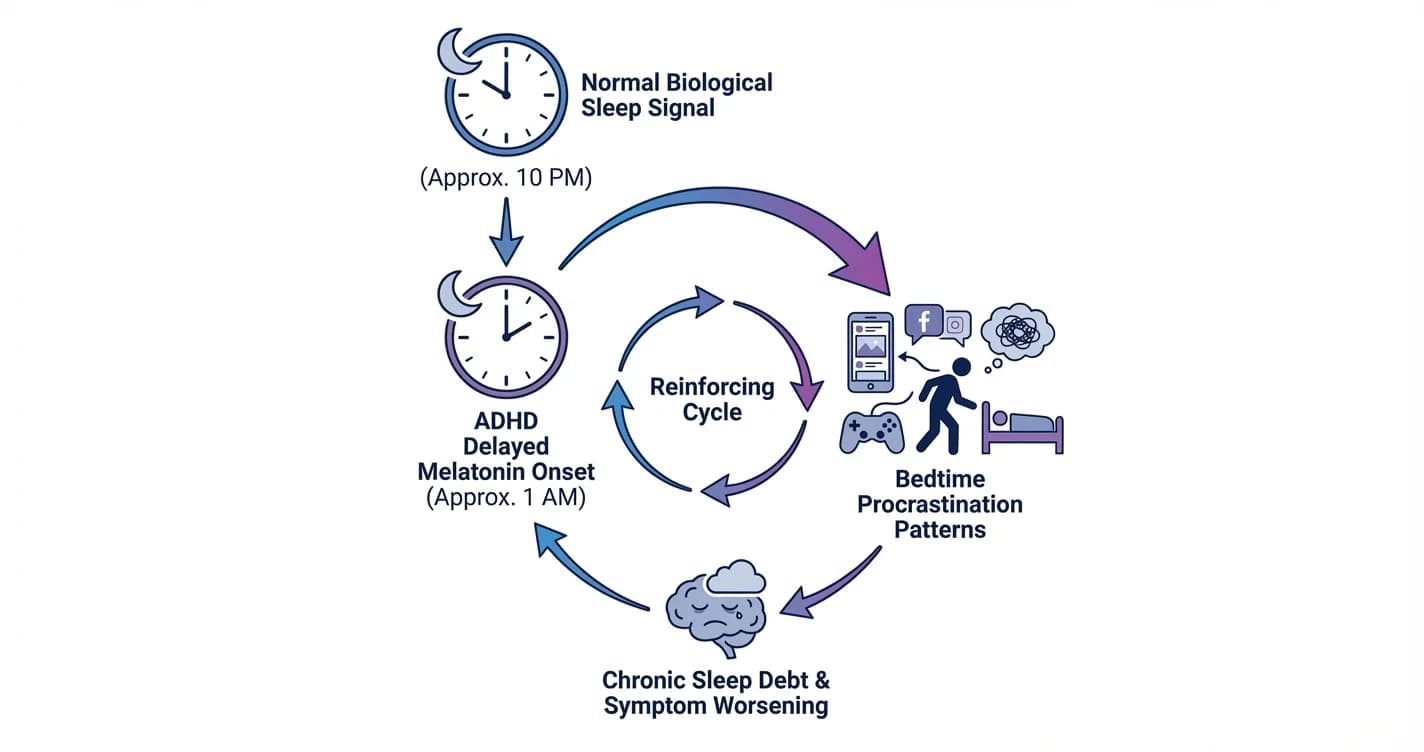
ADHD Sleep Cycle Disruption: Melatonin Delay and Bedtime Procrastination Patterns
Understanding how attention regulation difficulties interfere with natural sleep timing and the nightly wind-down process
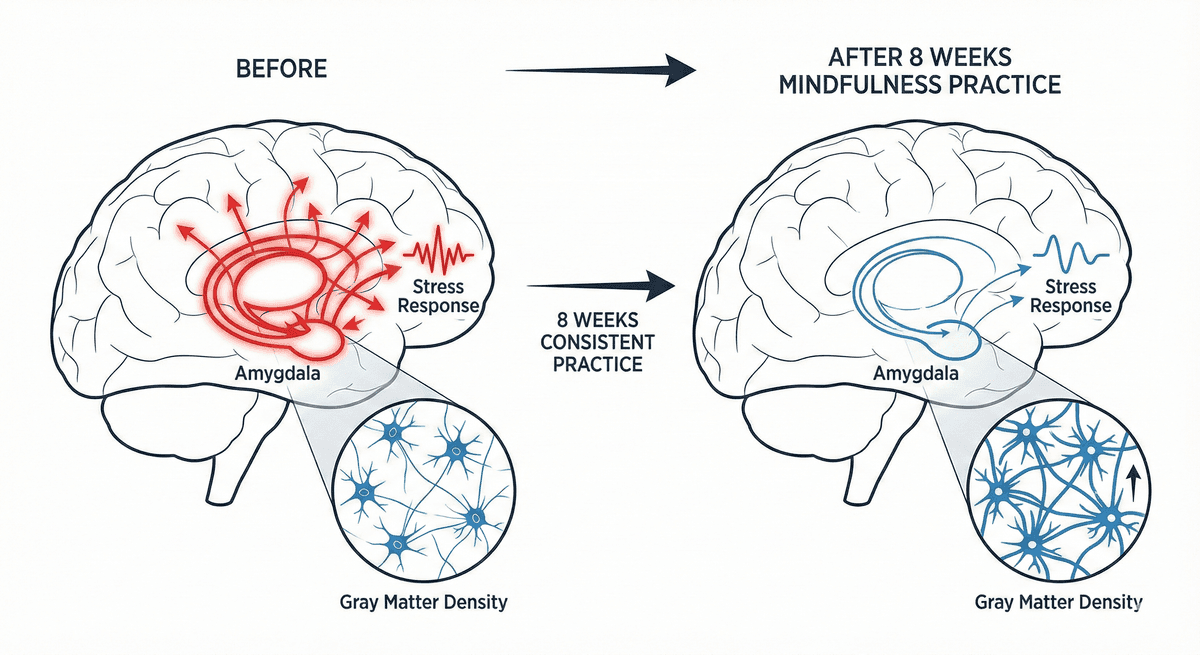
Amygdala Reactivity Reduction: Gray Matter Changes After Eight Weeks of Mindfulness Practice
Discover how eight weeks of mindfulness practice reshapes the brain, reducing amygdala reactivity and building lasting neural resilience.
Disclaimer: This article is for informational purposes only and does not constitute medical advice, diagnosis, or treatment. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition. If you are in crisis or think you may have an emergency, call 988 (Suicide & Crisis Lifeline) or go to the nearest emergency room. Outside the US? Find a crisis line in your country.