Acceptance and Commitment Therapy for Trauma Responses
Trauma responses don't always look like flashbacks or nightmares. Sometimes they appear as persistent avoidance, emotional numbness, hypervigilance, or...

Key Takeaways
- Trauma responses don't always look like flashbacks or nightmares
- Sometimes they appear as persistent avoidance, emotional numbness, hypervigilance, or rigid patterns that keep you
- Acceptance and Commitment Therapy for trauma responses offers a distinctive approach: rather than focusing primarily
Introduction
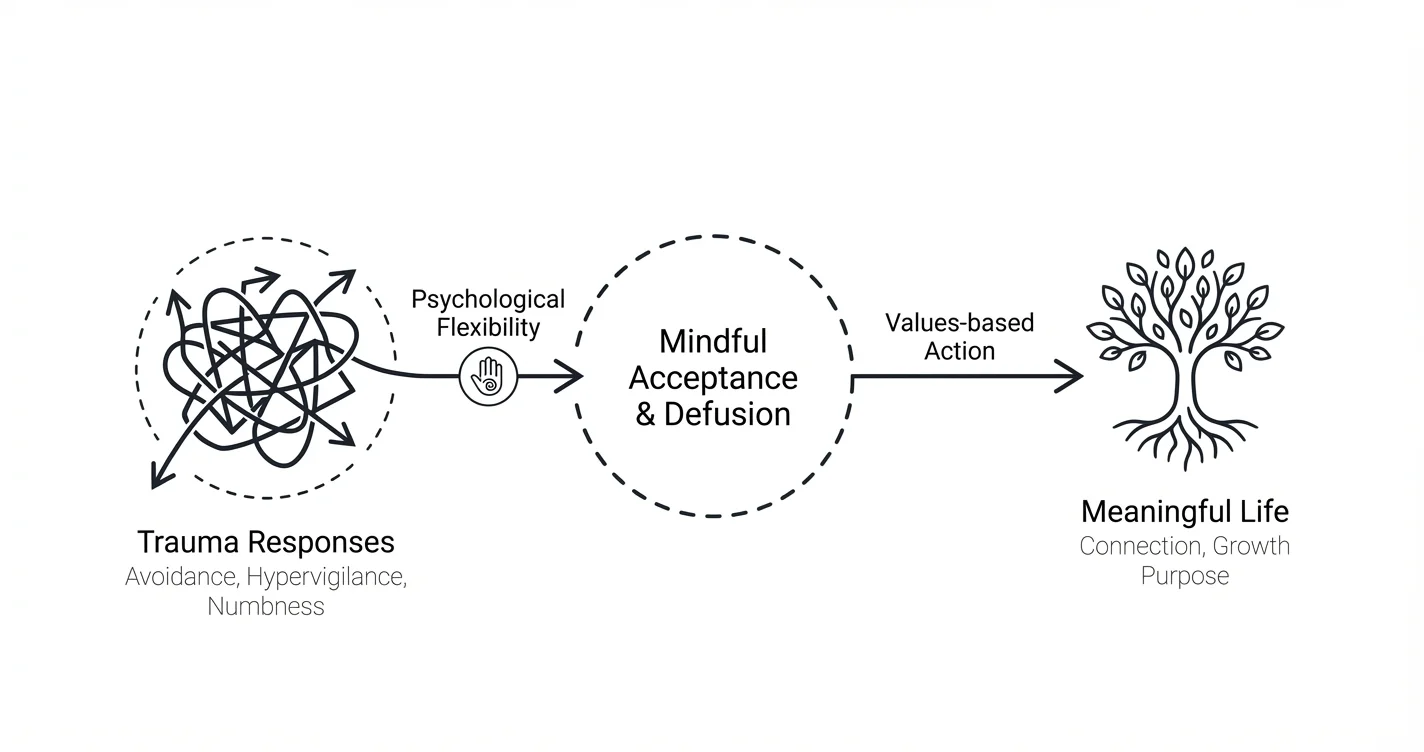
Trauma responses don't always look like flashbacks or nightmares. Sometimes they appear as persistent avoidance, emotional numbness, hypervigilance, or rigid patterns that keep you stuck in survival mode long after the threat has passed. Acceptance and Commitment Therapy for trauma responses offers a distinctive approach: rather than focusing primarily on reducing symptoms or revisiting traumatic memories, ACT teaches you to change your relationship with difficult internal experiences while moving toward what matters most in your life.
This evidence-based therapeutic framework combines mindfulness strategies, acceptance practices, and values-based action to help people develop psychological flexibility—the ability to stay present with uncomfortable emotions and thoughts while still taking meaningful action. For those dealing with trauma responses, this approach addresses a core challenge: the ways we try to control or avoid painful internal experiences often create more suffering and keep us disconnected from meaningful life.
Understanding Trauma Responses Through an ACT Lens
Trauma responses represent your nervous system's attempt to protect you from perceived threats. These can include fight, flight, freeze, or fawn responses that once served a protective function but now activate in situations that aren't actually dangerous. Research indicates that trauma fundamentally changes how the brain processes threat and safety signals, leading to persistent patterns of hyperarousal, avoidance, and disconnection.
Acceptance and Commitment Therapy for trauma responses reframes these patterns not as pathology to eliminate, but as understandable protective strategies that have become unhelpful. The ACT model identifies experiential avoidance—the attempt to control or escape uncomfortable thoughts, feelings, memories, and bodily sensations—as a central process that maintains suffering. When trauma survivors try to suppress intrusive memories, numb difficult emotions, or avoid reminders of their experiences, these efforts often backfire, intensifying distress and narrowing their lives.
ACT practitioners recognize that recovery involves a fundamental shift in how you relate to your internal experiences. Rather than asking "How do I make these trauma responses go away?" ACT asks "How can I make space for these difficult experiences while still doing what matters to me?" This distinction matters because many trauma responses resist direct control—trying harder to not think about something often makes it more intrusive, and attempting to force yourself to feel calm can paradoxically increase anxiety.
The Six Core Processes of ACT for Trauma Work
Acceptance and Commitment Therapy for trauma responses operates through six interconnected processes that build psychological flexibility. Each addresses specific ways trauma impacts your relationship with your internal world and your capacity for meaningful action.
Acceptance involves making space for difficult thoughts, emotions, memories, and sensations rather than fighting them. For trauma survivors, this doesn't mean liking or wanting these experiences—it means reducing the struggle against what's already present. When you notice a trauma response activating, acceptance practices help you observe the sensations, thoughts, and impulses without immediately reacting or trying to make them disappear.
Cognitive defusion creates distance from unhelpful thought patterns. Trauma often generates thoughts like "I'm broken," "It's not safe to trust anyone," or "Something terrible will happen." Rather than challenging whether these thoughts are true or false, defusion techniques help you see thoughts as mental events—words and images your mind produces—rather than literal truths that must control your behavior. You might notice "I'm having the thought that I'm broken" instead of fusing with "I am broken."
Present moment awareness addresses the way trauma pulls attention into the past (ruminating about what happened) or future (worrying about what might happen). Mindfulness practices strengthen your ability to anchor in the present, noticing what's actually happening right now rather than being swept away by trauma-driven narratives. This process helps distinguish between remembering danger and experiencing actual current threat.
Self-as-context develops a stable sense of self that exists beyond your trauma history and current symptoms. Trauma can dominate identity—"I am a trauma survivor" becomes the entire self-concept. This ACT process helps you access a broader perspective: you're the person who has had these experiences and responses, but you're not defined or limited by them.
Values clarification reconnects you with what genuinely matters. Trauma responses often pull life in directions driven by fear and avoidance rather than chosen values. ACT helps identify what you care about in domains like relationships, personal growth, creativity, and contribution, creating a compass for action that isn't dictated by trauma.
Committed action translates values into concrete behavior patterns. This process addresses the way trauma responses create behavioral rigidity—avoiding situations, relationships, or experiences because they might trigger discomfort. Through committed action, you take steps aligned with your values even when trauma responses show up, gradually expanding your behavioral flexibility.
Practical ACT Techniques for Managing Trauma Responses
Experienced therapists working with trauma incorporate specific ACT interventions that help people develop new responses to triggers and difficult internal experiences. These techniques translate the six core processes into practical skills you can use when trauma responses activate.
Expansion practices help you physically make space for difficult sensations that accompany trauma responses. When you notice tightness in your chest, a knot in your stomach, or tension throughout your body, expansion involves breathing into these sensations, imagining space opening around them rather than bracing against them. This counteracts the natural tendency to tighten and resist uncomfortable bodily experiences, which often intensifies them.
Dropping anchor combines several ACT processes into an emergency technique for moments of overwhelm. When a trauma response floods your system, this practice involves: acknowledging what you're experiencing without fighting it, connecting with your physical body through deliberate movement or sensation, and engaging your attention with the environment around you. Tools like Lovon.app can guide you through grounding techniques like this during late-night overwhelm or when something triggering just happened.
Values-based exposure reframes approaching feared situations. Rather than exposure for the purpose of reducing anxiety, ACT-based exposure asks: "What would I approach if I were moving toward what matters, even though discomfort might come along?" This shifts motivation from symptom reduction to values pursuit, which research suggests improves willingness to engage with difficult experiences.
Defusion exercises help during intrusive thoughts or painful memories. Techniques include: repeating a harsh self-judgment slowly until it becomes just sounds, thanking your mind for the thought, naming the story ("there's my 'I'm not safe' story again"), or visualizing thoughts as leaves floating down a stream. These practices don't eliminate thoughts but change their impact on your behavior.
Willingness work directly addresses avoidance patterns. This involves identifying specific situations, people, or experiences you avoid because of trauma responses, then asking: "What am I willing to experience (in terms of discomfort) to move toward what I value?" Willingness isn't wanting distress—it's choosing to experience it as a side effect of valued action.
How ACT Differs from Other Trauma Approaches
Understanding how Acceptance and Commitment Therapy for trauma responses differs from other evidence-based treatments helps clarify when it might be particularly useful. Unlike exposure-based approaches that focus intensively on reducing symptom severity through repeated revisiting of trauma memories, ACT emphasizes changing your relationship with symptoms rather than eliminating them directly.
Practitioners note that many clients remain highly motivated and work hard in therapy, yet progress stalls not because of insufficient effort but because of misunderstandings about recovery timelines. Research on therapeutic change suggests that mental health recovery resembles steering a large ship rather than a responsive car—there's often significant delay between implementing effective strategies and seeing results. This lag causes many people to abandon helpful approaches prematurely, before changes become apparent.
ACT addresses this challenge by shifting focus from symptom reduction as the primary outcome to behavioral flexibility and values alignment. You might still experience trauma responses—intrusive memories, hypervigilance, emotional reactivity—but these symptoms progressively lose their power to dictate your choices. This matters because complete symptom elimination isn't always realistic, and making recovery contingent on becoming symptom-free can paradoxically maintain struggle and avoidance.
Cognitive Behavioral Therapy for trauma typically works to identify and challenge distorted thoughts related to safety, trust, and self-worth. ACT takes a different approach: rather than evaluating whether thoughts are accurate or rational, it teaches defusion—noticing thoughts without being controlled by them regardless of their content. Both approaches demonstrate effectiveness, but ACT may particularly benefit those who've struggled with rumination or found thought-challenging exhausting or ineffective.
Some practitioners integrate ACT principles with other modalities, recognizing that different aspects of trauma recovery benefit from different approaches. Eye Movement Desensitization and Reprocessing (EMDR) processes specific traumatic memories, while ACT addresses the ongoing patterns of experiential avoidance and behavioral inflexibility that trauma creates. These approaches complement rather than compete with each other.
Applying ACT Principles in Daily Life After Trauma
Translating ACT concepts into everyday moments requires practice and patience. When working with trauma responses outside formal therapy, several strategies help build psychological flexibility as part of your routine.
Morning values check-in involves spending a few minutes identifying one small action aligned with your values for that day. This practice counteracts the way trauma responses can make life feel reactive and driven by avoiding discomfort. Even noticing "Today I value connection, so I'll reach out to one friend" creates intentionality.
Noticing avoidance patterns with curiosity rather than judgment helps identify where trauma responses limit your life. When you find yourself declining invitations, putting off difficult conversations, or staying in your comfort zone, ask: "What discomfort am I avoiding? What matters to me in this situation?" This awareness creates choice points where you might act differently.
Self-compassion during responses addresses the additional suffering that comes from judging yourself for having trauma reactions. When a response activates—you snap at someone, feel suddenly panicked, or shut down emotionally—ACT-consistent self-compassion involves acknowledging "This is a moment of suffering, this is part of being human, may I be kind to myself" rather than harsh self-criticism that compounds distress.
Creating space between trigger and action leverages the pause that mindfulness practice develops. Trauma responses often create urgency—immediate impulses to flee, fight, freeze, or please. Building even a few seconds between the trigger and your behavioral response allows space to choose: "This response is here. What action aligns with who I want to be in this moment?"
Support tools can bridge the gap between therapy sessions when you need to process what's happening. Services like Lovon.app provide on-demand conversation for working through a difficult moment, preparing for a challenging situation, or simply talking through patterns you're noticing. These resources complement formal therapy by offering accessible support during the actual moments when trauma responses show up in your daily life.
When to Seek Professional Support for Trauma Responses
While ACT principles and techniques can be practiced independently, working with a trained therapist significantly enhances effectiveness, particularly for complex trauma presentations. Professional support becomes essential when trauma responses create substantial functional impairment—interfering with work, relationships, self-care, or safety.
Specific indicators that professional help is needed include: persistent thoughts of self-harm or suicide, severe dissociation that creates gaps in awareness or memory, substance use as a primary coping strategy, trauma responses that haven't improved with self-help approaches after several months, or increasing avoidance that progressively narrows your life.
Therapists trained specifically in ACT for trauma can provide individualized guidance, help you navigate stuck points, and adjust the approach based on your particular trauma history and current responses. Look for licensed mental health professionals who list ACT or contextual behavioral science in their specializations, ideally with specific training in trauma treatment.
The therapeutic relationship itself serves as a practice ground for many ACT principles—noticing what shows up in session, staying present with vulnerability, and taking risks aligned with your values. This experiential learning often proves more powerful than simply understanding ACT concepts intellectually.
Conclusion
Acceptance and Commitment Therapy for trauma responses offers a compassionate, empirically-supported path forward that doesn't require eliminating all symptoms before you can live meaningfully. By developing psychological flexibility—the capacity to be present with difficult internal experiences while taking values-based action—you progressively reduce trauma's control over your choices and behaviors.
The journey involves learning to notice trauma responses with curiosity rather than fear, creating space for uncomfortable thoughts and feelings rather than struggling against them, and consistently taking small steps toward what matters even when discomfort comes along. Recovery isn't linear, and setbacks don't erase progress—they're opportunities to practice the skills ACT develops.
Whether you're working with a therapist, using accessible tools like Lovon.app for between-session support, or applying these principles independently, the core insight remains: you don't have to wait until trauma responses disappear to start building the life you value. Start where you are, work with what shows up, and take the next smallest step in a valued direction.
Disclaimer: This is general information, not medical advice or diagnosis. If symptoms are severe, affecting your daily life, or you're having thoughts of self-harm—seek professional help. In the US: call or text 988 (Suicide & Crisis Lifeline). For immediate danger: 911 or local emergency services.
How AI Support Helps You Heal
AI emotional support isn't about replacing human connection — it's about filling the gaps. The moments when you need to talk at 2 AM, when you don't want to burden your friends again, or when you simply need someone to listen without judgment.
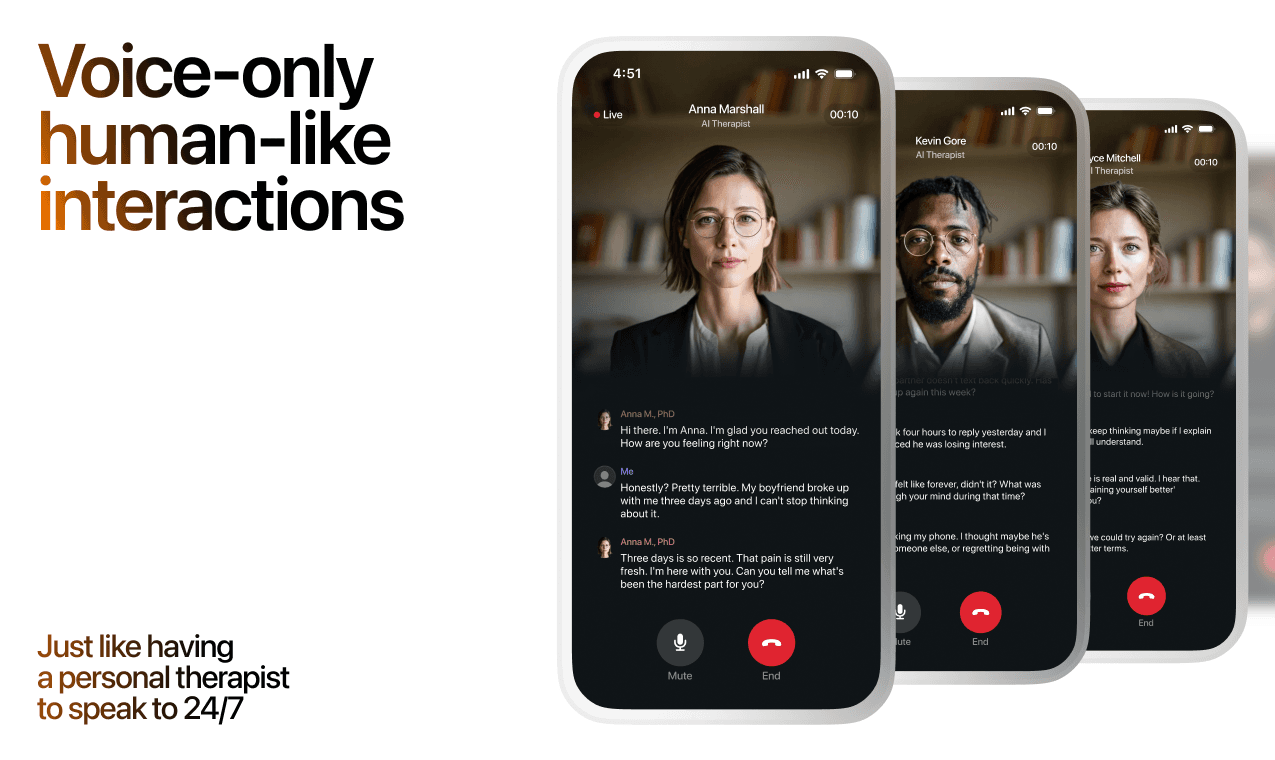
Here's what happens in a typical Lovon session:
You share what's on your mind
There's no script, no intake form, no waiting room. You speak or type whatever you're feeling — in your own words, at your own pace.
Lovon validates and explores
Using frameworks from CBT (Cognitive Behavioral Therapy) and motivational interviewing, Lovon acknowledges your feelings first, then gently helps you explore them. No dismissive "just move on" advice.
You build coping skills together
Lovon doesn't just listen — it actively works with you on evidence-based techniques: thought reframing, urge surfing, behavioral experiments, and more.
What a Session with Lovon Looks Like
When to Seek Professional Help
AI support is a valuable tool, but it's not a replacement for professional care. Please consider reaching out to a licensed therapist if you experience any of the following:
- Persistent thoughts of self-harm or suicide
- Inability to perform daily activities (work, eating, sleeping) for more than 2 weeks
- Turning to alcohol or substances to cope
- Intense anger or desire to harm your ex-partner
- Complete emotional numbness that doesn't improve over time
Crisis Resources (US): If you're in immediate danger, call 988 (Suicide & Crisis Lifeline) or text HOME to 741741 (Crisis Text Line). Available 24/7, free, and confidential.
Outside the US? Find a crisis line in your country
Ready to Start?
Your healing journey can begin right now
1 free conversation. No credit card. No judgment. Just a safe space to process what you're going through.
Frequently Asked Questions
Is AI therapy a replacement for a real therapist?
Is my conversation with Lovon AI private?
How is Lovon different from ChatGPT for emotional support?
Can I use Lovon if I'm already seeing a therapist?
Can I try Lovon for free?
About the Author
The Lovon Editorial Team
Mental Health & Wellness Content Team
The Lovon Editorial Team develops mental health and wellness content designed to make psychological concepts accessible and actionable. Our goal is to bridge the gap between clinical research and everyday life - helping you understand why your mind works the way it does and what you can do about it....
Similar Articles
Amygdala and Prefrontal Cortex Connection: Training Emotional Regulation Through Mindfulness
How mindfulness practices reshape neural pathways to strengthen emotional control and reduce reactivity
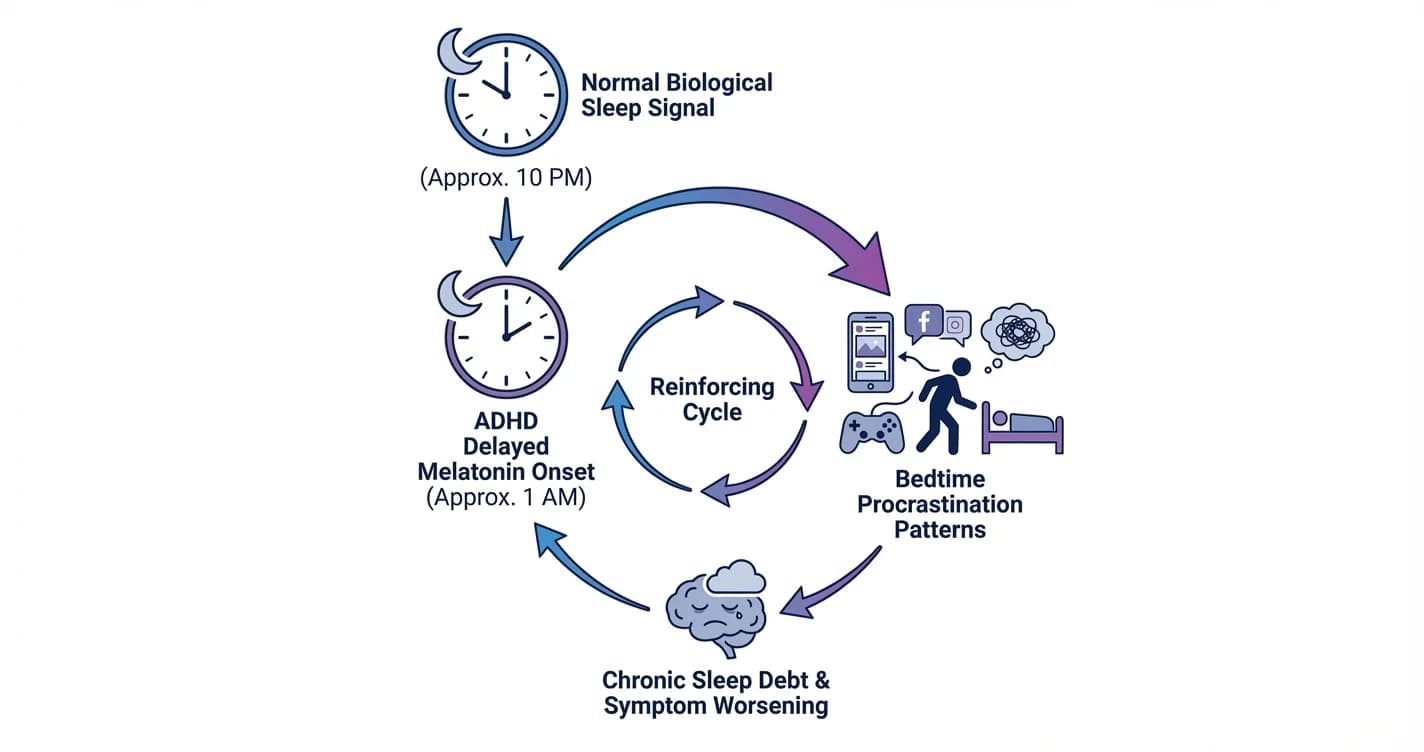
ADHD Sleep Cycle Disruption: Melatonin Delay and Bedtime Procrastination Patterns
Understanding how attention regulation difficulties interfere with natural sleep timing and the nightly wind-down process
ADHD Comorbidity with Anxiety and Depression Cycles
Understanding the Complex Interplay Between ADHD and Recurring Mental Health Patterns
Disclaimer: This article is for informational purposes only and does not constitute medical advice, diagnosis, or treatment. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition. If you are in crisis or think you may have an emergency, call 988 (Suicide & Crisis Lifeline) or go to the nearest emergency room. Outside the US? Find a crisis line in your country.