Best Treatments for Depression That Doesn't Respond to Medication
When antidepressants don't provide relief, the frustration can feel overwhelming. Treatment-resistant depression affects a significant portion of people...

Key Takeaways
- Core beliefs and deeply ingrained negative schemas
- Behavioral activation to counter withdrawal and avoidance
- Cognitive restructuring techniques for persistent rumination
- Problem-solving skills for chronic stressors
- Mindfulness practices for present-moment awareness
Introduction
When antidepressants don't provide relief, the frustration can feel overwhelming. Treatment-resistant depression affects a significant portion of people seeking help for depressive disorders, leaving many wondering what options remain when medications fail to work. The best treatments for depression that doesn't respond to medication often involve specialized psychotherapy approaches, lifestyle interventions, and advanced therapeutic techniques that address the condition from multiple angles. This comprehensive guide explores evidence-based alternatives and complementary strategies that mental health professionals recommend when standard pharmaceutical interventions fall short. Based on current clinical research and expert practitioners' experiences, these approaches offer genuine hope for managing chronic depression that proves resistant to medication alone.
Understanding Treatment-Resistant Depression
Treatment-resistant depression typically refers to major depressive disorder that hasn't adequately responded to at least two different antidepressant trials at appropriate dosages and duration. However, "resistance" doesn't mean hopelessness—it often signals that a different therapeutic approach may be needed.
Research suggests that various factors contribute to medication non-response, including genetic variations affecting drug metabolism, co-occurring conditions, chronic stress, and the complex interplay between biological, psychological, and environmental influences. Understanding that depression exists on a spectrum helps explain why a one-size-fits-all approach rarely works.
Some individuals experience what practitioners call "partial response"—where symptoms improve slightly but never fully resolve. Others find medications provide no noticeable benefit whatsoever. In both cases, expanding treatment beyond pharmacology becomes essential for meaningful recovery.
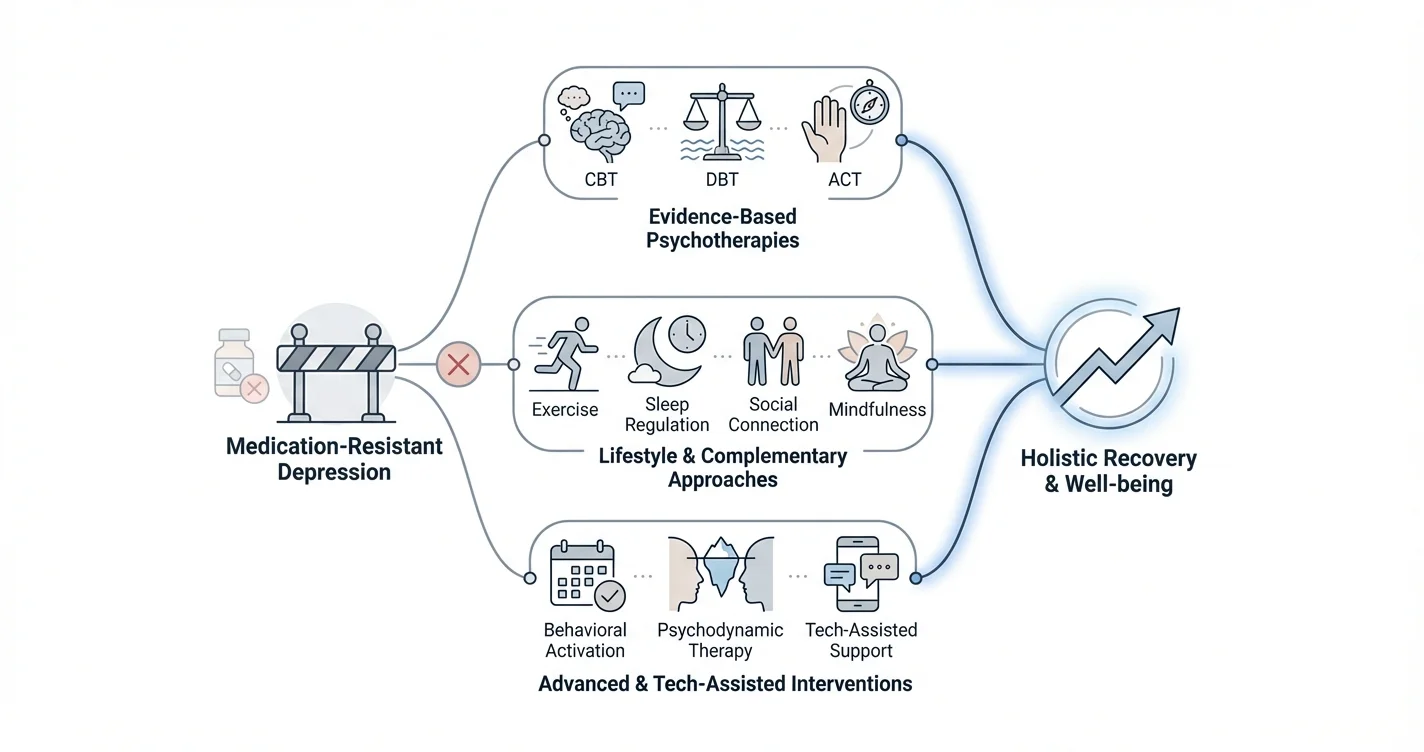
Evidence-Based Psychotherapy Approaches for Medication-Resistant Depression
Cognitive Behavioral Therapy (CBT)
Cognitive Behavioral Therapy remains one of the most rigorously studied therapeutic approaches for treatment-resistant depression. Studies indicate that CBT can be as effective as medication for some individuals and may provide longer-lasting benefits by teaching concrete skills for managing depressive thinking patterns.
CBT focuses on identifying and restructuring negative thought patterns that perpetuate depressive states. When working with treatment-resistant depression, therapists typically employ enhanced protocols that address:
- Core beliefs and deeply ingrained negative schemas
- Behavioral activation to counter withdrawal and avoidance
- Cognitive restructuring techniques for persistent rumination
- Problem-solving skills for chronic stressors
Many practitioners report that patients who haven't responded to medication often show significant improvement when CBT is delivered with sufficient intensity and duration—typically 16-20 sessions or more for complex cases.
Dialectical Behavior Therapy (DBT)
Originally developed for borderline personality disorder, Dialectical Behavior Therapy has shown promise for chronic depression, particularly when emotional dysregulation plays a central role. DBT combines acceptance-based strategies with change-oriented techniques, teaching four core skill sets:
- Mindfulness practices for present-moment awareness
- Distress tolerance skills for managing crisis situations
- Emotion regulation techniques for reducing vulnerability to mood episodes
- Interpersonal effectiveness training for navigating relationships
For individuals whose depression involves intense emotional reactivity, self-destructive behaviors, or relationship difficulties, DBT may address underlying patterns that medication alone cannot reach.
Acceptance and Commitment Therapy (ACT)
Acceptance and Commitment Therapy takes a different approach by focusing less on symptom reduction and more on building psychological flexibility. ACT helps individuals develop a different relationship with depressive thoughts and feelings rather than trying to eliminate them.
Key components include:
- Acceptance of difficult internal experiences without struggle
- Cognitive defusion techniques to reduce the power of negative thoughts
- Clarifying personal values independent of mood states
- Committed action toward meaningful life goals despite depression
Research suggests ACT may be particularly valuable for chronic depression that hasn't responded to more traditional symptom-focused treatments.
Advanced Therapeutic Interventions When Medications Fail
Psychodynamic and Interpersonal Approaches
Long-term psychodynamic therapy explores how past experiences, unconscious conflicts, and relational patterns contribute to persistent depression. While requiring more time investment, some studies indicate this approach can produce lasting changes for chronic depression.
Interpersonal Therapy (IPT) specifically targets relationship difficulties, role transitions, grief, and interpersonal deficits that may maintain depressive states. Research shows IPT can be effective for treatment-resistant cases, particularly when depression relates to ongoing relational stress or unresolved loss.
Mindfulness-Based Cognitive Therapy (MBCT)
Mindfulness-Based Cognitive Therapy combines mindfulness meditation practices with cognitive therapy elements. Originally developed to prevent relapse in recurrent depression, MBCT helps individuals recognize early warning signs and disengage from depressive rumination.
Practitioners note that MBCT works particularly well for people who experience repetitive negative thinking patterns that medication doesn't adequately address. The approach teaches individuals to observe thoughts without automatically believing or reacting to them—a skill that becomes increasingly important when depression has become a familiar, almost comfortable state despite its suffering.
One practitioner with decades of depression experience noted the paradoxical fear of healing—the way familiar suffering can feel safer than the unknown territory of recovery. This insight highlights why therapeutic approaches addressing identity, meaning, and relationship to one's experience may reach aspects of depression that biological interventions cannot.
Behavioral Activation
Behavioral activation operates on the principle that depression perpetuates itself through withdrawal and inactivity. This structured approach helps individuals systematically re-engage with potentially rewarding activities, even when motivation is absent.
The technique involves:
- Monitoring current activity patterns and mood connections
- Identifying values-based activities that might provide meaning or pleasure
- Scheduling specific behaviors regardless of current motivation
- Gradually building momentum through small, achievable steps
Research indicates behavioral activation can be as effective as more complex therapies for certain individuals, making it a valuable component of treatment plans for medication-resistant depression.
Complementary and Integrative Approaches
Lifestyle Modifications With Therapeutic Support
While lifestyle changes alone rarely resolve treatment-resistant depression, when integrated with psychotherapy they can significantly enhance outcomes:
Exercise interventions: Structured exercise programs, particularly aerobic activity, show evidence for reducing depressive symptoms. Some research suggests regular physical activity may produce brain changes similar to certain antidepressants.
Sleep regulation: Addressing sleep disturbances through behavioral interventions like cognitive behavioral therapy for insomnia (CBT-I) can improve mood stability. Sleep and depression maintain a bidirectional relationship—each affecting the other.
Nutritional psychiatry: Emerging research explores how dietary patterns influence mental health. While not a standalone treatment, nutritional approaches may support other interventions.
Light therapy: For some individuals, particularly those with seasonal patterns or circadian rhythm disturbances, structured light exposure may provide benefit.
Technology-Assisted Therapeutic Support
Digital mental health tools have expanded access to therapeutic support between traditional sessions. Platforms like Lovon.app provide on-demand voice-based conversations that help individuals process difficult emotions, work through relationship conflicts, and identify recurring patterns when they need support most—late at night, between therapy appointments, or when situations are unfolding in real-time.
These tools function as complementary resources rather than replacements for professional treatment, offering reflection and perspective during moments when traditional therapy isn't immediately available. For someone managing chronic depression, having accessible support during vulnerable periods can help maintain therapeutic gains and prevent deterioration.
Social Connection and Relational Healing
Depression typically involves withdrawal from social contact, yet isolation perpetuates depressive states. Therapeutic approaches that rebuild social connections include:
- Group therapy formats providing both support and accountability
- Interpersonal skill-building to address relationship difficulties
- Structured social activities integrated into treatment plans
- Peer support programs connecting individuals with shared experiences
Research consistently shows that quality social relationships predict better outcomes in depression treatment, regardless of whether medication is involved.
Addressing Psychological Barriers to Recovery
An often-overlooked aspect of treatment-resistant depression involves psychological factors that may unconsciously maintain depressive states. Some individuals develop identities deeply intertwined with their depression after years of struggling with the condition.
This phenomenon—where healing feels threatening because it requires becoming someone unfamiliar—can create subtle resistance to recovery even while consciously desiring relief. Therapeutic approaches that address these identity concerns include:
- Exploring ambivalence about recovery in a non-judgmental space
- Gradually building a sense of self that includes but isn't limited to depression
- Identifying fears about what might be expected or demanded without depression as an "excuse"
- Developing new coping strategies before relinquishing familiar (if painful) patterns
Tools like Lovon.app can provide space to explore these complex feelings between therapy sessions, helping individuals articulate concerns they might struggle to name and preparing them for deeper therapeutic work.
Understanding that recovery involves not just symptom reduction but fundamental shifts in how one relates to oneself and the world helps explain why purely biological interventions sometimes prove insufficient for lasting change.
When to Seek Professional Help
If you're experiencing treatment-resistant depression, professional guidance remains essential for several reasons:
Comprehensive assessment: Determining whether apparent medication resistance might actually reflect misdiagnosis, inadequate treatment trials, or co-occurring conditions requires expert evaluation.
Safety concerns: If you're experiencing thoughts of self-harm, significant functional impairment, or worsening symptoms, immediate professional support is necessary.
Specialized treatment: Many effective interventions for treatment-resistant depression—including the psychotherapy approaches discussed here—require trained professionals for proper implementation.
Consider seeking help from mental health professionals specializing in treatment-resistant depression, including psychologists trained in evidence-based therapies, psychiatrists who can evaluate medication strategies comprehensively, and therapists with expertise in chronic or complex depression presentations.
Conclusion
The best treatments for depression that doesn't respond to medication involve comprehensive approaches that address psychological, behavioral, social, and lifestyle factors contributing to persistent symptoms. Evidence-based psychotherapies like CBT, DBT, and ACT offer proven alternatives to medication-only approaches, while advanced interventions including psychodynamic therapy, mindfulness-based treatments, and behavioral activation provide additional pathways to recovery.
Recovery from treatment-resistant depression rarely follows a straight line, and what works differs significantly between individuals. The combination of professional psychotherapy, lifestyle modifications, supportive technologies, and attention to relational healing creates multiple entry points for improvement. Tools like Lovon.app can complement professional treatment by providing accessible support during difficult moments, helping maintain therapeutic progress between sessions.
If medications haven't provided the relief you need, remember that treatment-resistant doesn't mean treatment-impossible. Working with qualified mental health professionals who understand evidence-based alternatives to pharmacological approaches can open pathways to recovery that address the full complexity of your experience. The journey may require patience and persistence, but numerous therapeutic options exist beyond medication alone.
Disclaimer: This is general information, not medical advice or diagnosis. If symptoms are severe, affecting your daily life, or you're having thoughts of self-harm — seek professional help. In the US: call or text 988 (Suicide & Crisis Lifeline). For immediate danger: 911 or local emergency services.
How AI Support Helps You Heal
AI emotional support isn't about replacing human connection — it's about filling the gaps. The moments when you need to talk at 2 AM, when you don't want to burden your friends again, or when you simply need someone to listen without judgment.
Here's what happens in a typical Lovon session:
You share what's on your mind
There's no script, no intake form, no waiting room. You speak or type whatever you're feeling — in your own words, at your own pace.
Lovon validates and explores
Using frameworks from CBT (Cognitive Behavioral Therapy) and motivational interviewing, Lovon acknowledges your feelings first, then gently helps you explore them. No dismissive "just move on" advice.
You build coping skills together
Lovon doesn't just listen — it actively works with you on evidence-based techniques: thought reframing, urge surfing, behavioral experiments, and more.
What a Session with Lovon Looks Like
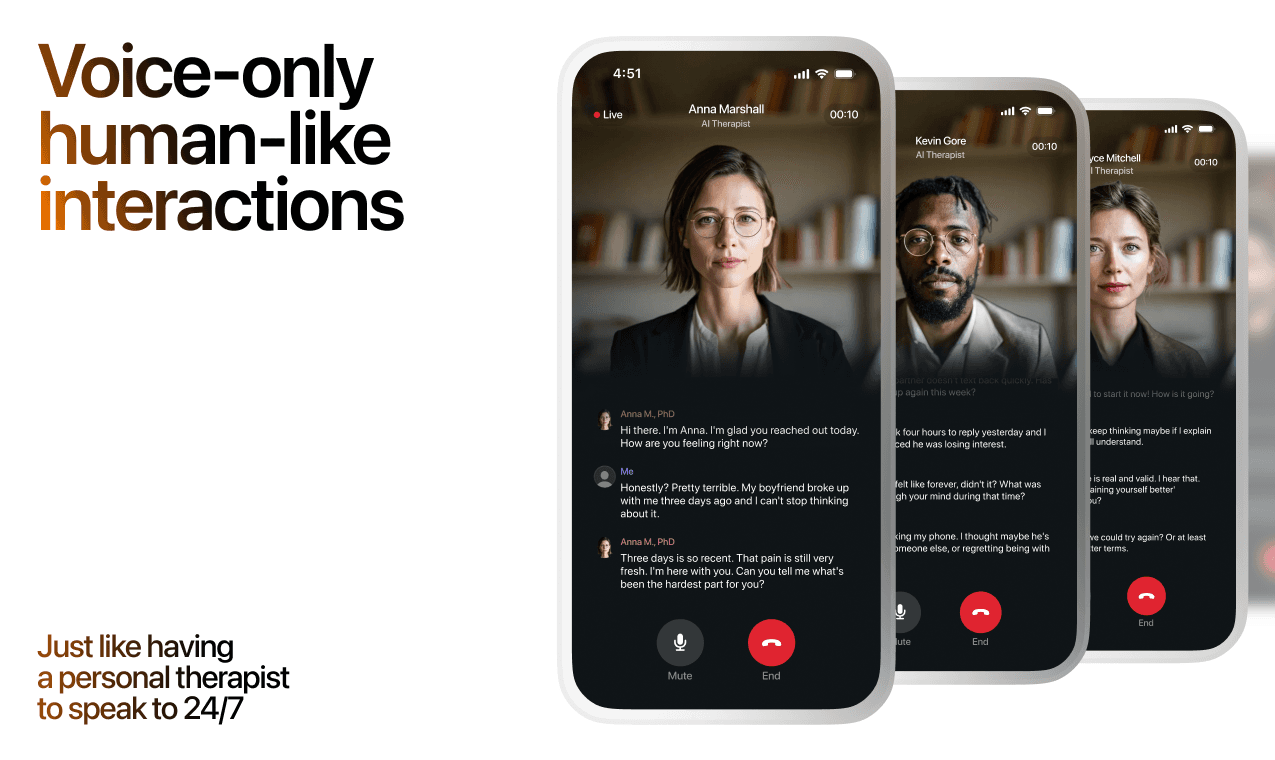
When to Seek Professional Help
AI support is a valuable tool, but it's not a replacement for professional care. Please consider reaching out to a licensed therapist if you experience any of the following:
- Persistent thoughts of self-harm or suicide
- Inability to perform daily activities (work, eating, sleeping) for more than 2 weeks
- Turning to alcohol or substances to cope
- Intense anger or desire to harm your ex-partner
- Complete emotional numbness that doesn't improve over time
Crisis Resources (US): If you're in immediate danger, call 988 (Suicide & Crisis Lifeline) or text HOME to 741741 (Crisis Text Line). Available 24/7, free, and confidential.
Outside the US? Find a crisis line in your country
Ready to Start?
Your healing journey can begin right now
1 free conversation. No credit card. No judgment. Just a safe space to process what you're going through.
Frequently Asked Questions
Is AI therapy a replacement for a real therapist?
Is my conversation with Lovon AI private?
How is Lovon different from ChatGPT for emotional support?
Can I use Lovon if I'm already seeing a therapist?
Can I try Lovon for free?
About the Author
The Lovon Editorial Team
Mental Health & Wellness Content Team
The Lovon Editorial Team develops mental health and wellness content designed to make psychological concepts accessible and actionable. Our goal is to bridge the gap between clinical research and everyday life - helping you understand why your mind works the way it does and what you can do about it....
Similar Articles
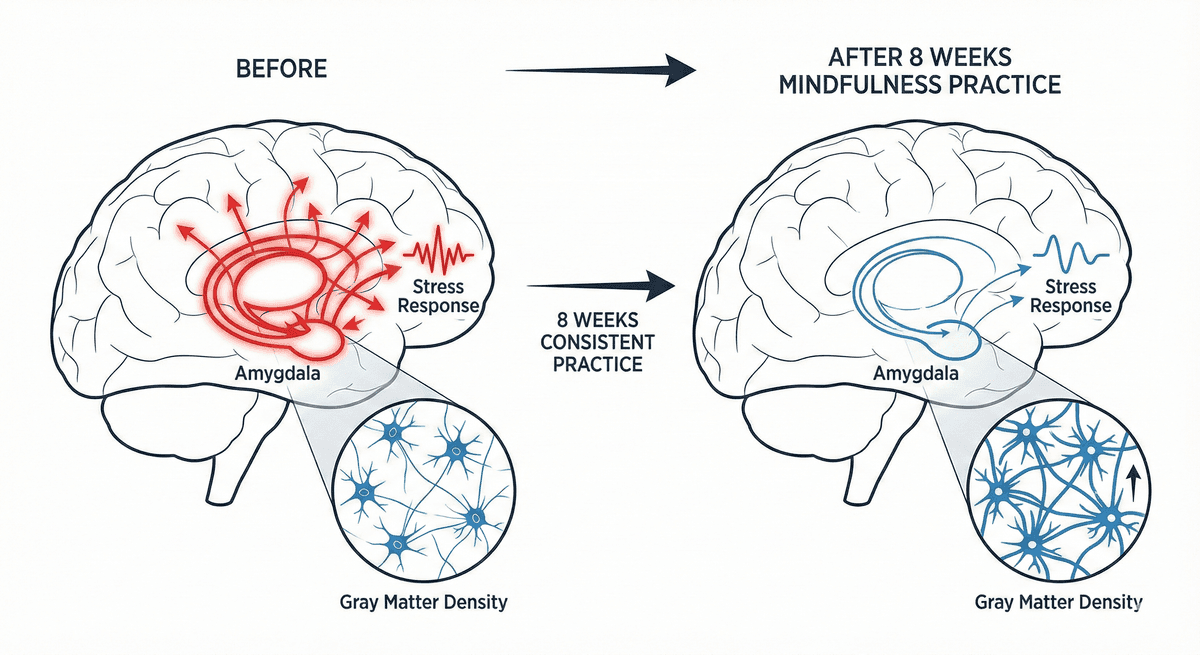
Amygdala Reactivity Reduction: Gray Matter Changes After Eight Weeks of Mindfulness Practice
Discover how eight weeks of mindfulness practice reshapes the brain, reducing amygdala reactivity and building lasting neural resilience.
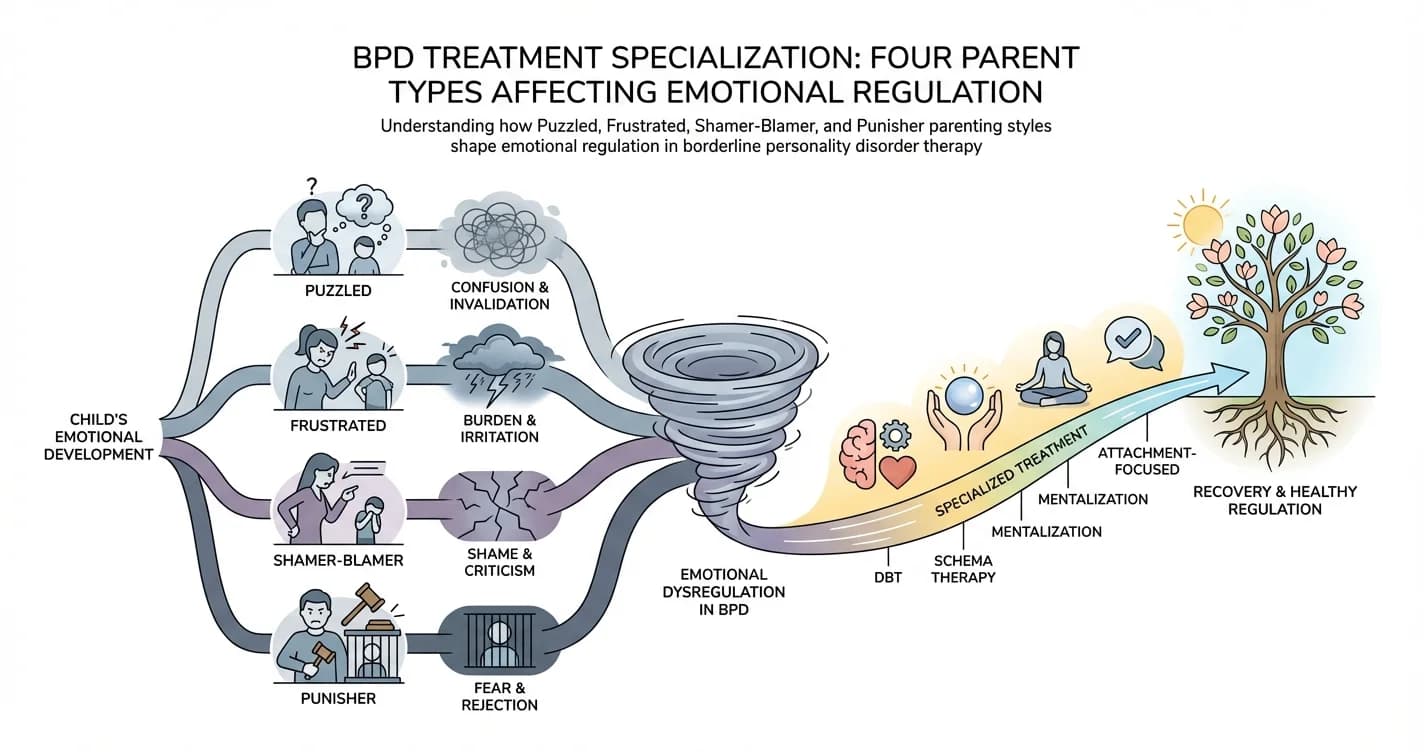
BPD Treatment Specialization: Four Parent Types Affecting Emotional Regulation
For individuals with borderline personality disorder (BPD), emotional regulation difficulties rarely emerge in isolation. Research increasingly suggests that
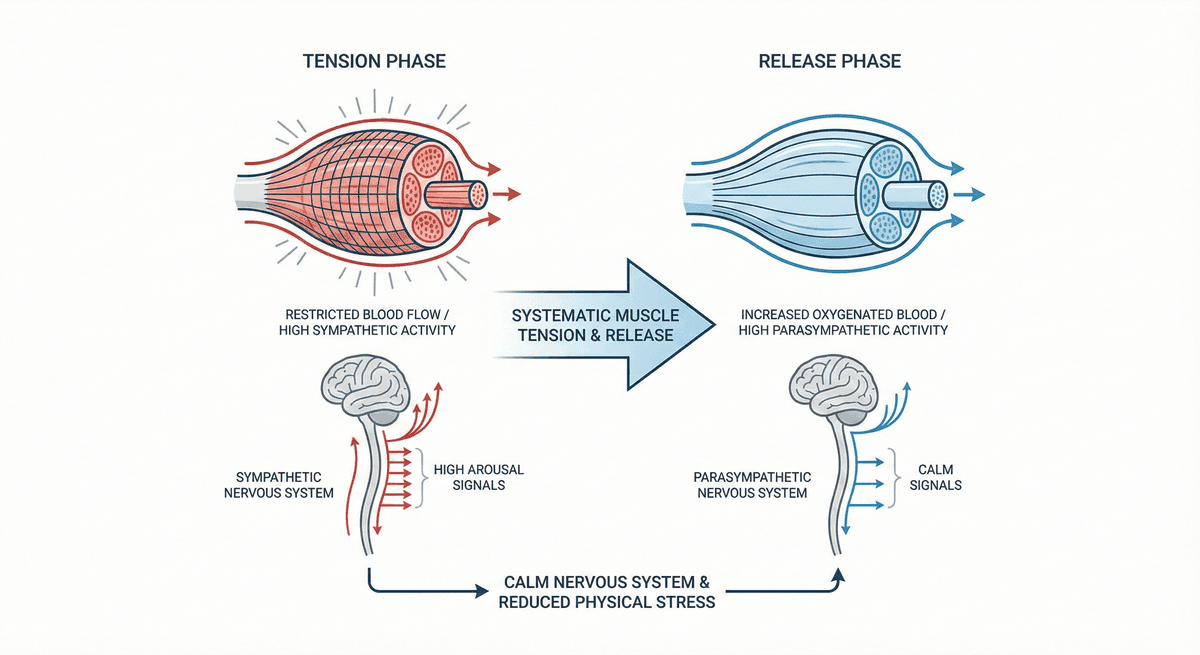
Progressive Muscle Relaxation for Stress Reduction
A systematic muscle group tension and release technique that calms the nervous system and reduces physical stress.
Disclaimer: This article is for informational purposes only and does not constitute medical advice, diagnosis, or treatment. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition. If you are in crisis or think you may have an emergency, call 988 (Suicide & Crisis Lifeline) or go to the nearest emergency room. Outside the US? Find a crisis line in your country.