PANDAS: Pediatric Autoimmune Neuropsychiatric Disorder Linked to Streptococcal Infections
When a child suddenly develops severe obsessive-compulsive behaviors, uncontrollable tics, or dramatic personality changes seemingly overnight, parents often

Key Takeaways
- Intrusive, repetitive thoughts that cause significant distress
- Compulsive rituals around contamination, symmetry, or checking
- Excessive concern with illness or harm
- Dramatic increase in anxiety around specific themes
- Motor tics (eye blinking, facial grimacing, shoulder shrugging)
Introduction
When a child suddenly develops severe obsessive-compulsive behaviors, uncontrollable tics, or dramatic personality changes seemingly overnight, parents often feel bewildered and frightened. While many conditions can cause behavioral shifts in children, PANDAS—pediatric autoimmune neuropsychiatric disorder linked to streptococcal infections—represents a specific syndrome where these dramatic changes follow a strep throat or scarlet fever infection. Understanding this condition requires recognizing how the body's immune response to streptococcal bacteria may inadvertently target brain tissue, producing profound neuropsychiatric symptoms. This article examines the mechanisms, recognition patterns, and management approaches for PANDAS based on current clinical understanding and expert observations from pediatric specialists working with affected families as of January 2026.
Understanding PANDAS and Its Autoimmune Mechanisms
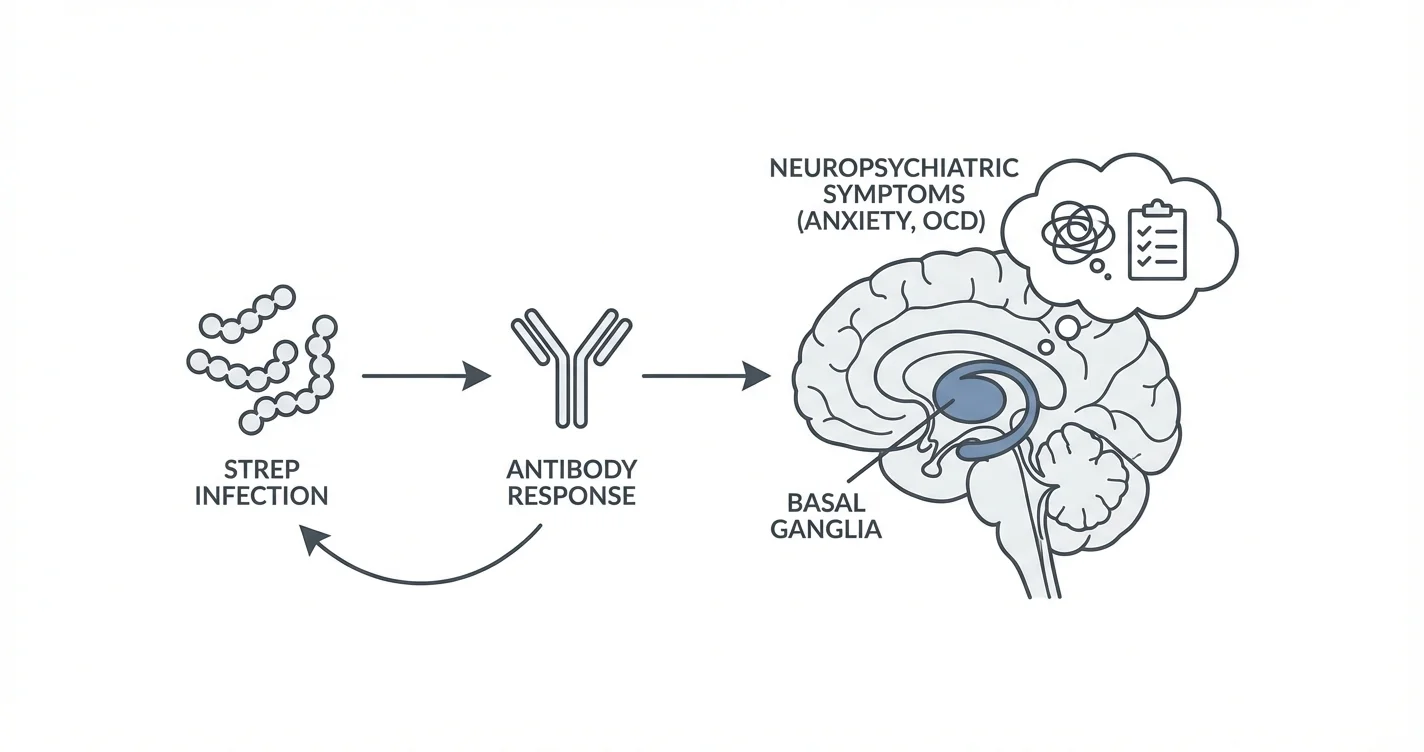
PANDAS represents a pediatric autoimmune neuropsychiatric disorder linked to streptococcal infections, specifically Group A Streptococcus (GAS), the bacteria responsible for strep throat and scarlet fever. The condition is characterized by an abrupt onset of obsessive-compulsive symptoms, tics, or both following a streptococcal infection. Research suggests that in susceptible children, the immune system's antibodies produced to fight the strep bacteria may cross-react with proteins in the basal ganglia—brain structures involved in movement control and behavior regulation.
This molecular mimicry hypothesis proposes that antibodies intended to target streptococcal antigens instead bind to neuronal tissues, triggering inflammation in specific brain regions. Clinical observations indicate that this autoimmune response can produce dramatic behavioral and neurological changes within days or weeks of the initial infection, though the infection itself may have resolved or produced only mild symptoms.
Practitioners note that PANDAS functions as an episodic disorder, meaning symptoms may improve and then recur with subsequent streptococcal exposures. This pattern of symptom fluctuation related to infections distinguishes PANDAS from gradual-onset conditions and helps guide clinical recognition. The episodic nature also creates significant uncertainty for families, as children may experience periods of relative normalcy punctuated by acute symptom flares.
Recognizing PANDAS: Symptom Patterns and Clinical Presentation
The hallmark feature of this pediatric autoimmune neuropsychiatric disorder linked to streptococcal infections is the sudden, dramatic onset of symptoms. Parents frequently describe their child as "not themselves" or report that changes occurred "literally overnight." Key symptom categories include:
Obsessive-Compulsive Behaviors:
- Intrusive, repetitive thoughts that cause significant distress
- Compulsive rituals around contamination, symmetry, or checking
- Excessive concern with illness or harm
- Dramatic increase in anxiety around specific themes
Movement Abnormalities:
- Motor tics (eye blinking, facial grimacing, shoulder shrugging)
- Vocal tics (throat clearing, sniffing, words or sounds)
- Choreiform movements (involuntary, dance-like motions)
- Handwriting deterioration due to fine motor changes
Behavioral and Emotional Shifts:
- Sudden separation anxiety in previously independent children
- Mood lability with irritability or emotional outbursts
- Sleep disturbances and nighttime fears
- Regression in developmental skills
- Changes in eating patterns or new food restrictions
Experts emphasize that the temporal relationship between streptococcal infection and symptom onset provides crucial diagnostic information. While some children have documented positive strep tests, others may have had asymptomatic or minimally symptomatic infections, making the connection less obvious to families and clinicians. This diagnostic complexity means that careful clinical history-taking becomes essential for recognition.
Diagnostic Approaches and Clinical Evaluation
Diagnosing PANDAS involves integrating clinical history, physical examination, and laboratory testing. Unlike conditions with definitive biomarkers, diagnosis relies significantly on pattern recognition and clinical judgment. Medical evaluation typically includes several components:
Clinical History Assessment: Medical practitioners look for evidence of acute symptom onset, temporal association with documented or suspected streptococcal infection, and episodic symptom course with periods of improvement. The abrupt nature of symptom appearance—developing over 24 to 48 hours rather than gradually over months—provides critical diagnostic information.
Laboratory Testing: Testing may include throat cultures or rapid strep tests to identify active infections, and anti-streptolysin O (ASO) and anti-DNase B antibody titers to detect recent streptococcal exposure. However, specialists note that antibody titers reflect recent immune exposure to streptococcal bacteria but don't confirm causation of neuropsychiatric symptoms, making interpretation complex. Elevated titers indicate recent strep exposure but are common in children even without PANDAS.
Differential Diagnosis: Clinicians must distinguish PANDAS from other conditions presenting with similar symptoms, including primary obsessive-compulsive disorder, tic disorders, Sydenham's chorea (another post-streptococcal neurological condition), and other autoimmune encephalopathies. This process requires careful evaluation of symptom timeline, associated features, and response patterns.
The episodic nature of symptoms that may resolve and recur with subsequent infections represents a distinguishing feature. According to pediatric specialists, families often notice that their child returns to baseline functioning between episodes, though some children develop persistent symptoms requiring ongoing management.
Treatment Approaches and Management Strategies
Managing this streptococcal infection-triggered pediatric autoimmune neuropsychiatric disorder typically involves multiple therapeutic approaches, often used in combination based on symptom severity and individual presentation:
Antibiotic Treatment: When active streptococcal infections are identified, appropriate antibiotic therapy addresses the triggering infection. Some practitioners also consider prophylactic antibiotics to prevent recurrent strep infections in children with documented PANDAS, though this approach remains debated and should be discussed thoroughly with healthcare providers familiar with the condition.
Immunomodulatory Interventions: For severe cases, treatments targeting the underlying immune response may be considered. These specialized interventions are typically reserved for children with significant functional impairment and are administered by physicians experienced in autoimmune conditions.
Symptomatic Management: Addressing the neuropsychiatric symptoms themselves often involves evidence-based treatments for obsessive-compulsive symptoms and tics. Cognitive-behavioral therapy, particularly exposure and response prevention for OCD symptoms, provides children with skills to manage intrusive thoughts and compulsions. This therapeutic approach helps even when symptoms have an autoimmune trigger.
Supportive Care: Families benefit from education about the episodic nature of the condition and strategies for managing acute symptom flares. School accommodations may be necessary during symptomatic periods, and emotional support for both the affected child and family members helps address the psychological impact of dramatic behavioral changes.
For families navigating the emotional turbulence of caring for a child with PANDAS, accessible support resources like Lovon.app can provide on-demand emotional processing when concerns arise between medical appointments. While such tools don't replace specialized medical care, they offer parents a space to work through the stress and uncertainty that accompanies managing a complex pediatric condition.
Long-Term Outlook and Family Considerations
The episodic nature of PANDAS means that long-term outcomes vary considerably among affected children. Some experience a single episode with complete resolution, while others have recurring symptoms with streptococcal exposures throughout childhood. Clinical observations suggest that many children show improvement as their immune systems mature, with symptoms often diminishing during adolescence.
However, practitioners emphasize that this trajectory isn't universal—some children develop persistent neuropsychiatric symptoms requiring ongoing management even after the autoimmune component stabilizes. Early recognition and appropriate treatment appear to influence outcomes, though research continues to clarify which specific interventions provide the most benefit.
Family Impact Considerations:
The sudden onset and unpredictable course of PANDAS create significant stress for families. Parents often report feeling dismissed when describing their child's dramatic overnight changes, particularly if medical providers are unfamiliar with the condition. Connecting with healthcare practitioners experienced in pediatric autoimmune conditions and finding supportive communities can help families navigate diagnosis and treatment decisions.
Siblings may also struggle with the disruption caused by a brother or sister's sudden behavioral changes and the family attention directed toward managing acute symptoms. Family therapy or individual support for siblings helps address these impacts.
When to Seek Professional Help
Parents should seek immediate medical evaluation when children develop sudden, dramatic neuropsychiatric symptoms, particularly following known or suspected streptococcal infections. Specific signs warranting prompt assessment include:
- Abrupt onset of severe obsessive-compulsive behaviors that interfere with daily functioning
- New motor or vocal tics appearing suddenly rather than gradually
- Dramatic personality changes, regression, or behavioral shifts occurring over days
- Separation anxiety so severe the child cannot attend school or separate from parents
- Any indication that the child may harm themselves or others
- Rapid deterioration in functioning across multiple domains (academic, social, self-care)
Specialists in pediatric neurology, rheumatology, immunology, or psychiatry with experience in autoimmune neuropsychiatric conditions can provide comprehensive evaluation. Since PANDAS remains a relatively uncommon condition, seeking providers familiar with its presentation and management improves diagnostic accuracy and treatment planning.
Conclusion
PANDAS—pediatric autoimmune neuropsychiatric disorder linked to streptococcal infections—represents a complex condition where immune responses to common bacterial infections may trigger dramatic neuropsychiatric symptoms in susceptible children. Recognition depends on identifying the characteristic pattern of sudden symptom onset following streptococcal exposure, combined with the episodic course that distinguishes this disorder from other pediatric neuropsychiatric conditions. While diagnostic and treatment approaches continue evolving as research clarifies underlying mechanisms, early recognition and comprehensive management addressing both the infectious trigger and resulting symptoms offer the best outcomes for affected children. Families navigating this challenging condition benefit from connecting with experienced healthcare providers, accessing appropriate treatments, and finding support resources like Lovon.app to process the emotional demands of managing unpredictable symptom fluctuations. As understanding of autoimmune neuropsychiatric conditions advances, improved recognition and targeted interventions promise better support for children affected by these striking post-infectious syndromes.
Disclaimer: This is general information, not medical advice or diagnosis. If symptoms are severe, affecting your daily life, or you're having thoughts of self-harm — seek professional help. In the US: call or text 988 (Suicide & Crisis Lifeline). For immediate danger: 911 or local emergency services.
How AI Support Helps You Heal
AI emotional support isn't about replacing human connection — it's about filling the gaps. The moments when you need to talk at 2 AM, when you don't want to burden your friends again, or when you simply need someone to listen without judgment.
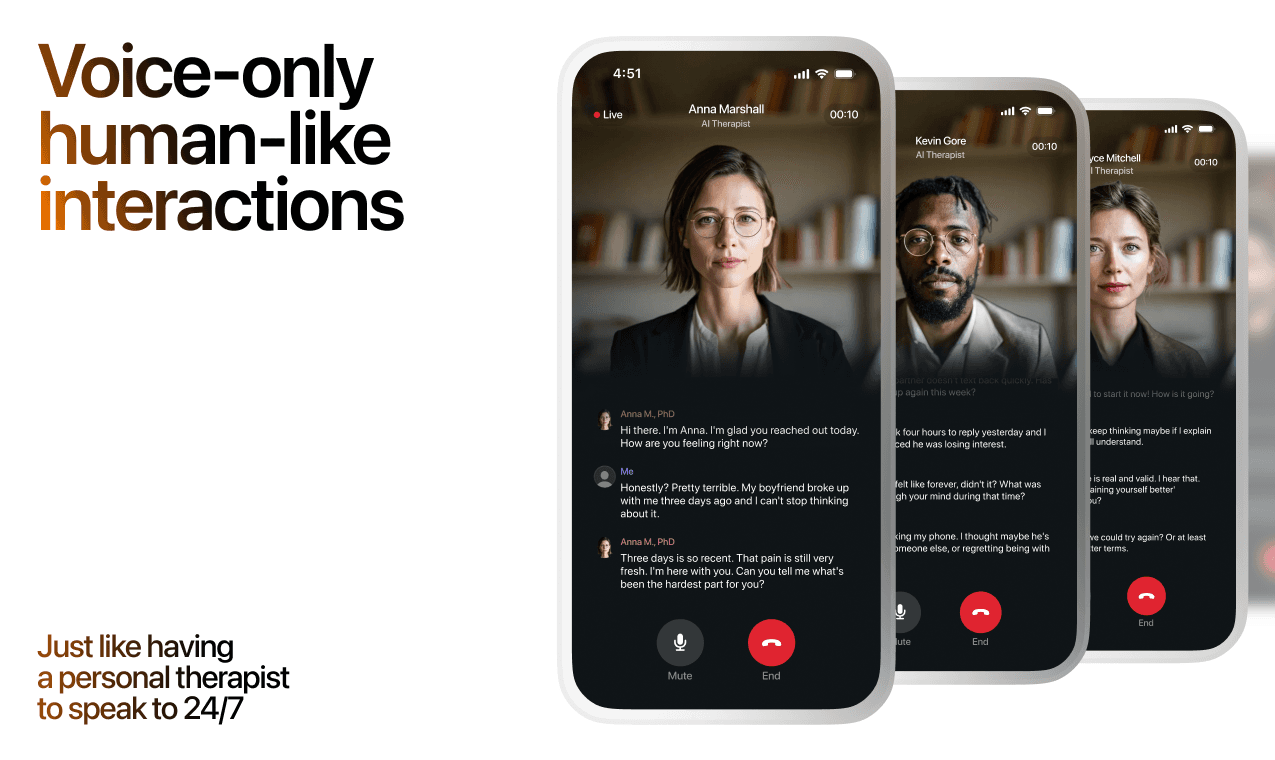
Here's what happens in a typical Lovon session:
You share what's on your mind
There's no script, no intake form, no waiting room. You speak or type whatever you're feeling — in your own words, at your own pace.
Lovon validates and explores
Using frameworks from CBT (Cognitive Behavioral Therapy) and motivational interviewing, Lovon acknowledges your feelings first, then gently helps you explore them. No dismissive "just move on" advice.
You build coping skills together
Lovon doesn't just listen — it actively works with you on evidence-based techniques: thought reframing, urge surfing, behavioral experiments, and more.
What a Session with Lovon Looks Like
When to Seek Professional Help
AI support is a valuable tool, but it's not a replacement for professional care. Please consider reaching out to a licensed therapist if you experience any of the following:
- Persistent thoughts of self-harm or suicide
- Inability to perform daily activities (work, eating, sleeping) for more than 2 weeks
- Turning to alcohol or substances to cope
- Intense anger or desire to harm your ex-partner
- Complete emotional numbness that doesn't improve over time
Crisis Resources (US): If you're in immediate danger, call 988 (Suicide & Crisis Lifeline) or text HOME to 741741 (Crisis Text Line). Available 24/7, free, and confidential.
Outside the US? Find a crisis line in your country
Ready to Start?
Your healing journey can begin right now
1 free conversation. No credit card. No judgment. Just a safe space to process what you're going through.
Frequently Asked Questions
Is AI therapy a replacement for a real therapist?
Is my conversation with Lovon AI private?
How is Lovon different from ChatGPT for emotional support?
Can I use Lovon if I'm already seeing a therapist?
Can I try Lovon for free?
About the Author
The Lovon Editorial Team
Mental Health & Wellness Content Team
The Lovon Editorial Team develops mental health and wellness content designed to make psychological concepts accessible and actionable. Our goal is to bridge the gap between clinical research and everyday life - helping you understand why your mind works the way it does and what you can do about it....
Similar Articles
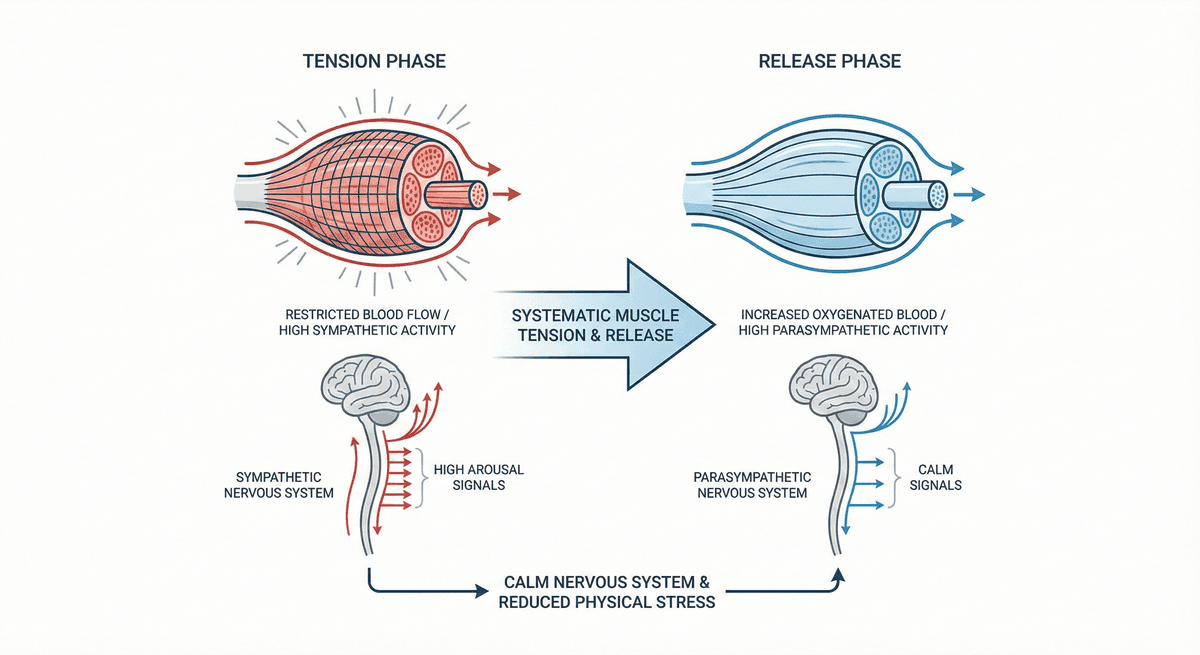
Progressive Muscle Relaxation for Stress Reduction
A systematic muscle group tension and release technique that calms the nervous system and reduces physical stress.
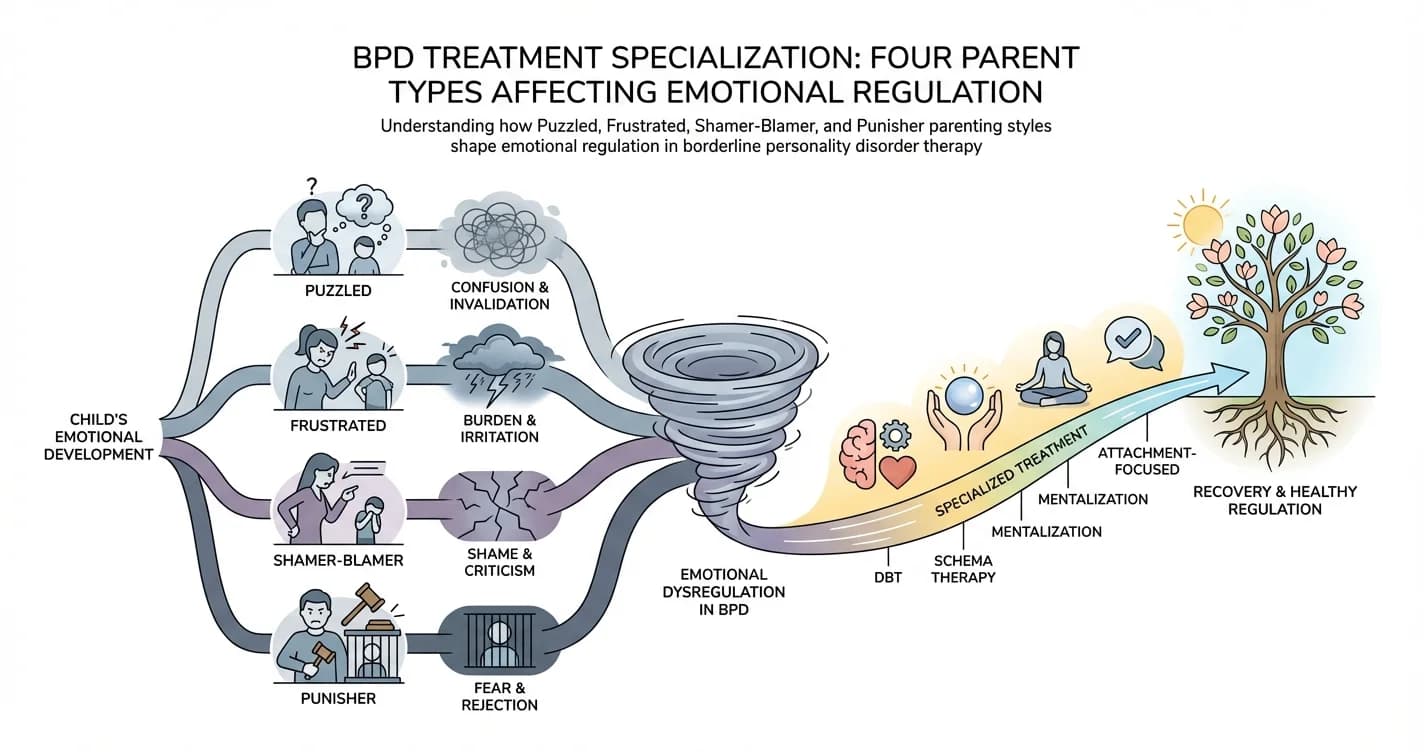
BPD Treatment Specialization: Four Parent Types Affecting Emotional Regulation
For individuals with borderline personality disorder (BPD), emotional regulation difficulties rarely emerge in isolation. Research increasingly suggests that
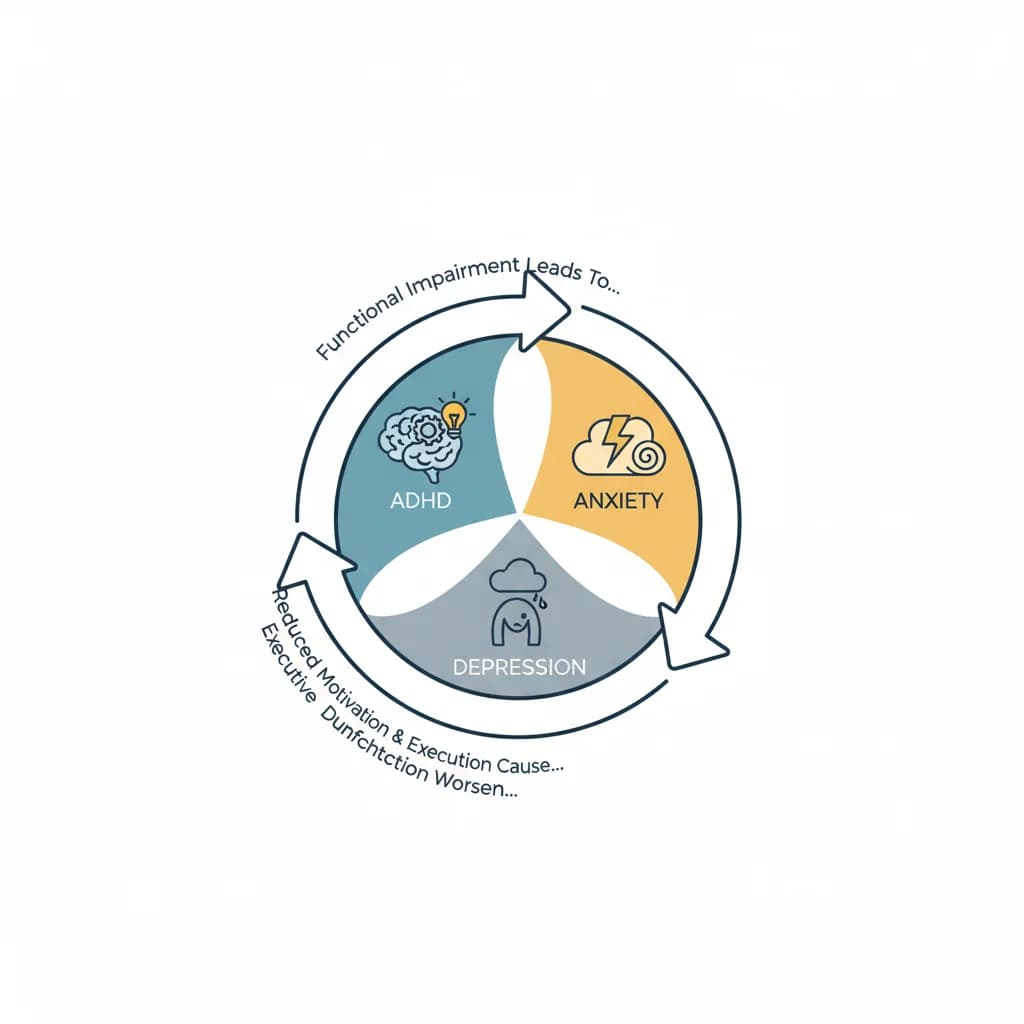
ADHD Comorbidity with Anxiety and Depression Cycles
Understanding the Complex Interplay Between ADHD and Recurring Mental Health Patterns
Disclaimer: This article is for informational purposes only and does not constitute medical advice, diagnosis, or treatment. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition. If you are in crisis or think you may have an emergency, call 988 (Suicide & Crisis Lifeline) or go to the nearest emergency room. Outside the US? Find a crisis line in your country.