Amygdala and Prefrontal Cortex Partnership in Emotional Regulation
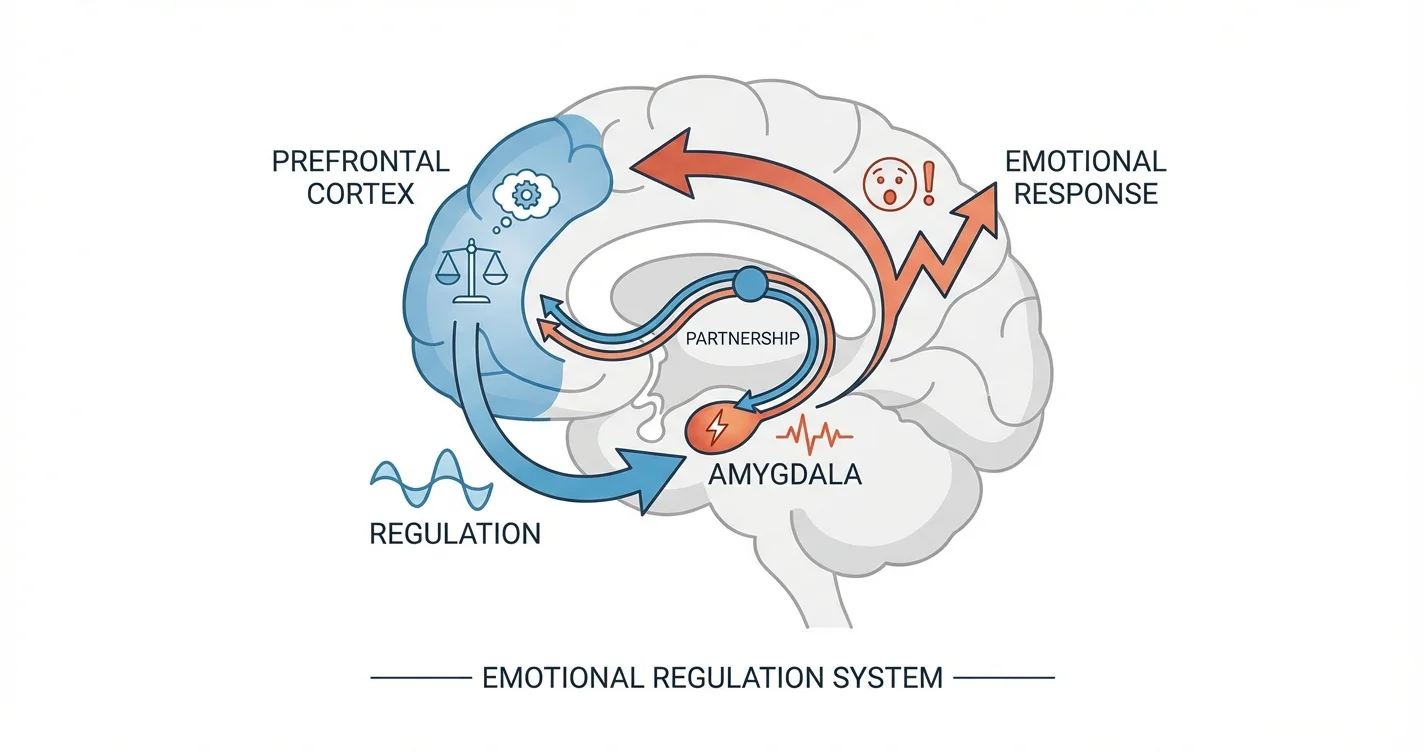
The partnership between the amygdala and prefrontal cortex represents one of the most crucial relationships in your brain's emotional processing system.

Key Takeaways
- Cognitive reappraisal: Your prefrontal cortex helps you reframe situations, finding alternative interpretations that
- Contextual assessment: It evaluates whether current circumstances truly warrant the emotional intensity your
- Inhibitory signaling: The prefrontal cortex sends signals that can reduce amygdala activation when threats are
- Decision support: It helps you choose thoughtful responses rather than acting on immediate emotional impulses
- Journaling about emotional experiences
Introduction
The partnership between the amygdala and prefrontal cortex represents one of the most crucial relationships in your brain's emotional processing system. These two regions work in constant communication to help you navigate stress, make decisions, and regulate your emotional responses to the world around you. When this partnership functions smoothly, you can process challenging emotions effectively and respond thoughtfully rather than reactively. However, when stress, trauma, or mental health conditions disrupt this connection, emotional regulation becomes significantly more difficult. Understanding how the amygdala and prefrontal cortex partnership operates can help you recognize patterns in your own emotional responses and identify strategies that may support better emotional balance.
The Core Functions of Each Brain Region
The amygdala serves as your brain's threat detection system, rapidly scanning your environment for potential dangers and triggering immediate protective responses. This almond-shaped structure processes emotional information—particularly fear, anxiety, and stress—within fractions of a second, initiating physiological changes before you consciously register what's happening. When the amygdala detects a threat, it activates your sympathetic nervous system, preparing your body for fight, flight, or freeze responses.
The prefrontal cortex, located behind your forehead, handles higher-order cognitive functions including reasoning, planning, decision-making, and impulse control. This region develops more slowly than the amygdala, with full maturation extending into the mid-twenties. The prefrontal cortex evaluates emotional responses initiated by the amygdala, providing context and applying reasoning to determine whether a threat is genuine or manageable.
Neuroimaging studies indicate that these regions are connected through neural pathways that allow bidirectional communication. The prefrontal cortex can send inhibitory signals to dampen amygdala activity when a perceived threat doesn't warrant a full stress response. This regulatory capacity is what allows you to calm yourself during stressful situations or reconsider initial emotional reactions.
How the Amygdala and Prefrontal Cortex Partnership Regulates Emotions
The relationship between these brain regions operates like a system of checks and balances. When you encounter a stressful situation—perhaps a difficult conversation or unexpected setback—your amygdala responds first, activating emotional and physiological reactions. Within moments, your prefrontal cortex assesses the situation, drawing on memory, context, and rational evaluation.
In a healthy partnership, the prefrontal cortex can modulate the amygdala's initial alarm response. Research suggests this process involves several mechanisms:
- Cognitive reappraisal: Your prefrontal cortex helps you reframe situations, finding alternative interpretations that may be less threatening
- Contextual assessment: It evaluates whether current circumstances truly warrant the emotional intensity your amygdala is generating
- Inhibitory signaling: The prefrontal cortex sends signals that can reduce amygdala activation when threats are reassessed as manageable
- Decision support: It helps you choose thoughtful responses rather than acting on immediate emotional impulses
This regulatory capacity varies considerably between individuals and across different circumstances. Chronic stress, trauma exposure, sleep deprivation, and various mental health conditions can all affect how effectively the prefrontal cortex regulates amygdala activity. When this partnership is disrupted, people may experience heightened emotional reactivity, difficulty calming down after stress, or challenges with impulse control.
The Partnership Under Stress and During Trauma
Acute stress temporarily shifts the balance of power in this partnership, often enhancing amygdala activity while reducing prefrontal cortex effectiveness. Studies indicate that stress hormones like cortisol can impair prefrontal cortex function, making it harder to think clearly or regulate emotions during highly stressful moments. This explains why you might react more intensely or make decisions you later regret when you're overwhelmed.
Chronic stress creates more lasting changes in this relationship. Prolonged exposure to stress hormones may strengthen amygdala responses while weakening prefrontal cortex connections. People experiencing chronic stress often report feeling constantly on edge, having difficulty calming down, or reacting disproportionately to minor stressors—all signs of an amygdala-prefrontal cortex partnership that's become imbalanced.
Trauma can create particularly significant disruptions to this system. When someone experiences traumatic events, the amygdala may become hypersensitive, perceiving threats in situations that others might consider safe. Meanwhile, the prefrontal cortex's regulatory capacity may be diminished, making it harder to reassess these threat perceptions rationally. This pattern contributes to symptoms commonly seen in post-traumatic stress, including hypervigilance, emotional flashbacks, and difficulty feeling safe.
However, it's important to note that multiple factors contribute to how trauma affects individuals, including genetic predispositions, previous experiences, available support systems, and individual temperament. The brain demonstrates remarkable plasticity, and targeted interventions may help restore more balanced functioning between these regions.
Supporting the Amygdala and Prefrontal Cortex Partnership in Therapy
Various therapeutic approaches specifically target this brain partnership to improve emotional regulation. These interventions work by strengthening the prefrontal cortex's regulatory capacity and reducing amygdala hyperactivity.
Cognitive-behavioral therapy (CBT) helps people identify and modify thought patterns that may unnecessarily activate the amygdala. By practicing cognitive reappraisal—examining evidence for and against anxious thoughts—clients strengthen prefrontal cortex pathways involved in emotional regulation. Over time, this practice may help the prefrontal cortex more effectively modulate amygdala responses.
Mindfulness-based interventions appear to enhance connectivity between the prefrontal cortex and amygdala. Regular mindfulness practice involves observing emotions without immediately reacting, which may strengthen the neural pathways that allow the prefrontal cortex to influence amygdala activity. Some people find that consistent mindfulness practice helps them notice emotional reactions earlier and respond more thoughtfully.
Trauma-focused therapies like EMDR (Eye Movement Desensitization and Reprocessing) and trauma-focused CBT work to process traumatic memories in ways that may reduce amygdala hyperactivity. These approaches help clients revisit difficult memories while engaging the prefrontal cortex's capacity for creating new understanding and context.
For people who find traditional talk therapy challenging, tools like Lovon.app provide on-demand support for processing emotions and working through stressors. Speaking with an AI therapist between sessions can help you practice reflecting on emotional patterns and considering different perspectives—activities that engage prefrontal cortex functions. This kind of accessible support may complement professional therapy by providing additional opportunities to practice emotional regulation skills.
Practical Strategies for Strengthening This Neural Partnership
Beyond formal therapy, several evidence-based practices may support healthier amygdala-prefrontal cortex functioning. These approaches work by either reducing unnecessary amygdala activation or strengthening prefrontal cortex regulatory capacity.
Physical exercise appears to benefit both regions. Regular physical activity is associated with reduced amygdala reactivity to stress and improved prefrontal cortex function. Even moderate exercise—such as walking, swimming, or cycling—may support this partnership when practiced consistently.
Sleep quality significantly affects this relationship. Sleep deprivation impairs prefrontal cortex function more dramatically than it affects the amygdala, creating an imbalance that often results in increased emotional reactivity. Prioritizing consistent sleep schedules and adequate sleep duration may help maintain balanced functioning between these regions.
Naming emotions—a practice sometimes called "affect labeling"—engages prefrontal cortex regions involved in language processing. Research suggests that putting feelings into words may reduce amygdala activation, which is why talking through emotions often helps people feel calmer. You might try:
- Journaling about emotional experiences
- Discussing feelings with trusted friends or therapists
- Using emotion vocabulary to describe internal experiences with specificity
- Speaking aloud about what you're feeling during stressful moments
Breathing exercises that extend your exhale relative to your inhale can activate your parasympathetic nervous system, which helps calm amygdala activation. Some people find that box breathing (four counts in, four counts hold, four counts out, four counts hold) or simply focusing on slower, deeper breaths helps them engage prefrontal cortex regulation during emotional moments.
Grounding techniques that focus attention on sensory experiences in the present moment can interrupt amygdala-driven stress spirals by redirecting prefrontal cortex attention. Describing five things you can see, four you can touch, three you can hear, two you can smell, and one you can taste is a common approach.
When Professional Support May Be Needed
While understanding the amygdala and prefrontal cortex partnership can help you recognize patterns in your emotional responses, significant difficulties with emotional regulation often benefit from professional guidance. Consider seeking support from a therapist or counselor if you notice:
- Persistent difficulty calming down after stressful events
- Emotional reactions that feel disproportionate to situations and don't improve with self-help strategies
- Intrusive memories or flashbacks that interfere with daily functioning
- Avoidance of situations or relationships due to emotional overwhelm
- Significant changes in sleep, appetite, or ability to concentrate
- Feelings of hopelessness or thoughts of self-harm
Mental health professionals can offer assessments, evidence-based treatments, and personalized strategies that address your specific patterns. For some people, medication combined with therapy may be helpful—discuss medication options with a psychiatrist or prescriber if emotional regulation difficulties are significantly affecting your quality of life.
Between therapy sessions or when immediate professional support isn't available, platforms like Lovon.app can provide additional opportunities to process emotions and work through patterns. However, these tools complement rather than replace professional treatment for serious mental health concerns.
Conclusion
The amygdala and prefrontal cortex partnership forms the foundation of your emotional regulation system, constantly communicating to help you navigate stress and respond appropriately to your environment. When this relationship functions well, you can acknowledge emotions without being overwhelmed by them and respond thoughtfully rather than reactively. Understanding how stress, trauma, and mental health conditions affect this partnership helps explain common emotional regulation challenges and points toward interventions that may help.
By recognizing when your amygdala might be overactive or your prefrontal cortex needs support, you can make informed choices about practices and treatments that may strengthen this crucial neural relationship. Whether through therapy, daily practices like mindfulness and exercise, or accessible support tools, investing in this partnership is an investment in your emotional wellbeing and capacity to handle life's inevitable challenges.
Disclaimer: This is general information, not medical advice or diagnosis. If symptoms are severe, affecting your daily life, or you're having thoughts of self-harm — seek professional help. In the US: call or text 988 (Suicide & Crisis Lifeline). For immediate danger: 911 or local emergency services.
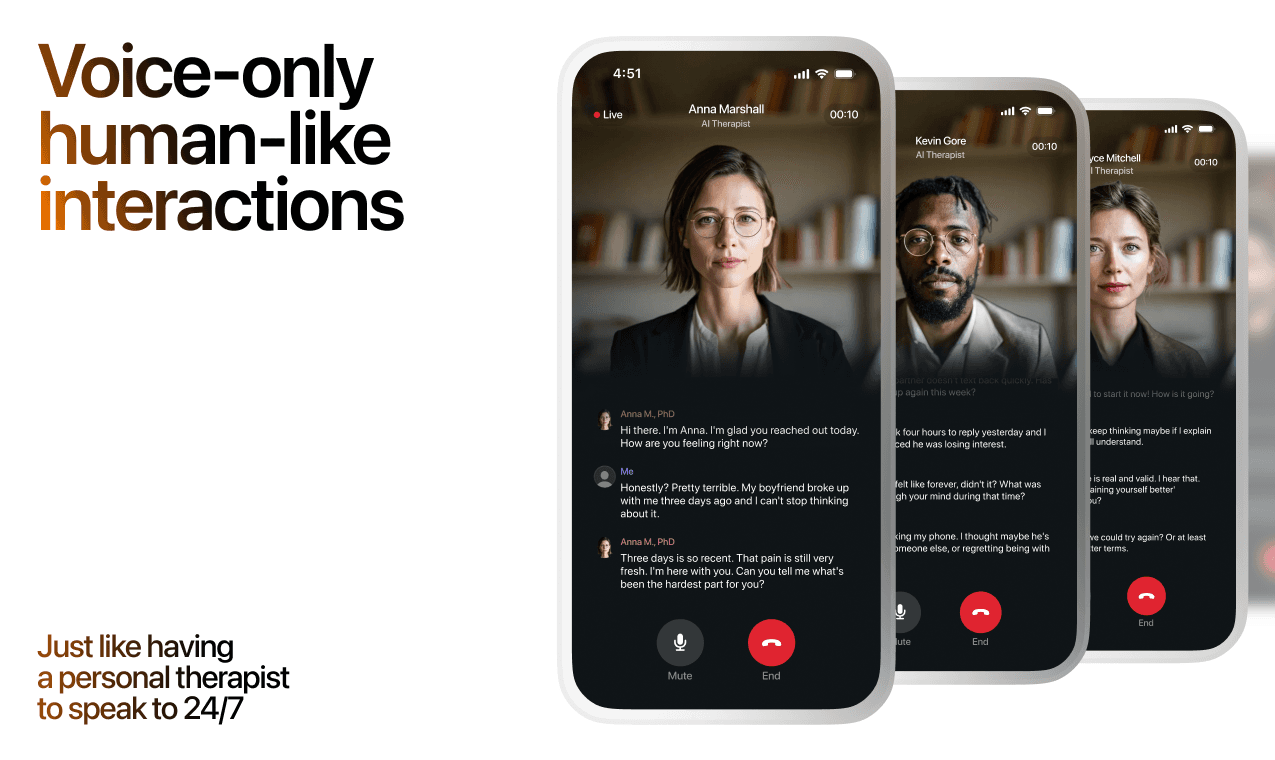
How AI Support Helps You Heal
AI emotional support isn't about replacing human connection — it's about filling the gaps. The moments when you need to talk at 2 AM, when you don't want to burden your friends again, or when you simply need someone to listen without judgment.
Here's what happens in a typical Lovon session:
You share what's on your mind
There's no script, no intake form, no waiting room. You speak or type whatever you're feeling — in your own words, at your own pace.
Lovon validates and explores
Using frameworks from CBT (Cognitive Behavioral Therapy) and motivational interviewing, Lovon acknowledges your feelings first, then gently helps you explore them. No dismissive "just move on" advice.
You build coping skills together
Lovon doesn't just listen — it actively works with you on evidence-based techniques: thought reframing, urge surfing, behavioral experiments, and more.
What a Session with Lovon Looks Like
When to Seek Professional Help
AI support is a valuable tool, but it's not a replacement for professional care. Please consider reaching out to a licensed therapist if you experience any of the following:
- Persistent thoughts of self-harm or suicide
- Inability to perform daily activities (work, eating, sleeping) for more than 2 weeks
- Turning to alcohol or substances to cope
- Intense anger or desire to harm your ex-partner
- Complete emotional numbness that doesn't improve over time
Crisis Resources (US): If you're in immediate danger, call 988 (Suicide & Crisis Lifeline) or text HOME to 741741 (Crisis Text Line). Available 24/7, free, and confidential.
Outside the US? Find a crisis line in your country
Ready to Start?
Your healing journey can begin right now
1 free conversation. No credit card. No judgment. Just a safe space to process what you're going through.
Frequently Asked Questions
Is AI therapy a replacement for a real therapist?
Is my conversation with Lovon AI private?
How is Lovon different from ChatGPT for emotional support?
Can I use Lovon if I'm already seeing a therapist?
Can I try Lovon for free?
About the Author
The Lovon Editorial Team
Mental Health & Wellness Content Team
The Lovon Editorial Team develops mental health and wellness content designed to make psychological concepts accessible and actionable. Our goal is to bridge the gap between clinical research and everyday life - helping you understand why your mind works the way it does and what you can do about it....
Similar Articles
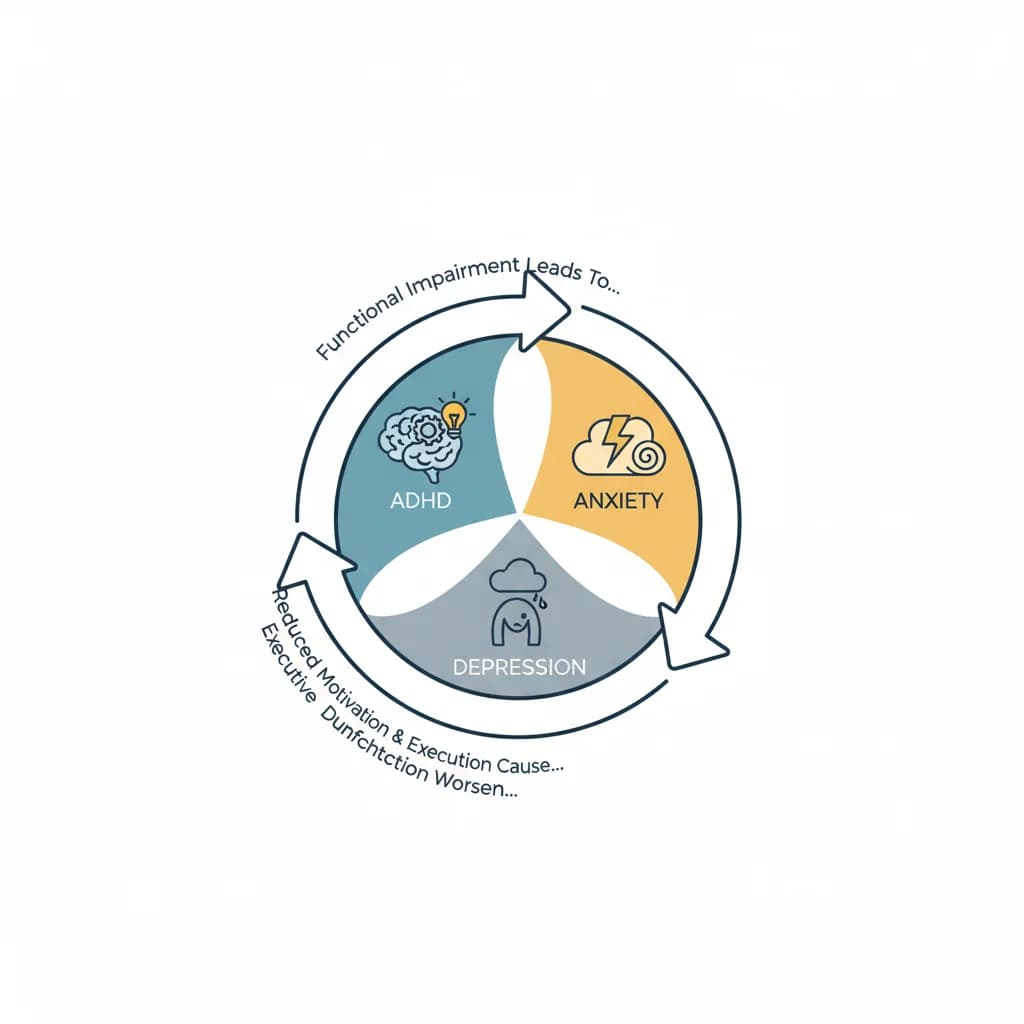
ADHD Comorbidity with Anxiety and Depression Cycles
Understanding the Complex Interplay Between ADHD and Recurring Mental Health Patterns
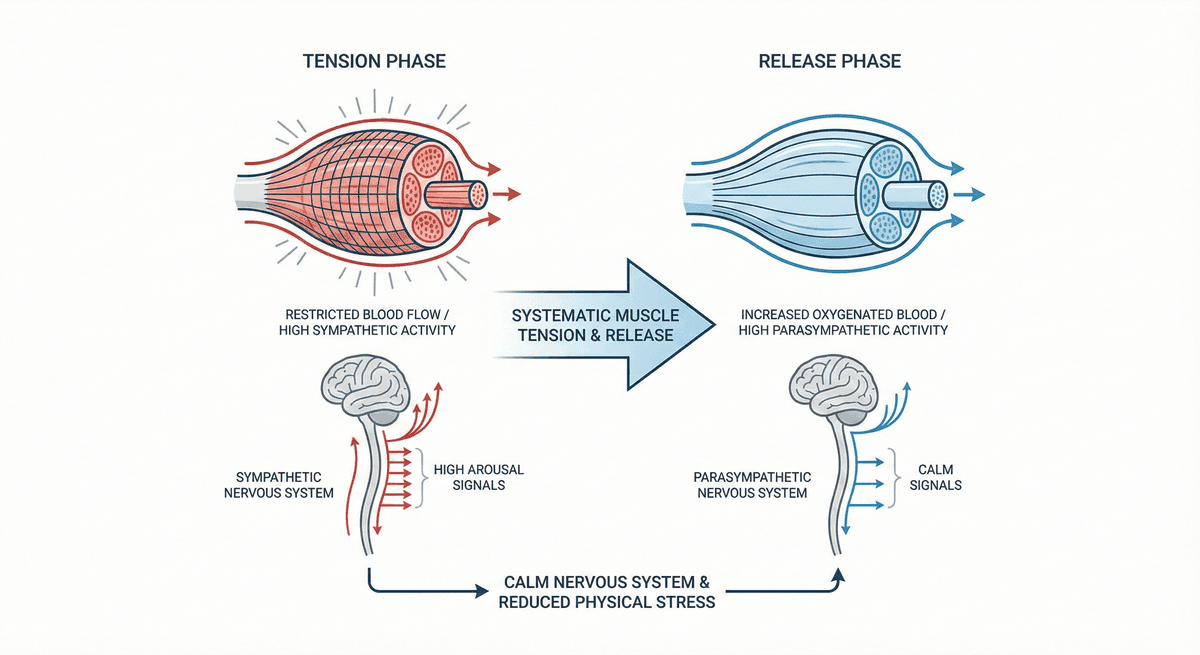
Progressive Muscle Relaxation for Stress Reduction
A systematic muscle group tension and release technique that calms the nervous system and reduces physical stress.
Amygdala and Prefrontal Cortex Connection: Training Emotional Regulation Through Mindfulness
How mindfulness practices reshape neural pathways to strengthen emotional control and reduce reactivity
Disclaimer: This article is for informational purposes only and does not constitute medical advice, diagnosis, or treatment. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition. If you are in crisis or think you may have an emergency, call 988 (Suicide & Crisis Lifeline) or go to the nearest emergency room. Outside the US? Find a crisis line in your country.