Amygdala Reactivity Reduction Through Evidence-Based Techniques
The amygdala, a small almond-shaped structure deep within the brain, acts as your neurological alarm system—constantly scanning for threats and triggering...

Key Takeaways
- Chronic stress exposure: Prolonged stress appears to sensitize the amygdala, making it respond more intensely to
- Sleep deprivation: Studies suggest that insufficient sleep is associated with increased amygdala activation and
- Early life experiences: Developmental research indicates that early relational patterns and stress exposure may
- Individual temperament and genetic factors: Some people appear to have naturally more sensitive nervous systems
- Reduced prefrontal regulation: When the connection between the prefrontal cortex and amygdala weakens, regulatory
Introduction
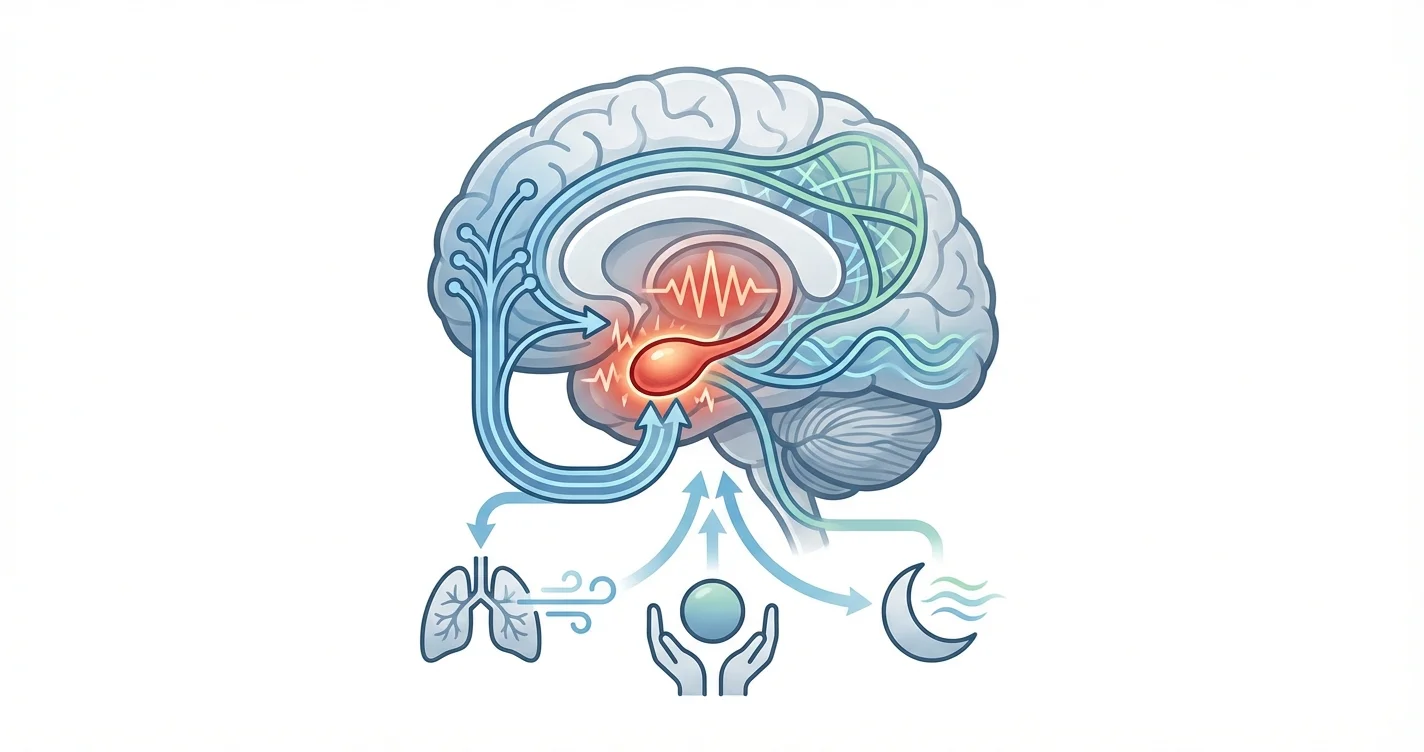
The amygdala, a small almond-shaped structure deep within the brain, acts as your neurological alarm system—constantly scanning for threats and triggering rapid emotional responses. When this threat-detection system becomes overly sensitive, you may find yourself caught in cycles of anxiety, emotional overwhelm, and stress responses that feel disproportionate to the situations you face. Amygdala reactivity reduction refers to the process of recalibrating this threat response system, helping you respond to stressors with greater emotional balance rather than automatic fight-or-flight reactions.
This heightened amygdala activity isn't a character flaw or weakness—it's a physiological pattern that develops from various factors including chronic stress, past experiences, and individual nervous system sensitivity. Understanding how to reduce amygdala reactivity involves working with your nervous system rather than against it, using techniques grounded in neuroscience research and clinical practice.
This article examines evidence-based approaches to calming amygdala reactivity, from immediate regulation strategies to longer-term brain-changing practices that build resilience over time.
Understanding Amygdala Reactivity and the Threat Response System
The amygdala processes potential threats remarkably quickly—neuroimaging studies suggest it can initiate responses within fractions of a second, often before your conscious awareness catches up. This rapid processing served our ancestors well when facing immediate physical dangers, but in modern life, this same system can misinterpret psychological stressors, social tensions, or even ambiguous situations as genuine threats.
When the amygdala detects a potential threat, it triggers a cascade of physiological changes: your heart rate increases, stress hormones like cortisol and adrenaline flood your system, and your prefrontal cortex—the region responsible for rational thinking and perspective—temporarily goes offline. Research indicates that this threat response can remain activated long after the initial trigger has passed, particularly in individuals who've experienced chronic stress or trauma.
Several factors contribute to heightened amygdala reactivity:
- Chronic stress exposure: Prolonged stress appears to sensitize the amygdala, making it respond more intensely to subsequent stressors
- Sleep deprivation: Studies suggest that insufficient sleep is associated with increased amygdala activation and decreased connectivity with regulatory brain regions
- Early life experiences: Developmental research indicates that early relational patterns and stress exposure may shape amygdala sensitivity
- Individual temperament and genetic factors: Some people appear to have naturally more sensitive nervous systems
- Reduced prefrontal regulation: When the connection between the prefrontal cortex and amygdala weakens, regulatory control decreases
Understanding these mechanisms helps remove self-blame from the equation. When you react intensely to situations others seem to handle easily, you're not being "too sensitive"—your threat detection system is operating on a different calibration, one that can be adjusted through consistent practice.
Evidence-Based Techniques for Immediate Amygdala Reactivity Reduction
When you notice your threat response activating—whether through rapid heartbeat, emotional flooding, or racing thoughts—specific techniques can help downregulate amygdala activity in the moment. These approaches work by engaging physiological and neurological pathways that signal safety to your nervous system.
Controlled breathing techniques appear to be among the most effective immediate interventions. Extended exhale breathing—where your exhale is longer than your inhale—activates the parasympathetic nervous system, which counteracts the stress response. A practical approach involves inhaling for a count of four and exhaling for a count of six to eight. The physiological shift isn't immediate but typically begins within several breathing cycles.
Bilateral stimulation involves alternating sensory input between the left and right sides of your body, which some research suggests may help process emotional activation. Simple methods include:
- Tapping alternately on your thighs or crossing your arms and tapping your shoulders
- Watching your finger move slowly left to right while keeping your head still
- Walking while paying attention to the alternating sensations in your feet
Cold exposure to the face triggers what's called the dive reflex—a physiological response that rapidly shifts your nervous system state. Research indicates this can be particularly effective during moments of intense emotional activation. Practical applications include splashing cold water on your face, holding a cold pack against your forehead and cheeks, or briefly submerging your face in cold water.
Grounding techniques redirect attention from internal threat signals to present-moment sensory information. The 5-4-3-2-1 method involves identifying five things you can see, four you can touch, three you can hear, two you can smell, and one you can taste. This process appears to help shift neural activity away from the amygdala and toward sensory processing regions.
Naming emotions—a practice sometimes called affect labeling—has been associated with reduced amygdala activation in neuroimaging studies. When you can identify and verbally label what you're feeling ("I'm noticing anxiety," "This is fear about the presentation"), it appears to engage prefrontal regions that help regulate emotional intensity.
These techniques work best when practiced regularly, not just during crises. Your nervous system learns patterns through repetition, so using these approaches during mild activation builds neural pathways that become more accessible during intense moments.
Long-Term Practices for Reducing Amygdala Reactivity
While immediate regulation techniques help in the moment, certain practices appear to create lasting changes in amygdala structure and function when practiced consistently over time. These approaches work by strengthening the regulatory connections between your prefrontal cortex and amygdala while potentially reducing baseline amygdala sensitivity.
Mindfulness meditation has been associated with structural changes in the brain, including modifications to the amygdala. Research suggests that regular mindfulness practice may reduce the volume and reactivity of the amygdala while strengthening prefrontal regulatory networks. The practice involves observing your thoughts, emotions, and sensations without immediately reacting to them—essentially training your brain to notice activation without being overwhelmed by it.
Starting a mindfulness practice doesn't require hour-long sessions. Many practitioners find that consistency matters more than duration—ten minutes daily appears more beneficial than occasional longer sessions. Focus on observing whatever arises without judgment: thoughts, emotions, physical sensations, or sounds. When you notice your mind wandering (which happens constantly), simply redirect attention back to your chosen focus point.
Physical exercise consistently shows associations with reduced anxiety and improved emotional regulation. Aerobic exercise in particular appears to influence stress hormone regulation and may promote neuroplasticity—the brain's ability to form new neural connections. Movement also provides a natural outlet for the physical energy generated by stress activation.
Therapy approaches that specifically target amygdala reactivity include trauma-focused therapies and approaches that work directly with nervous system regulation. Eye Movement Desensitization and Reprocessing (EMDR), somatic experiencing, and internal family systems therapy all address the underlying patterns that maintain heightened threat responses. For support between therapy sessions or when you need to process something that's activating your stress response, tools like Lovon.app provide on-demand access to talk through what's happening and gain perspective on your reactions.
Sleep optimization deserves special attention given its bidirectional relationship with amygdala reactivity. Poor sleep increases amygdala sensitivity, while high amygdala activation interferes with sleep quality—creating a challenging cycle. Strategies that may support better sleep include:
- Maintaining consistent sleep and wake times, including weekends
- Creating a wind-down routine that signals safety to your nervous system
- Limiting stimulating content (news, conflict, intense media) in the hours before bed
- Addressing physical comfort factors like temperature, light, and sound
- Discussing potential sleep supports with a healthcare provider if needed
Nutrition and lifestyle factors also play a role in nervous system regulation, though their effects vary considerably between individuals. Some research suggests that blood sugar fluctuations, caffeine sensitivity, and alcohol consumption may influence amygdala reactivity, though the mechanisms are complex and individual responses differ significantly.
Creating a Personalized Amygdala Reactivity Reduction Plan
Because nervous system patterns develop over time and reflect your unique biology and experiences, amygdala reactivity reduction works best when tailored to your specific patterns and circumstances. A personalized approach involves identifying your activation triggers, recognizing your early warning signs, and selecting techniques that match your situation.
Mapping your reactivity patterns provides crucial information about when and why your amygdala activates intensely. Consider tracking:
- Situations that consistently trigger strong reactions (interpersonal conflict, performance situations, uncertainty, specific types of interactions)
- Times of day when you're more vulnerable (many people experience heightened reactivity when tired, hungry, or overstimulated)
- Early physical signs that your threat response is activating (tension patterns, breathing changes, emotional shifts, thought patterns)
- Current stressors that may be sensitizing your nervous system (work demands, relationship tensions, life transitions)
Building a graduated approach helps you work with your nervous system's current capacity rather than overwhelming it. This might involve starting with situations that produce mild activation and practicing regulation techniques there before addressing more intense triggers. You're essentially training your nervous system that it can handle activation and return to baseline—a pattern that becomes stronger with repetition.
Combining immediate and long-term strategies creates both crisis support and foundational change. You might use breathing techniques and cold exposure during acute activation while building your mindfulness practice and addressing sleep patterns for longer-term shifts. When processing recurring patterns or preparing for situations you know will be challenging, resources like Lovon.app can help you understand what's happening and develop strategies tailored to your specific circumstances.
Tracking your progress helps you notice shifts that might otherwise be invisible. Because amygdala reactivity changes gradually, you might not perceive daily improvements. However, when you look back over weeks or months, you may notice that situations that previously overwhelmed you now feel more manageable, your recovery time has shortened, or the intensity of your reactions has decreased.
It's important to note that progress isn't linear. You may experience periods of increased reactivity during times of high stress, illness, or life transitions. This doesn't mean you've lost progress—your nervous system is responding to current demands. During these periods, focusing on basic nervous system support (sleep, nutrition, using your immediate regulation techniques) matters more than maintaining your full practice routine.
When Professional Support Becomes Essential
While the self-directed strategies covered in this article can support amygdala reactivity reduction, certain situations indicate that professional guidance is important. The distinction isn't about severity alone—it's about whether your current approach is producing meaningful improvements and whether your reactions are significantly impacting your daily functioning.
Consider seeking professional support when:
- Your emotional reactions consistently interfere with work, relationships, or daily responsibilities
- You experience frequent panic attacks or periods when you feel completely overwhelmed
- You have persistent thoughts of harming yourself or others
- You're using substances to manage emotional intensity
- You've experienced trauma that continues affecting your present functioning
- Self-directed techniques haven't produced noticeable improvements over several months
- Your sleep, eating, or other basic functioning has become significantly disrupted
Mental health professionals who specialize in anxiety, trauma, or nervous system regulation can provide assessment and treatment approaches specifically designed to address heightened threat responses. Depending on your situation, this might include trauma-focused therapy, cognitive-behavioral approaches, medication evaluation, or somatic therapies that work directly with nervous system patterns.
Some people benefit from a combination of professional therapy and supplementary support tools. For instance, you might work with a therapist weekly while using an on-demand resource like Lovon.app when something activating happens between sessions and you need immediate support to process it.
If you're uncertain whether professional help would be beneficial, err on the side of consultation. A brief assessment with a mental health professional can help clarify whether your current approach is sufficient or whether additional support would be helpful. Many practitioners offer initial consultations specifically for this purpose.
Conclusion
Amygdala reactivity reduction is neither a quick fix nor an impossible goal—it's a gradual process of working with your nervous system to recalibrate threat responses that no longer serve you. The techniques covered here, from immediate regulation strategies like extended exhale breathing and cold exposure to longer-term practices like mindfulness and sleep optimization, provide multiple pathways for creating change.
Your nervous system developed its current patterns over time, often for understandable reasons. Shifting these patterns requires patience, consistency, and self-compassion. Some days your threat response will activate intensely despite your best efforts, and that's part of the process rather than evidence of failure. Progress shows up in gradual changes: slightly faster recovery times, moments when you notice activation early and intervene, situations that bother you less intensely than before.
Start with one or two techniques that feel accessible given your current circumstances. Perhaps you focus on establishing a basic breathing practice and improving sleep consistency before adding additional strategies. As these become more automatic, your capacity to work with more challenging activation increases—building on itself over time.
The goal isn't eliminating all emotional reactions or never feeling threatened. Your amygdala serves important protective functions that you want to preserve. Instead, amygdala reactivity reduction means developing the capacity to respond to genuine threats while filtering out false alarms, giving you more choice in how you engage with life's inevitable challenges.
Disclaimer:
This is general information, not medical advice or diagnosis. If symptoms are severe, affecting your daily life, or you're having thoughts of self-harm—seek professional help. In the US: call or text 988 (Suicide & Crisis Lifeline). For immediate danger: 911 or local emergency services.
How AI Support Helps You Heal
AI emotional support isn't about replacing human connection — it's about filling the gaps. The moments when you need to talk at 2 AM, when you don't want to burden your friends again, or when you simply need someone to listen without judgment.
Here's what happens in a typical Lovon session:
You share what's on your mind
There's no script, no intake form, no waiting room. You speak or type whatever you're feeling — in your own words, at your own pace.
Lovon validates and explores
Using frameworks from CBT (Cognitive Behavioral Therapy) and motivational interviewing, Lovon acknowledges your feelings first, then gently helps you explore them. No dismissive "just move on" advice.
You build coping skills together
Lovon doesn't just listen — it actively works with you on evidence-based techniques: thought reframing, urge surfing, behavioral experiments, and more.
What a Session with Lovon Looks Like
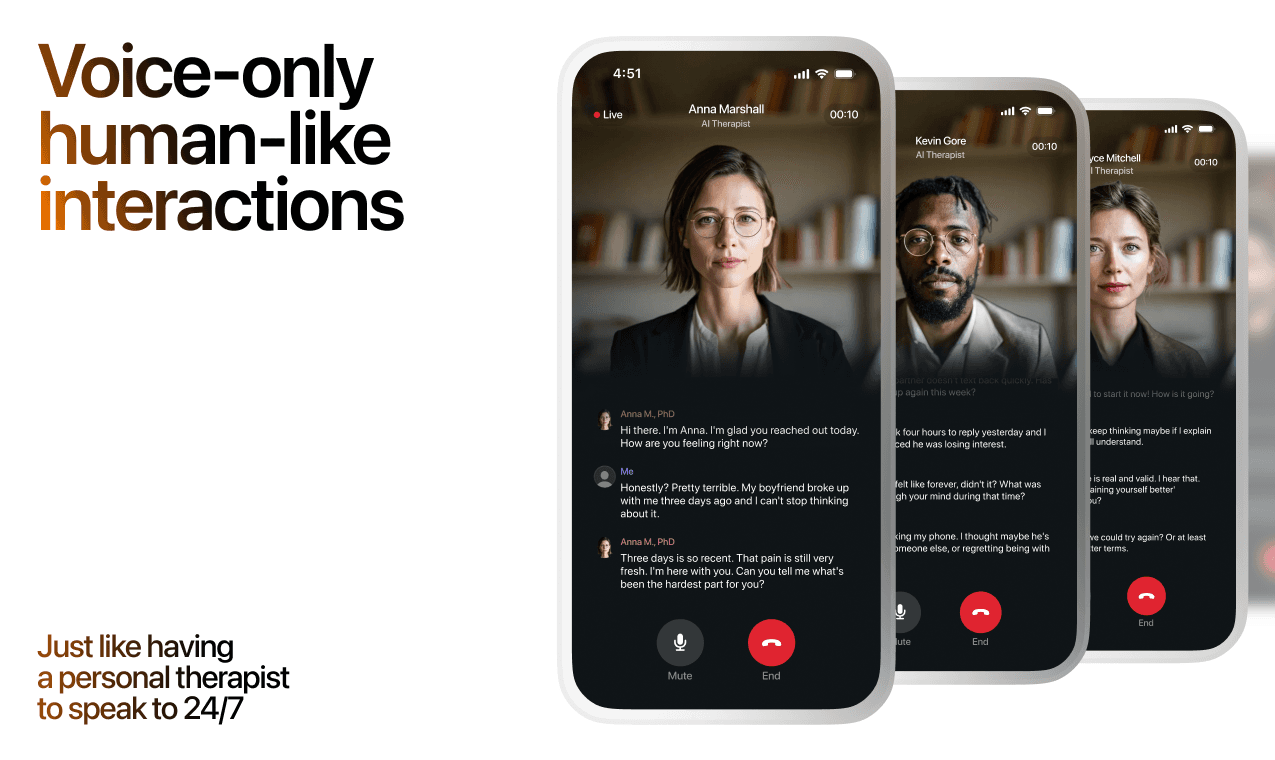
When to Seek Professional Help
AI support is a valuable tool, but it's not a replacement for professional care. Please consider reaching out to a licensed therapist if you experience any of the following:
- Persistent thoughts of self-harm or suicide
- Inability to perform daily activities (work, eating, sleeping) for more than 2 weeks
- Turning to alcohol or substances to cope
- Intense anger or desire to harm your ex-partner
- Complete emotional numbness that doesn't improve over time
Crisis Resources (US): If you're in immediate danger, call 988 (Suicide & Crisis Lifeline) or text HOME to 741741 (Crisis Text Line). Available 24/7, free, and confidential.
Outside the US? Find a crisis line in your country
Ready to Start?
Your healing journey can begin right now
1 free conversation. No credit card. No judgment. Just a safe space to process what you're going through.
Frequently Asked Questions
Is AI therapy a replacement for a real therapist?
Is my conversation with Lovon AI private?
How is Lovon different from ChatGPT for emotional support?
Can I use Lovon if I'm already seeing a therapist?
Can I try Lovon for free?
About the Author
The Lovon Editorial Team
Mental Health & Wellness Content Team
The Lovon Editorial Team develops mental health and wellness content designed to make psychological concepts accessible and actionable. Our goal is to bridge the gap between clinical research and everyday life - helping you understand why your mind works the way it does and what you can do about it....
Similar Articles
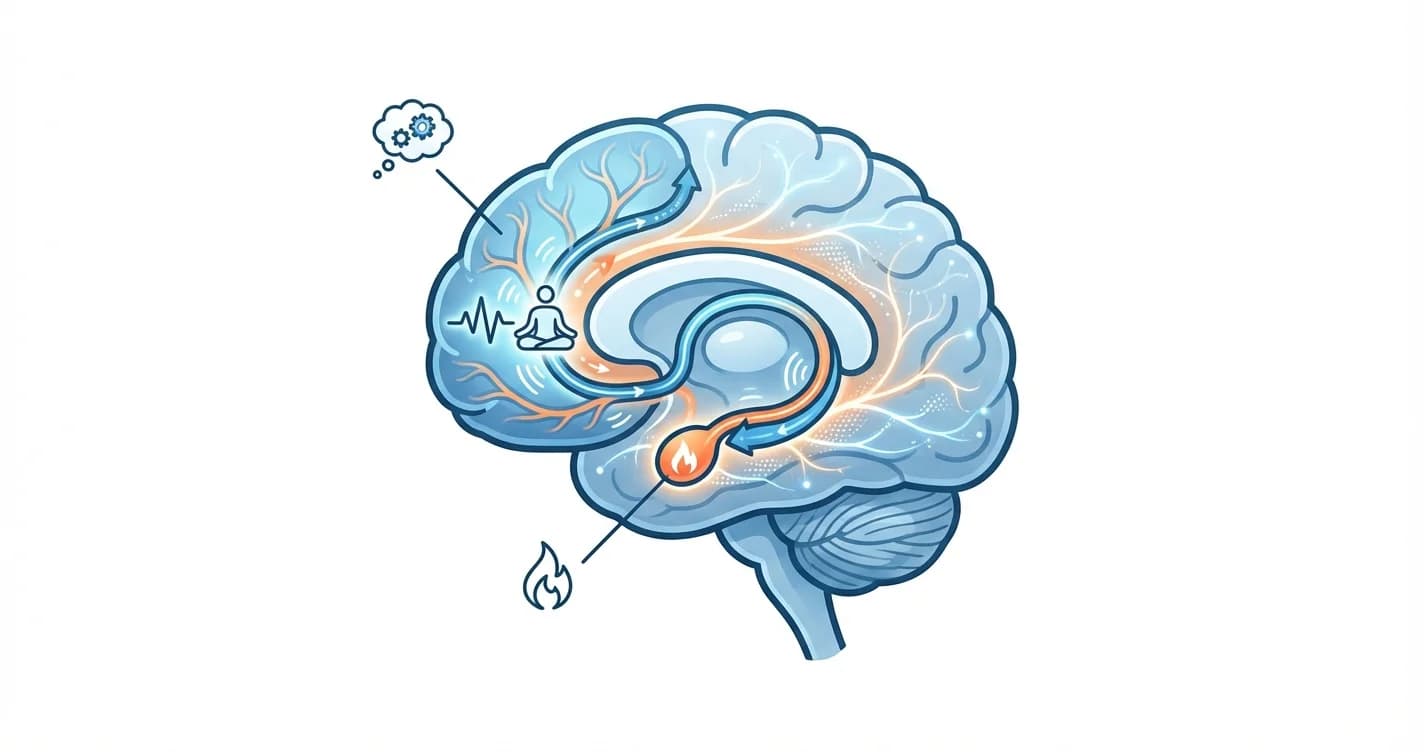
Amygdala and Prefrontal Cortex Connection: Training Emotional Regulation Through Mindfulness
How mindfulness practices reshape neural pathways to strengthen emotional control and reduce reactivity
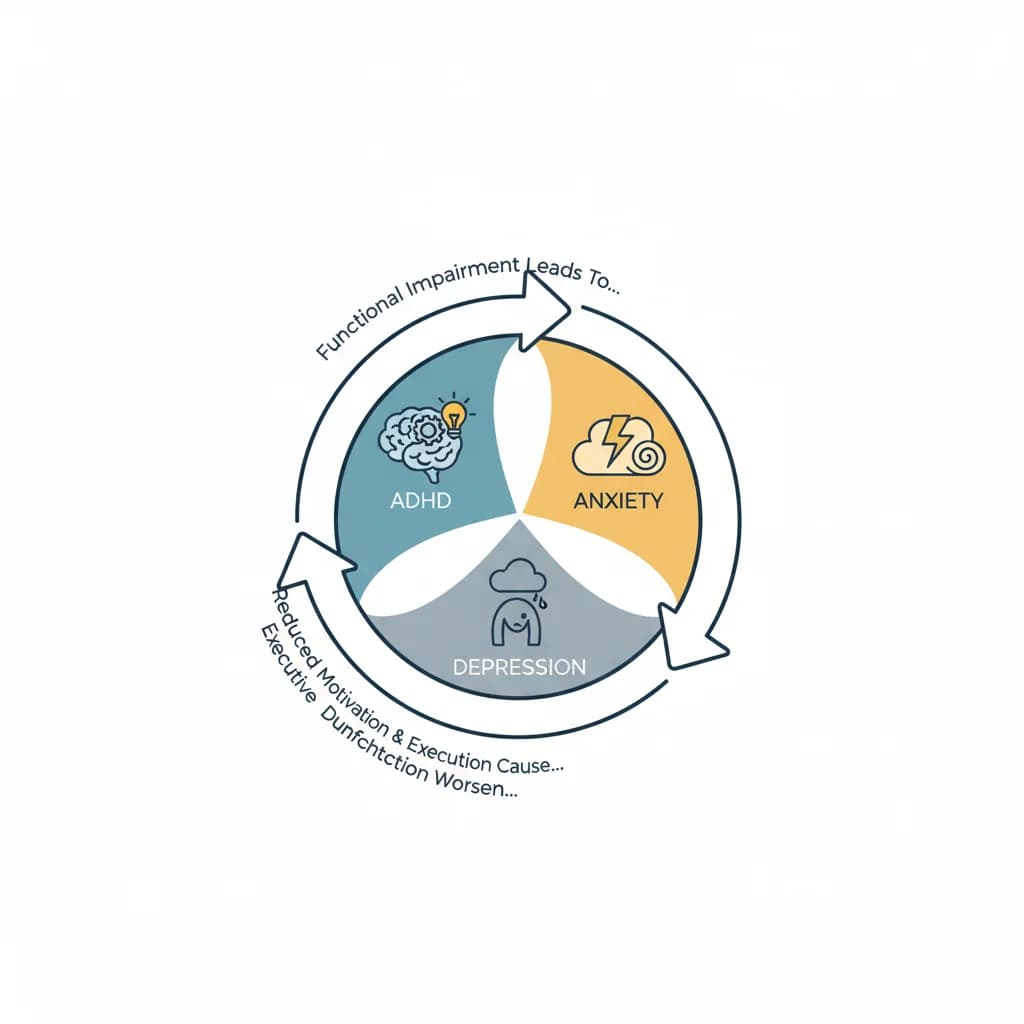
ADHD Comorbidity with Anxiety and Depression Cycles
Understanding the Complex Interplay Between ADHD and Recurring Mental Health Patterns
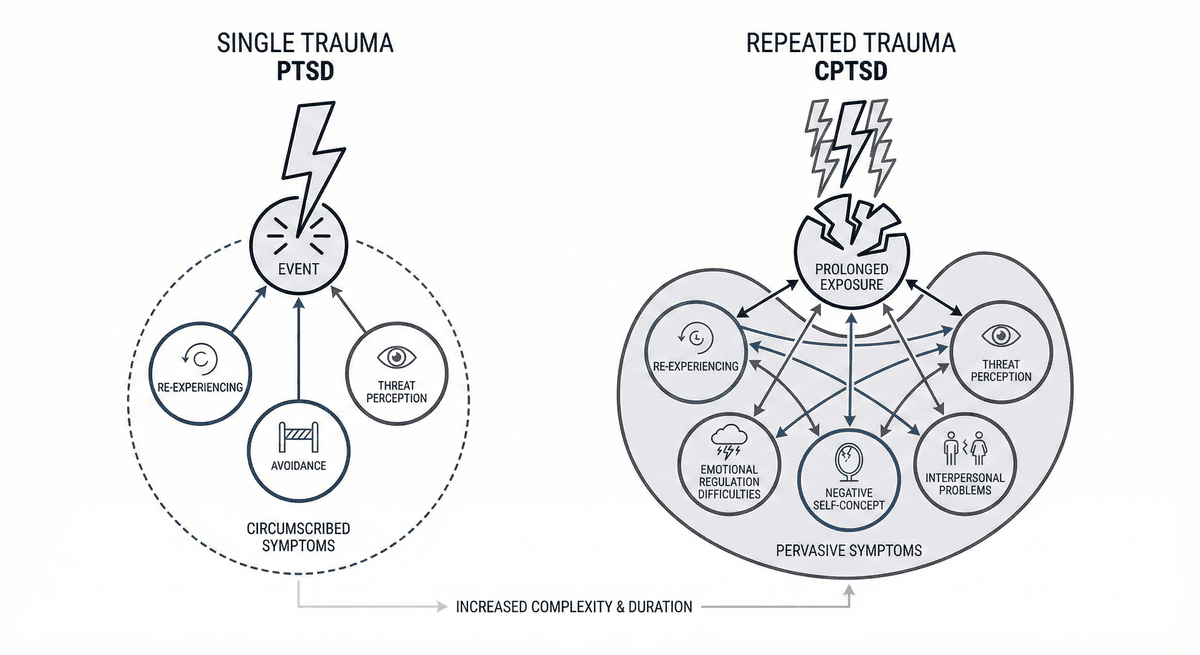
PTSD vs CPTSD: Single Trauma vs Repeated Trauma Symptom Differences
Learn how PTSD from a single traumatic event differs from CPTSD shaped by repeated trauma, including symptom patterns and treatment approaches.
Disclaimer: This article is for informational purposes only and does not constitute medical advice, diagnosis, or treatment. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition. If you are in crisis or think you may have an emergency, call 988 (Suicide & Crisis Lifeline) or go to the nearest emergency room. Outside the US? Find a crisis line in your country.