Complex PTSD: Understanding Symptoms, Causes, and Treatment
Complex PTSD (C-PTSD) represents a distinct form of trauma response that emerges from prolonged, repeated exposure to traumatic circumstances,...

Key Takeaways
- Maintaining appropriate boundaries in relationships
- Trusting others or allowing emotional closeness
- Persistent patterns of withdrawal or emotional distance
- Difficulty feeling connected even in safe relationships
- Confusion about normal relationship expectations
Complex-ptsd-understanding-treatment
Introduction
Complex PTSD (C-PTSD) represents a distinct form of trauma response that emerges from prolonged, repeated exposure to traumatic circumstances, particularly when escape feels impossible. Unlike standard PTSD, which often results from a single traumatic event, complex post-traumatic stress disorder develops through sustained trauma—such as chronic childhood abuse, domestic violence, long-term captivity, or ongoing emotional neglect. The condition affects not just how individuals process specific memories, but fundamentally shapes their sense of self, their relationships, and their capacity to regulate emotions. As mental health understanding evolves, clinicians increasingly recognize that complex PTSD requires specialized approaches that address both trauma symptoms and deeper disruptions to identity and interpersonal functioning. This article examines the distinguishing features of C-PTSD, evidence-based treatment approaches, and practical strategies for recovery based on current clinical understanding.
What Makes Complex PTSD Different
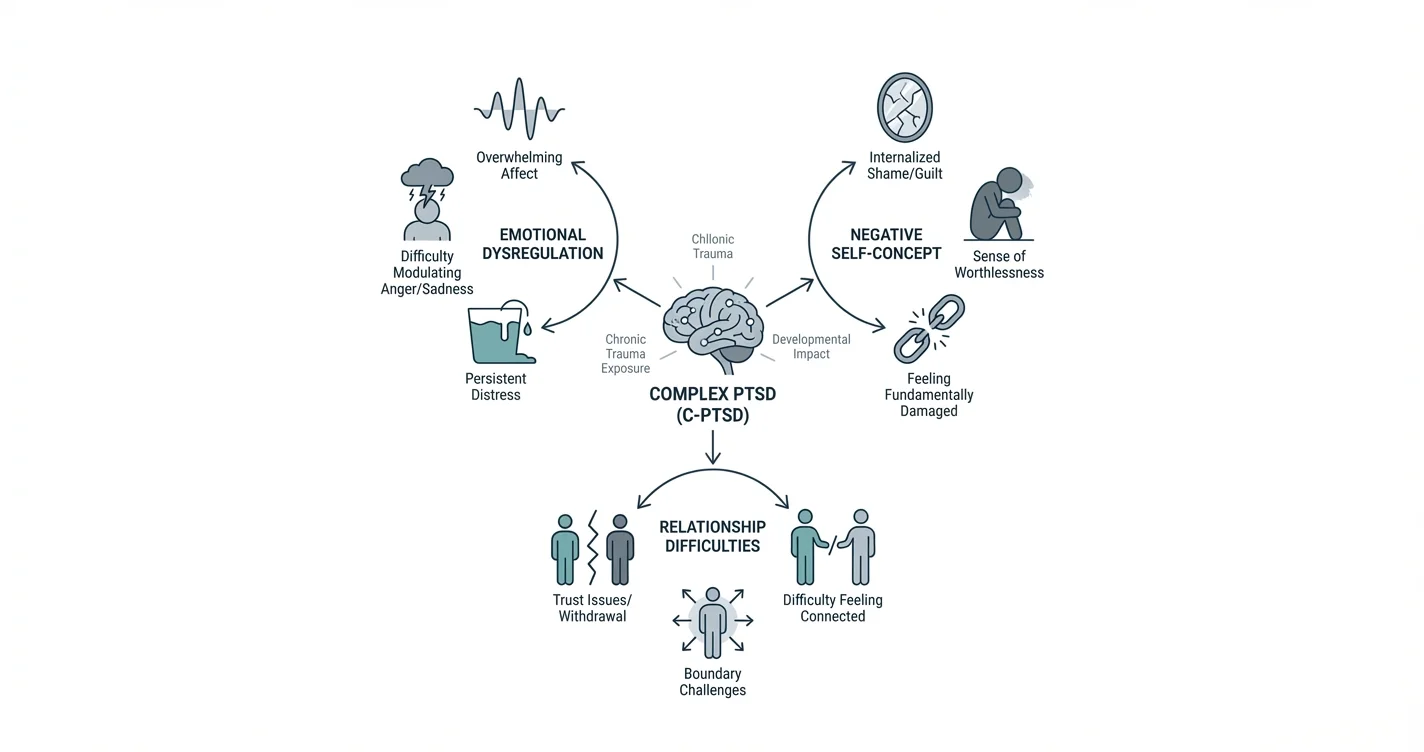
Complex post-traumatic stress disorder extends beyond the classic PTSD symptom clusters of intrusive memories, avoidance, and hyperarousal. Research suggests that C-PTSD involves three additional symptom domains that reflect the pervasive impact of sustained trauma on psychological development and functioning.
The first domain involves persistent difficulties with emotional regulation. People with complex PTSD often experience emotions as overwhelming and uncontrollable, struggling with intense anger, profound sadness, or consuming shame that feels disproportionate to present circumstances. This difficulty stems from developmental periods when the nervous system was repeatedly overwhelmed without adequate support for learning self-regulation.
The second distinguishing feature centers on negative self-concept. While standard PTSD may involve guilt about specific traumatic events, complex PTSD typically includes a deeply internalized sense of worthlessness, defectiveness, or fundamental brokenness. Clinical experience shows this isn't simply low self-esteem but a core belief about one's identity forged through relational trauma.
The third domain encompasses relationship difficulties. Individuals with C-PTSD frequently struggle with:
- Maintaining appropriate boundaries in relationships
- Trusting others or allowing emotional closeness
- Persistent patterns of withdrawal or emotional distance
- Difficulty feeling connected even in safe relationships
- Confusion about normal relationship expectations
These symptoms reflect what happens when trauma occurs within primary relationships during formative developmental periods. While genetic predispositions and individual temperament also contribute to how these patterns develop, the sustained nature of the trauma fundamentally shapes attachment systems and interpersonal expectations.
The Origins and Context of Complex PTSD
Complex post-traumatic stress disorder typically emerges from situations involving repeated trauma where the person cannot escape or feels powerless to change their circumstances. Common contexts include chronic childhood abuse or neglect, domestic violence relationships, human trafficking, prisoner-of-war experiences, or long-term situations involving coercive control.
The developmental timing of trauma significantly influences how C-PTSD manifests. When trauma occurs during childhood—particularly during critical periods of brain development and identity formation—it can disrupt fundamental capacities for self-regulation, relationship formation, and self-understanding. Early experiences play a significant role in these patterns, though genetic factors and individual temperament also contribute to how trauma affects each person.
Neuroimaging studies suggest that sustained trauma may affect brain regions involved in emotional regulation, threat detection, and self-referential processing. The stress response systems, when chronically activated during development, may become sensitized in ways that persist into adulthood. However, the brain retains considerable capacity for adaptation and healing, which forms the foundation for effective treatment approaches.
Importantly, complex PTSD can develop in anyone exposed to prolonged traumatic circumstances—it reflects the impact of overwhelming experiences, not personal weakness or inherent vulnerability. The condition represents the nervous system's adaptation to sustained threat when escape wasn't possible.
Evidence-Based Complex PTSD Treatment Approaches
Treatment for complex post-traumatic stress disorder typically requires specialized approaches that address both trauma processing and the broader impacts on emotional regulation, self-concept, and relationships. Clinical consensus suggests that effective treatment often unfolds in phases rather than following a linear protocol.
Phase-Based Treatment Framework
The first phase typically focuses on stabilization and skill-building. Before directly processing traumatic memories, individuals benefit from developing capacity for emotional regulation, distress tolerance, and recognizing present safety. This foundation proves essential because the emotional dysregulation characteristic of C-PTSD can make direct trauma work overwhelming without adequate coping resources.
During this phase, therapeutic work might include:
- Learning to identify and modulate emotional states
- Developing grounding techniques for managing flashbacks or dissociation
- Building awareness of trauma triggers and response patterns
- Establishing routines that support nervous system regulation
- Beginning to recognize the difference between past threat and present safety
The second phase involves carefully processing traumatic memories and experiences. For complex PTSD, this process often requires working through multiple traumatic experiences and addressing the relational context in which trauma occurred. Therapeutic approaches may help individuals make sense of fragmented memories, challenge distorted beliefs formed during trauma, and gradually reduce the emotional intensity attached to traumatic recollections.
The third phase emphasizes integration and rebuilding—developing a coherent sense of self beyond trauma identity, establishing meaningful relationships, and pursuing valued activities. This involves addressing the identity disruption and relationship difficulties that distinguish C-PTSD from standard PTSD.
Specialized Therapeutic Modalities
Several therapeutic approaches have shown promise for complex PTSD treatment, though research continues to evolve. Dialectical Behavior Therapy (DBT) originally developed for borderline personality disorder, offers structured skills for emotion regulation that many clinicians find valuable for the emotional dysregulation component of C-PTSD.
Eye Movement Desensitization and Reprocessing (EMDR) and trauma-focused cognitive-behavioral approaches may be adapted for complex trauma, though pacing and preparation become particularly important. Some practitioners integrate parts-work or internal family systems concepts to address the fragmentation some individuals experience.
Schema therapy specifically targets deeply held negative beliefs about self and relationships—directly addressing the negative self-concept component of complex post-traumatic stress disorder. This approach helps identify and modify patterns established during developmental trauma periods.
Practical Strategies for Managing Complex PTSD Symptoms
Between therapeutic sessions or as complement to professional treatment, various strategies may help manage the daily challenges of complex PTSD. Individual responses vary considerably, so discovering what works requires patience and experimentation.
Emotional Regulation Practices
Since emotional dysregulation represents a core challenge in C-PTSD, developing tools for managing overwhelming emotions proves essential. Some people find the following approaches helpful:
- Sensory grounding techniques that bring attention to present-moment physical experience
- Breathing exercises that engage the parasympathetic nervous system
- Physical movement that helps metabolize stress activation
- Creative expression through writing, art, or music as emotion processing
- Self-compassion practices that counter harsh self-judgment
These strategies work differently for different individuals. What grounds one person might agitate another, making personal exploration important.
Recognizing and Managing Triggers
Complex PTSD often involves heightened sensitivity to environmental or interpersonal cues that unconsciously signal danger based on past experience. Learning to recognize these triggers represents an important step toward managing responses. This might involve noticing specific situations, relationship dynamics, or sensory experiences that consistently provoke intense reactions.
When triggers occur, having a prepared response can prevent escalation. This might include removing oneself from the situation when possible, using grounding techniques, reaching out to support, or simply recognizing "this is a trauma response, not present danger."
Relationship Navigation
The relationship difficulties in complex post-traumatic stress disorder can feel particularly challenging. Some strategies that individuals find helpful include:
- Communicating needs and boundaries clearly, even when this feels uncomfortable
- Noticing patterns of relationship behavior that replicate trauma dynamics
- Gradually practicing vulnerability in safe relationships
- Seeking relationships with people who demonstrate consistent reliability
- Working with a therapist to understand how past trauma affects current relationships
Tools like Lovon.app can provide accessible support for processing relationship difficulties as they arise, offering a space to talk through conflicts or confusing interpersonal dynamics without waiting for a scheduled therapy appointment. The on-demand availability can be particularly valuable when processing emotions immediately after a triggering interaction.
Building Daily Stability
Consistent routines and self-care practices support nervous system regulation. This might include regular sleep schedules, balanced nutrition, physical activity appropriate to individual capacity, and limiting substances that affect mood or arousal states. While these fundamentals don't cure complex PTSD, they create conditions that make symptom management more manageable.
When to Seek Professional Help
Complex PTSD typically requires professional treatment to address its full scope. Self-help strategies can complement but generally don't replace specialized therapeutic support for this condition. Consider seeking professional help if you experience:
- Persistent intrusive memories, flashbacks, or nightmares related to past trauma
- Overwhelming emotions that significantly interfere with daily functioning
- Deep feelings of worthlessness, shame, or believing something is fundamentally wrong with you
- Consistent difficulties maintaining relationships or jobs
- Dissociative experiences or feeling disconnected from yourself
- Self-destructive behaviors or thoughts of self-harm
- Avoidance patterns that significantly limit your life
Mental health professionals who specialize in trauma treatment—including therapists trained in evidence-based trauma modalities, psychologists with expertise in complex PTSD, and psychiatrists who can evaluate whether medication might support your treatment—can provide comprehensive assessment and develop appropriate treatment plans.
Platforms like Lovon.app can serve as an accessible resource for processing emotions and working through immediate stressors between therapy sessions, though they complement rather than replace specialized trauma treatment for complex post-traumatic stress disorder.
The Path Forward: Recovery and Growth
Complex PTSD recovery rarely follows a linear path. Progress often involves periods of improvement interspersed with setbacks, particularly when new situations trigger old patterns. Understanding this as normal rather than evidence of failure helps maintain realistic expectations and self-compassion throughout the healing process.
Recovery from complex post-traumatic stress disorder doesn't necessarily mean eliminating all symptoms or erasing the impact of what happened. Rather, it involves developing capacity to manage symptoms, building a sense of self that extends beyond trauma identity, establishing relationships characterized by safety and reciprocity, and pursuing meaningful life activities despite the challenges trauma created.
Many individuals working through complex PTSD discover unexpected strengths—profound empathy, heightened awareness of others' suffering, resilience, and depth of character forged through navigating tremendous difficulty. While no one would choose the experiences that created C-PTSD, the process of healing can cultivate capacities that enrich life in unexpected ways.
The emerging understanding of neuroplasticity—the brain's capacity for change throughout life—offers hope that even deeply ingrained patterns established during developmental trauma can shift with appropriate support and practice. Recovery remains possible regardless of how long symptoms have persisted or how severe the original trauma.
Conclusion
Complex PTSD represents a distinct trauma response emerging from prolonged, repeated traumatic experiences that fundamentally affect emotional regulation, self-concept, and relationship capacity. Unlike standard PTSD, complex post-traumatic stress disorder requires treatment approaches that address not just traumatic memories but the pervasive developmental and relational impacts of sustained trauma. Evidence-based treatments typically follow a phased approach, beginning with stabilization and skill-building before processing traumatic material and ultimately focusing on integration and rebuilding. While professional treatment provides essential support for addressing complex PTSD, various practical strategies can help manage daily symptoms and support recovery. Understanding the specific features of C-PTSD, accessing appropriate specialized treatment, and developing personalized coping approaches offer a path toward healing that honors both the reality of trauma's impact and the genuine possibility of recovery and growth.
Disclaimer: This is general information, not medical advice or diagnosis. If symptoms are severe, affecting your daily life, or you're having thoughts of self-harm—seek professional help. In the US: call or text 988 (Suicide & Crisis Lifeline). For immediate danger: 911 or local emergency services.
How AI Support Helps You Heal
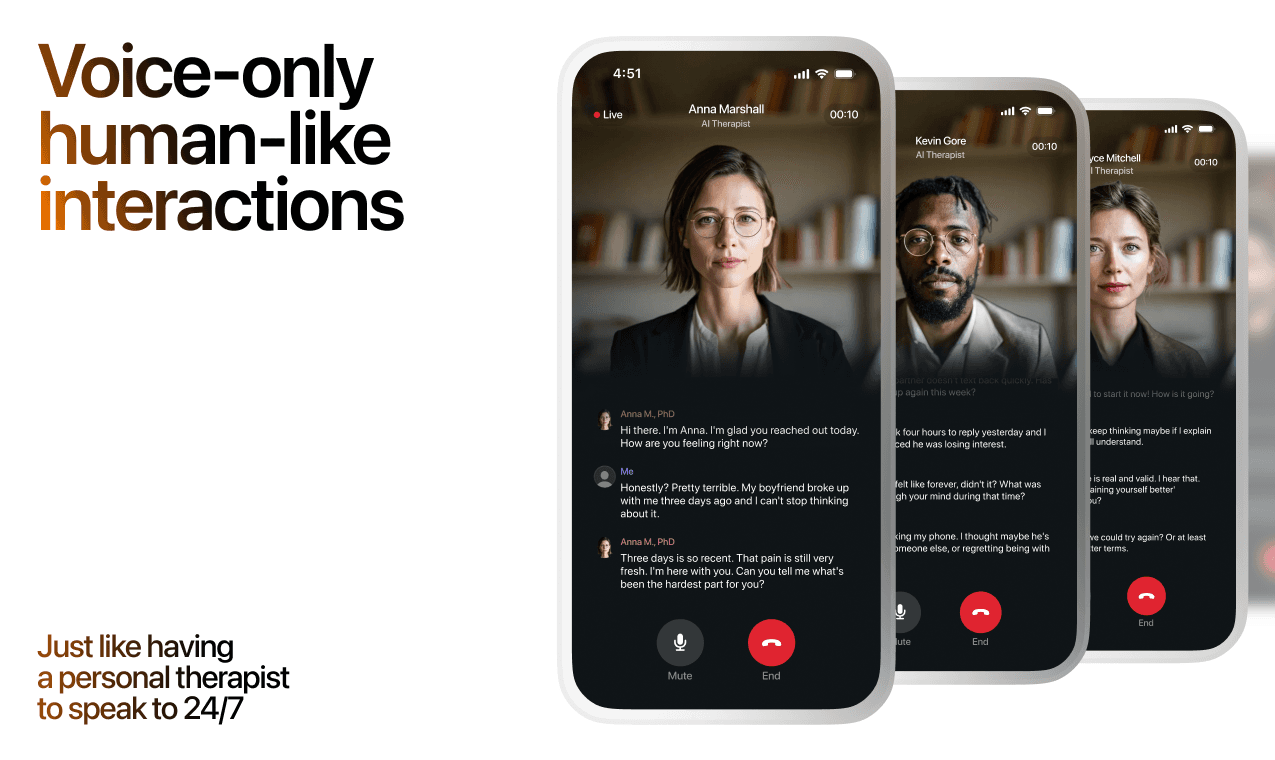
AI emotional support isn't about replacing human connection — it's about filling the gaps. The moments when you need to talk at 2 AM, when you don't want to burden your friends again, or when you simply need someone to listen without judgment.
Here's what happens in a typical Lovon session:
You share what's on your mind
There's no script, no intake form, no waiting room. You speak or type whatever you're feeling — in your own words, at your own pace.
Lovon validates and explores
Using frameworks from CBT (Cognitive Behavioral Therapy) and motivational interviewing, Lovon acknowledges your feelings first, then gently helps you explore them. No dismissive "just move on" advice.
You build coping skills together
Lovon doesn't just listen — it actively works with you on evidence-based techniques: thought reframing, urge surfing, behavioral experiments, and more.
What a Session with Lovon Looks Like
When to Seek Professional Help
AI support is a valuable tool, but it's not a replacement for professional care. Please consider reaching out to a licensed therapist if you experience any of the following:
- Persistent thoughts of self-harm or suicide
- Inability to perform daily activities (work, eating, sleeping) for more than 2 weeks
- Turning to alcohol or substances to cope
- Intense anger or desire to harm your ex-partner
- Complete emotional numbness that doesn't improve over time
Crisis Resources (US): If you're in immediate danger, call 988 (Suicide & Crisis Lifeline) or text HOME to 741741 (Crisis Text Line). Available 24/7, free, and confidential.
Outside the US? Find a crisis line in your country
Ready to Start?
Your healing journey can begin right now
1 free conversation. No credit card. No judgment. Just a safe space to process what you're going through.
Frequently Asked Questions
Is AI therapy a replacement for a real therapist?
Is my conversation with Lovon AI private?
How is Lovon different from ChatGPT for emotional support?
Can I use Lovon if I'm already seeing a therapist?
Can I try Lovon for free?
About the Author
The Lovon Editorial Team
Mental Health & Wellness Content Team
The Lovon Editorial Team develops mental health and wellness content designed to make psychological concepts accessible and actionable. Our goal is to bridge the gap between clinical research and everyday life - helping you understand why your mind works the way it does and what you can do about it....
Similar Articles
Amygdala and Prefrontal Cortex Connection: Training Emotional Regulation Through Mindfulness
How mindfulness practices reshape neural pathways to strengthen emotional control and reduce reactivity
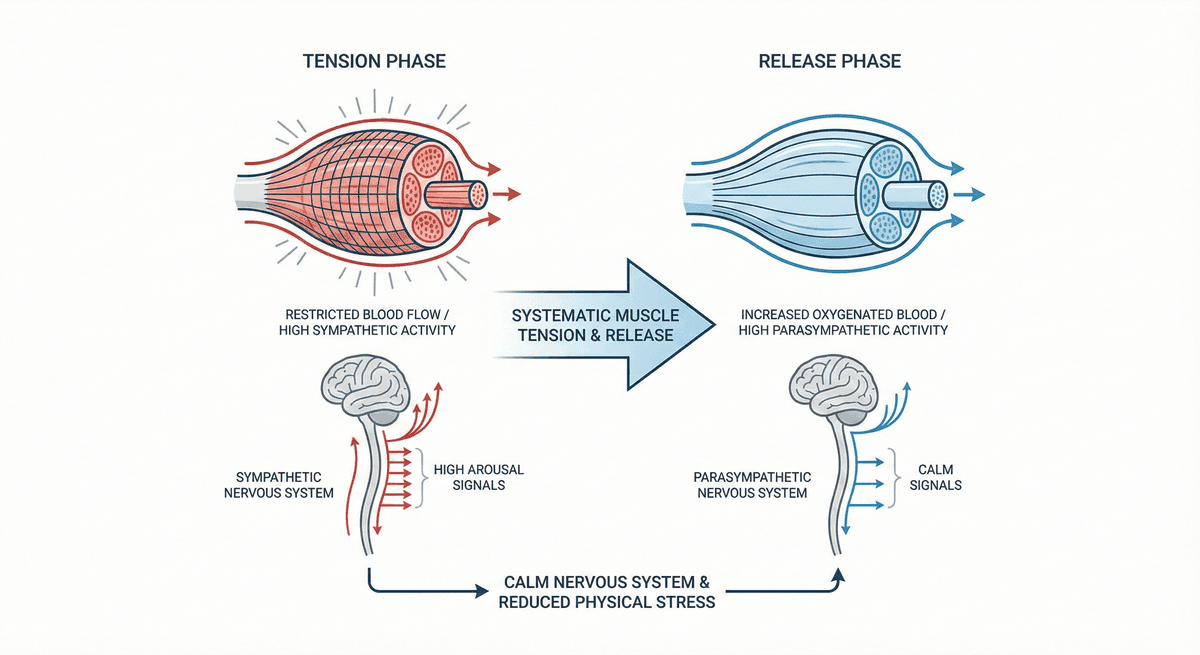
Progressive Muscle Relaxation for Stress Reduction
A systematic muscle group tension and release technique that calms the nervous system and reduces physical stress.
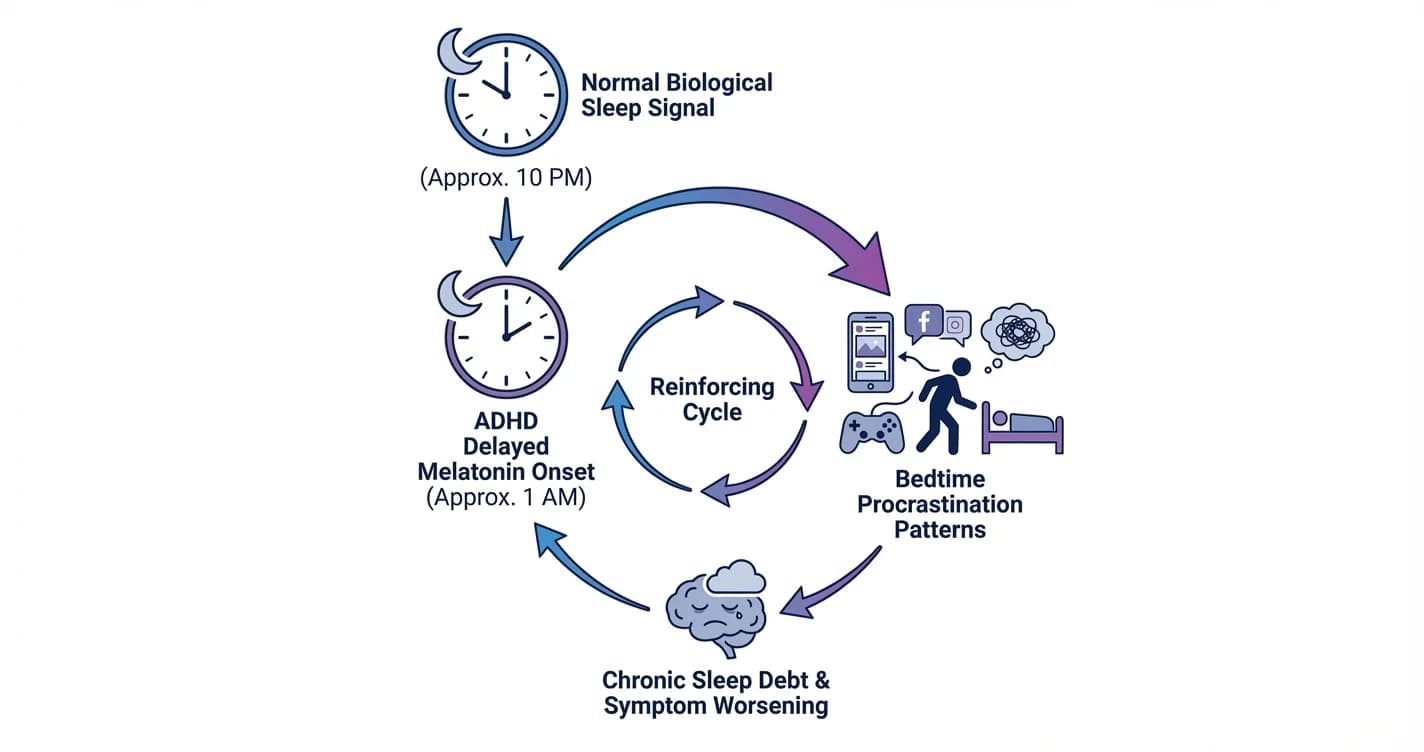
ADHD Sleep Cycle Disruption: Melatonin Delay and Bedtime Procrastination Patterns
Understanding how attention regulation difficulties interfere with natural sleep timing and the nightly wind-down process
Disclaimer: This article is for informational purposes only and does not constitute medical advice, diagnosis, or treatment. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition. If you are in crisis or think you may have an emergency, call 988 (Suicide & Crisis Lifeline) or go to the nearest emergency room. Outside the US? Find a crisis line in your country.