Defensiveness as Nervous System Threat Response
Defensiveness as Nervous System Threat Response

Key Takeaways
- Fight responses: Explaining, justifying, counterattacking, raising voice, deflecting blame
- Flight responses: Withdrawing from conversation, changing subject, leaving the room
- Freeze responses: Shutting down emotionally, going silent, mental blanking
- Fawn responses: Over-apologizing, people-pleasing, immediately agreeing to avoid conflict
- Automatic activation before conscious thought
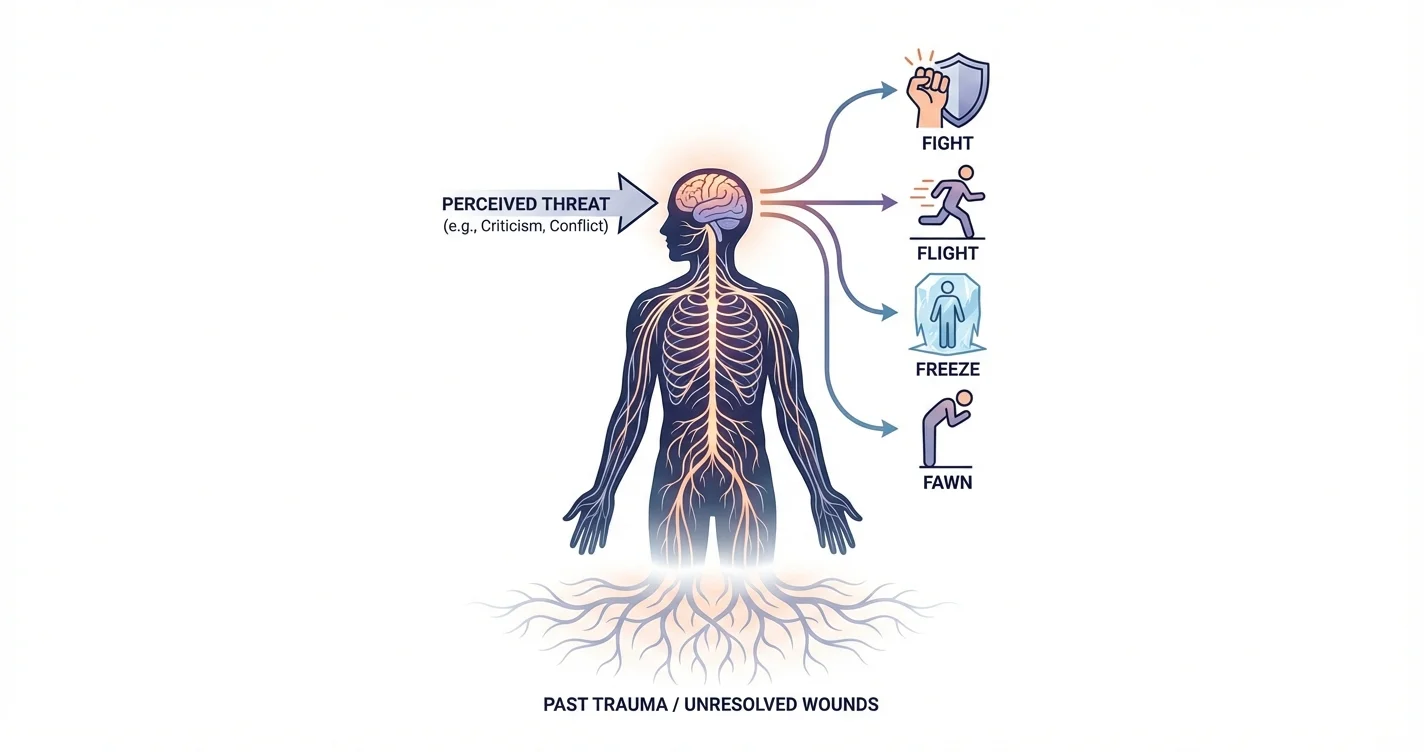
When someone offers feedback and you feel your chest tighten, your mind racing to justify yourself, or words tumbling out before you've consciously decided to speak—that's not a character flaw. Defensiveness as a nervous system threat response is an involuntary physiological reaction that occurs when your brain interprets criticism, conflict, or emotional vulnerability as danger. This automatic response happens beneath conscious awareness, engaging the same neural pathways that would activate if you faced a physical threat. Understanding this mechanism transforms how we relate to our own reactions and those of others, revealing that defensive behavior isn't about stubbornness or pride—it's about survival systems doing exactly what they're designed to do. Research in neuroscience and trauma-informed psychology increasingly shows that emotional reactions often exceed the objective severity of a situation because they're filtering present moments through accumulated past experiences. When your nervous system detects threat cues that mirror earlier wounds—abandonment, criticism, helplessness, or rejection—it responds to both the current situation and the unresolved emotional content from previous experiences simultaneously. This layering explains why a minor comment from a partner can trigger a reaction that feels completely disproportionate, or why constructive feedback at work can feel like an attack on your entire identity. Defensiveness operates through your autonomic nervous system, the part of your nervous system that regulates involuntary functions like heart rate, breathing, and stress responses. When your brain's threat-detection systems—particularly the amygdala—perceive danger, they initiate a cascade of physiological changes designed to help you survive. This happens within fractions of a second, well before your prefrontal cortex (the reasoning part of your brain) can evaluate whether the threat is actual or perceived. The body responds not to logical assessment of safety, but to perception of threat. This distinction is critical: your nervous system doesn't wait for conscious confirmation that danger is real. It operates on a "better safe than sorry" principle, activating defensive responses whenever certain patterns, tones, facial expressions, or situations resemble previous threatening experiences. This is why someone with a history of harsh criticism might react defensively to neutral feedback, while someone else might not register the same comment as threatening at all. Defensive reactions manifest along a continuum of nervous system activation states:
- Fight responses: Explaining, justifying, counterattacking, raising voice, deflecting blame
- Flight responses: Withdrawing from conversation, changing subject, leaving the room
- Freeze responses: Shutting down emotionally, going silent, mental blanking
- Fawn responses: Over-apologizing, people-pleasing, immediately agreeing to avoid conflict Each of these represents your nervous system's attempt to manage threat and return to safety. According to clinical perspectives on trauma and attachment, the specific defensive pattern you default to often reflects what worked (or seemed to work) in your earliest relationships when facing conflict or emotional intensity. The threat response that generates defensiveness involves multiple interconnected systems working in rapid coordination. When something touches a sensitive area—your competence, your worthiness, your identity, your need for connection—your brain interprets this as danger and mobilizes defensive resources. Neurologically, this process involves the amygdala detecting threat cues and signaling the hypothalamus, which activates the sympathetic nervous system. Stress hormones like adrenaline release rapidly, preparing your body for action. Your heart rate increases, blood flows to major muscle groups, and cognitive resources narrow to focus on the perceived threat. Meanwhile, activity in the prefrontal cortex—responsible for perspective-taking, nuance, and thoughtful response—decreases. This physiological shift explains why defensiveness feels so compelling in the moment but often appears irrational in hindsight. During threat activation, your nervous system prioritizes immediate survival over accurate interpretation. Subtle details, alternative perspectives, and long-term consequences become temporarily inaccessible as your system focuses exclusively on neutralizing the perceived danger right now. Key characteristics of nervous system-driven defensiveness include:
- Automatic activation before conscious thought
- Physical sensations: tension, heat, racing heart, shallow breathing
- Narrowed cognitive focus on protecting self-image or safety
- Difficulty accessing empathy or alternative perspectives during activation
- Reaction intensity that seems mismatched to the triggering event
- Pattern consistency across different situations or relationships Experts in nervous system regulation emphasize that these reactions become especially pronounced when current triggers connect to unresolved wounds from the past. Your nervous system maintains implicit memories of previous threats—times you were criticized, rejected, abandoned, or made to feel inadequate. When present situations echo these earlier experiences, your body responds to both timelines simultaneously, creating reactions that feel overwhelming because they're addressing accumulated pain, not just the immediate moment. Understanding which situations activate your defensive nervous system response requires recognizing that threat perception is deeply individualized, shaped by your attachment history, past relationships, and learned associations about safety and danger.
Attachment-Related Triggers
The nervous system stores templates from early relationships that shape how you interpret connection and conflict throughout life. These attachment patterns create specific vulnerability points where defensiveness emerges as protection against re-experiencing early relational pain. For individuals with anxious attachment patterns, defensiveness often manifests when connection feels uncertain. The nervous system reacts to perceived signs of withdrawal, disinterest, or abandonment—activating desperate attempts to prove worthiness, force reassurance, or control the other person's availability. This may look like defensively demanding explanations for delayed responses, preemptively attacking before anticipated rejection, or aggressively seeking validation. These reactions reflect a nervous system conditioned in relationships that provided inconsistent safety, where connection felt perpetually precarious. For those with avoidant attachment patterns, defensiveness activates when intimacy, emotional demands, or vulnerability threaten autonomy. The nervous system interprets emotional closeness as dangerous entrapment or loss of control, triggering withdrawal, dismissiveness, or intellectual deflection. What appears as defensive coldness or rationalization is often a nervous system strategy developed in early environments where emotional needs were dismissed or where dependency felt unsafe.
Identity and Self-Esteem Vulnerabilities
Defensiveness intensifies when feedback touches aspects of identity you're uncertain about or have been criticized for historically. If you've internalized messages about being inadequate, incompetent, or unworthy, situations that could confirm these fears activate powerful threat responses. Your nervous system mobilizes to prevent the pain of having your worst self-perceptions validated. This explains why the same feedback delivered to two different people produces dramatically different reactions. Someone secure in their competence at a particular skill might receive critical feedback with curiosity, while someone carrying shame about that same skill experiences the identical feedback as threatening attack, triggering immediate defensiveness.
Environmental and Relational Context
The state of your nervous system before an interaction significantly influences defensiveness thresholds. When you're already stressed, under-slept, hungry, or emotionally depleted, your threat detection systems become more sensitive, lowering the bar for what registers as danger. Additionally, certain relationship dynamics—power imbalances, histories of criticism, or unresolved conflicts—create contexts where your nervous system maintains heightened vigilance, ready to defend at the smallest provocation. Research on interpersonal neurobiology suggests that we continuously co-regulate nervous systems with people around us. In relationships marked by consistent safety and attunement, nervous systems remain more regulated, making defensive responses less frequent and intense. Conversely, in relationships with chronic conflict, criticism, or emotional unpredictability, nervous systems remain in protective states, generating defensiveness as a baseline stance rather than an occasional reaction. Approaching defensiveness through a nervous system lens transforms intervention from "controlling your reactions" to "creating safety conditions that allow regulation." This distinction matters because attempting to force yourself or others to "just stop being defensive" typically intensifies threat perception, escalating the very pattern you're trying to change.
Recognition and Naming
The first step in working with defensive threat responses involves developing awareness of your own activation patterns. This means learning to recognize the physical sensations, thoughts, and impulses that signal your nervous system has entered defensive mode. Common early warning signs include:
- Heat or tension in chest, throat, or shoulders
- Rapid heartbeat or shallow breathing
- Sudden urge to speak, explain, or leave
- Mental cataloging of counterarguments or justifications
- Feeling misunderstood or attacked Practitioners emphasize that noticing activation is not the same as judging it. The goal isn't to criticize yourself for having defensive reactions, but to develop the capacity to recognize when your nervous system has shifted into threat response. This recognition creates a small space between automatic reaction and chosen response—not always enough to change the pattern immediately, but sufficient to begin building different neural pathways over time.
Self-Regulation Strategies
When you notice defensive activation, interventions that signal safety to your nervous system prove more effective than cognitive strategies alone. Your body responds to physical and environmental cues of safety, gradually allowing your threat response to deactivate. Immediate regulation techniques include:
- Extending your exhale (breathing out longer than breathing in activates the parasympathetic calming response)
- Physically grounding yourself through feeling your feet on the floor or your body in the chair
- Creating brief distance from the triggering conversation (if possible) without full avoidance
- Placing hand on chest or heart, offering yourself the physical sensation of support
- Engaging peripheral vision rather than fixed focus (softening gaze reduces threat signaling) These interventions work because they directly communicate safety to the nervous system through physical sensations, bypassing cognitive processes that may be temporarily offline during activation. Tools like Lovon.app can provide a space to process defensive reactions after they occur, helping you understand what specifically felt threatening and developing compassionate awareness of your patterns without judgment.
Repairing After Defensive Reactions
Accepting that defensive threat responses will sometimes happen allows you to develop repair skills rather than pursuing the impossible goal of never being defensive. Repair involves acknowledging when you reacted from a protective state and reconnecting after your nervous system has settled. Effective repair doesn't require extensive explanation or apology, but it does require genuine acknowledgment. Simple statements like "I got defensive earlier—I'd like to hear what you were actually trying to say" or "When you brought that up, I felt attacked and shut down. Can we try that conversation again?" communicate that you recognize your defensive response and are willing to reengage from a more regulated state. This approach proves especially valuable in intimate relationships, where patterns of defensiveness create destructive cycles. When both partners understand defensiveness as nervous system threat response rather than character deficiency or deliberate obstinacy, they can develop collaborative approaches to working with these patterns rather than blaming each other for having them. While occasional defensive reactions represent normal nervous system functioning, chronic defensiveness—where threat responses dominate most interactions—signals that your nervous system remains in a persistent state of dysregulation, perceiving danger as constant rather than occasional. Addressing chronic defensiveness requires more than individual regulation techniques; it typically involves examining and healing the underlying experiences that trained your nervous system to perceive the world as persistently threatening. This often means working with patterns rooted in developmental trauma, attachment wounds, or prolonged exposure to critical, invalidating, or unsafe environments.
Therapeutic Approaches
Trauma-informed therapy modalities specifically address the nervous system patterning that creates chronic defensiveness. Approaches like Somatic Experiencing, EMDR (Eye Movement Desensitization and Reprocessing), and Internal Family Systems help process stored threat responses and update your nervous system's understanding of current safety. These approaches recognize that defensiveness protecting old wounds won't simply disappear through insight or willpower. Instead, healing requires helping your nervous system complete threat responses that were interrupted, process emotions that weren't safe to feel at the time, and gradually learn that vulnerability and feedback in present relationships don't carry the same danger they did historically. Clinical perspectives emphasize that healing begins when we listen to defensive reactions instead of judging them. Each defensive response contains information about what your nervous system perceives as threatening and what it's working to protect. Approaching these reactions with curiosity rather than shame allows you to understand the legitimate function they've served, even as you work toward developing more flexible responses.
Building Secure Relationships
The nervous system develops and heals in relationship. While individual work matters, chronic defensiveness often softens most significantly in the context of relationships that consistently demonstrate safety, attunement, and non-retaliation when you're vulnerable. This doesn't mean you need perfect relationships to heal defensive patterns—such relationships don't exist. Rather, it means cultivating relationships where repair happens consistently, where your defensive reactions don't result in abandonment or escalation, and where you gradually learn through embodied experience that expressing needs, acknowledging mistakes, and being seen in your imperfection doesn't lead to the consequences your nervous system fears. For some people, on-demand support resources like Lovon.app provide a non-judgmental space to practice articulating vulnerable feelings and examining defensive patterns without the added complexity of managing another person's nervous system simultaneously. This kind of practice can build capacity for bringing these skills into more complex relational contexts.
The Role of Self-Compassion
Working with defensive nervous system responses requires recognizing that these patterns developed for legitimate reasons—they represent your system's best attempt to keep you safe given the information and resources available at the time. While some research suggests that self-compassion practices may help reduce threat reactivity over time, it's important to acknowledge that developing self-compassion itself can feel threatening to nervous systems conditioned in critical or invalidating environments. The goal isn't to immediately feel compassionate toward yourself—that expectation can become another source of shame when defensiveness arises. Instead, it's about gradually, incrementally developing the capacity to notice defensive reactions without adding layers of self-judgment that intensify nervous system activation. Even simple acknowledgment—"I'm having a defensive reaction right now"—without immediate attempts to change or fix it can begin shifting your relationship with these patterns. While understanding defensiveness as nervous system threat response can transform your relationship with these patterns, certain situations indicate the need for professional support:
- Defensive reactions consistently damage important relationships despite your efforts to change patterns
- Chronic defensiveness prevents you from maintaining employment, friendships, or intimate partnerships
- You experience intense physical symptoms (panic attacks, rage, dissociation) when receiving feedback or experiencing conflict
- Defensive patterns are connected to trauma history that requires specialized treatment
- You feel chronically unsafe in relationships or struggle to distinguish actual threats from perceived ones
- Attempts to work with defensiveness on your own have led to increased shame, hopelessness, or self-criticism Mental health professionals specializing in trauma, attachment, and nervous system regulation—including trauma therapists, somatic therapists, and therapists trained in EMDR or Sensorimotor Psychotherapy—can provide targeted support for addressing the root patterns generating chronic defensiveness. While self-help strategies and understanding offer valuable tools, they complement rather than replace professional treatment when defensive patterns significantly impair functioning or quality of life. Understanding defensiveness as nervous system threat response fundamentally reframes these reactions from character flaws requiring elimination to protective mechanisms deserving compassionate attention. When you recognize that defensive behaviors represent your autonomic nervous system perceiving danger and mobilizing survival responses, you can approach these patterns with curiosity about what your system is working to protect rather than shame about having the reactions at all. The path forward isn't about never experiencing defensiveness—that's neither realistic nor necessary. Instead, it involves gradually expanding your window of tolerance for feedback, conflict, and vulnerability by addressing the underlying experiences that trained your nervous system to perceive these situations as threatening. This happens through combination of nervous system regulation skills, healing relationships that demonstrate consistent safety, and often professional support that addresses the roots of chronic threat perception. As you develop these capacities, defensive reactions naturally become less frequent and intense—not because you're controlling them better, but because your nervous system genuinely perceives less threat in situations that previously activated protective responses. This shift allows for the vulnerability, receptivity, and authentic connection that chronic defensiveness blocks, creating space for relationships and self-understanding that feel genuinely safe rather than perpetually threatening. Disclaimer: This is general information, not medical advice or diagnosis. If symptoms are severe, affecting your daily life, or you're having thoughts of self-harm—seek professional help. In the US: call or text 988 (Suicide & Crisis Lifeline). For immediate danger: 911 or local emergency services.
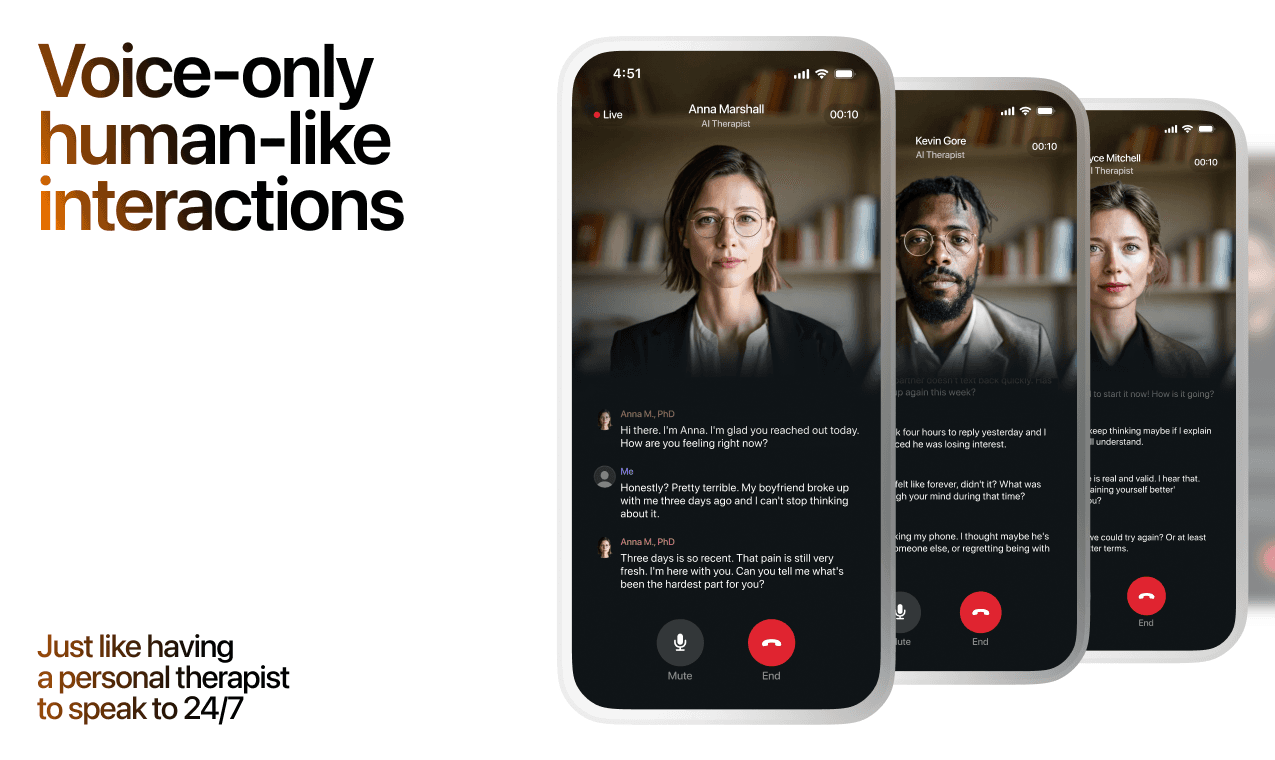
How AI Support Helps You Heal
AI emotional support isn't about replacing human connection — it's about filling the gaps. The moments when you need to talk at 2 AM, when you don't want to burden your friends again, or when you simply need someone to listen without judgment.
Here's what happens in a typical Lovon session:
You share what's on your mind
There's no script, no intake form, no waiting room. You speak or type whatever you're feeling — in your own words, at your own pace.
Lovon validates and explores
Using frameworks from CBT (Cognitive Behavioral Therapy) and motivational interviewing, Lovon acknowledges your feelings first, then gently helps you explore them. No dismissive "just move on" advice.
You build coping skills together
Lovon doesn't just listen — it actively works with you on evidence-based techniques: thought reframing, urge surfing, behavioral experiments, and more.
What a Session with Lovon Looks Like
When to Seek Professional Help
AI support is a valuable tool, but it's not a replacement for professional care. Please consider reaching out to a licensed therapist if you experience any of the following:
- Persistent thoughts of self-harm or suicide
- Inability to perform daily activities (work, eating, sleeping) for more than 2 weeks
- Turning to alcohol or substances to cope
- Intense anger or desire to harm your ex-partner
- Complete emotional numbness that doesn't improve over time
Crisis Resources (US): If you're in immediate danger, call 988 (Suicide & Crisis Lifeline) or text HOME to 741741 (Crisis Text Line). Available 24/7, free, and confidential.
Outside the US? Find a crisis line in your country
Ready to Start?
Your healing journey can begin right now
1 free conversation. No credit card. No judgment. Just a safe space to process what you're going through.
Frequently Asked Questions
Is AI therapy a replacement for a real therapist?
Is my conversation with Lovon AI private?
How is Lovon different from ChatGPT for emotional support?
Can I use Lovon if I'm already seeing a therapist?
Can I try Lovon for free?
About the Author
The Lovon Editorial Team
Mental Health & Wellness Content Team
The Lovon Editorial Team develops mental health and wellness content designed to make psychological concepts accessible and actionable. Our goal is to bridge the gap between clinical research and everyday life - helping you understand why your mind works the way it does and what you can do about it....
Similar Articles
ADHD Comorbidity with Anxiety and Depression Cycles
Understanding the Complex Interplay Between ADHD and Recurring Mental Health Patterns
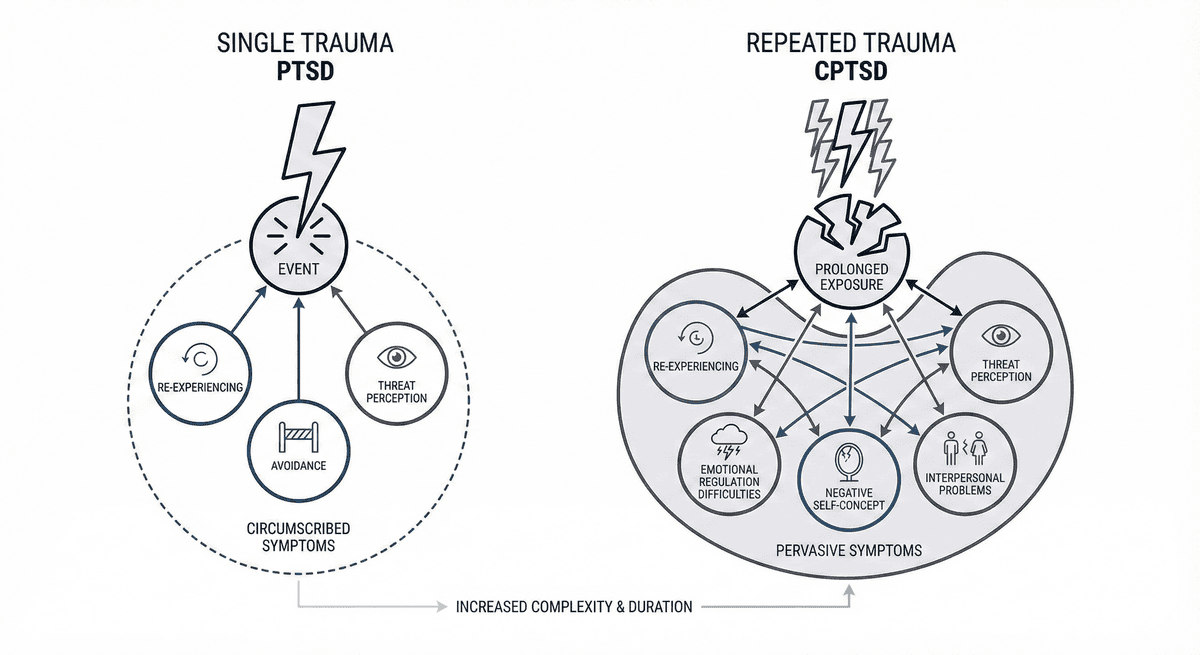
PTSD vs CPTSD: Single Trauma vs Repeated Trauma Symptom Differences
Learn how PTSD from a single traumatic event differs from CPTSD shaped by repeated trauma, including symptom patterns and treatment approaches.
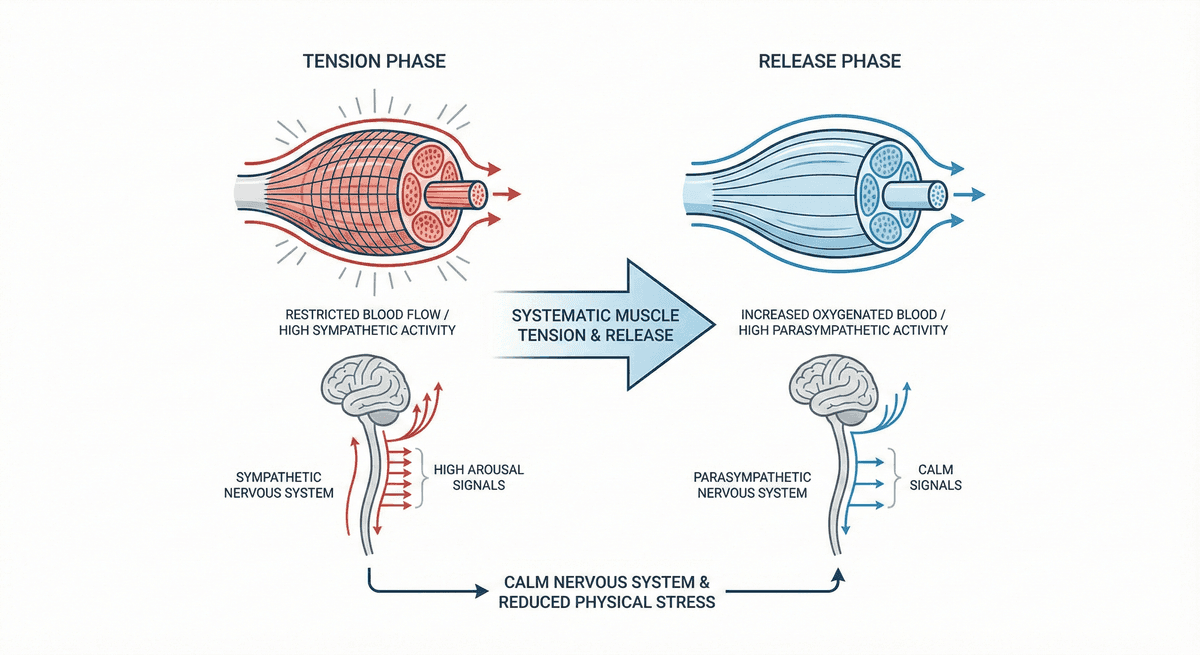
Progressive Muscle Relaxation for Stress Reduction
A systematic muscle group tension and release technique that calms the nervous system and reduces physical stress.
Disclaimer: This article is for informational purposes only and does not constitute medical advice, diagnosis, or treatment. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition. If you are in crisis or think you may have an emergency, call 988 (Suicide & Crisis Lifeline) or go to the nearest emergency room. Outside the US? Find a crisis line in your country.