How to Retrain Your Nervous System for Safety Without Performance Anxiety
Many people struggle with a nervous system that remains locked in patterns of hypervigilance, threat detection, and performance-driven anxiety—even when...

Key Takeaways
- Intentional contact with physical surfaces—noticing the chair supporting you, your feet on the ground, the texture
- Orienting to your actual environment by slowly looking around and naming what you see, allowing your eyes to rest on
- Tracking sensations of temperature, weight, and pressure in your body without trying to change them
- Starting point: Bottom-up (body to mind) rather than top-down (mind to body)
- Primary focus: Building capacity for regulation rather than managing symptoms
Introduction
Many people struggle with a nervous system that remains locked in patterns of hypervigilance, threat detection, and performance-driven anxiety—even when they're objectively safe. Learning how to retrain your nervous system for safety without performance anxiety involves understanding how your body processes threat, building new patterns of regulation, and creating authentic safety signals rather than forcing yourself to "perform" calm. This guide draws on contemporary somatic therapy principles, attachment research, and trauma-informed approaches to help you rewire automatic stress responses. Unlike traditional anxiety treatment that often focuses on symptom management, nervous system retraining addresses the underlying physiological patterns that generate anxiety in the first place.
The difference between genuine safety and performed safety matters profoundly: when you try to convince your nervous system you're safe through willpower or positive thinking alone, you often create additional stress. Effective nervous system regulation requires working with your body's signals rather than overriding them.
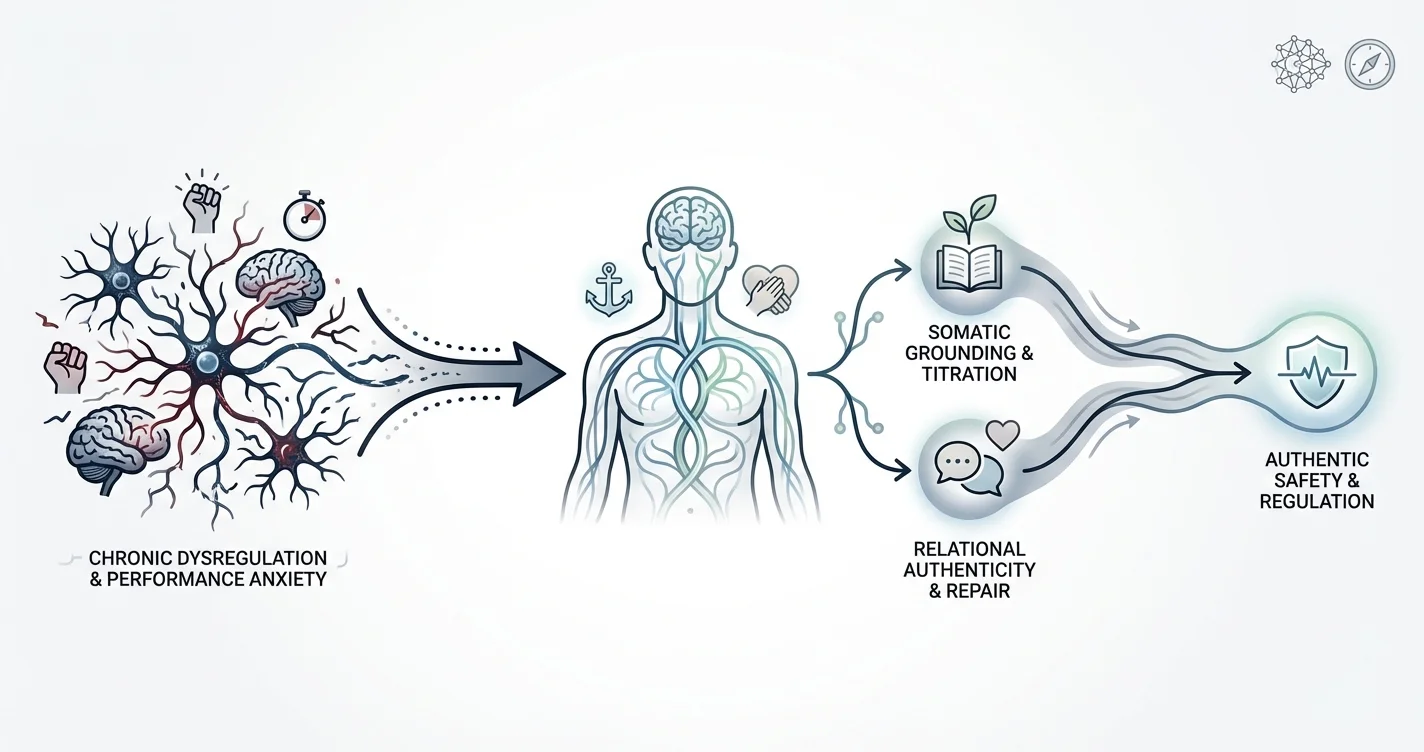
Understanding Nervous System Dysregulation and Safety Detection
Your nervous system constantly scans your environment for signals of safety or threat through a process neuroscientists describe as neuroception—an unconscious detection system that operates before conscious awareness. When this system becomes calibrated to detect threat even in safe situations, you experience chronic activation: elevated heart rate, muscle tension, racing thoughts, and the feeling of waiting for something bad to happen.
Research in polyvagal theory suggests that the nervous system has multiple defensive states beyond simple "fight or flight." When the sympathetic nervous system activates repeatedly without resolution, it can create patterns where your body interprets normal situations—a work presentation, a difficult conversation, even moments of rest—as threats requiring performance or vigilance.
For many adults, particularly those who experienced parentification or emotional role reversal in childhood, the nervous system learned early that safety required constant monitoring of others' emotional states and performing competence beyond developmental capacity. When children are asked to be the "mature one" or take emotional responsibility for adults, they develop nervous systems calibrated to performance rather than authentic connection. This creates a paradox: the harder you try to appear calm and capable, the more your body registers the effort as stress.
Understanding this distinction helps explain why traditional "just relax" advice often fails—it asks you to perform relaxation, which activates the same performance anxiety patterns you're trying to escape.
Somatic Therapy Techniques for Nervous System Safety
Effective nervous system retraining works through the body rather than bypassing it. Somatic approaches recognize that safety must be experienced physiologically, not just understood intellectually.
Grounding and Present-Moment Orientation
Practitioners recommend starting with simple sensory grounding that helps your nervous system register present safety. This involves:
- Intentional contact with physical surfaces—noticing the chair supporting you, your feet on the ground, the texture of objects you're touching
- Orienting to your actual environment by slowly looking around and naming what you see, allowing your eyes to rest on neutral or pleasant objects
- Tracking sensations of temperature, weight, and pressure in your body without trying to change them
These practices work because threat responses orient you toward potential danger (scanning, hypervigilance), while safety responses allow relaxed awareness of your actual surroundings. The goal isn't to force calm but to give your nervous system accurate information about current reality.
Pendulation Between Activation and Settling
Rather than trying to eliminate activation entirely, effective somatic work involves gentle movement between states. You might notice a moment of tension or anxiety, acknowledge it without judgment, then intentionally notice something that feels neutral or easier in your body—perhaps your breath moving naturally, or the lack of tension in one hand compared to a tight shoulder.
This pendulation trains your nervous system that activation doesn't have to spiral, and that settling is possible even when activation is present. Over time, this builds capacity for regulation rather than suppression.
Titration of Challenging Material
When working with nervous system patterns connected to past experiences, trauma-informed approaches emphasize titration—working with small, manageable amounts of activation rather than overwhelming your system. Tools like Lovon.app can support this process by providing on-demand space to process emotional activation as it arises, helping you stay within what's called your "window of tolerance" where learning and integration can occur.
Building Authentic Safety Through Relational Honesty
One of the most powerful ways to retrain your nervous system for safety involves shifting how you show up in relationships—moving from performance and people-pleasing toward what practitioners call authentic presence.
Many people develop patterns of what's termed self-abandonment: shrinking their needs, hiding their feelings, and performing agreeability to keep relationships feeling stable. While this strategy may have provided survival safety in childhood or previous relationships, it paradoxically signals danger to your nervous system. When you consistently hide your internal experience, your body registers the disconnection between inner truth and outer presentation as a threat.
Authenticity as a Safety Signal
Relationship experts working with attachment and nervous system regulation emphasize that authenticity—being honest about your feelings even when uncomfortable—actually signals safety to your nervous system. When you can express that you're upset, uncertain, or need something, and the relationship continues, your body receives evidence that connection can withstand honesty.
This doesn't mean unloading every feeling without consideration, but rather practicing what one practitioner describes as "you don't have to guess what's going on inside of me." This transparency reduces the cognitive and emotional load of performance, allowing your nervous system to settle.
Permission Over Confidence
An important reframe in this work involves recognizing that self-love in relationships functions more as permission than confidence. Rather than building yourself up to feel worthy of taking up space, you simply give yourself permission to exist as you are—anxious, uncertain, imperfect—within the relationship. This subtle shift reduces performance pressure significantly.
The Role of Repair
For trauma survivors and those with developmental experiences of inconsistent caregiving, witnessing and experiencing repair—the return and restoration of connection after conflict or rupture—provides powerful nervous system retraining. When disagreements happen and both people come back to address what occurred, acknowledge impact, and restore connection, it teaches your body that conflict doesn't mean permanent abandonment.
Practitioners emphasize that repair matters more than perfection. You don't need flawless regulation or to never feel anxious; you need the experience that ruptures can be addressed and relationship can be restored. This builds secure attachment patterns that support nervous system regulation.
Step-by-Step Guide to Nervous System Retraining for Trauma Survivors
Implementing nervous system retraining as a trauma survivor requires specific attention to pacing and safety-building. The following approach integrates somatic, relational, and cognitive elements:
Step 1: Establish External Safety and Routine
Before deep nervous system work, establish as much external predictability as possible. This might include consistent sleep and wake times, regular meals, and identifying actual safe spaces and relationships. Your nervous system regulates more easily when external conditions are genuinely more predictable.
Step 2: Develop Sensation Awareness Without Judgment
Practice noticing body sensations—tension, temperature, pressure, movement—without immediately trying to change them. Start with 2-3 minutes daily, simply observing and naming what you notice. This builds what's called interoceptive awareness, helping you distinguish between actual threat responses and habitual patterns.
Step 3: Identify Your Window of Tolerance
Notice what level and type of activation you can experience while still maintaining some sense of choice and presence. When you move outside this window into hyperarousal (panic, rage) or hypoarousal (shutdown, dissociation), your nervous system is in a defensive state where retraining is difficult. Learning to recognize your edges helps you work skillfully with activation.
Step 4: Practice Co-Regulation
Identify relationships or resources that help your nervous system settle. This might include specific people, animals, nature settings, or supportive tools like therapy or on-demand resources such as Lovon.app. Co-regulation—the experience of your nervous system settling in the presence of another regulated system—is a fundamental building block of safety.
Step 5: Experiment With Small Authenticity
In relationships that feel relatively safe, practice small moments of honesty about your internal experience. This might sound like "I'm feeling a bit overwhelmed and need a few minutes" or "I'm uncertain about this and need to think." Notice what happens in your body when you express rather than hide your state.
Step 6: Build Capacity Through Gentle Challenge
Once you have some baseline regulation skills, gradually expose yourself to situations that typically trigger performance anxiety, but with support and resources in place. The goal isn't to eliminate the anxiety response but to practice staying somewhat present and resourced while it occurs, teaching your nervous system that activation doesn't equal danger.
Step 7: Integrate and Reflect
Regularly reflect on what you're noticing—what helps your system settle, what triggers activation, what patterns are shifting. This metacognitive awareness helps consolidate learning and allows you to adjust your approach based on what actually works for your unique nervous system.
Nervous System Regulation Therapy Versus Traditional Anxiety Treatment
Understanding the differences between nervous system-focused approaches and traditional anxiety treatment helps clarify why retraining work may feel different from other interventions you've tried.
Traditional cognitive-behavioral approaches to anxiety often focus on identifying and challenging anxious thoughts, gradually exposing yourself to feared situations, and developing coping strategies to manage symptoms. These approaches can be highly effective, particularly for specific phobias and certain anxiety disorders.
Nervous system regulation therapy, however, starts from a different premise: that anxiety symptoms emerge from a nervous system calibrated to detect threat even in safe situations. Rather than primarily working with thoughts or behaviors, this approach addresses the underlying physiological patterns.
Key differences include:
- Starting point: Bottom-up (body to mind) rather than top-down (mind to body)
- Primary focus: Building capacity for regulation rather than managing symptoms
- Relationship to activation: Working with the nervous system's protective responses rather than trying to eliminate them
- Role of past experience: Explicitly addressing how developmental and traumatic experiences shaped current nervous system patterns
- Definition of success: Increased flexibility and range of regulation rather than absence of anxiety
For many people, an integrated approach works best—using cognitive tools to work with unhelpful thought patterns while simultaneously retraining the underlying nervous system responses that generate those thoughts in the first place.
It's important to note that nervous system retraining isn't a quick fix and may not be appropriate as a sole intervention for all anxiety presentations. Some people benefit most from medication support, structured therapy, or addressing specific life circumstances contributing to stress before deep nervous system work becomes possible.
When to Seek Professional Help
While the techniques described here can support nervous system regulation, certain situations warrant professional support. Consider seeking help from a trauma-informed therapist, somatic experiencing practitioner, or other mental health professional specializing in nervous system work if you experience:
- Frequent dissociation, numbness, or feeling disconnected from your body
- Intrusive memories, flashbacks, or nightmares related to past trauma
- Severe panic attacks that significantly limit your daily functioning
- Self-harm urges or thoughts of suicide
- Inability to function in important life areas (work, relationships, self-care) due to anxiety or dysregulation
- Substance use to manage overwhelming emotions or nervous system activation
Professional support is particularly important for complex trauma survivors, as deep nervous system work can sometimes activate defensive responses that are difficult to navigate alone. A skilled practitioner can help you work at an appropriate pace and provide co-regulation when your own system becomes overwhelmed.
Look for therapists trained in modalities such as Somatic Experiencing, Sensorimotor Psychotherapy, EMDR, or other body-based trauma approaches. These practitioners understand how to work with nervous system activation in ways that build capacity rather than re-traumatize.
Conclusion
Learning how to retrain your nervous system for safety without performance anxiety is a gradual process of building new physiological patterns, practicing authentic presence in relationships, and developing the capacity to stay present with activation rather than either performing calm or becoming overwhelmed. The most effective approaches combine somatic awareness practices, relational honesty, and trauma-informed pacing that respects your nervous system's current capacity.
Remember that genuine safety feels different from performed safety—it involves settling and presence rather than effortful control. By working with your body's signals rather than overriding them, practicing small moments of authenticity, and allowing for repair when ruptures occur, you create the conditions for your nervous system to recalibrate toward safety and connection.
Start with small, consistent practices rather than trying to overhaul everything at once. Notice what actually helps your system settle rather than what you think should work. And consider both self-directed practices and professional support as you build new patterns of regulation that allow you to show up more fully in your life without the constant pressure to perform invulnerability.
Disclaimer:
This is general information, not medical advice or diagnosis. If symptoms are severe, affecting your daily life, or you're having thoughts of self-harm — seek professional help. In the US: call or text 988 (Suicide & Crisis Lifeline). For immediate danger: 911 or local emergency services.
How AI Support Helps You Heal
AI emotional support isn't about replacing human connection — it's about filling the gaps. The moments when you need to talk at 2 AM, when you don't want to burden your friends again, or when you simply need someone to listen without judgment.
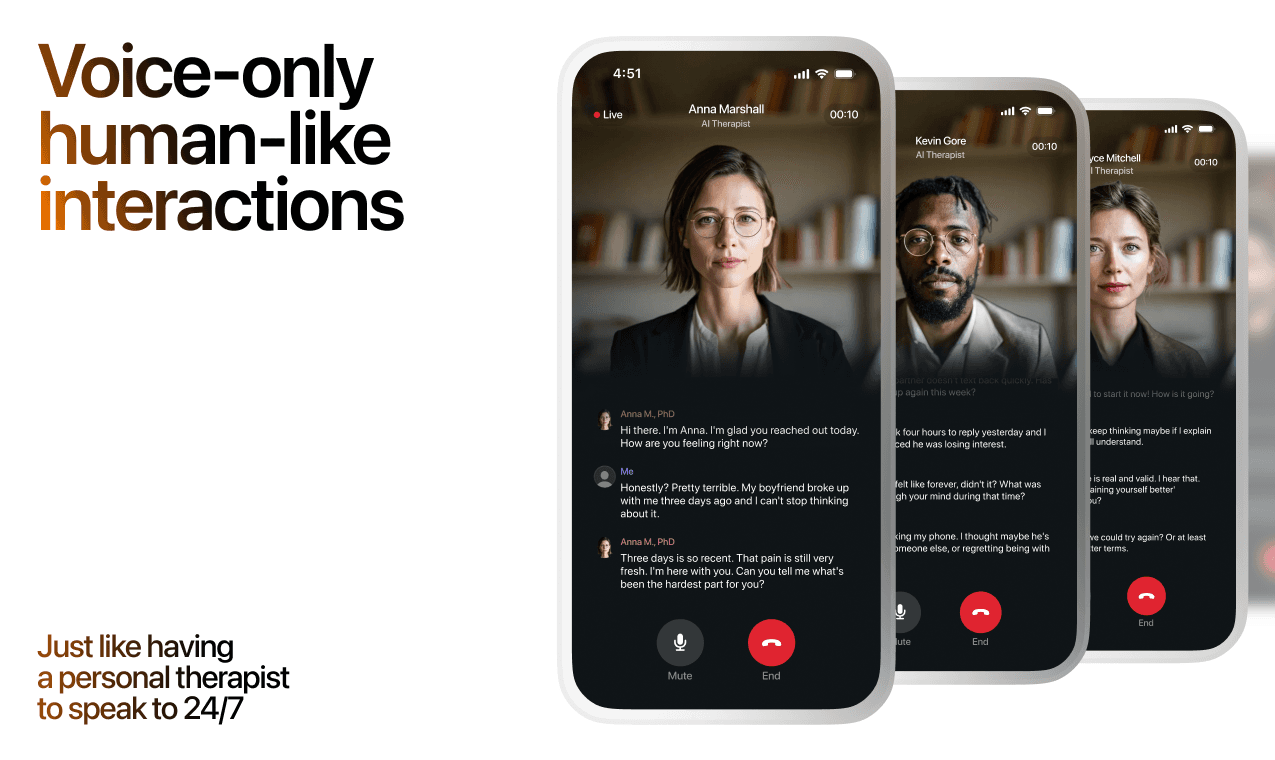
Here's what happens in a typical Lovon session:
You share what's on your mind
There's no script, no intake form, no waiting room. You speak or type whatever you're feeling — in your own words, at your own pace.
Lovon validates and explores
Using frameworks from CBT (Cognitive Behavioral Therapy) and motivational interviewing, Lovon acknowledges your feelings first, then gently helps you explore them. No dismissive "just move on" advice.
You build coping skills together
Lovon doesn't just listen — it actively works with you on evidence-based techniques: thought reframing, urge surfing, behavioral experiments, and more.
What a Session with Lovon Looks Like
When to Seek Professional Help
AI support is a valuable tool, but it's not a replacement for professional care. Please consider reaching out to a licensed therapist if you experience any of the following:
- Persistent thoughts of self-harm or suicide
- Inability to perform daily activities (work, eating, sleeping) for more than 2 weeks
- Turning to alcohol or substances to cope
- Intense anger or desire to harm your ex-partner
- Complete emotional numbness that doesn't improve over time
Crisis Resources (US): If you're in immediate danger, call 988 (Suicide & Crisis Lifeline) or text HOME to 741741 (Crisis Text Line). Available 24/7, free, and confidential.
Outside the US? Find a crisis line in your country
Ready to Start?
Your healing journey can begin right now
1 free conversation. No credit card. No judgment. Just a safe space to process what you're going through.
Frequently Asked Questions
Is AI therapy a replacement for a real therapist?
Is my conversation with Lovon AI private?
How is Lovon different from ChatGPT for emotional support?
Can I use Lovon if I'm already seeing a therapist?
Can I try Lovon for free?
About the Author
The Lovon Editorial Team
Mental Health & Wellness Content Team
The Lovon Editorial Team develops mental health and wellness content designed to make psychological concepts accessible and actionable. Our goal is to bridge the gap between clinical research and everyday life - helping you understand why your mind works the way it does and what you can do about it....
Similar Articles
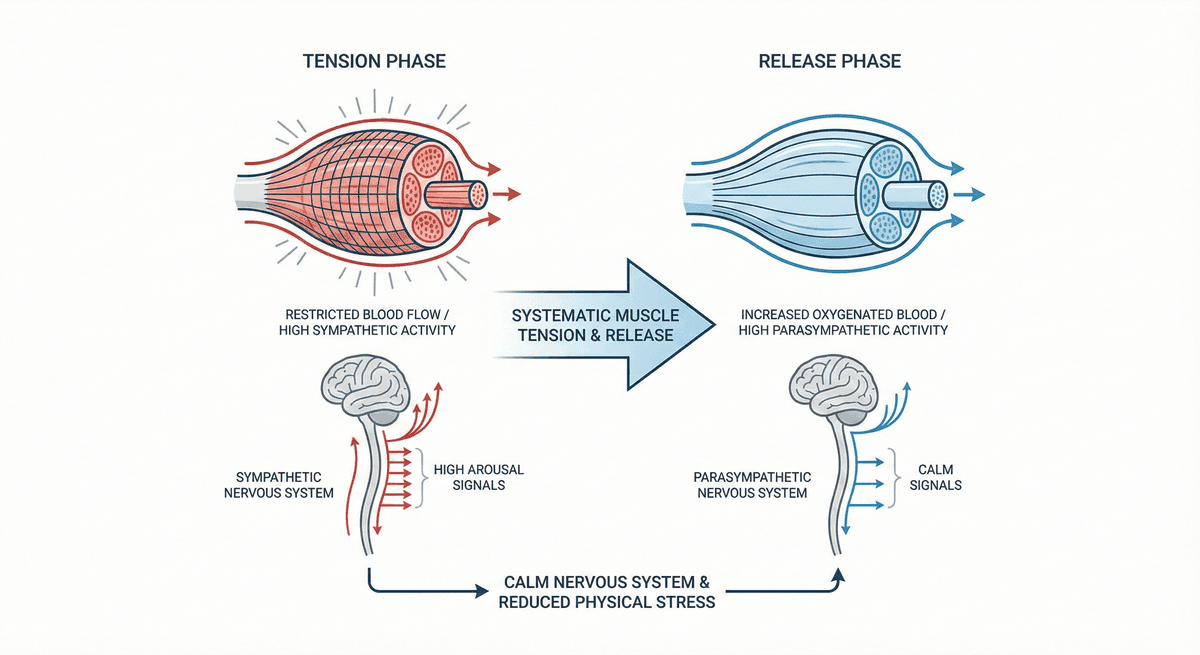
Progressive Muscle Relaxation for Stress Reduction
A systematic muscle group tension and release technique that calms the nervous system and reduces physical stress.
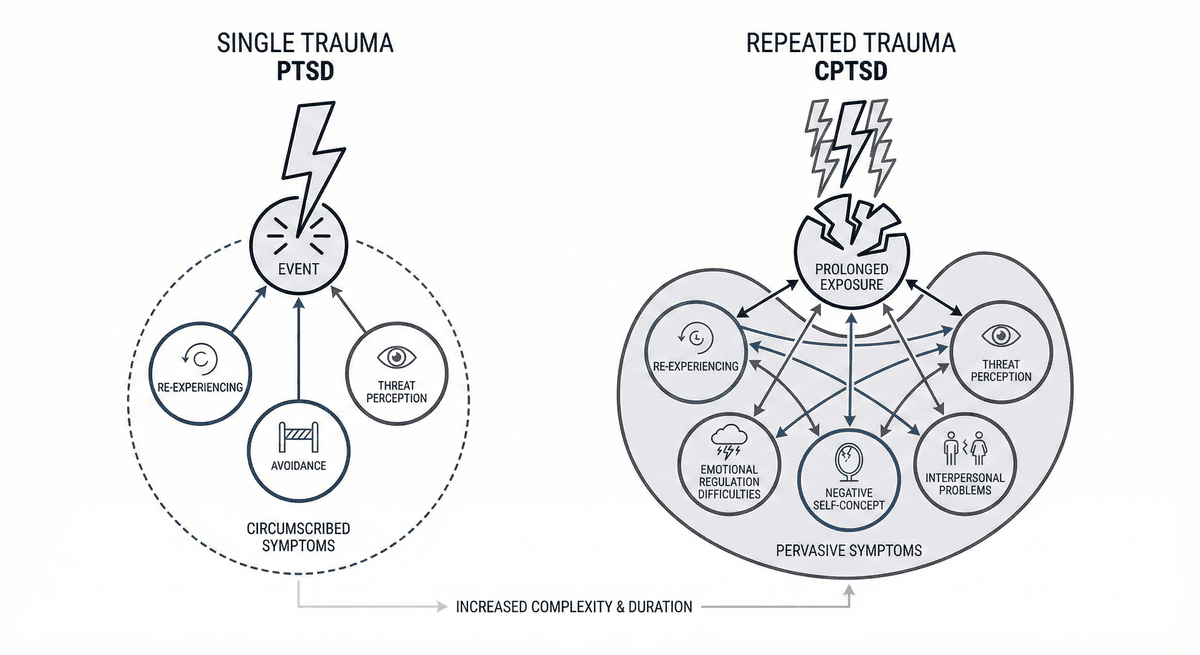
PTSD vs CPTSD: Single Trauma vs Repeated Trauma Symptom Differences
Learn how PTSD from a single traumatic event differs from CPTSD shaped by repeated trauma, including symptom patterns and treatment approaches.
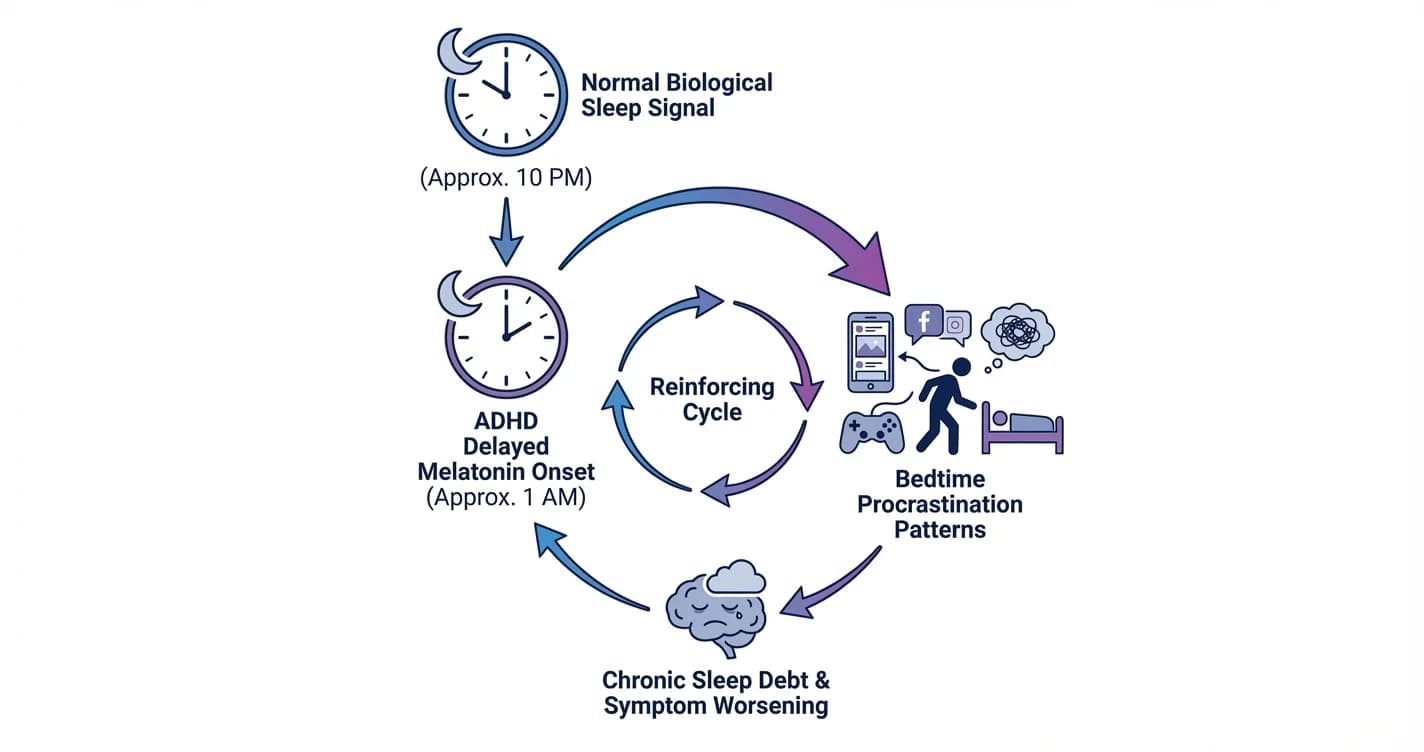
ADHD Sleep Cycle Disruption: Melatonin Delay and Bedtime Procrastination Patterns
Understanding how attention regulation difficulties interfere with natural sleep timing and the nightly wind-down process
Disclaimer: This article is for informational purposes only and does not constitute medical advice, diagnosis, or treatment. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition. If you are in crisis or think you may have an emergency, call 988 (Suicide & Crisis Lifeline) or go to the nearest emergency room. Outside the US? Find a crisis line in your country.