Inner Child Healing for Nervous System Regulation and Stored Trauma
When your body reacts to stress with overwhelming intensity—heart racing, chest tightening, mind spiraling—it''s often not just responding to what''s happening

Key Takeaways
- Hyperarousal: chronic tension, difficulty relaxing, hypervigilance, startle responses
- Hypoarousal: numbness, dissociation, fatigue, emotional flatness
- Dysregulation: rapid cycling between activated and shut-down states
- Somatic symptoms: digestive issues, chronic pain, tension without clear physical cause
- Pause the thought spiral and bring attention to physical sensations
Introduction
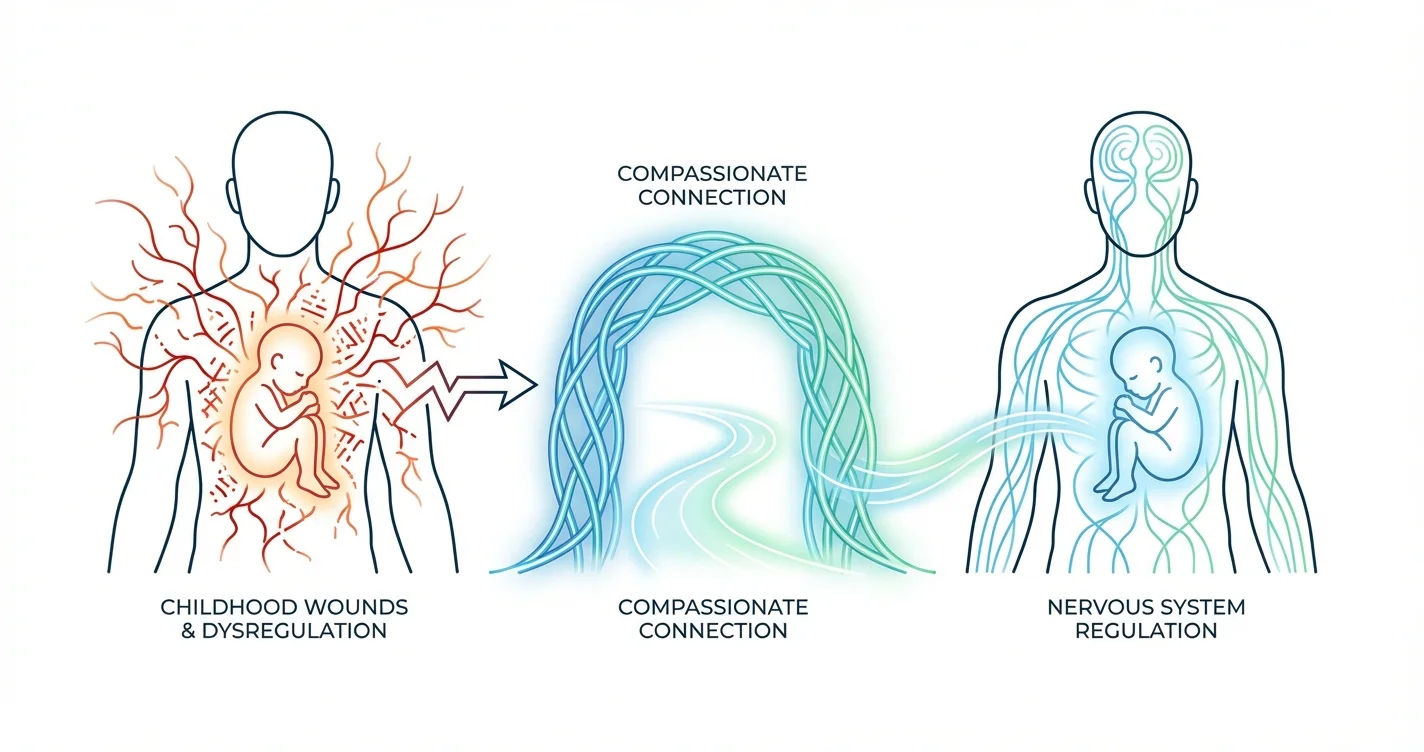
When your body reacts to stress with overwhelming intensity—heart racing, chest tightening, mind spiraling—it's often not just responding to what's happening now. Your nervous system may be replaying old patterns learned long ago, when you were young and survival depended on hypervigilance, shutdown, or pleasing others. Inner child healing for nervous system regulation and stored trauma responses offers a pathway to address these deeply embedded reactions at their source. This approach recognizes that many adult trauma responses originate from childhood experiences that shaped how your nervous system learned to perceive and respond to threat. By turning inward to address these early wounds with compassion rather than judgment, you can begin to release stored physiological patterns and create new, more regulated responses to stress.
Understanding How Childhood Experiences Shape Your Nervous System
Your nervous system develops its threat-detection patterns during childhood, when your brain is highly plastic and learning which signals mean safety versus danger. During these formative years, experiences of neglect, unpredictability, criticism, or trauma teach your body specific survival strategies. Research in developmental neuroscience suggests that these early adaptations—freezing when a parent was angry, becoming hypervigilant to emotional shifts, or suppressing needs to avoid conflict—become embedded as automatic physiological responses.
The critical insight is that these patterns don't simply remain as memories. They persist in your body through measurable physiological changes, including altered cortisol response patterns and inflammatory markers that maintain a state of alert even when objective danger has passed. Your adult nervous system may continue operating from these childhood threat models, interpreting situations through the lens of old wounds rather than present reality.
This is why someone who experienced emotional neglect as a child might feel their heart race and palms sweat during minor disagreements—their nervous system learned that withdrawal of connection signals danger. Understanding this connection between childhood experience and current physiological responses is the foundation of inner child work for trauma regulation.
The Body Keeps Score: Why Stored Trauma Isn't Just Mental
One of the most significant shifts in trauma understanding is recognizing that traumatic experiences don't only create psychological memories—they create physiological imprints. When practitioners work with clients on nervous system regulation and stored trauma responses, they're addressing real biological patterns, not just thought processes.
Studies in psychoneuroimmunology indicate that chronic stress and trauma can influence inflammatory pathways and stress hormone regulation in ways that persist years after the original events. Your body may continue producing stress responses—elevated cortisol, activation of the sympathetic nervous system, inflammatory cascades—even when consciously you know you're safe.
This is why positive thinking alone rarely resolves trauma responses. You can't simply think your way out of patterns that exist at the autonomic nervous system level. The work requires engaging with the parts of yourself that hold these patterns—often the younger, wounded aspects that therapists call the "inner child." These aren't abstract concepts but representations of the developmental stages when specific threat responses were learned and encoded.
Key physiological markers of stored trauma responses include:
- Hyperarousal: chronic tension, difficulty relaxing, hypervigilance, startle responses
- Hypoarousal: numbness, dissociation, fatigue, emotional flatness
- Dysregulation: rapid cycling between activated and shut-down states
- Somatic symptoms: digestive issues, chronic pain, tension without clear physical cause
Shifting From "Why" to "What": A Foundational Inner Child Approach
One of the most practical techniques in inner child healing for nervous system regulation involves a fundamental shift in how you address distressing patterns. When you notice yourself stuck in shame, anxiety, or reactivity, your instinct might be to ask "Why am I like this?" or "What's wrong with me?"
However, practitioners note that these "why" questions often fuel rumination and shame cycles rather than leading to change. The analytical mind trying to explain dysfunction tends to reinforce negative self-narratives: "I'm broken," "I'm too sensitive," "I'll never change." This analytical approach keeps you in your thinking brain—the very part that's often disconnected from the body-based patterns driving your distress.
A more effective approach involves shifting to compassionate, need-based questions: "What do I need right now?" or "What does my younger self need in this moment?" This simple reframing moves you from judgment to compassion, from analysis to embodied awareness. It helps you access the part of your brain that can respond with care rather than criticism.
In practice, this might look like:
Old pattern: Feeling anxious before a social event and thinking "Why do I always get so nervous? Everyone else is fine. What's wrong with me?"
Inner child approach: Noticing the anxiety and asking "What does my nervous system need right now? What would help my younger self feel safer?"
This shift from analytical rumination to compassionate inquiry helps break the cycle of self-judgment that often intensifies nervous system dysregulation. Tools like Lovon.app can support this practice by providing an immediate space to process these patterns through voice-based reflection when they arise, helping you identify needs and develop compassionate responses in real time.
Practical Methods for Inner Child Healing and Nervous System Regulation
Working with your inner child to regulate stored trauma responses involves specific, actionable techniques that address both the psychological and physiological dimensions of healing.
Using Visual Anchors for Compassion
One effective method involves working with childhood photographs. When you're experiencing a strong trauma response—anxiety, shame, reactivity—looking at a photo of yourself as a child can help activate a compassionate rather than critical response. It's often easier to feel care for a young child (even your younger self) than for your adult self in distress.
The practice involves:
- Select a childhood photo that evokes tenderness—ideally from around the age when difficult patterns began
- When you notice dysregulation, look at this image
- Ask: "What would this child need right now?"
- Respond to yourself with the same compassion you'd offer that child
This technique leverages the brain's capacity for self-compassion by creating psychological distance that makes care more accessible.
Body-Based Awareness for Breaking Rumination
Since stored trauma lives in the body, effective regulation requires moving from mental analysis to somatic awareness. When you notice rumination or anxiety building:
- Pause the thought spiral and bring attention to physical sensations
- Notice where tension, tightness, or numbness appears in your body
- Name sensations without judgment: "I notice tightness in my chest, tension in my shoulders"
- Ask your body what it needs: rest, movement, connection, boundaries
This approach recognizes that your nervous system's wisdom often isn't accessible through thinking. By attending to body signals, you can access information about what your system actually needs to return to regulation.
Reparenting Through Internal Dialogue
Inner child work involves developing an internal nurturing voice that provides what may have been missing in childhood. This isn't about blaming parents—genetic factors, temperament, and multiple influences contribute to how patterns develop—but about recognizing unmet developmental needs and addressing them now.
Practical reparenting involves:
- Noticing self-critical thoughts and pausing to ask if you'd speak this way to a child
- Developing affirming statements: "You're doing your best," "Your feelings make sense," "I'm here with you"
- Offering yourself what you needed then: validation, reassurance, permission to have needs
- Setting boundaries that protect your capacity rather than pushing through at all costs
Some people find it helpful to work with a therapist specializing in inner child approaches, while others explore these practices through journaling, meditation, or on-demand support tools that help process emotions as they arise.
Integrating Inner Child Work With Nervous System Regulation Techniques
Inner child healing becomes most effective when combined with direct nervous system regulation practices. These approaches work synergistically—addressing the psychological wounds while also teaching your physiology new response patterns.
Polyvagal-Informed Approaches
Research in polyvagal theory, developed by Dr. Stephen Porges, provides a framework for understanding how your autonomic nervous system shifts between states of safety (ventral vagal), threat response (sympathetic), and shutdown (dorsal vagal). Inner child work can be enhanced by recognizing which state you're in and using appropriate regulation techniques:
When hyperaroused (sympathetic activation): Your inner child may need grounding and containment. Techniques include deep breathing, progressive muscle relaxation, or placing a hand on your heart while offering reassurance.
When hypoaroused (dorsal shutdown): Your younger self may need gentle activation and engagement. Approaches include movement, cold water on the face, or connection with a safe person.
Building ventral vagal capacity: This involves creating experiences of safety and connection—with yourself through self-compassion practices, with others through secure relationships, and with your environment through predictable routines.
Creating Safety Signals for Your Nervous System
Your system needs consistent signals that you're no longer in the circumstances that created the original wounds. This involves:
- Developing reliable self-soothing practices your body learns to trust
- Creating physical environments that feel safe (lighting, temperature, organization)
- Establishing routines that provide predictability
- Identifying relationships that offer co-regulation (where your nervous system calms in another's safe presence)
- Using transitional objects or rituals that signal safety to younger parts
Tools like Lovon.app can serve as one form of consistent support, offering on-demand processing when you need to talk through a stress response or prepare for a triggering situation, helping your nervous system recognize that you have reliable resources now that weren't available in childhood.
Addressing Complex Patterns: When Inner Child Work Reveals Deeper Wounds
As you engage in inner child healing for nervous system regulation and stored trauma responses, you may encounter patterns that are more complex than anticipated. This is normal—trauma responses often involve multiple layers developed across different developmental stages.
Recognizing When Professional Support Is Needed
While self-directed inner child work offers valuable tools, some patterns require professional guidance. Consider seeking specialized support when:
- You experience dissociation, flashbacks, or intrusive memories that interfere with daily functioning
- Self-harm urges or suicidal thoughts emerge when exploring childhood experiences
- Substance use increases as you engage with painful memories
- Relationship patterns become more destructive rather than improving
- Physical symptoms worsen or new health concerns develop
Professionals who specialize in trauma-informed inner child work include therapists trained in Internal Family Systems (IFS), somatic experiencing, EMDR, or psychodynamic approaches. These practitioners can help you navigate complex trauma responses safely while building regulation capacity.
Understanding That Healing Isn't Linear
One of the most important trust signals in inner child work is acknowledging that progress rarely follows a straight path. You may experience:
- Periods of increased emotional intensity as stored material surfaces
- Regression to old patterns during stress, even after significant progress
- Oscillation between insight and resistance
- Variability in regulation capacity depending on context and resources
This isn't failure—it's the nature of working with deep-seated patterns. Your nervous system has maintained these responses for years because at one time they promoted survival. Changing them requires patience, repetition, and self-compassion through setbacks.
When to Seek Professional Help
If you're experiencing any of the following, consider reaching out to a mental health professional who specializes in trauma and inner child work:
- Persistent symptoms of anxiety, depression, or PTSD that interfere with work, relationships, or daily activities
- Difficulty functioning in important life areas despite self-help efforts
- Thoughts of self-harm or suicide
- Dissociative experiences that feel unmanageable
- Substance use as a primary coping mechanism
- Relationship patterns that repeatedly cause significant harm
Types of professionals who can help include licensed therapists, psychologists, or counselors specializing in trauma treatment, somatic therapies, or depth-oriented approaches. Many offer modalities specifically designed for inner child and nervous system work, including Internal Family Systems therapy, somatic experiencing, sensorimotor psychotherapy, and EMDR.
Conclusion
Inner child healing for nervous system regulation and stored trauma responses offers a pathway to address the root of many adult stress patterns. By recognizing that your current reactions often originate from survival strategies learned in childhood, you can approach dysregulation with compassion rather than criticism. The shift from asking "Why am I like this?" to "What do I need right now?" represents a fundamental reorientation from judgment to care—one that allows your nervous system to begin releasing old patterns and building new capacities for regulation.
This work requires patience and often benefits from multiple forms of support. Whether through self-directed practices like working with childhood photos and body-based awareness, structured therapeutic relationships, or accessible tools like Lovon.app for processing in the moment, the journey involves teaching your nervous system that you're no longer in the circumstances that created the original wounds. As you develop this internal sense of safety and self-compassion, the stored trauma responses that once protected you can gradually soften, allowing for greater regulation, resilience, and capacity to be present in your life.
The path forward involves small, consistent practices rather than dramatic breakthroughs—meeting yourself with the compassion your younger self needed, building safety signals your body can trust, and honoring the wisdom of patterns that once helped you survive even as you create new responses for who you're becoming.
Disclaimer: This is general information, not medical advice or diagnosis. If symptoms are severe, affecting your daily life, or you're having thoughts of self-harm—seek professional help. In the US: call or text 988 (Suicide & Crisis Lifeline). For immediate danger: 911 or local emergency services.
How AI Support Helps You Heal
AI emotional support isn't about replacing human connection — it's about filling the gaps. The moments when you need to talk at 2 AM, when you don't want to burden your friends again, or when you simply need someone to listen without judgment.
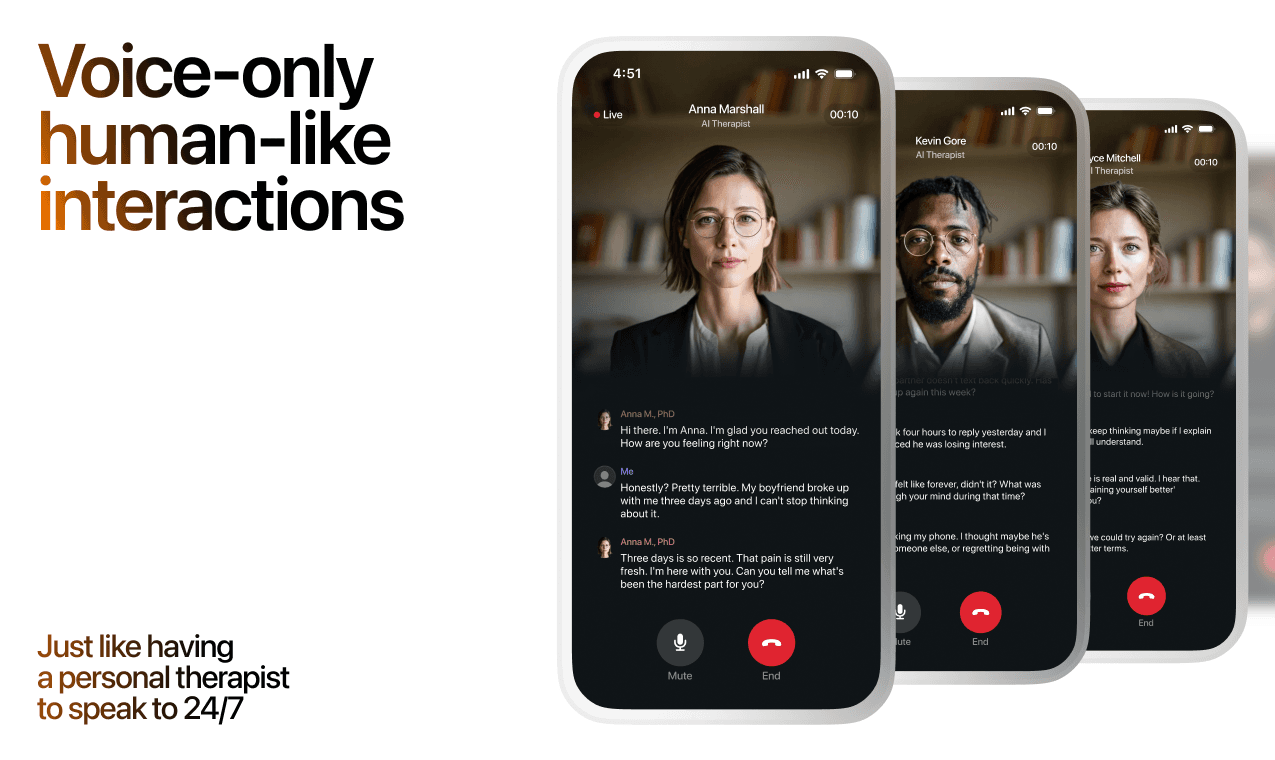
Here's what happens in a typical Lovon session:
You share what's on your mind
There's no script, no intake form, no waiting room. You speak or type whatever you're feeling — in your own words, at your own pace.
Lovon validates and explores
Using frameworks from CBT (Cognitive Behavioral Therapy) and motivational interviewing, Lovon acknowledges your feelings first, then gently helps you explore them. No dismissive "just move on" advice.
You build coping skills together
Lovon doesn't just listen — it actively works with you on evidence-based techniques: thought reframing, urge surfing, behavioral experiments, and more.
What a Session with Lovon Looks Like
When to Seek Professional Help
AI support is a valuable tool, but it's not a replacement for professional care. Please consider reaching out to a licensed therapist if you experience any of the following:
- Persistent thoughts of self-harm or suicide
- Inability to perform daily activities (work, eating, sleeping) for more than 2 weeks
- Turning to alcohol or substances to cope
- Intense anger or desire to harm your ex-partner
- Complete emotional numbness that doesn't improve over time
Crisis Resources (US): If you're in immediate danger, call 988 (Suicide & Crisis Lifeline) or text HOME to 741741 (Crisis Text Line). Available 24/7, free, and confidential.
Outside the US? Find a crisis line in your country
Ready to Start?
Your healing journey can begin right now
1 free conversation. No credit card. No judgment. Just a safe space to process what you're going through.
Frequently Asked Questions
Is AI therapy a replacement for a real therapist?
Is my conversation with Lovon AI private?
How is Lovon different from ChatGPT for emotional support?
Can I use Lovon if I'm already seeing a therapist?
Can I try Lovon for free?
About the Author
The Lovon Editorial Team
Mental Health & Wellness Content Team
The Lovon Editorial Team develops mental health and wellness content designed to make psychological concepts accessible and actionable. Our goal is to bridge the gap between clinical research and everyday life - helping you understand why your mind works the way it does and what you can do about it....
Similar Articles
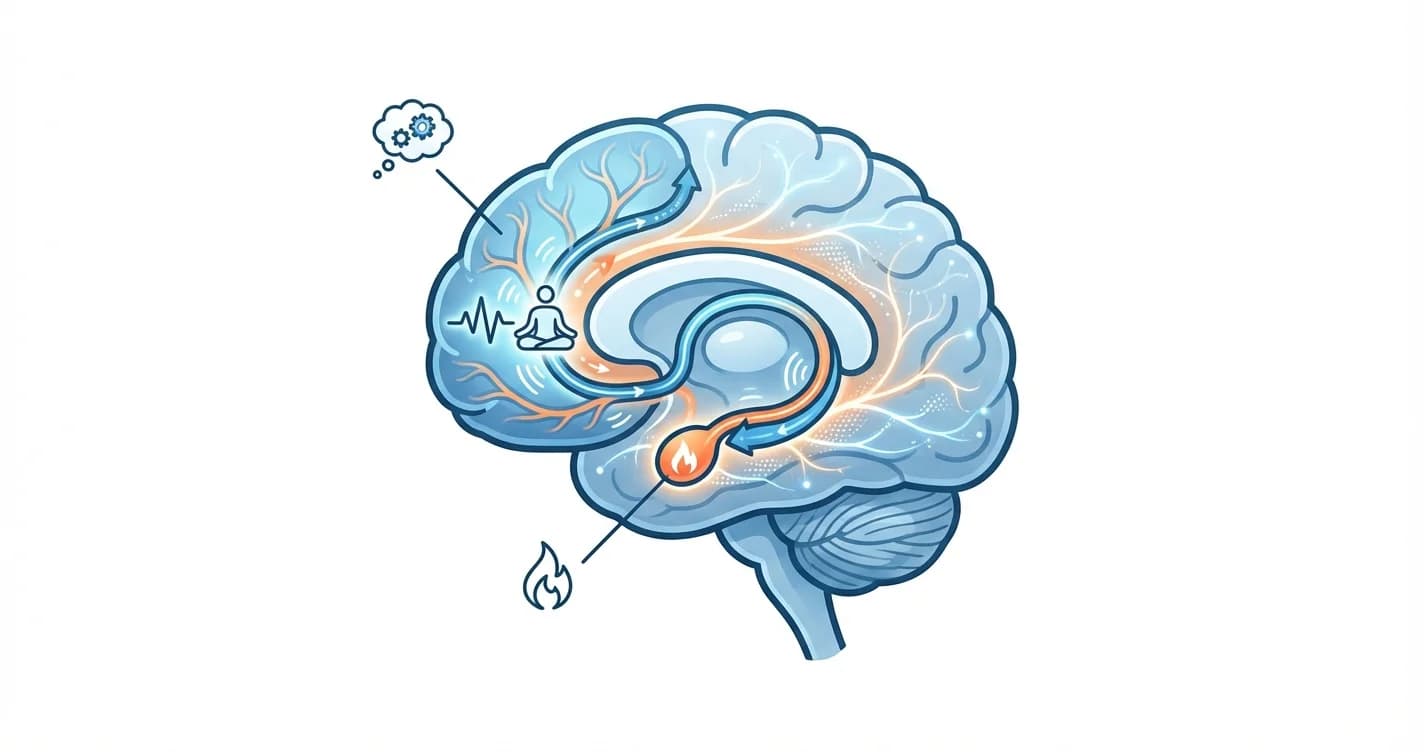
Amygdala and Prefrontal Cortex Connection: Training Emotional Regulation Through Mindfulness
How mindfulness practices reshape neural pathways to strengthen emotional control and reduce reactivity
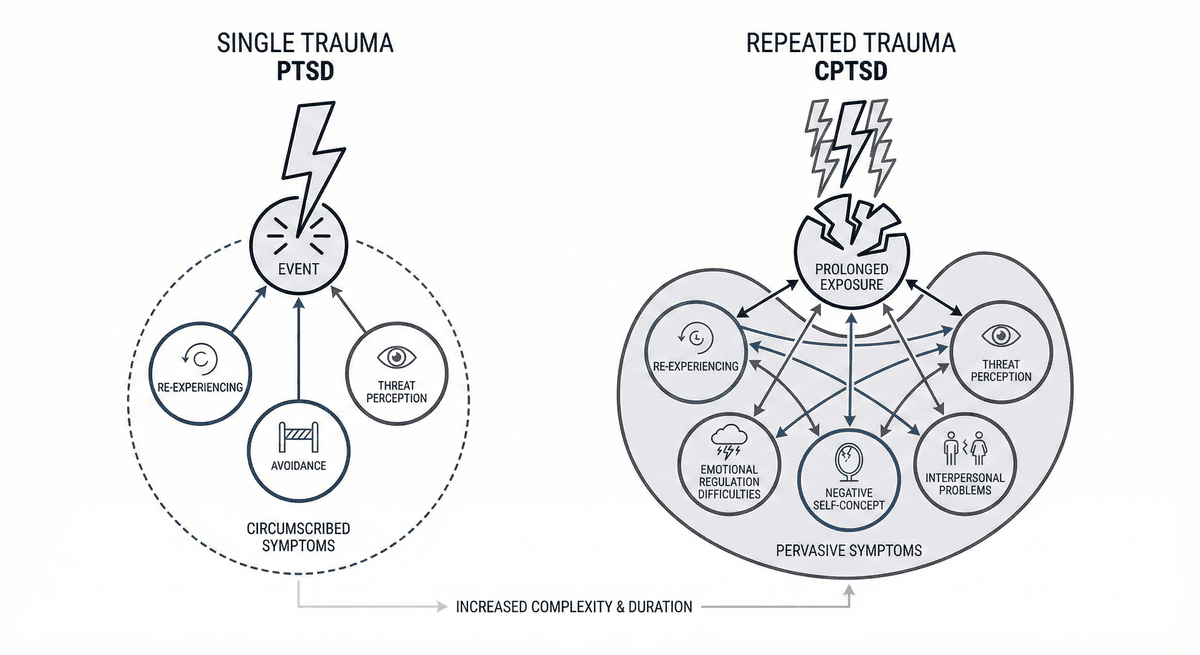
PTSD vs CPTSD: Single Trauma vs Repeated Trauma Symptom Differences
Learn how PTSD from a single traumatic event differs from CPTSD shaped by repeated trauma, including symptom patterns and treatment approaches.
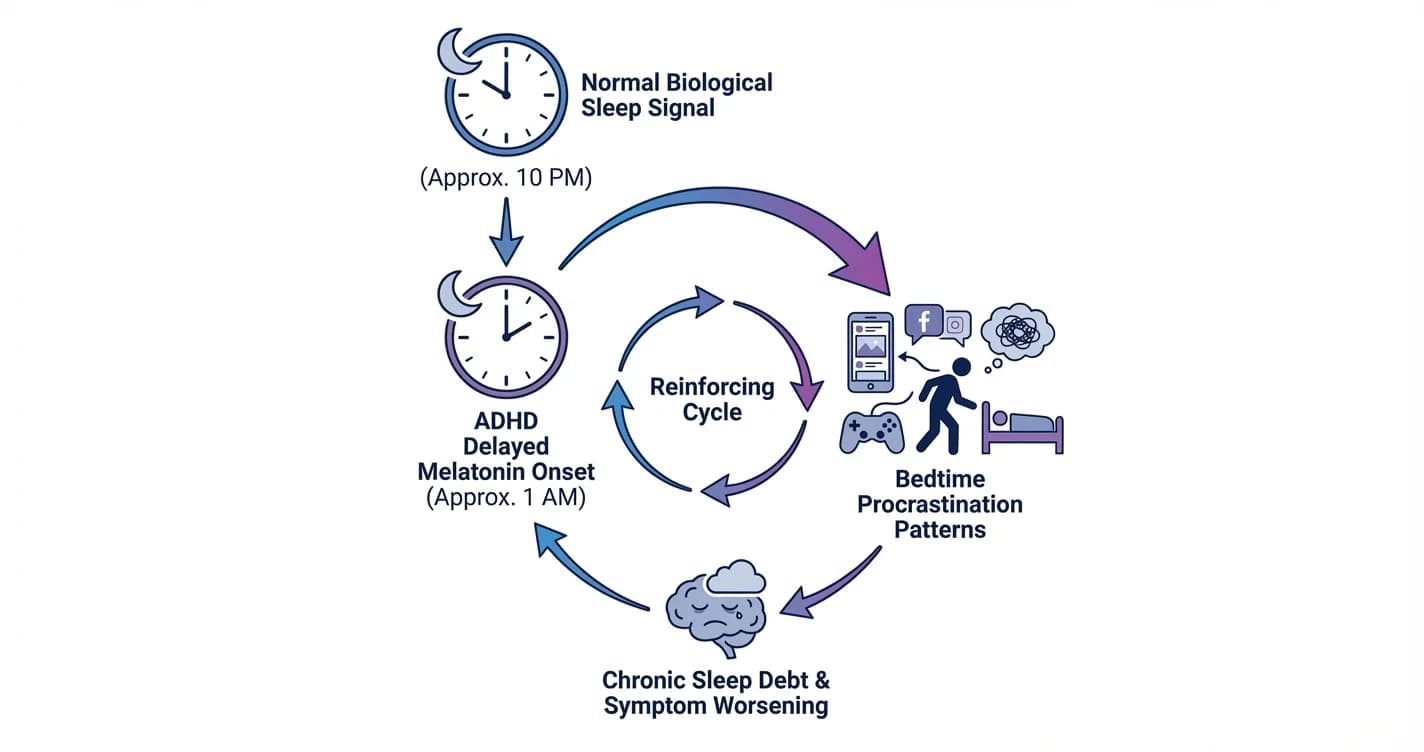
ADHD Sleep Cycle Disruption: Melatonin Delay and Bedtime Procrastination Patterns
Understanding how attention regulation difficulties interfere with natural sleep timing and the nightly wind-down process
Disclaimer: This article is for informational purposes only and does not constitute medical advice, diagnosis, or treatment. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition. If you are in crisis or think you may have an emergency, call 988 (Suicide & Crisis Lifeline) or go to the nearest emergency room. Outside the US? Find a crisis line in your country.