Understanding Therapy Progress Obstacles and How to Move Forward
Many people enter therapy with high hopes for rapid transformation, only to find themselves frustrated when progress feels slower than expected.

Key Takeaways
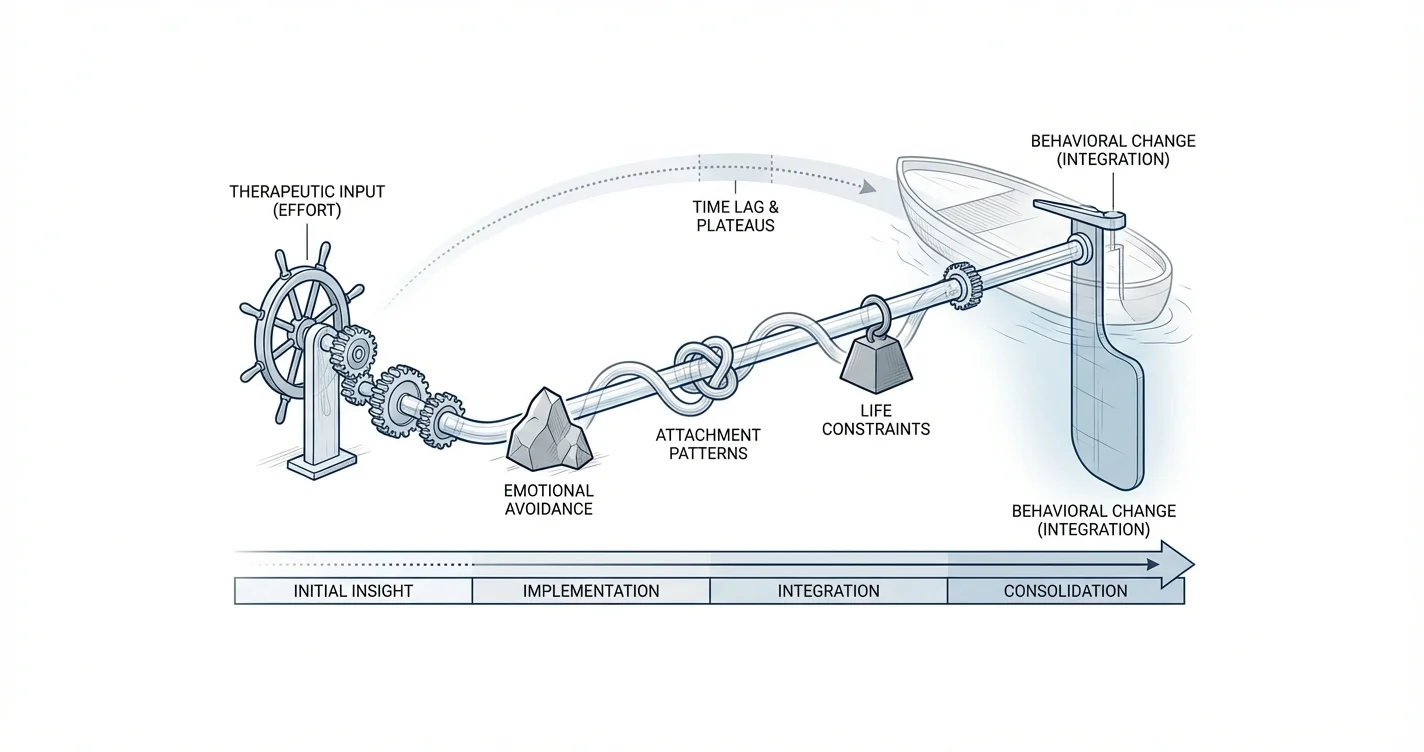
- Initial insight phase (weeks 1-4): Understanding patterns and developing awareness
- Implementation phase (weeks 4-12): Practicing new behaviors with inconsistent results
- Integration phase (months 3-6): New patterns becoming more automatic with visible progress
- Consolidation phase (months 6-12): Sustained change that feels natural rather than effortful
- Symptoms significantly impair your ability to work, maintain relationships, or handle daily responsibilities
Introduction
Many people enter therapy with high hopes for rapid transformation, only to find themselves frustrated when progress feels slower than expected. Therapy progress obstacles affect nearly everyone at some point in their mental health journey, and understanding these barriers is the first step toward overcoming them. This article draws on expert clinical insights and current research to examine why therapeutic progress sometimes stalls, what the most common obstacles are, and how both clients and practitioners can navigate these challenges more effectively. Rather than viewing plateaus as failures, recognizing therapy progress obstacles as a natural part of the healing process can help you adjust expectations and strategies for more sustainable growth.
The Timeline Misconception: Why Progress Feels Slow
One of the most significant therapy progress obstacles stems from misunderstanding how change actually unfolds in mental health treatment. According to clinical practitioners who work extensively with clients experiencing therapeutic plateaus, the primary reason people abandon effective strategies prematurely is unrealistic expectations about recovery timelines.
Mental health change operates more like steering a large ship than driving a car. When you turn a ship's wheel, the vessel doesn't immediately change direction—there's substantial lag between input and visible results. Similarly, therapeutic interventions often create internal shifts long before external changes become apparent. Research in neuroplasticity suggests that forming new neural pathways and behavioral patterns requires consistent repetition over weeks or months, not days.
This delay between effort and observable results creates what experts describe as a motivation trap. Clients frequently apply tremendous effort to implementing therapeutic strategies, see minimal immediate change, and conclude the approach isn't working. In reality, most clients demonstrate strong motivation and work ethic—the issue isn't lack of effort but rather premature evaluation of effectiveness.
The typical timeline for noticing meaningful therapeutic change includes:
- Initial insight phase (weeks 1-4): Understanding patterns and developing awareness
- Implementation phase (weeks 4-12): Practicing new behaviors with inconsistent results
- Integration phase (months 3-6): New patterns becoming more automatic with visible progress
- Consolidation phase (months 6-12): Sustained change that feels natural rather than effortful
Understanding this natural progression helps contextualize temporary plateaus as expected waypoints rather than dead ends.
Common Therapy Progress Barriers
Several specific obstacles consistently emerge across different therapeutic modalities and client populations. Identifying which barriers apply to your situation enables more targeted problem-solving.
Emotional avoidance represents one of the most pervasive therapy progress obstacles. While therapy aims to process difficult emotions, the natural human instinct is to avoid psychological discomfort. Clients may unconsciously steer conversations away from painful topics, minimize significant experiences, or intellectualize emotions rather than feeling them. This protective mechanism, while understandable, prevents the emotional processing necessary for healing.
Attachment patterns and therapeutic alliance issues can create significant barriers. Research from attachment theory indicates that people with insecure attachment styles may struggle to trust their therapist, anticipate rejection, or have difficulty accepting support—the very elements that make therapy effective. These patterns often replay childhood relational dynamics within the therapeutic relationship itself.
Life circumstances and practical constraints frequently impede progress in ways that have nothing to do with the therapy itself. Financial stress, demanding work schedules, lack of social support, or ongoing trauma exposure make it difficult to implement therapeutic strategies or maintain consistent attendance. Studies indicate that environmental stability significantly predicts treatment outcomes.
Skill deficits and readiness gaps occur when therapy requires capacities the client hasn't yet developed. For example, dialectical behavior therapy assumes certain emotional regulation abilities, while psychodynamic approaches require tolerance for ambiguity. When therapeutic demands exceed current capabilities, progress naturally stalls until foundational skills develop.
Mismatched therapeutic approaches sometimes explain persistent obstacles. Not every modality suits every person or problem. Cognitive-behavioral therapy excels for anxiety and specific behavioral issues, while relational or psychodynamic approaches may better address attachment wounds and identity concerns. What looks like resistance might actually be incompatibility between method and need.
Recognizing When You're Stuck Versus When You're Processing
Distinguishing between productive therapeutic work and genuine stagnation requires nuanced assessment. Not all apparent lack of progress represents a therapy progress obstacle that needs intervention.
Productive processing often feels uncomfortable and slow but includes signs of deepening work: increased emotional awareness, recognition of patterns previously invisible, temporary increase in distress as defenses soften, and growing capacity to sit with difficult feelings. This phase may not produce immediate behavioral change but represents essential groundwork.
Genuine stagnation typically involves: repetitive sessions covering the same ground without new insights, consistent avoidance of agreed-upon homework or practice, feeling emotionally disconnected during sessions, or absence of any change—internal or external—over extended periods (three months or more).
According to practitioners specializing in treatment-resistant cases, the distinction often comes down to movement. Even slow progress involves some form of change—shifting perspectives, new questions emerging, or gradually increasing tolerance for discomfort. True obstacles create a static quality where nothing shifts despite consistent effort.
Strategies to Overcome Therapeutic Plateaus
When facing therapy progress obstacles, several evidence-based approaches can help restore momentum. These strategies work best when discussed collaboratively with your therapist rather than implemented unilaterally.
Adjust your timeline expectations by explicitly mapping realistic milestones with your therapist. Break large goals into smaller indicators of progress that might otherwise go unnoticed. Celebrate intermediate achievements like "I noticed my anger pattern before reacting" rather than waiting for "I never get inappropriately angry anymore."
Directly address the obstacle in session rather than working around it. If you notice yourself avoiding certain topics, name that pattern. If you feel disconnected from your therapist, discuss the disconnect itself. Meta-conversations about the therapy process often unlock progress that focusing solely on content cannot achieve.
Experiment with adjunct support to complement traditional therapy. Tools like Lovon.app provide on-demand processing between sessions when difficult emotions arise or patterns emerge. Having accessible support for real-time processing can help maintain momentum when weekly sessions alone aren't sufficient. Some people find that talking through situations shortly after they occur helps identify patterns more clearly than retrospective discussion days later.
Implement structured between-session practice with specific, achievable actions. Vague intentions like "be more assertive" rarely translate to behavior change. Concrete practices like "use the specific communication script we developed in one low-stakes conversation this week" provide clearer feedback about what's working.
Consider modality shifts if current approaches consistently produce minimal results after giving them adequate time (typically three to six months of engaged effort). This doesn't mean previous work was wasted—insights and self-awareness from one approach often make subsequent modalities more effective.
Evaluate medication options through consultation with a psychiatrist when psychological symptoms significantly impair functioning or create barriers to engaging with therapy. For some conditions, physiological interventions enable the emotional stability necessary for therapeutic work to gain traction. Discuss medication options with a healthcare provider to determine if this might support your therapeutic progress.
When Therapy Progress Obstacles Indicate Deeper Issues
Sometimes persistent barriers signal that current treatment isn't adequately addressing underlying complexity. While individual variation exists in how quickly people respond to therapy, certain patterns suggest the need for more intensive or specialized support.
Indicators that obstacles may reflect inadequate treatment intensity include: consistent implementation of therapeutic strategies with zero improvement, worsening symptoms despite engaged participation, intrusive symptoms (flashbacks, dissociation, severe anxiety) that prevent engagement with therapy content, and multiple treatment attempts across different modalities producing similar results.
Research from trauma-specialized treatment centers indicates that people with complex developmental trauma, significant dissociation, or severe attachment disruption often require specialized approaches that standard outpatient therapy doesn't provide. These might include trauma-focused modalities like EMDR or internal family systems, more frequent sessions, or intensive outpatient programs.
If practical obstacles consistently prevent therapy engagement—such as cost, scheduling conflicts, or transportation barriers—exploring alternative formats can help. Teletherapy, community mental health services, group therapy, or accessible options like Lovon.app can provide continuity of support when traditional weekly individual therapy isn't sustainable. While these don't replace specialized treatment when needed, they can maintain therapeutic momentum during gaps or transitions.
The Role of Self-Compassion in Navigating Obstacles
How you relate to therapy progress obstacles themselves significantly impacts whether they become temporary setbacks or permanent barriers. Research on therapeutic outcomes consistently finds that self-compassion—treating yourself with the same kindness you'd offer a struggling friend—predicts better long-term results than self-criticism.
When progress stalls, the natural tendency is self-blame: "I'm not trying hard enough," "I'm too broken to heal," or "I'm wasting my therapist's time." These judgments create additional emotional burden that further impedes progress. Clinical experience suggests that most clients experiencing obstacles are actually working extremely hard—the issue isn't effort but rather timing, approach, or external factors beyond their control.
Practicing self-compassion while facing therapy progress obstacles involves acknowledging difficulty without judgment ("This is genuinely hard right now"), recognizing shared humanity ("Many people struggle with similar obstacles"), and responding with kindness ("What would help me feel supported through this?"). This stance creates psychological space to problem-solve rather than spiral into shame.
When to Seek Additional Professional Support
While self-help strategies and standard outpatient therapy effectively address many mental health concerns, certain situations require more intensive professional intervention. Recognizing when therapy progress obstacles indicate the need for specialized care ensures you receive appropriate support.
Seek consultation with specialized providers or higher levels of care when:
- Symptoms significantly impair your ability to work, maintain relationships, or handle daily responsibilities
- You experience thoughts of self-harm or suicide
- Substance use escalates or interferes with functioning
- Eating disorder behaviors intensify
- Dissociation or flashbacks regularly disrupt daily life
- Multiple therapy attempts produce no improvement despite genuine engagement
Mental health professionals specializing in treatment-resistant conditions can assess whether diagnostic complexity, trauma history, or other factors require specialized approaches. Psychiatrists can evaluate whether medication might address physiological barriers to progress. Intensive outpatient programs provide more frequent support when weekly sessions aren't sufficient.
Conclusion
Therapy progress obstacles are a normal part of the healing journey rather than indicators of personal failure or ineffective treatment. Understanding that meaningful change operates on a delayed timeline—more like steering a ship than driving a car—helps contextualize temporary plateaus as expected phases rather than permanent barriers. The most common obstacles include unrealistic timeline expectations, emotional avoidance, attachment patterns affecting the therapeutic relationship, practical life constraints, and sometimes mismatched therapeutic approaches. Recognizing which specific barriers apply to your situation enables targeted strategies: adjusting expectations, directly discussing obstacles with your therapist, implementing structured practice, considering complementary support tools, or exploring different therapeutic modalities when current approaches consistently produce minimal results. Resources like Lovon.app can provide accessible between-session support for processing emotions and maintaining momentum when obstacles arise. Most importantly, approaching therapy progress obstacles with self-compassion rather than self-criticism creates the psychological foundation for sustainable growth. If you're experiencing persistent obstacles despite genuine engagement, discussing your concerns directly with your therapist or seeking consultation with specialized providers can help identify whether adjustments to your current approach or additional support might better address your needs.
Disclaimer: This is general information, not medical advice or diagnosis. If symptoms are severe, affecting your daily life, or you're having thoughts of self-harm—seek professional help. In the US: call or text 988 (Suicide & Crisis Lifeline). For immediate danger: 911 or local emergency services.
How AI Support Helps You Heal
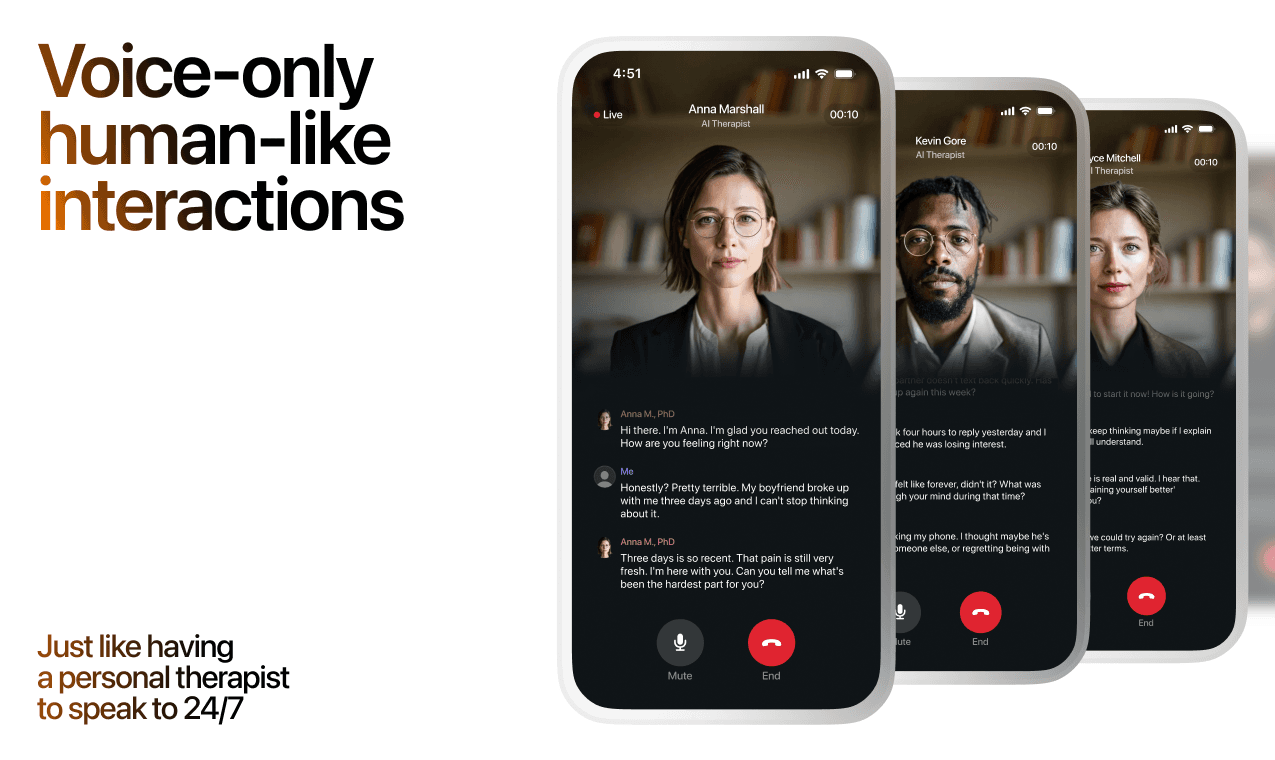
AI emotional support isn't about replacing human connection — it's about filling the gaps. The moments when you need to talk at 2 AM, when you don't want to burden your friends again, or when you simply need someone to listen without judgment.
Here's what happens in a typical Lovon session:
You share what's on your mind
There's no script, no intake form, no waiting room. You speak or type whatever you're feeling — in your own words, at your own pace.
Lovon validates and explores
Using frameworks from CBT (Cognitive Behavioral Therapy) and motivational interviewing, Lovon acknowledges your feelings first, then gently helps you explore them. No dismissive "just move on" advice.
You build coping skills together
Lovon doesn't just listen — it actively works with you on evidence-based techniques: thought reframing, urge surfing, behavioral experiments, and more.
What a Session with Lovon Looks Like
When to Seek Professional Help
AI support is a valuable tool, but it's not a replacement for professional care. Please consider reaching out to a licensed therapist if you experience any of the following:
- Persistent thoughts of self-harm or suicide
- Inability to perform daily activities (work, eating, sleeping) for more than 2 weeks
- Turning to alcohol or substances to cope
- Intense anger or desire to harm your ex-partner
- Complete emotional numbness that doesn't improve over time
Crisis Resources (US): If you're in immediate danger, call 988 (Suicide & Crisis Lifeline) or text HOME to 741741 (Crisis Text Line). Available 24/7, free, and confidential.
Outside the US? Find a crisis line in your country
Ready to Start?
Your healing journey can begin right now
1 free conversation. No credit card. No judgment. Just a safe space to process what you're going through.
Frequently Asked Questions
Is AI therapy a replacement for a real therapist?
Is my conversation with Lovon AI private?
How is Lovon different from ChatGPT for emotional support?
Can I use Lovon if I'm already seeing a therapist?
Can I try Lovon for free?
About the Author
The Lovon Editorial Team
Mental Health & Wellness Content Team
The Lovon Editorial Team develops mental health and wellness content designed to make psychological concepts accessible and actionable. Our goal is to bridge the gap between clinical research and everyday life - helping you understand why your mind works the way it does and what you can do about it....
Similar Articles
ADHD Comorbidity with Anxiety and Depression Cycles
Understanding the Complex Interplay Between ADHD and Recurring Mental Health Patterns
Amygdala and Prefrontal Cortex Connection: Training Emotional Regulation Through Mindfulness
How mindfulness practices reshape neural pathways to strengthen emotional control and reduce reactivity
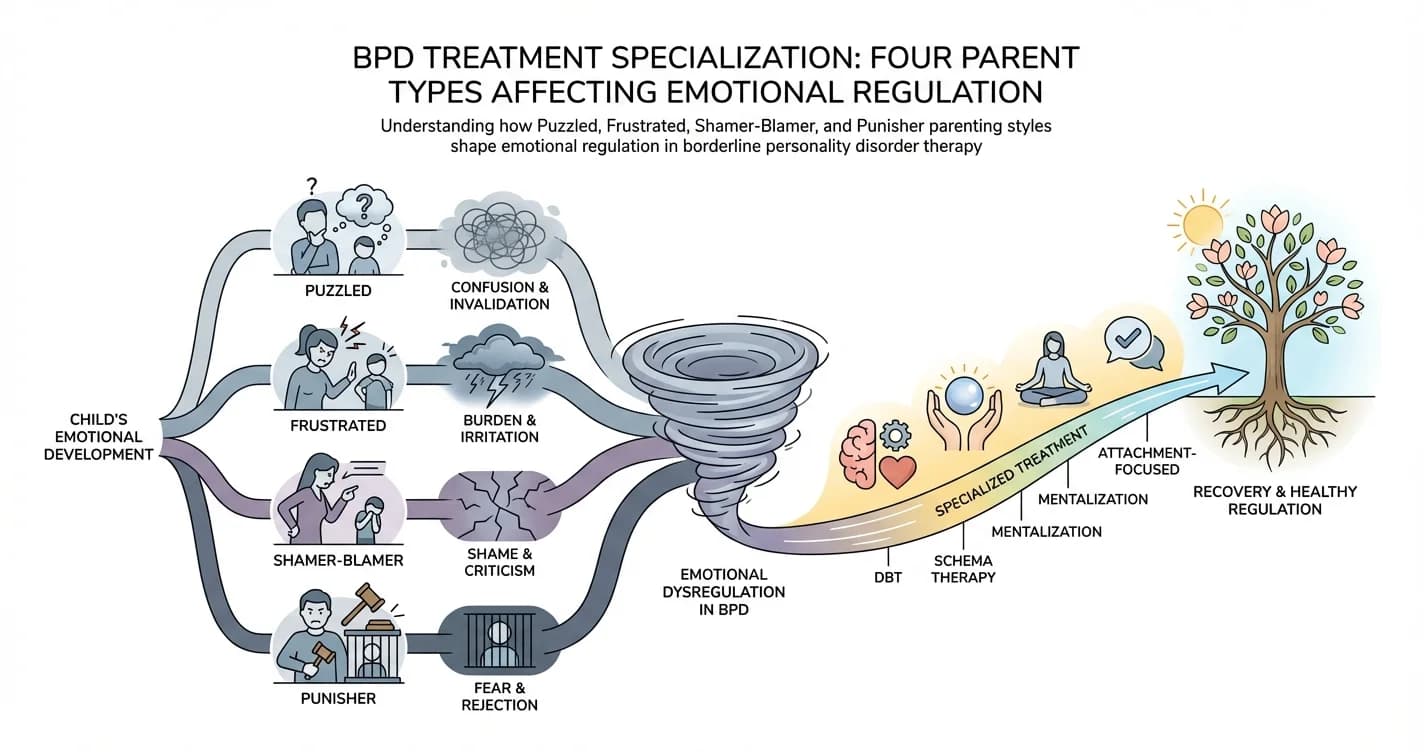
BPD Treatment Specialization: Four Parent Types Affecting Emotional Regulation
For individuals with borderline personality disorder (BPD), emotional regulation difficulties rarely emerge in isolation. Research increasingly suggests that
Disclaimer: This article is for informational purposes only and does not constitute medical advice, diagnosis, or treatment. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition. If you are in crisis or think you may have an emergency, call 988 (Suicide & Crisis Lifeline) or go to the nearest emergency room. Outside the US? Find a crisis line in your country.