Understanding Toxic Parent Accountability Patterns
When adult children attempt to address harm caused by their parents, they often encounter a predictable set of responses that deflect, minimize, or...

Key Takeaways
- Shame intolerance: Some people experience acknowledgment of wrongdoing as a fundamental threat to their self-concept
- Generational patterns: Parents who never witnessed healthy accountability in their own families may lack models for
- Investment in narrative: After years of justifying their parenting approach, admitting harm would require
- Power dynamics: Acknowledging a child's perspective—even an adult child—may feel like surrendering parental
- Limiting contact to specific contexts (holidays only, phone calls but not visits)
Introduction
When adult children attempt to address harm caused by their parents, they often encounter a predictable set of responses that deflect, minimize, or reverse blame. These toxic parent accountability patterns represent systematic ways emotionally harmful caregivers avoid taking responsibility for their actions. Understanding these patterns is essential for anyone seeking to establish healthier boundaries or process the impact of a difficult upbringing. Research in family systems therapy suggests that accountability avoidance stems from multiple factors including shame intolerance, rigid defense mechanisms, and sometimes personality characteristics that make acknowledging fault exceptionally difficult. This article examines the most common accountability patterns displayed by toxic parents, explores why these patterns persist, and provides practical approaches for managing interactions when genuine accountability remains unlikely.
Core Accountability Evasion Patterns
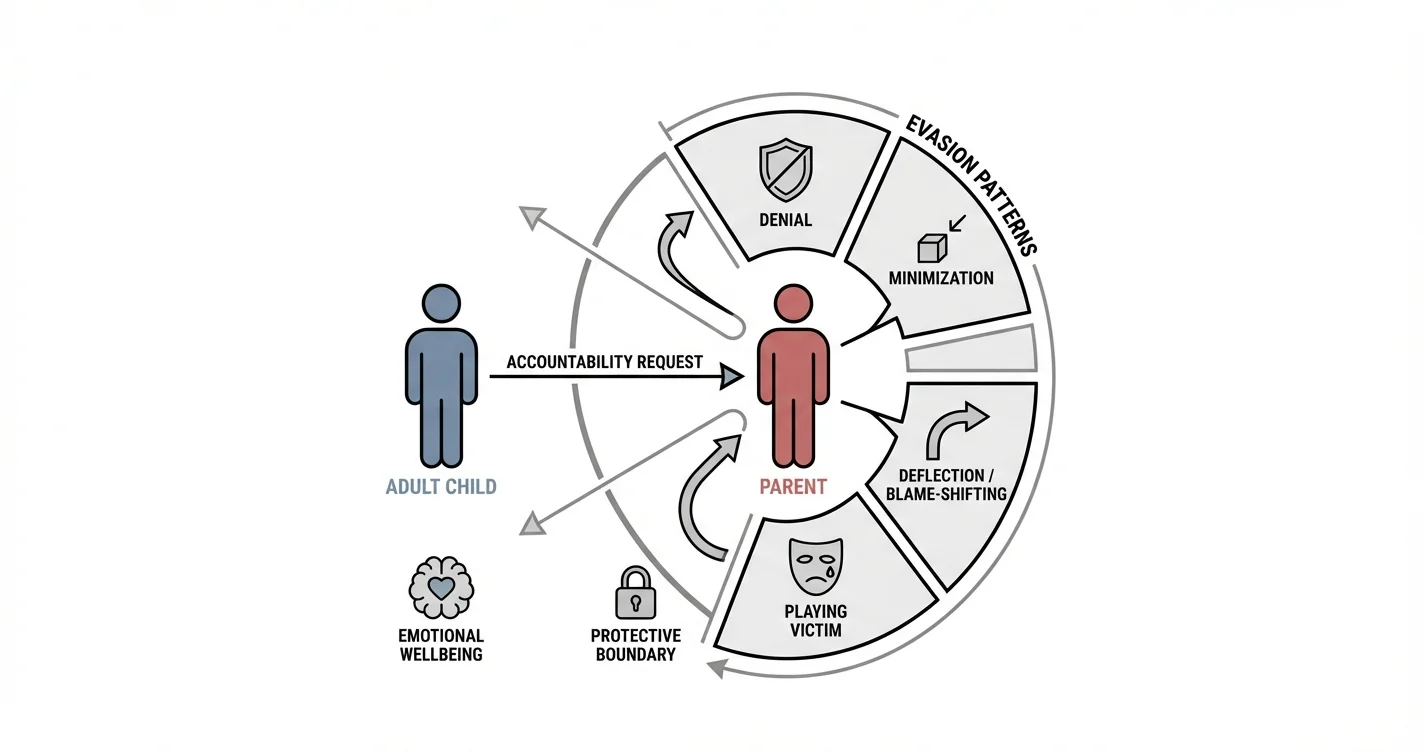
Toxic parent accountability patterns typically fall into several recognizable categories that mental health professionals encounter regularly in their work with adult children of dysfunctional families. These patterns serve the psychological function of protecting the parent's self-image while maintaining existing family dynamics.
The most prevalent pattern involves outright denial—insisting that harmful events simply never occurred. When confronted with specific memories of neglect, verbal abuse, or other damaging behaviors, parents employing this pattern may express genuine confusion or accuse their adult child of fabricating stories. This response can be particularly destabilizing because it forces the person seeking accountability to question their own memory and perception.
A closely related pattern is minimization, where parents acknowledge that something happened but characterize it as insignificant, exaggerated, or misinterpreted. Phrases like "you're too sensitive" or "that wasn't a big deal" exemplify this approach. Clinical experience suggests that minimization often proves more frustrating than outright denial because it acknowledges reality while simultaneously invalidating the emotional impact.
Deflection and blame-shifting represent another major category of toxic parent accountability behaviors. Rather than addressing the concern raised, parents using this pattern immediately redirect attention to the adult child's perceived flaws, other family members' behavior, or external circumstances beyond their control. The conversation shifts from "this is what you did that hurt me" to "well, you weren't an easy child" or "I was dealing with so much stress at the time."
Why Accountability Patterns Persist
Understanding why these patterns exist doesn't excuse harmful behavior, but it can help adult children develop more realistic expectations and protect their emotional wellbeing during interactions.
Research on personality development and trauma responses indicates that some individuals develop rigid psychological defenses that make acknowledging mistakes feel psychologically threatening. For parents with certain personality characteristics or their own unprocessed trauma, admitting fault may trigger overwhelming shame that their psyche has learned to avoid at all costs.
Several factors contribute to persistent accountability avoidance:
- Shame intolerance: Some people experience acknowledgment of wrongdoing as a fundamental threat to their self-concept rather than as an opportunity for growth
- Generational patterns: Parents who never witnessed healthy accountability in their own families may lack models for how to apologize genuinely or make amends
- Investment in narrative: After years of justifying their parenting approach, admitting harm would require dismantling a carefully constructed story about who they are
- Power dynamics: Acknowledging a child's perspective—even an adult child—may feel like surrendering parental authority in families where hierarchy remains rigid
The attachment patterns established in childhood also play a significant role. While early experiences with caregivers significantly influence how accountability patterns develop, genetic factors and individual temperament also contribute to how these dynamics unfold. Some parents may have grown up in environments where admitting mistakes was punished, creating deeply ingrained defensive responses that persist across decades.
Tools like Lovon.app can help adult children process the emotional impact of these dynamics by providing a space to talk through interactions, identify patterns, and develop strategies for protecting their wellbeing—particularly valuable when traditional therapy isn't immediately accessible or when processing is needed between professional sessions.
Recognizing Accountability Pattern Variations
Not all toxic parent accountability patterns manifest identically. Recognizing the specific variation you're encountering helps you adjust expectations and response strategies appropriately.
The "playing victim" pattern involves parents positioning themselves as the injured party when confronted. They may cry, express how hurt they are by accusations, or claim that raising concerns constitutes abuse toward them. This reversal puts the adult child in the position of comforter rather than person seeking acknowledgment, effectively derailing any possibility of genuine accountability.
The selective memory pattern involves parents remembering events in ways that consistently cast their actions in the most favorable light. Unlike deliberate lying, this may involve genuine memory reconstruction over time, where uncomfortable truths have been mentally rewritten into more palatable versions. When confronted with contrary accounts, these parents often appear genuinely confused because their remembered version feels real to them.
The conditional acknowledgment pattern represents a particularly frustrating variation where parents offer what initially sounds like accountability but immediately follow with justifications that negate it. "I'm sorry you feel that way, but you have to understand..." or "Maybe I shouldn't have done that, however you don't realize how difficult..." These non-apologies maintain the appearance of engagement while avoiding genuine responsibility.
Some parents employ the counterattack pattern, responding to attempts at accountability with aggressive criticism or threats. This might include threatening to cut off contact, bringing up the adult child's past mistakes in detail, or making statements designed to wound. This pattern often appears when parents feel their control or image is most threatened.
Understanding which patterns you're encountering helps you recognize when you're facing systemic avoidance rather than simple misunderstanding. This recognition is essential for determining whether continued attempts at dialogue serve your wellbeing or simply perpetuate frustrating cycles.
Practical Approaches When Accountability Remains Unlikely
When dealing with toxic parent accountability patterns, shifting focus from changing the parent's behavior to protecting your own wellbeing often represents the most productive approach. This doesn't mean accepting harmful treatment, but rather recognizing what remains within your control.
Adjusting expectations forms the foundation of this approach. If a parent has demonstrated consistent accountability avoidance across years or decades, expecting a sudden shift sets you up for repeated disappointment. Accepting that genuine acknowledgment may never come—while still recognizing that you deserved better—allows you to stop investing emotional energy in an outcome you cannot control.
Setting clear boundaries becomes essential when accountability isn't forthcoming. This might involve:
- Limiting contact to specific contexts (holidays only, phone calls but not visits)
- Establishing topics that are off-limits for discussion
- Deciding in advance how you'll respond when certain patterns emerge
- Being willing to end conversations or leave situations when boundaries are violated
Boundaries work most effectively when you focus on your own actions rather than trying to control the parent's behavior. "I won't continue conversations where I'm being yelled at" proves more enforceable than "you need to stop yelling at me."
Seeking validation elsewhere addresses the fundamental need that drives many accountability-seeking attempts. When a parent cannot or will not acknowledge harm, finding validation through therapy, support groups, trusted friends, or partners who understand your experience helps meet that legitimate need. Resources like Lovon.app provide on-demand support for processing difficult family interactions, particularly valuable when you need to talk through an encounter that just occurred and your regular support network isn't immediately available.
Documenting your reality can help counter gaslighting and memory distortion. Keeping a private journal of interactions, saving concerning messages or emails, and noting patterns helps you trust your own perceptions when dealing with parents who consistently deny or reframe events. This documentation serves your own clarity rather than "evidence" to present to the parent.
Grieving the parent you needed represents an important psychological process. Many adult children of toxic parents find themselves stuck because part of them still hopes for the acknowledgment and relationship they deserved. Allowing yourself to grieve the parent who could take accountability—while dealing with the parent you actually have—creates space for acceptance and forward movement.
When to Seek Professional Support
Working through the impact of toxic parent accountability patterns often benefits from professional guidance, particularly when these dynamics have affected your self-esteem, relationship patterns, or emotional regulation. Several signs indicate that professional support may be helpful:
Persistent difficulty trusting your own perceptions or memory, especially if you find yourself constantly questioning whether your feelings are valid. This often results from prolonged exposure to gaslighting and minimization patterns. Therapists specializing in family trauma can help you rebuild confidence in your own experience.
Recurring relationship difficulties that mirror parent-child dynamics, such as repeatedly choosing partners who deflect accountability or finding yourself unable to set boundaries in adult relationships. These patterns may indicate that early experiences have shaped your relational templates in ways that benefit from therapeutic exploration.
Emotional overwhelm when anticipating or recovering from family interactions. If preparing for a phone call with your parent triggers significant anxiety or you need days to recover emotionally from family gatherings, this suggests the relationship's impact on your wellbeing warrants professional attention. Therapists can help you develop coping strategies and determine what level of contact serves your health.
Considering estrangement or significant contact reduction without a clear sense of whether this decision aligns with your values and needs. These significant choices benefit from processing with someone who understands both the potential relief and the complex emotions that may accompany limiting family contact.
Mental health professionals who specialize in family systems, complex trauma, or adult children of dysfunctional families can provide frameworks for understanding your experience, validating your perceptions, and developing strategies tailored to your specific situation. The combination of professional therapy and accessible support tools creates a comprehensive approach to healing and boundary-setting.
Conclusion
Toxic parent accountability patterns—including denial, minimization, blame-shifting, and playing victim—represent systematic ways emotionally harmful parents avoid responsibility for their actions. These patterns persist due to multiple factors including shame intolerance, generational cycles, and sometimes personality characteristics that make acknowledging fault exceptionally difficult. While early experiences with caregivers play a significant role, genetic factors and individual temperament also contribute to how these dynamics develop. Recognizing these patterns helps adult children adjust expectations, understanding that genuine accountability may not be possible regardless of how clearly concerns are communicated. The most effective approach typically involves shifting focus from changing the parent to protecting your own wellbeing through boundary-setting, seeking validation elsewhere, and grieving the relationship you deserved but didn't receive. Whether you choose limited contact, modified relationships, or estrangement, validating your own experience and surrounding yourself with support—through therapy, trusted relationships, or resources like Lovon.app—provides the foundation for healing from these difficult family dynamics.
Disclaimer: This is general information, not medical advice or diagnosis. If symptoms are severe, affecting your daily life, or you're having thoughts of self-harm—seek professional help. In the US: call or text 988 (Suicide & Crisis Lifeline). For immediate danger: 911 or local emergency services.
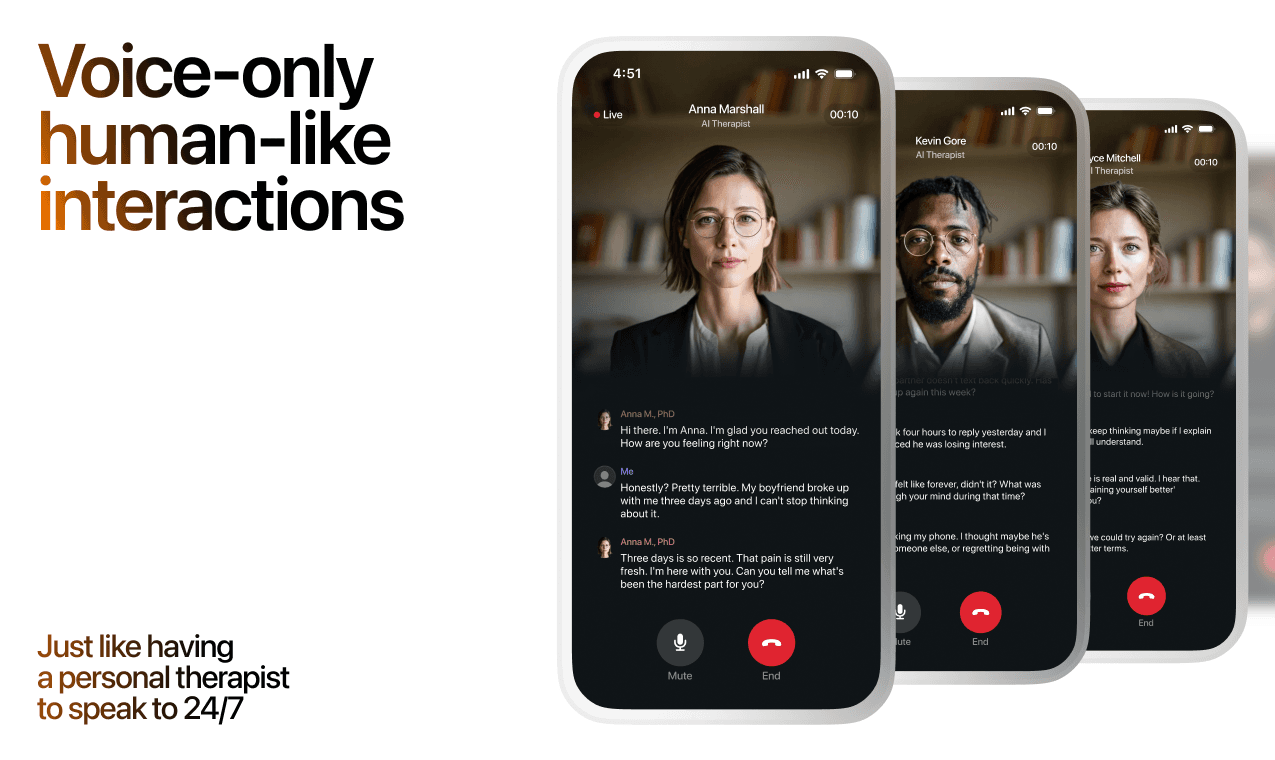
How AI Support Helps You Heal
AI emotional support isn't about replacing human connection — it's about filling the gaps. The moments when you need to talk at 2 AM, when you don't want to burden your friends again, or when you simply need someone to listen without judgment.
Here's what happens in a typical Lovon session:
You share what's on your mind
There's no script, no intake form, no waiting room. You speak or type whatever you're feeling — in your own words, at your own pace.
Lovon validates and explores
Using frameworks from CBT (Cognitive Behavioral Therapy) and motivational interviewing, Lovon acknowledges your feelings first, then gently helps you explore them. No dismissive "just move on" advice.
You build coping skills together
Lovon doesn't just listen — it actively works with you on evidence-based techniques: thought reframing, urge surfing, behavioral experiments, and more.
What a Session with Lovon Looks Like
When to Seek Professional Help
AI support is a valuable tool, but it's not a replacement for professional care. Please consider reaching out to a licensed therapist if you experience any of the following:
- Persistent thoughts of self-harm or suicide
- Inability to perform daily activities (work, eating, sleeping) for more than 2 weeks
- Turning to alcohol or substances to cope
- Intense anger or desire to harm your ex-partner
- Complete emotional numbness that doesn't improve over time
Crisis Resources (US): If you're in immediate danger, call 988 (Suicide & Crisis Lifeline) or text HOME to 741741 (Crisis Text Line). Available 24/7, free, and confidential.
Outside the US? Find a crisis line in your country
Ready to Start?
Your healing journey can begin right now
1 free conversation. No credit card. No judgment. Just a safe space to process what you're going through.
Frequently Asked Questions
Is AI therapy a replacement for a real therapist?
Is my conversation with Lovon AI private?
How is Lovon different from ChatGPT for emotional support?
Can I use Lovon if I'm already seeing a therapist?
Can I try Lovon for free?
About the Author
The Lovon Editorial Team
Mental Health & Wellness Content Team
The Lovon Editorial Team develops mental health and wellness content designed to make psychological concepts accessible and actionable. Our goal is to bridge the gap between clinical research and everyday life - helping you understand why your mind works the way it does and what you can do about it....
Similar Articles
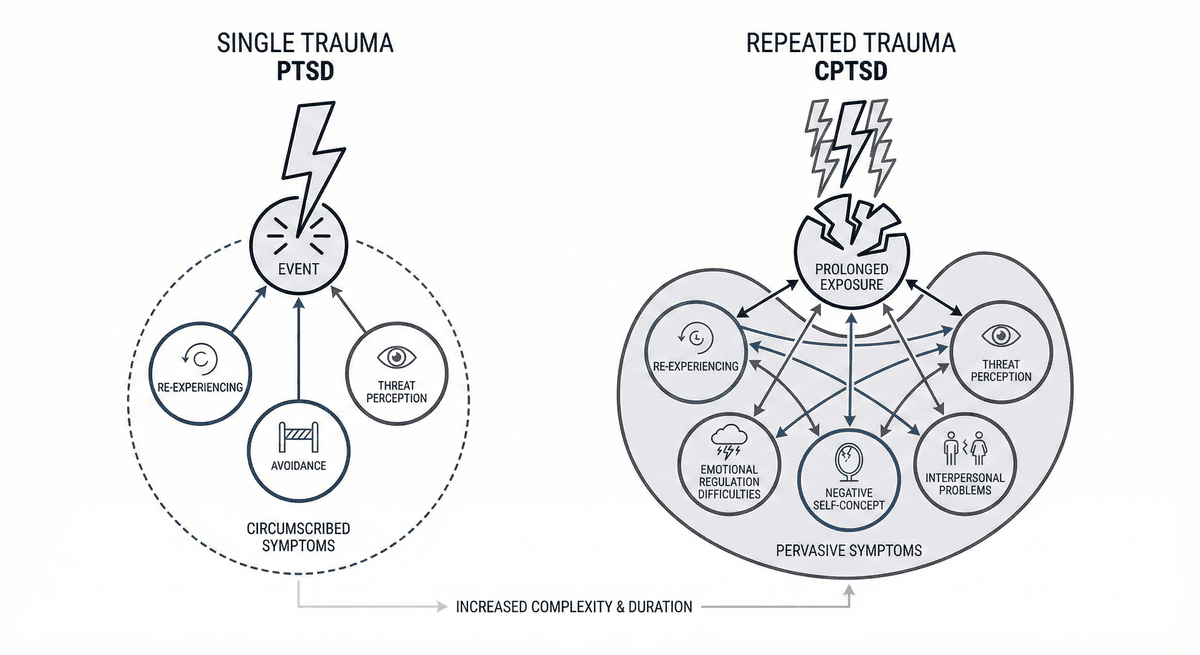
PTSD vs CPTSD: Single Trauma vs Repeated Trauma Symptom Differences
Learn how PTSD from a single traumatic event differs from CPTSD shaped by repeated trauma, including symptom patterns and treatment approaches.
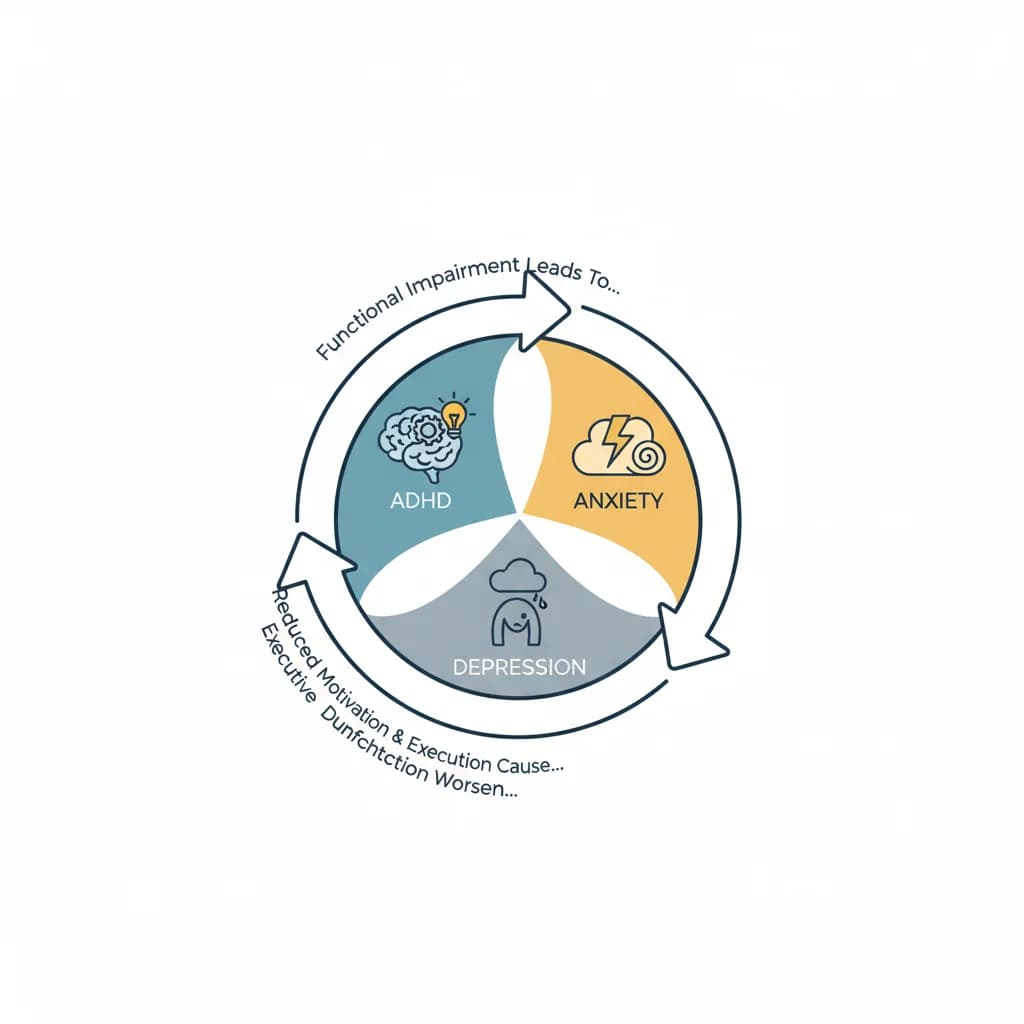
ADHD Comorbidity with Anxiety and Depression Cycles
Understanding the Complex Interplay Between ADHD and Recurring Mental Health Patterns
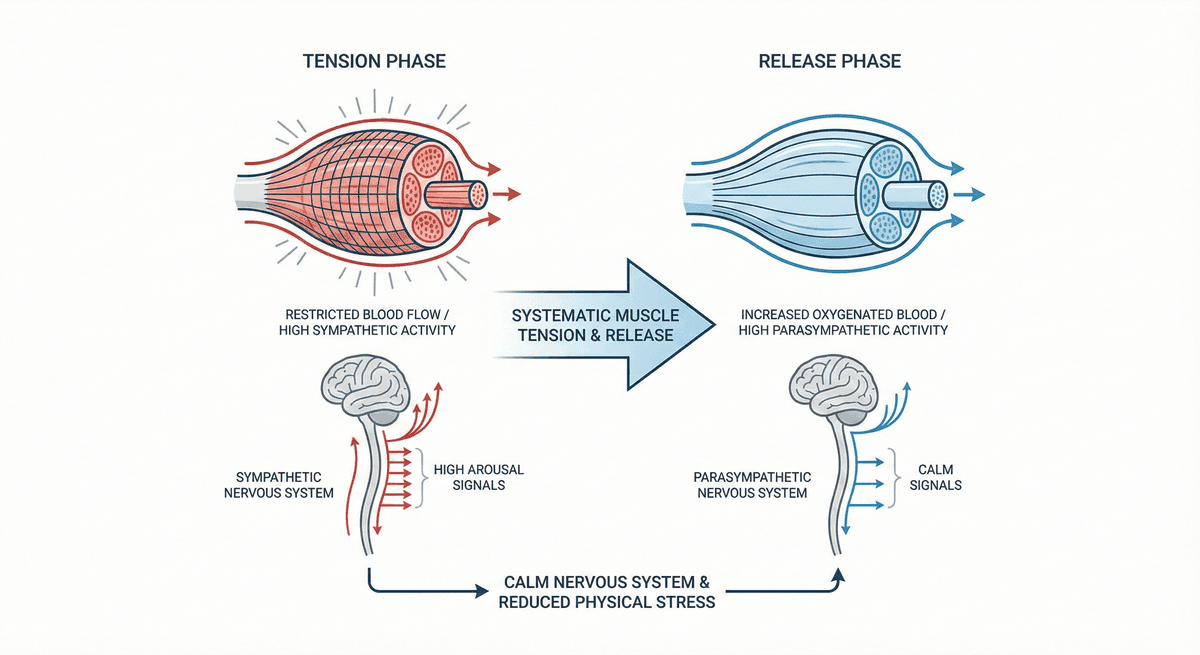
Progressive Muscle Relaxation for Stress Reduction
A systematic muscle group tension and release technique that calms the nervous system and reduces physical stress.
Disclaimer: This article is for informational purposes only and does not constitute medical advice, diagnosis, or treatment. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition. If you are in crisis or think you may have an emergency, call 988 (Suicide & Crisis Lifeline) or go to the nearest emergency room. Outside the US? Find a crisis line in your country.