EMDR Therapy Using Bilateral Stimulation for Trauma Memory Processing
EMDR Therapy Using Bilateral Stimulation for Trauma Memory Processing

Key Takeaways
- Thoughts of self-harm or suicide
- Inability to function in daily activities due to trauma symptoms
- Severe dissociation or loss of time
- Substance use to manage trauma symptoms
- Re-traumatization in current relationships or situations
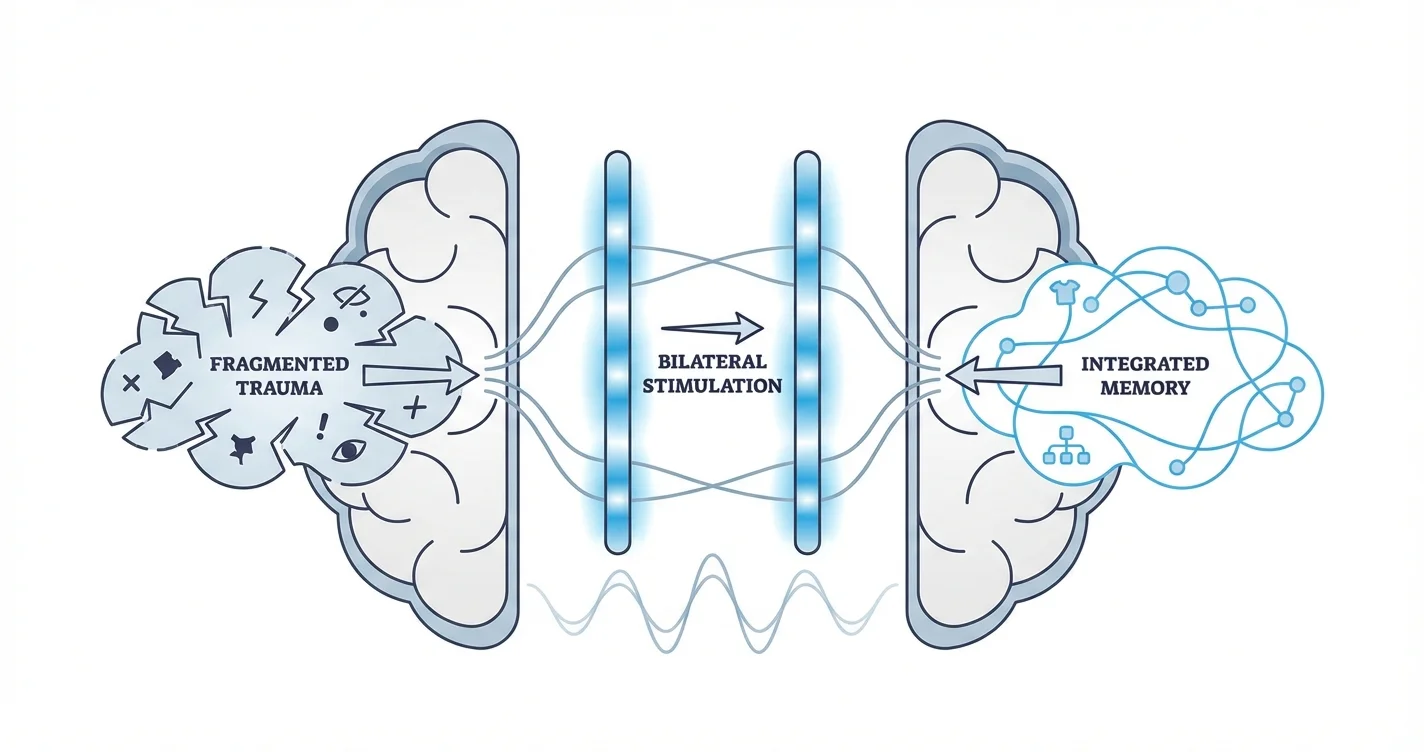
Traumatic memories don't always process the way ordinary memories do. They can remain fragmented, emotionally charged, and intrusive—disrupting daily life and well-being. EMDR therapy using bilateral stimulation for trauma memory processing has emerged as a powerful therapeutic approach that helps the brain integrate these fragmented experiences into coherent, less distressing narratives. This article explores how bilateral stimulation works in EMDR, the science behind trauma memory processing, and practical considerations for those seeking this form of treatment. This comprehensive guide draws on clinical research, practitioner insights, and established therapeutic frameworks to provide an authoritative overview of EMDR's bilateral stimulation techniques. Whether you're considering EMDR therapy, supporting someone through trauma recovery, or simply seeking to understand how the brain processes difficult experiences, this article offers evidence-based information to inform your understanding. Eye Movement Desensitization and Reprocessing (EMDR) therapy is a structured therapeutic approach that uses bilateral stimulation—alternating sensory input to both sides of the body—to facilitate trauma memory processing. The fundamental principle involves engaging the brain's natural healing mechanisms while a person recalls traumatic experiences in a controlled, therapeutic environment. Bilateral stimulation typically takes one of three forms: guided eye movements following a therapist's fingers or light bar, alternating tactile sensations through handheld buzzers or tapping, or auditory tones delivered through headphones. Research suggests that this alternating left-right stimulation may support the brain's ability to process information similarly to what occurs during REM sleep, when the eyes move rapidly and the brain consolidates memories. According to clinical frameworks outlined in trauma psychology research, traumatic memories often become stored in fragmented ways. Rather than forming cohesive narratives with clear beginnings, middles, and ends, these memories may exist as sensory fragments—images, sounds, body sensations, or intense emotions—disconnected from their context. This fragmentation can contribute to symptoms like flashbacks, hypervigilance, and emotional dysregulation that characterize trauma-related conditions. The bilateral stimulation component of EMDR appears to help the brain reprocess these fragmented memory components, integrating them into more complete, adaptive memory networks. Practitioners note that as clients engage in bilateral stimulation while recalling traumatic material, the memories often become less emotionally intense and more like ordinary autobiographical memories—accessible but not overwhelming. EMDR therapy follows a structured eight-phase protocol that ensures safe and effective trauma memory processing through bilateral stimulation. Understanding this framework helps clarify how the approach differs from simply discussing traumatic experiences or exposure therapy. Phase 1: History Taking and Treatment Planning The therapist gathers comprehensive information about your history, identifies specific traumatic memories to target, and develops an individualized treatment plan. This phase establishes therapeutic rapport and determines readiness for trauma processing. Phase 2: Preparation Before beginning bilateral stimulation for trauma processing, therapists teach stabilization techniques and coping skills. This foundation ensures you have resources to manage emotional intensity both during and between sessions. Preparation may involve learning grounding techniques, establishing a "safe place" visualization, or practicing self-regulation strategies. Phase 3: Assessment For each targeted memory, the therapist helps identify the vivid image representing the trauma, associated negative beliefs about yourself, desired positive beliefs, current emotions, physical sensations, and baseline distress levels. This assessment creates specific targets for the bilateral stimulation work. Phase 4: Desensitization This phase involves the core bilateral stimulation for processing traumatic memories. While focusing on the targeted memory components, you simultaneously engage in bilateral stimulation—typically following the therapist's fingers with your eyes for 20-30 seconds at a time. After each set of bilateral stimulation, you briefly report what you notice. The therapist continues this process, allowing your brain to make its own connections and associations, until the memory loses its emotional charge. Phase 5: Installation Once distress decreases, bilateral stimulation continues while strengthening the desired positive belief about yourself in relation to the memory. This phase helps consolidate adaptive perspectives. Phase 6: Body Scan You mentally scan your body while thinking of the incident and positive belief, identifying any residual physical tension or discomfort. Bilateral stimulation addresses any remaining somatic disturbances. Phase 7: Closure Each session ends with stabilization, ensuring you feel grounded before leaving. Therapists provide guidance for managing any processing that continues between sessions. Phase 8: Reevaluation Subsequent sessions begin by assessing progress and identifying any related memories or situations that need addressing. Clinical experience suggests that this structured approach prevents overwhelming flooding while systematically addressing trauma's multiple dimensions—cognitive, emotional, sensory, and somatic. Understanding the neurobiology of trauma helps clarify why bilateral stimulation in EMDR for processing traumatic memories may be effective. Traumatic experiences can overwhelm the brain's normal information processing systems, particularly affecting areas involved in memory, emotion regulation, and threat detection. Research in neuroscience indicates that traumatic memories may become encoded differently than ordinary memories. The amygdala, the brain's threat detection center, can remain hyperactivated in relation to trauma reminders, triggering intense emotional and physiological responses. Meanwhile, areas involved in contextual memory and narrative construction may show reduced activation, contributing to the fragmented, decontextualized quality of traumatic memories. Studies examining neuroimaging during EMDR suggest that bilateral stimulation may facilitate communication between brain regions, particularly between areas involved in emotional processing and those involved in cognitive integration. This enhanced connectivity appears to support the transformation of traumatic memories from fragmented, emotionally overwhelming experiences into integrated autobiographical memories. The bilateral nature of the stimulation may be significant. Some research suggests that alternating left-right input engages both brain hemispheres in the processing work, potentially facilitating integration between emotional and logical processing. However, it's important to note that the precise mechanisms remain an active area of research, and multiple factors likely contribute to EMDR's effectiveness. For those seeking accessible support while working through difficult emotions, tools like Lovon.app provide on-demand resources for processing stress and emotional experiences between therapy sessions. While such tools don't replace professional EMDR therapy, they can offer support for emotional regulation and reflection. Clinical observations suggest that during bilateral stimulation, clients often report spontaneous insights, emotional release, shifts in body sensations, and changed perspectives about themselves and their experiences. These changes appear to reflect genuine memory reconsolidation rather than merely talking about or habituating to distressing content. While EMDR therapy bilateral stimulation shows promise for trauma memory processing, several practical considerations affect its appropriateness and effectiveness for different individuals and situations. Treatment Readiness and Stability EMDR with bilateral stimulation for trauma processing requires sufficient emotional stability to engage with difficult material without becoming overwhelmed. Therapists assess factors like current safety, support systems, substance use, and ability to use coping skills. For individuals with significant dissociation, complex trauma, or current crisis situations, preparatory stabilization work may need to extend longer before beginning trauma-focused bilateral stimulation. Types of Trauma Most Responsive to EMDR Research suggests EMDR demonstrates particular effectiveness for single-incident traumas like accidents, natural disasters, or assault. Complex trauma resulting from repeated childhood experiences may respond to EMDR but often requires longer treatment and additional therapeutic approaches addressing developmental needs, attachment patterns, and identity issues. Bilateral Stimulation Modality Selection While eye movements remain the most researched form of bilateral stimulation in EMDR, some individuals find tactile (tapping, buzzers) or auditory bilateral stimulation more comfortable or accessible. Practitioners adjust the modality based on client preference, physical limitations, or what produces the strongest processing effect. Some people find eye movements tiring or difficult, while others prefer the discrete nature of tactile stimulation. Session Frequency and Treatment Duration Standard EMDR protocols typically involve weekly sessions of 60-90 minutes. Some research examines intensive formats with multiple sessions over several days, which may suit certain situations. The number of sessions needed varies considerably depending on trauma complexity, the number of memories requiring processing, and individual factors. Single-trauma cases might resolve in 3-6 sessions of bilateral stimulation work (plus preparation and closure phases), while complex trauma may require extended treatment. Integration with Other Therapeutic Approaches EMDR using bilateral stimulation for trauma memory processing often works best as part of comprehensive treatment. Many therapists integrate EMDR with other evidence-based approaches like cognitive-behavioral techniques, somatic therapies, or attachment-focused work. Between sessions, individuals might benefit from support tools like Lovon.app for processing daily stressors and maintaining emotional balance. Potential Challenges and Limitations Some individuals experience temporary increases in distressing memories, dreams, or emotions as processing continues between sessions. While generally manageable with preparation and support, these effects require consideration. EMDR may not be appropriate during acute crisis periods or when external circumstances require immediate practical problem-solving rather than memory processing. Additionally, not everyone responds equally to bilateral stimulation. A small percentage of clients find the process ineffective or uncomfortable, and some trauma presentations may benefit more from other therapeutic approaches. Quality EMDR therapy involves ongoing assessment and flexibility to adjust the approach based on individual response. If you're experiencing symptoms that suggest unprocessed trauma—intrusive memories, nightmares, hypervigilance, emotional numbness, avoidance of trauma reminders, or relationship difficulties—seeking evaluation from a mental health professional trained in trauma treatment is an important step. EMDR therapy using bilateral stimulation for trauma memory processing requires specialized training, and therapists certified in EMDR have completed specific coursework, practice, and consultation requirements. Look for licensed mental health professionals (psychologists, licensed clinical social workers, licensed professional counselors, or psychiatrists) with EMDR training verified through professional organizations. An initial consultation can help determine whether EMDR using bilateral stimulation for processing traumatic memories is appropriate for your specific situation, or whether other approaches might be more suitable. Signs that professional help is particularly urgent include:
- Thoughts of self-harm or suicide
- Inability to function in daily activities due to trauma symptoms
- Severe dissociation or loss of time
- Substance use to manage trauma symptoms
- Re-traumatization in current relationships or situations For individuals already in therapy, discussing EMDR as a potential addition or alternative to current treatment can help determine the best path forward. Some therapists incorporate bilateral stimulation techniques within other therapeutic frameworks, while others practice structured EMDR protocols. EMDR therapy using bilateral stimulation for trauma memory processing represents a significant advancement in trauma treatment, offering a structured approach that helps the brain integrate fragmented traumatic memories into adaptive memory networks. By combining focused attention on traumatic material with alternating bilateral stimulation, this approach facilitates natural healing processes that can reduce distress, change negative self-beliefs, and restore emotional balance. Understanding how bilateral stimulation works in EMDR therapy for trauma—from the eight-phase structure to the neurobiological mechanisms—empowers individuals to make informed decisions about treatment options. While EMDR shows particular promise for trauma memory processing, it works best as part of comprehensive care that includes preparation, ongoing support, and integration of therapeutic gains into daily life. If you're considering EMDR or seeking support for trauma-related difficulties, consulting with qualified mental health professionals can help determine the most appropriate approach for your unique circumstances. Whether through specialized trauma therapy, supportive resources, or a combination of approaches, healing from traumatic experiences is possible. Disclaimer: This is general information, not medical advice or diagnosis. If symptoms are severe, affecting your daily life, or you're having thoughts of self-harm — seek professional help. In the US: call or text 988 (Suicide & Crisis Lifeline). For immediate danger: 911 or local emergency services.
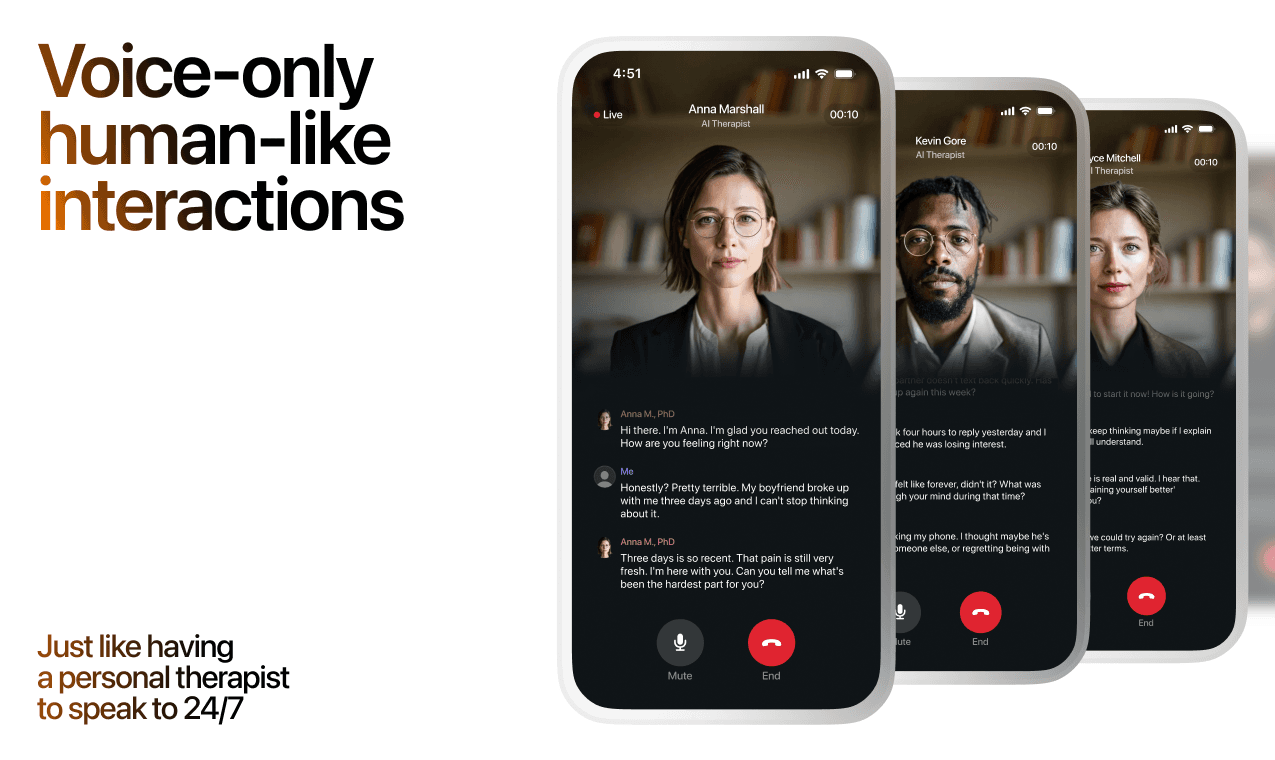
How AI Support Helps You Heal
AI emotional support isn't about replacing human connection — it's about filling the gaps. The moments when you need to talk at 2 AM, when you don't want to burden your friends again, or when you simply need someone to listen without judgment.
Here's what happens in a typical Lovon session:
You share what's on your mind
There's no script, no intake form, no waiting room. You speak or type whatever you're feeling — in your own words, at your own pace.
Lovon validates and explores
Using frameworks from CBT (Cognitive Behavioral Therapy) and motivational interviewing, Lovon acknowledges your feelings first, then gently helps you explore them. No dismissive "just move on" advice.
You build coping skills together
Lovon doesn't just listen — it actively works with you on evidence-based techniques: thought reframing, urge surfing, behavioral experiments, and more.
What a Session with Lovon Looks Like
When to Seek Professional Help
AI support is a valuable tool, but it's not a replacement for professional care. Please consider reaching out to a licensed therapist if you experience any of the following:
- Persistent thoughts of self-harm or suicide
- Inability to perform daily activities (work, eating, sleeping) for more than 2 weeks
- Turning to alcohol or substances to cope
- Intense anger or desire to harm your ex-partner
- Complete emotional numbness that doesn't improve over time
Crisis Resources (US): If you're in immediate danger, call 988 (Suicide & Crisis Lifeline) or text HOME to 741741 (Crisis Text Line). Available 24/7, free, and confidential.
Outside the US? Find a crisis line in your country
Ready to Start?
Your healing journey can begin right now
1 free conversation. No credit card. No judgment. Just a safe space to process what you're going through.
Frequently Asked Questions
Is AI therapy a replacement for a real therapist?
Is my conversation with Lovon AI private?
How is Lovon different from ChatGPT for emotional support?
Can I use Lovon if I'm already seeing a therapist?
Can I try Lovon for free?
About the Author
The Lovon Editorial Team
Mental Health & Wellness Content Team
The Lovon Editorial Team develops mental health and wellness content designed to make psychological concepts accessible and actionable. Our goal is to bridge the gap between clinical research and everyday life - helping you understand why your mind works the way it does and what you can do about it....
Similar Articles
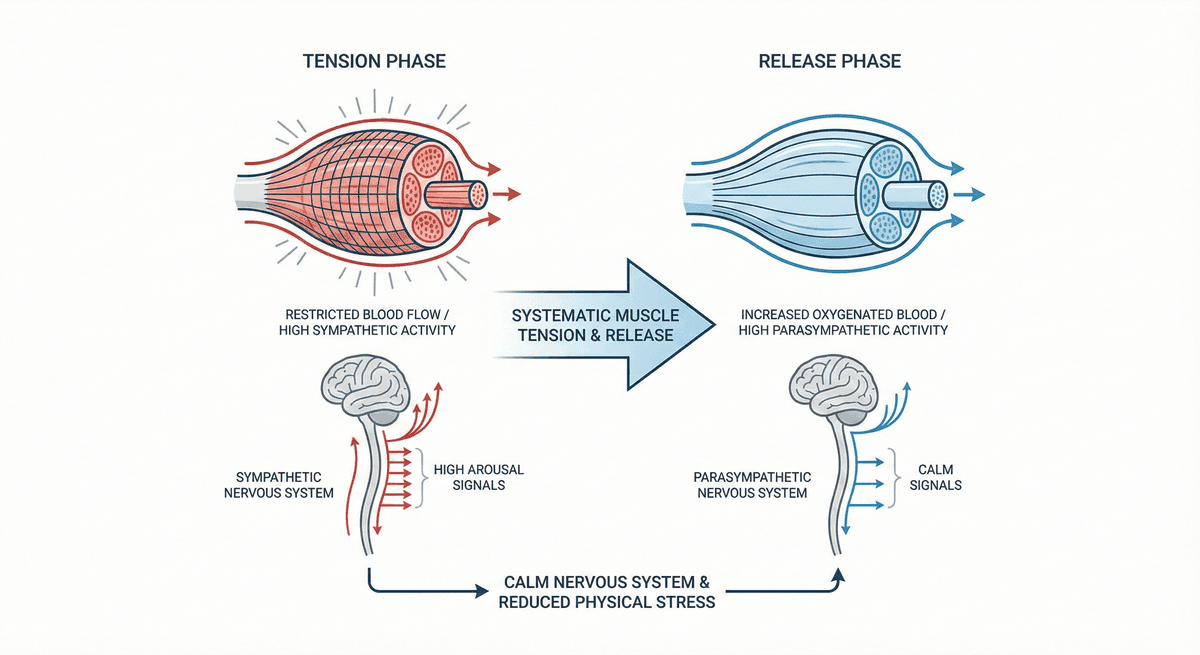
Progressive Muscle Relaxation for Stress Reduction
A systematic muscle group tension and release technique that calms the nervous system and reduces physical stress.
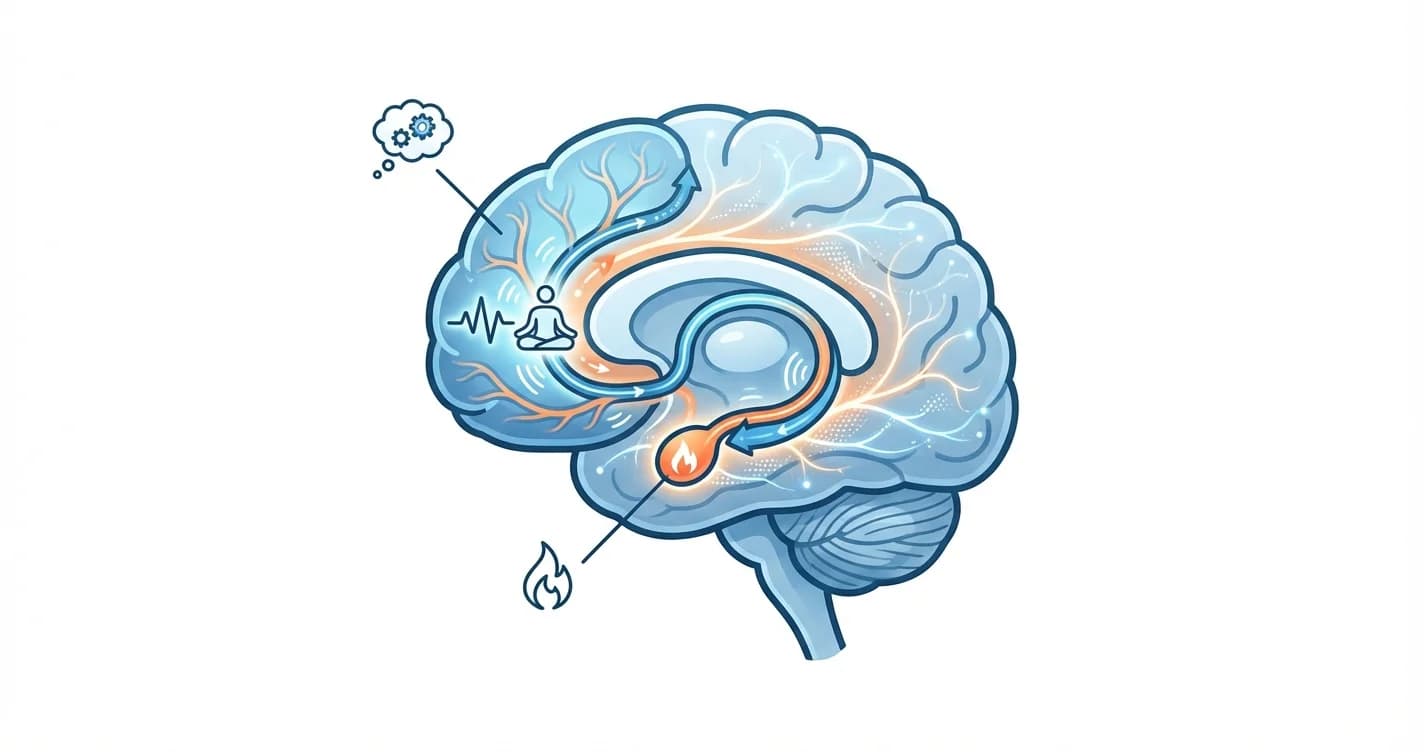
Amygdala and Prefrontal Cortex Connection: Training Emotional Regulation Through Mindfulness
How mindfulness practices reshape neural pathways to strengthen emotional control and reduce reactivity
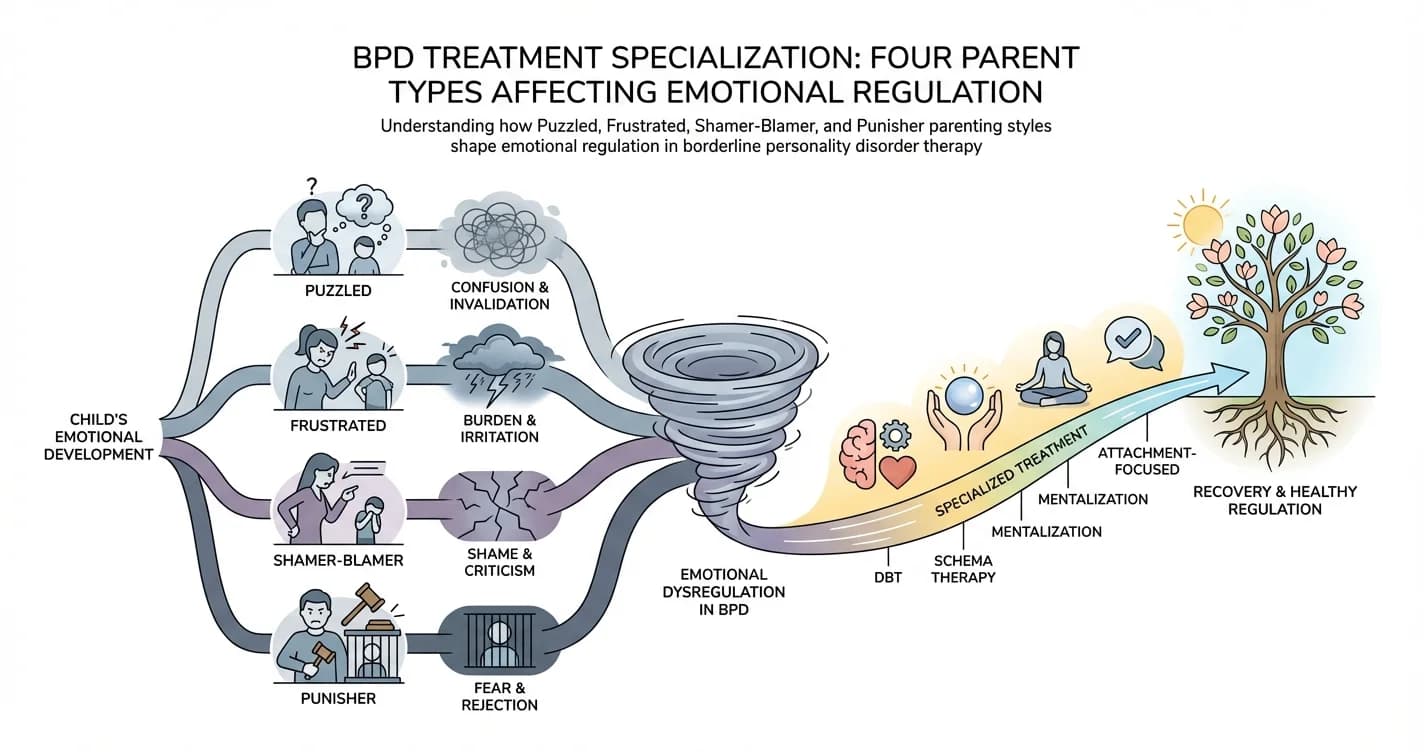
BPD Treatment Specialization: Four Parent Types Affecting Emotional Regulation
For individuals with borderline personality disorder (BPD), emotional regulation difficulties rarely emerge in isolation. Research increasingly suggests that
Disclaimer: This article is for informational purposes only and does not constitute medical advice, diagnosis, or treatment. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition. If you are in crisis or think you may have an emergency, call 988 (Suicide & Crisis Lifeline) or go to the nearest emergency room. Outside the US? Find a crisis line in your country.