Freeze, Flight, and Fawn Trauma Responses as Safety-Seeking Behavioral Patterns
When confronted with perceived danger or overwhelming stress, our nervous system activates automatic protective mechanisms known as trauma responses. The

Key Takeaways
- Abruptly ending conversations when topics become emotionally charged
- Leaving rooms during conflicts or tense interactions
- Avoiding people, places, or situations that trigger anxiety or discomfort
- Staying excessively busy to avoid processing difficult emotions
- Changing topics rapidly when discussions approach vulnerable territory
Introduction
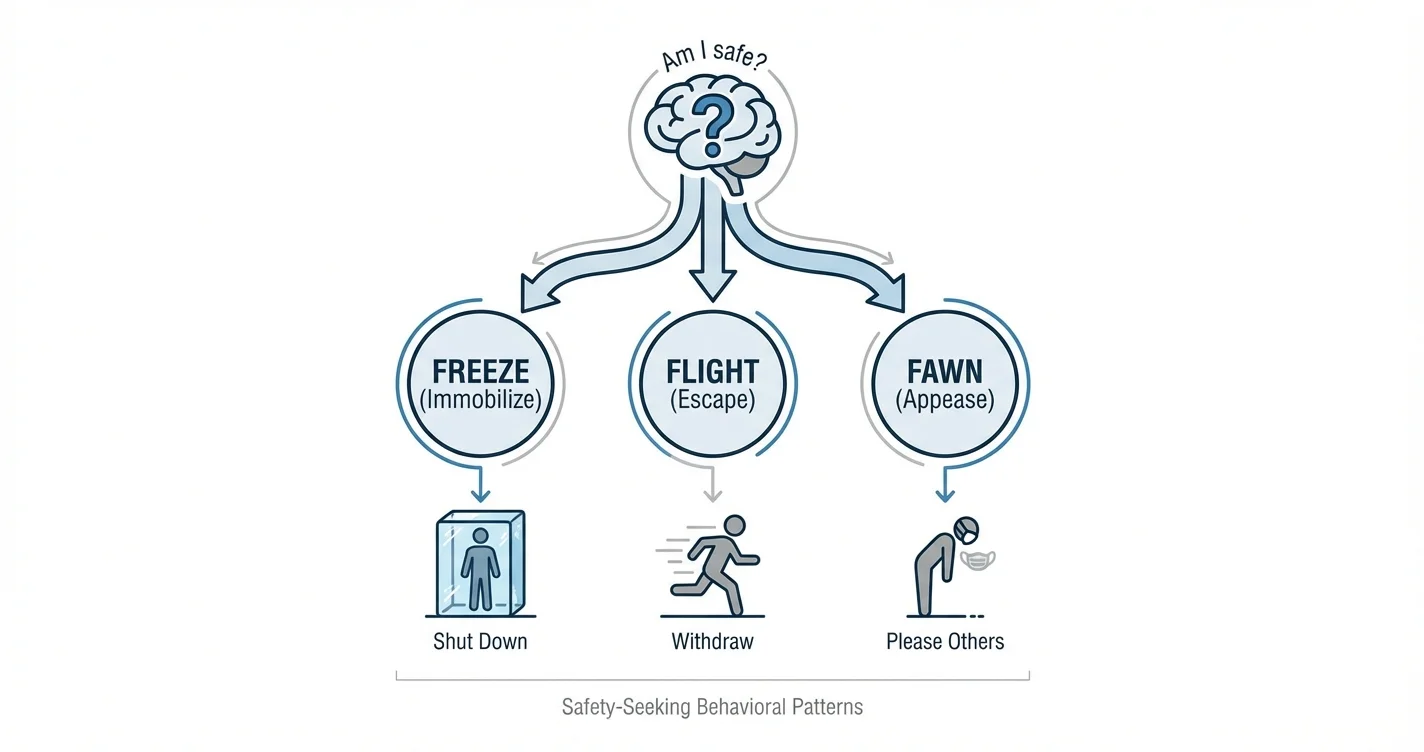
When confronted with perceived danger or overwhelming stress, our nervous system activates automatic protective mechanisms known as trauma responses. The freeze, flight, and fawn trauma responses represent safety-seeking behavioral patterns that evolved to maximize survival in threatening situations. Rather than conscious choices, these reactions emerge from deeply embedded neurobiological pathways designed to protect us when we encounter situations our system interprets as dangerous. Understanding these patterns illuminates why we respond the way we do during conflicts, stressful encounters, or situations that echo past experiences—and how recognizing these responses can help us develop more adaptive coping strategies.
These trauma responses aren't limited to dramatic or life-threatening situations. They activate during everyday interpersonal conflicts, workplace tensions, or moments when we feel emotionally vulnerable. This article explores the mechanisms behind these safety-seeking behavioral patterns, how they manifest in daily life, and practical approaches for working with rather than against these protective responses.
The Neurobiological Foundation of Safety-Seeking Behavioral Patterns
Trauma responses originate in the autonomic nervous system, which operates largely outside conscious awareness to regulate physiological states and survival behaviors. Research suggests that when the brain's threat-detection systems identify potential danger, they trigger rapid physiological changes that prioritize immediate survival over long-term planning or social connection.
The freeze, flight, and fawn trauma responses represent different strategies the nervous system employs based on its assessment of available options. These assessments happen extraordinarily quickly—within fractions of a second—based on both current sensory information and past experiences stored in implicit memory. The system essentially asks: "What gives me the best chance of staying safe right now?"
Flight responses typically activate when escape appears possible, mobilizing the body for rapid movement away from threat. Freeze responses emerge when the system determines that fighting or fleeing won't work, conserving energy and reducing visibility to potential threats. Fawn responses represent a distinctly interpersonal safety strategy: attempting to appease, please, or affiliate with the source of threat to minimize harm.
What makes these patterns particularly relevant to understanding trauma is that they become ingrained through repetition. When certain situations repeatedly trigger specific responses, those pathways strengthen, creating behavioral patterns that may activate even when actual danger isn't present. The nervous system, shaped by past experiences, may interpret situations as threatening that others would perceive as neutral or mildly stressful.
Recognizing Flight Response Patterns in Everyday Life
The flight response manifests as an impulse toward escape, withdrawal, or avoidance when situations feel overwhelming or threatening. This safety-seeking behavioral pattern involves physiological activation—increased heart rate, rapid breathing, heightened alertness—that prepares the body for movement away from perceived danger.
In modern contexts, flight responses rarely involve literal running away. Instead, they appear as:
- Abruptly ending conversations when topics become emotionally charged
- Leaving rooms during conflicts or tense interactions
- Avoiding people, places, or situations that trigger anxiety or discomfort
- Staying excessively busy to avoid processing difficult emotions
- Changing topics rapidly when discussions approach vulnerable territory
- Creating physical or emotional distance in relationships that feel threatening
Flight responses serve an important protective function. They create space between ourselves and what our system perceives as dangerous, allowing the nervous system to downregulate from heightened arousal. Problems emerge when flight becomes the default response to manageable stress, preventing us from developing distress tolerance or addressing relationship issues that require sustained engagement.
People who frequently experience flight responses may describe feeling trapped or restless in situations others find tolerable. They might struggle with commitments that limit their ability to leave, or experience relationship patterns where they withdraw when emotional intensity increases. Understanding flight as a safety-seeking mechanism rather than personal weakness or avoidance can shift how we approach these patterns.
Recognizing the early signs of flight activation—the impulse to leave, the urge to change subjects, the feeling that walls are closing in—creates opportunities for intervention. Some people find it helpful to identify whether the situation genuinely requires escape or whether their nervous system is responding to perceived rather than actual threat.
Understanding Freeze Response as a Protective Mechanism
The freeze response represents a distinct safety-seeking behavioral pattern that activates when the nervous system determines that active responses like flight won't ensure safety. During freeze states, the body enters a state of immobilization characterized by physical stillness, mental numbness, and reduced capacity for active response.
Freeze responses involve different physiological mechanisms than flight. Rather than mobilizing energy for action, freeze states involve a complex shutdown process. Some research suggests this response involves simultaneous activation of both accelerating and braking functions in the autonomic nervous system, creating a state of "frozen watchfulness" where the person remains alert to threat while physically immobilized.
In contemporary situations, freeze responses commonly appear as:
- Going blank or speechless during confrontations or difficult conversations
- Feeling physically stuck or unable to move in stressful situations
- Dissociating or feeling detached from one's body during overwhelming experiences
- Difficulty making decisions when facing multiple competing demands
- Experiencing mind-blanking during exams, presentations, or performance situations
- Numbing out emotionally when feelings become too intense
The freeze response often carries particular shame because it contradicts cultural narratives about "fighting back" or "standing up for yourself." People who freeze during threatening situations may harshly judge themselves for not responding differently. Understanding freeze as an automatic neurobiological safety strategy rather than personal failure provides important context for self-compassion.
Freeze states can range from brief moments of going blank to extended periods of shutdown, dissociation, or collapse. The intensity and duration often correspond to the perceived severity of threat and the person's past experiences with similar situations. For individuals with trauma histories, freeze responses may activate in situations that others wouldn't perceive as particularly threatening, reflecting a nervous system calibrated by past experiences where immobilization offered the best survival strategy.
Working with freeze responses requires patience and gentleness. Forcing ourselves to "just respond" or "snap out of it" typically intensifies the response. Instead, approaches that gently restore a sense of safety—through grounding techniques, supportive presence, or gradual re-engagement—tend to be more effective.
The Fawn Response as Interpersonal Safety-Seeking
The fawn response represents a safety-seeking behavioral pattern oriented around appeasing, pleasing, or affiliating with sources of potential threat. This response emerges from the recognition that safety sometimes depends on managing another person's emotional state or maintaining connection with someone who holds power over us.
Fawn responses involve attempting to reduce danger by making oneself useful, agreeable, or indispensable to the threatening party. This strategy appears frequently in situations where flight isn't possible and where the threat comes from someone on whom we depend or with whom we must maintain a relationship. Clinical observations suggest that fawn responses develop particularly in contexts of prolonged interpersonal threat, such as childhood environments where a caregiver's approval was unpredictable or conditional.
Common manifestations of fawn responses include:
- Automatically agreeing with others' opinions while suppressing your own
- Over-apologizing or taking responsibility for things that aren't your fault
- Difficulty setting boundaries or saying no to requests
- Prioritizing others' needs and feelings to the near-complete exclusion of your own
- Becoming hypervigilant to others' emotional states and adjusting behavior accordingly
- Seeking to be helpful, useful, or indispensable to avoid rejection or conflict
- Losing touch with your own preferences, opinions, and desires
The fawn response differs from genuine generosity, empathy, or cooperativeness. While healthy prosocial behaviors emerge from authentic care and choice, fawn responses are driven by fear and the need to prevent anticipated harm. People experiencing fawn responses often describe feeling compelled to please others, accompanied by anxiety about what might happen if they don't.
This safety-seeking pattern can become deeply embedded in identity and self-concept. Some people come to understand themselves primarily through their usefulness to others, struggling to identify their own needs, preferences, and boundaries separate from what others want from them. This pattern may persist even after leaving the situations that originally necessitated fawn responses, as the nervous system continues operating according to safety strategies that once protected them.
Recognizing fawn responses requires honest self-reflection about motivations behind people-pleasing behaviors. Questions that can illuminate fawn patterns include: "Am I doing this because I genuinely want to, or because I'm afraid of what happens if I don't?" and "Would I feel anxious or unsafe if I said no to this request?"
Tools like Lovon.app can provide a space to explore these patterns without the pressure of managing another person's reaction. Speaking through situations where fawn responses emerged—examining the feelings and fears driving the behavior—can help distinguish between automatic safety responses and authentic choices.
How These Patterns Interact and Shift Across Contexts
Trauma responses don't exist as fixed categories that define a person. Instead, individuals typically move between different safety-seeking behavioral patterns depending on circumstances, relationships, and perceived options. Understanding this fluidity helps explain why someone might freeze in one situation, flee in another, and fawn in a third.
The specific response that activates appears to depend on multiple factors including the nature of the perceived threat, the relationship with the threatening party, available escape routes, past experiences in similar situations, and the person's current physiological state. Some people notice consistent patterns—perhaps typically freezing during conflict—while others experience more variability.
These responses can also occur sequentially. Someone might initially attempt flight, then shift to freeze when escape appears impossible, or begin with fawn responses that transition to flight when appeasement strategies fail. Recognizing these shifts provides valuable information about what your nervous system perceives about safety and available options in different moments.
Context significantly influences which responses activate. With certain people—perhaps authority figures or those who remind us of past threatening relationships—fawn responses might predominate. In other situations where the threat feels less interpersonal, flight or freeze might activate instead. This context-dependence explains why we might respond quite differently to similar situations depending on subtle environmental or relational cues.
Working with these patterns involves developing awareness of which responses tend to activate in different contexts and what triggers those shifts. This awareness creates opportunities for gradual change. Rather than attempting to eliminate these protective responses entirely, the goal involves expanding the range of available responses and increasing the space between trigger and reaction.
Practical Approaches for Working With Safety-Seeking Responses
Recognizing freeze, flight, and fawn trauma responses as safety-seeking behavioral patterns opens pathways for working with rather than against these mechanisms. Effective approaches acknowledge these responses as protective while gently expanding our capacity to respond flexibly to different situations.
Building awareness without judgment forms the foundation for all other interventions. This involves noticing when these responses activate—the physical sensations, thoughts, and impulses that accompany them—without immediately trying to change them. Simple observation: "I'm noticing the urge to leave this conversation" or "I'm aware I've gone blank and can't think clearly right now" creates valuable space between automatic response and action.
Grounding techniques help regulate nervous system arousal, particularly during flight and freeze responses. These might include naming objects in your environment, feeling your feet on the floor, or engaging in gentle movement. The goal involves signaling safety to a nervous system stuck in threat-detection mode.
Gradual exposure and building distress tolerance allows for slowly expanding the range of situations you can stay present in rather than automatically fleeing or freezing. This works best when approached incrementally, starting with situations that trigger mild responses rather than overwhelming ones. Successfully staying present through manageable stress gradually updates the nervous system's threat assessments.
Boundary practice addresses fawn responses by creating small, low-stakes opportunities to say no, express preferences, or prioritize your needs. This might begin with declining minor requests from safe people, gradually building toward setting boundaries in more challenging relationships. Each successful boundary-setting experience provides evidence that disappointing others doesn't necessarily result in the feared consequences.
Working with trusted support significantly enhances this process. Therapists specializing in trauma can provide structured approaches for addressing these patterns. Between professional sessions, on-demand resources like Lovon.app offer opportunities to process experiences and explore patterns as they emerge, helping you understand your responses and develop alternative strategies in real-time.
Somatic practices that work directly with the body's stored responses—including certain forms of yoga, breathwork, or somatic experiencing—may help release some of the physiological patterns associated with chronic activation of these responses. These approaches recognize that trauma responses are embodied, not just cognitive, requiring body-oriented interventions.
When These Patterns Signal the Need for Professional Support
While understanding and working with trauma responses can happen independently, certain signs indicate that professional support would be beneficial or necessary. Safety-seeking behavioral patterns that significantly impair functioning, persist despite self-help efforts, or involve safety concerns warrant consultation with mental health professionals.
Consider seeking professional help when:
- Freeze, flight, or fawn responses activate so frequently or intensely that they interfere with work, relationships, or daily functioning
- You experience persistent dissociation, feeling disconnected from yourself or reality
- Safety-seeking behaviors involve self-harm, substance use, or other harmful coping strategies
- You're unable to engage in important relationships or activities due to these patterns
- Past trauma continues significantly impacting present functioning despite efforts to address it
- You're experiencing intrusive memories, flashbacks, or nightmares alongside these responses
Therapists trained in trauma-focused approaches—including EMDR, somatic experiencing, sensorimotor psychotherapy, or trauma-focused cognitive behavioral therapy—can provide structured support for addressing these patterns at their roots. These approaches work directly with how traumatic experiences are stored in memory and activated in present situations.
For individuals whose safety-seeking patterns developed in childhood or through prolonged relational trauma, longer-term therapeutic work addressing attachment patterns and core beliefs about safety may be beneficial. This work helps update the implicit learning that drives automatic responses, gradually shifting from hypervigilant threat-detection toward more nuanced assessments of safety and danger.
Medication may support some individuals experiencing intense anxiety, hypervigilance, or other symptoms that maintain chronic nervous system activation. Discussing medication options with a psychiatrist or prescriber can complement therapeutic work, potentially making it more accessible by reducing symptom intensity.
Conclusion
The freeze, flight, and fawn trauma responses represent sophisticated safety-seeking behavioral patterns evolved to protect us from harm. Rather than flaws or weaknesses, these responses reflect our nervous system's attempts to navigate situations it perceives as threatening based on both present circumstances and past experiences. Understanding these patterns as adaptive—even when they no longer serve us in current contexts—opens pathways for self-compassion and meaningful change.
Recognition forms the essential first step: noticing when these responses activate, what triggers them, and how they manifest in your particular experience. This awareness, combined with approaches that gently expand your window of tolerance and update your nervous system's threat assessments, can gradually shift these patterns. The process requires patience, as deeply embedded safety responses don't change through willpower or quick fixes, but through repeated experiences that teach your nervous system new information about safety and danger.
Whether through professional therapy, peer support, self-directed learning, or on-demand resources that help you process experiences as they unfold, working with these trauma responses involves honoring their protective origins while creating space for more flexible, adaptive responses. Your nervous system developed these patterns for good reason—and with the right support, it can learn new ways of seeking safety that serve your current life and relationships.
Disclaimer: This is general information, not medical advice or diagnosis. If symptoms are severe, affecting your daily life, or you're having thoughts of self-harm—seek professional help. In the US: call or text 988 (Suicide & Crisis Lifeline). For immediate danger: 911 or local emergency services.
How AI Support Helps You Heal
AI emotional support isn't about replacing human connection — it's about filling the gaps. The moments when you need to talk at 2 AM, when you don't want to burden your friends again, or when you simply need someone to listen without judgment.
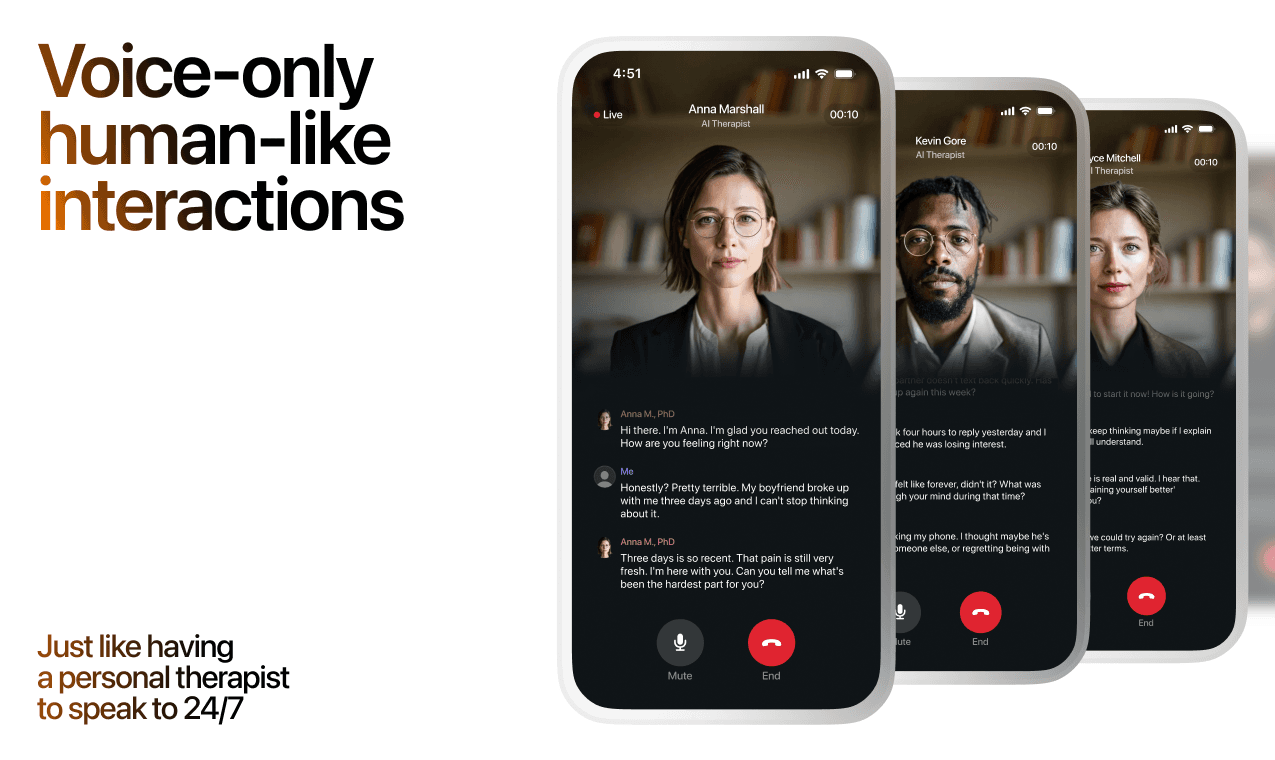
Here's what happens in a typical Lovon session:
You share what's on your mind
There's no script, no intake form, no waiting room. You speak or type whatever you're feeling — in your own words, at your own pace.
Lovon validates and explores
Using frameworks from CBT (Cognitive Behavioral Therapy) and motivational interviewing, Lovon acknowledges your feelings first, then gently helps you explore them. No dismissive "just move on" advice.
You build coping skills together
Lovon doesn't just listen — it actively works with you on evidence-based techniques: thought reframing, urge surfing, behavioral experiments, and more.
What a Session with Lovon Looks Like
When to Seek Professional Help
AI support is a valuable tool, but it's not a replacement for professional care. Please consider reaching out to a licensed therapist if you experience any of the following:
- Persistent thoughts of self-harm or suicide
- Inability to perform daily activities (work, eating, sleeping) for more than 2 weeks
- Turning to alcohol or substances to cope
- Intense anger or desire to harm your ex-partner
- Complete emotional numbness that doesn't improve over time
Crisis Resources (US): If you're in immediate danger, call 988 (Suicide & Crisis Lifeline) or text HOME to 741741 (Crisis Text Line). Available 24/7, free, and confidential.
Outside the US? Find a crisis line in your country
Ready to Start?
Your healing journey can begin right now
1 free conversation. No credit card. No judgment. Just a safe space to process what you're going through.
Frequently Asked Questions
Is AI therapy a replacement for a real therapist?
Is my conversation with Lovon AI private?
How is Lovon different from ChatGPT for emotional support?
Can I use Lovon if I'm already seeing a therapist?
Can I try Lovon for free?
About the Author
The Lovon Editorial Team
Mental Health & Wellness Content Team
The Lovon Editorial Team develops mental health and wellness content designed to make psychological concepts accessible and actionable. Our goal is to bridge the gap between clinical research and everyday life - helping you understand why your mind works the way it does and what you can do about it....
Similar Articles
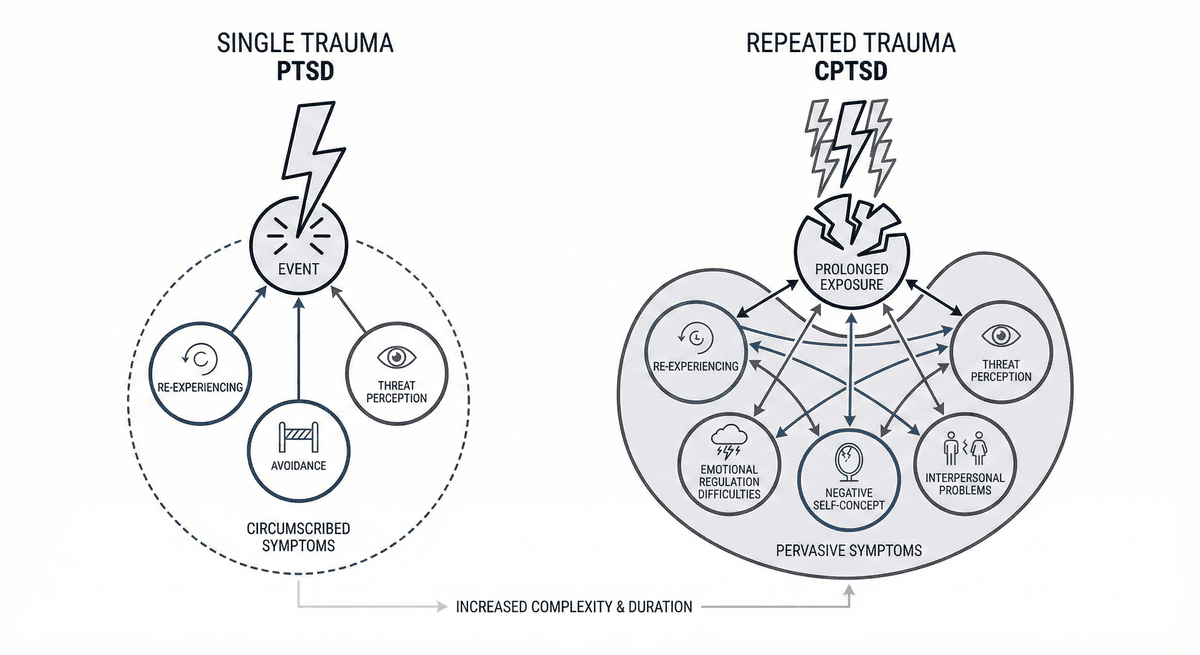
PTSD vs CPTSD: Single Trauma vs Repeated Trauma Symptom Differences
Learn how PTSD from a single traumatic event differs from CPTSD shaped by repeated trauma, including symptom patterns and treatment approaches.
Amygdala and Prefrontal Cortex Connection: Training Emotional Regulation Through Mindfulness
How mindfulness practices reshape neural pathways to strengthen emotional control and reduce reactivity
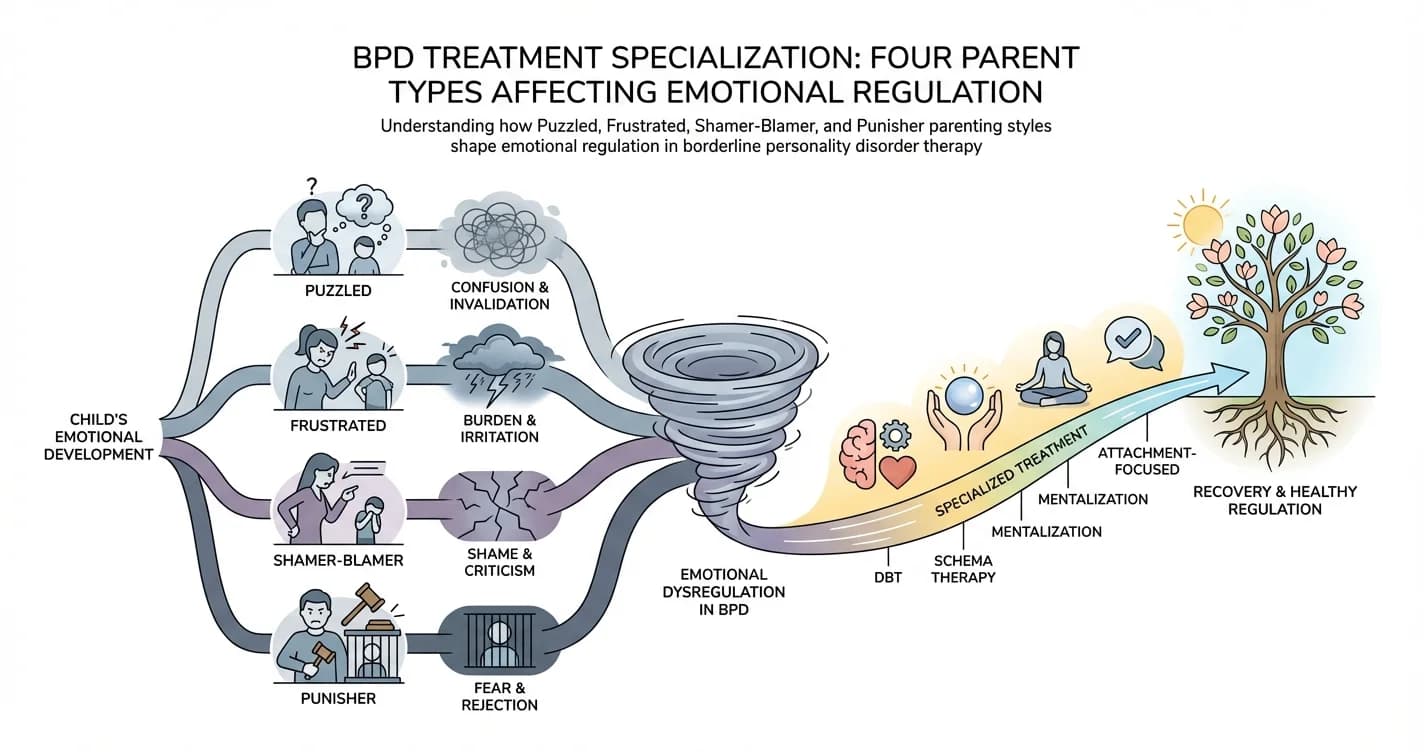
BPD Treatment Specialization: Four Parent Types Affecting Emotional Regulation
For individuals with borderline personality disorder (BPD), emotional regulation difficulties rarely emerge in isolation. Research increasingly suggests that
Disclaimer: This article is for informational purposes only and does not constitute medical advice, diagnosis, or treatment. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition. If you are in crisis or think you may have an emergency, call 988 (Suicide & Crisis Lifeline) or go to the nearest emergency room. Outside the US? Find a crisis line in your country.