How to Heal Trauma When Time Doesn't Help
"Time heals all wounds" is one of the most commonly offered reassurances after trauma, yet for many people, years can pass without the expected relief.

Key Takeaways
- Difficulty maintaining relationships, employment, or daily responsibilities due to trauma symptoms
- Intrusive memories, flashbacks, or nightmares that disrupt functioning
- Severe anxiety, depression, or emotional numbness that doesn't improve with self-help approaches
- Avoidance patterns that significantly limit your life
- Substance use to manage trauma-related distress
Introduction
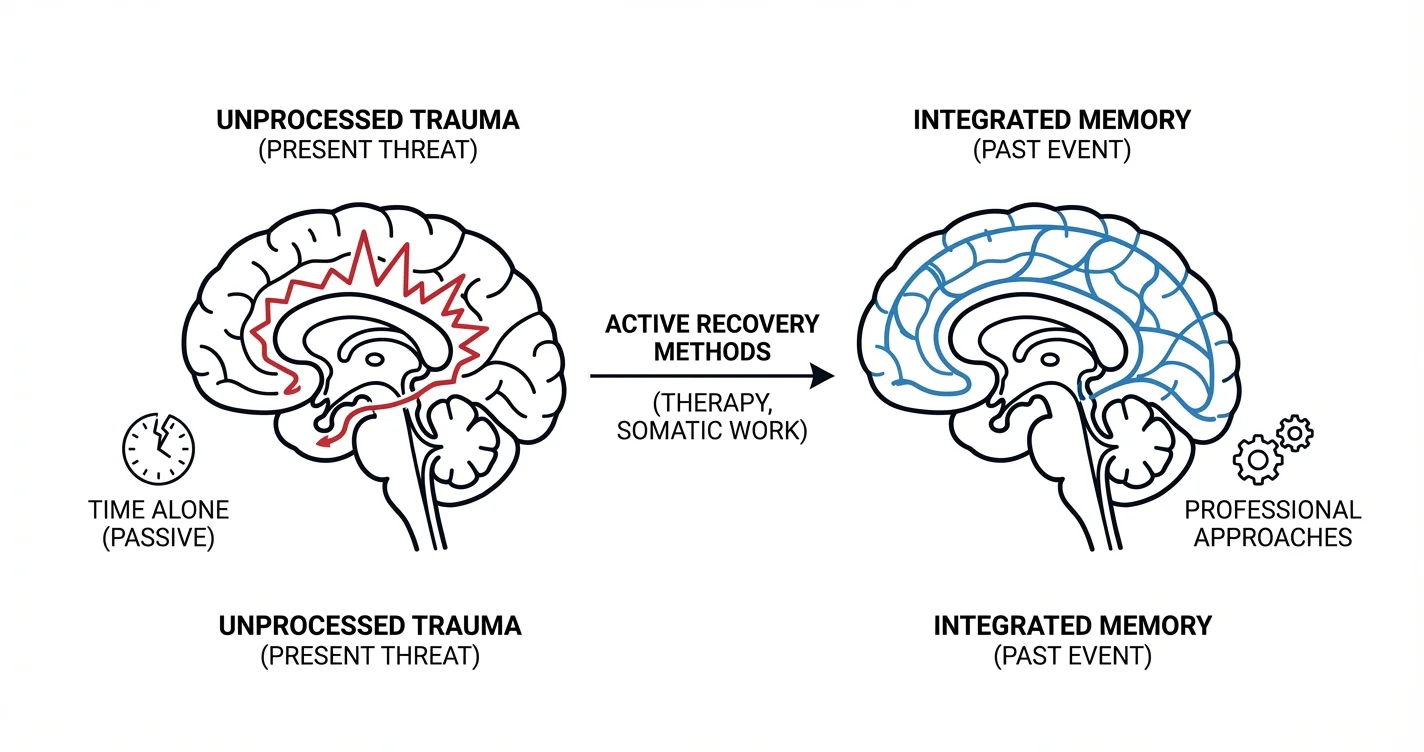
"Time heals all wounds" is one of the most commonly offered reassurances after trauma, yet for many people, years can pass without the expected relief. When intrusive memories, emotional reactivity, or avoidance patterns persist despite the passage of months or years, it becomes clear that time alone may not be sufficient. Understanding how to heal trauma when time doesn't help requires moving beyond passive waiting and engaging active recovery strategies. Research suggests that unprocessed trauma can remain encoded in ways that don't naturally fade with time, requiring intentional intervention to address. This guide explores why some traumatic experiences resist natural healing, what active approaches professionals recommend, and practical steps for moving toward recovery when simply waiting hasn't worked.
Why Time Alone Doesn't Always Heal Trauma
The adage about time healing wounds applies well to many difficult life experiences—breakups, disappointments, losses—where emotional distance naturally reduces intensity. Trauma, however, operates differently in the brain and body. Traumatic experiences appear to be encoded through different neurobiological pathways than ordinary memories, involving regions associated with threat detection and survival rather than narrative processing.
When a traumatic event occurs, the brain's threat-response systems may prioritize immediate survival over coherent memory formation. This can result in fragmented memories that lack the normal contextual information—time, sequence, resolution—that helps the brain file experiences as "past" rather than "present." Without this contextual processing, traumatic memories may continue triggering the same physiological responses years later, as if the threat is still occurring.
Studies indicate that avoidance—a natural response to trauma—can actually prevent the processing necessary for healing. When reminders of trauma are consistently avoided, the brain never receives corrective information that the danger has passed. This keeps the traumatic memory in a kind of suspended state, unintegrated and unchanged by time. Additionally, trauma can affect stress-response systems in ways that create ongoing physiological dysregulation, independent of conscious memory. This means someone might experience anxiety, hypervigilance, or emotional numbness as ongoing symptoms, even when they're not actively thinking about the traumatic event.
It's important to acknowledge that trauma responses vary significantly between individuals. Genetic factors, previous experiences, available support, and the nature of the trauma all contribute to how these patterns develop and persist.
Active Trauma Processing Approaches That Professionals Recommend
When time hasn't brought relief, evidence-based therapeutic approaches offer active methods for processing traumatic experiences. These approaches share a common principle: they help the brain recode traumatic memories in ways that reduce their emotional intensity and integrate them as past events rather than present threats.
Trauma-focused cognitive behavioral therapy involves gradually, safely engaging with trauma-related thoughts and memories in a controlled therapeutic environment. This approach helps identify patterns of thinking that maintain distress and develop alternative interpretations. The gradual exposure component allows the nervous system to learn that remembering the trauma is not itself dangerous, which can reduce avoidance and the power of intrusive memories.
Eye Movement Desensitization and Reprocessing (EMDR) uses bilateral stimulation—typically guided eye movements—while processing traumatic memories. Research suggests this approach may facilitate the brain's natural information-processing mechanisms, helping traumatic memories become less vivid and emotionally charged. Many people report significant reduction in trauma symptoms after a course of EMDR, though how and why it works continues to be studied.
Somatic approaches focus on the body's trauma responses rather than primarily on narrative or cognitive processing. Techniques like Somatic Experiencing recognize that trauma can become "stored" in physical patterns—chronic tension, shutdown responses, or hyperarousal—that persist independently of conscious thought. These approaches help people develop awareness of bodily sensations and gradually release stuck survival responses. For some individuals, particularly those with complex or preverbal trauma, body-centered approaches may access material that talk therapy alone cannot.
Internal Family Systems (IFS) therapy addresses trauma by working with different "parts" of the psyche that hold protective roles. This approach recognizes that people often develop internal protective mechanisms in response to trauma—parts that avoid, parts that criticize, parts that hold painful emotions. IFS helps people understand these protective patterns with compassion and gradually access and heal the wounded parts they protect. This can be particularly helpful for people experiencing internal conflict about their trauma or struggling with shame.
Different approaches work better for different people and different types of trauma. A therapist specializing in trauma can help determine which approach might be most appropriate for your specific situation.
Practical Steps for Active Trauma Recovery
Moving from understanding to action requires creating conditions that support healing while respecting your current capacity and safety. These steps can complement professional treatment or help you prepare for therapeutic work.
Establish baseline safety and stability first. Before engaging directly with traumatic material, it's important to have sufficient external stability and internal resources. This might include stable housing, basic physical health, support systems, and emotion-regulation skills. Research indicates that attempting trauma processing before establishing this foundation can be overwhelming and counterproductive. Skills like grounding techniques, breathing exercises, and identifying what helps you feel safe in the present moment create the foundation for deeper work.
Identify your window of tolerance. Trauma healing involves gradually expanding your capacity to experience difficult emotions and memories without becoming overwhelmed or shutting down. Learning to recognize when you're within your "window of tolerance"—able to engage with challenging material while staying present—versus when you're in hyperarousal (panic, rage, overwhelming anxiety) or hypoarousal (numbness, dissociation, shutdown) helps you pace your recovery appropriately.
Work with rather than against your nervous system. Effective trauma recovery involves helping your nervous system update its threat assessments rather than forcing yourself through triggers. This might mean starting with smaller, less overwhelming aspects of the trauma and gradually building toward more difficult material. It involves noticing what creates a sense of safety and gradually pairing trauma-related material with those safety signals, allowing your nervous system to learn new associations.
Tools like Lovon.app can provide accessible support for processing emotions and stress between therapy sessions, offering a space to talk through difficult feelings as they arise without waiting for your next scheduled appointment. Being able to process experiences soon after they occur can prevent accumulation of unprocessed material that compounds over time.
Address maintaining factors, not just original trauma. Sometimes what keeps trauma active isn't just the original event, but current circumstances that echo traumatic dynamics. This might include ongoing unsafe relationships, chronic stress that keeps your nervous system in high alert, or lack of agency in important life areas. Identifying and addressing these maintaining factors—which may require practical changes in life circumstances, relationships, or daily routines—can be as important as processing the original trauma.
When Standard Trauma Therapy Isn't Working
If you've tried therapy for trauma without experiencing meaningful change, several factors might be at play. Recognizing these can help you adjust your approach rather than conclude that you're simply unable to heal.
Therapeutic fit matters significantly. Not all therapists have specialized training in trauma, and even among trauma specialists, therapeutic style and approach vary. A therapist might be highly skilled but not the right match for your particular needs or personality. Working with someone who specializes specifically in trauma and whose approach resonates with you can make a substantial difference. Some people find that after years of traditional talk therapy with limited results, a few months with a trauma-specialized therapist using targeted approaches creates meaningful change.
Timing and readiness vary. Sometimes therapy doesn't work not because of the approach but because other factors—ongoing instability, active substance use, extreme stress—create conditions where trauma processing isn't safe or possible yet. This doesn't mean you can't heal; it means the current focus might need to be on stabilization rather than direct trauma work.
Complex trauma may require longer, different treatment. Developmental trauma or repeated traumatic experiences often create more pervasive impacts than single-incident trauma. These may affect identity, relationships, and emotional regulation in ways that require longer-term, relationship-focused therapy rather than symptom-focused approaches. If your trauma occurred in childhood or involved caregivers, approaches designed for adult single-incident trauma may not address the core issues.
Medication might be a helpful component. For some people, trauma symptoms include depression, anxiety, or sleep disturbances severe enough that they interfere with daily functioning and the capacity to engage in therapy. Discussing medication options with a psychiatrist or prescriber doesn't mean therapy "failed"—for some people, medication helps stabilize symptoms enough that therapeutic work becomes more accessible.
Services like Lovon.app can complement professional treatment by offering on-demand support when difficult feelings arise outside scheduled sessions, helping you process emotions as they occur rather than carrying them until your next appointment.
Understanding Complex and Developmental Trauma
Not all trauma looks the same, and recognizing different types helps explain why some wounds persist despite time and even initial treatment attempts. Complex trauma—resulting from repeated or prolonged traumatic experiences, particularly in childhood—can create distinct patterns that don't necessarily respond to approaches designed for single-incident trauma.
When trauma occurs in childhood, particularly in relationships with caregivers, it can affect development in pervasive ways. While early experiences play a significant role, genetic factors and individual temperament also contribute to how these patterns develop. The result may include difficulties with emotional regulation, relationship patterns, sense of self, and trust that extend beyond specific traumatic memories.
Complex trauma might manifest less as specific flashbacks and more as ongoing relationship difficulties, chronic feelings of emptiness or shame, difficulty trusting others, or patterns of self-sabotage. These impacts often aren't consciously connected to specific traumatic events, making them harder to recognize as trauma-related. This is why time alone is particularly ineffective—these patterns are woven into how someone relates to themselves and others, requiring active work to identify and change.
Treatment for complex trauma typically involves longer-term therapeutic relationships where the therapy relationship itself becomes part of healing. Learning to trust, establishing boundaries, experiencing rupture and repair, and developing more integrated self-understanding happen gradually through the therapeutic relationship, not just through processing specific memories.
When to Seek Professional Help
If you're experiencing symptoms that significantly affect your daily life, professional support is important. Specific signs that indicate the need for professional help include:
- Difficulty maintaining relationships, employment, or daily responsibilities due to trauma symptoms
- Intrusive memories, flashbacks, or nightmares that disrupt functioning
- Severe anxiety, depression, or emotional numbness that doesn't improve with self-help approaches
- Avoidance patterns that significantly limit your life
- Substance use to manage trauma-related distress
- Thoughts of self-harm or feeling unsafe
Professionals who can help include trauma-specialized therapists, psychologists, psychiatrists, and counselors with specific training in evidence-based trauma treatments. When seeking a therapist, it's appropriate to ask about their specific training and experience with trauma, what approaches they use, and whether they have experience with your particular type of trauma.
For complex or developmental trauma, look for professionals trained in approaches specifically designed for these presentations, such as schema therapy, psychodynamic therapy, or specialized complex trauma protocols. Self-help strategies and support tools can complement professional treatment but don't replace it when symptoms are severe or significantly impair functioning.
Conclusion: Moving Beyond Waiting to Active Healing
Understanding how to heal trauma when time doesn't help means shifting from passive hoping to active engagement with recovery. Time creates distance from traumatic events, but it doesn't automatically provide the processing, integration, and nervous system updating that allows trauma to be filed as truly "past." Research suggests that trauma operates through specific neurobiological mechanisms that may require targeted intervention to change. This isn't a failure on your part—it's simply how traumatic encoding works for some experiences and some people.
Active approaches—whether trauma-focused therapy, somatic work, or combinations of professional treatment and support resources—offer pathways forward when waiting hasn't brought relief. The specific approach that works best varies between individuals, and finding the right fit may require trying different options or working with different professionals. What works differs from person to person, and healing isn't linear—periods of progress often alternate with setbacks, which is a normal part of recovery.
Beginning with establishing safety, developing resources, and finding appropriate professional support creates the foundation for deeper trauma work. Tools like Lovon.app can provide accessible, on-demand support for processing emotions and stress as they arise, complementing professional treatment with immediate availability. Most importantly, if years have passed without improvement, this doesn't mean you can't heal—it means that active, intentional approaches designed specifically for trauma may be needed to create the change that time alone hasn't provided.
Disclaimer: This is general information, not medical advice or diagnosis. If symptoms are severe, affecting your daily life, or you're having thoughts of self-harm—seek professional help. In the US: call or text 988 (Suicide & Crisis Lifeline). For immediate danger: 911 or local emergency services.
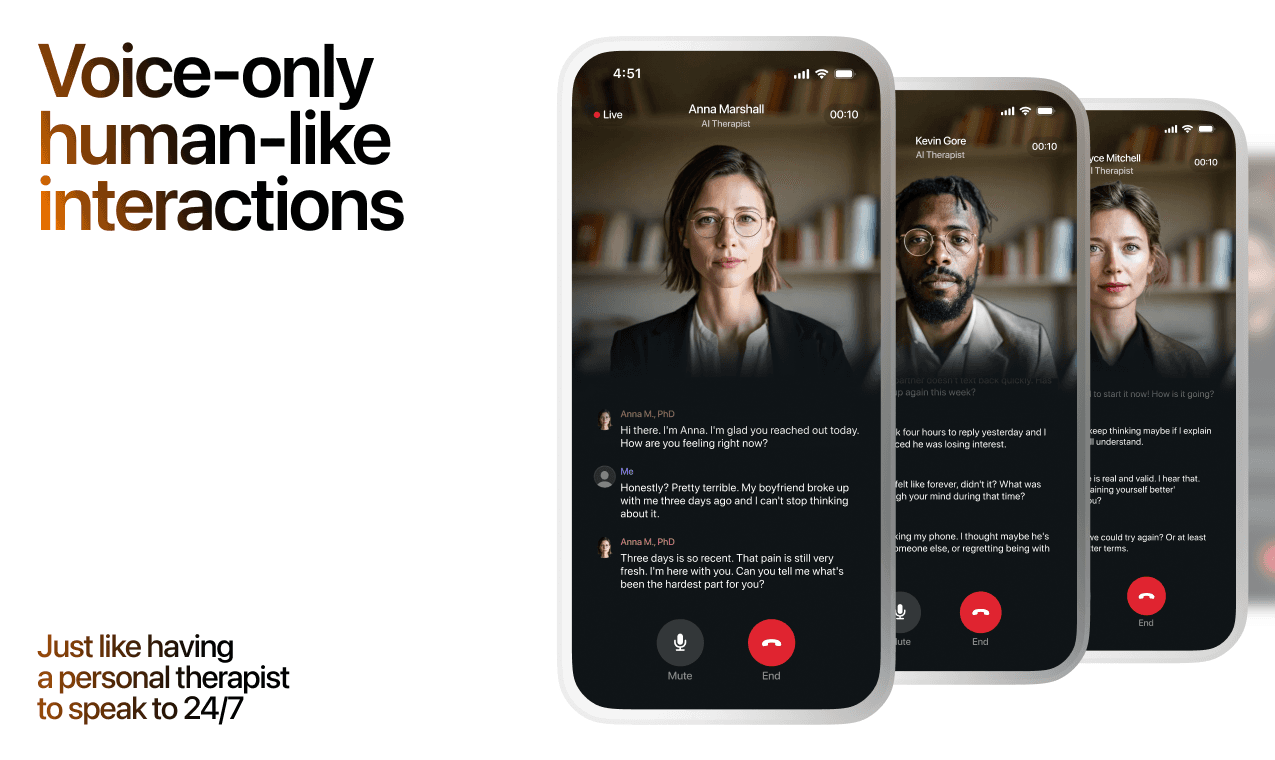
How AI Support Helps You Heal
AI emotional support isn't about replacing human connection — it's about filling the gaps. The moments when you need to talk at 2 AM, when you don't want to burden your friends again, or when you simply need someone to listen without judgment.
Here's what happens in a typical Lovon session:
You share what's on your mind
There's no script, no intake form, no waiting room. You speak or type whatever you're feeling — in your own words, at your own pace.
Lovon validates and explores
Using frameworks from CBT (Cognitive Behavioral Therapy) and motivational interviewing, Lovon acknowledges your feelings first, then gently helps you explore them. No dismissive "just move on" advice.
You build coping skills together
Lovon doesn't just listen — it actively works with you on evidence-based techniques: thought reframing, urge surfing, behavioral experiments, and more.
What a Session with Lovon Looks Like
When to Seek Professional Help
AI support is a valuable tool, but it's not a replacement for professional care. Please consider reaching out to a licensed therapist if you experience any of the following:
- Persistent thoughts of self-harm or suicide
- Inability to perform daily activities (work, eating, sleeping) for more than 2 weeks
- Turning to alcohol or substances to cope
- Intense anger or desire to harm your ex-partner
- Complete emotional numbness that doesn't improve over time
Crisis Resources (US): If you're in immediate danger, call 988 (Suicide & Crisis Lifeline) or text HOME to 741741 (Crisis Text Line). Available 24/7, free, and confidential.
Outside the US? Find a crisis line in your country
Ready to Start?
Your healing journey can begin right now
1 free conversation. No credit card. No judgment. Just a safe space to process what you're going through.
Frequently Asked Questions
Is AI therapy a replacement for a real therapist?
Is my conversation with Lovon AI private?
How is Lovon different from ChatGPT for emotional support?
Can I use Lovon if I'm already seeing a therapist?
Can I try Lovon for free?
About the Author
The Lovon Editorial Team
Mental Health & Wellness Content Team
The Lovon Editorial Team develops mental health and wellness content designed to make psychological concepts accessible and actionable. Our goal is to bridge the gap between clinical research and everyday life - helping you understand why your mind works the way it does and what you can do about it....
Similar Articles
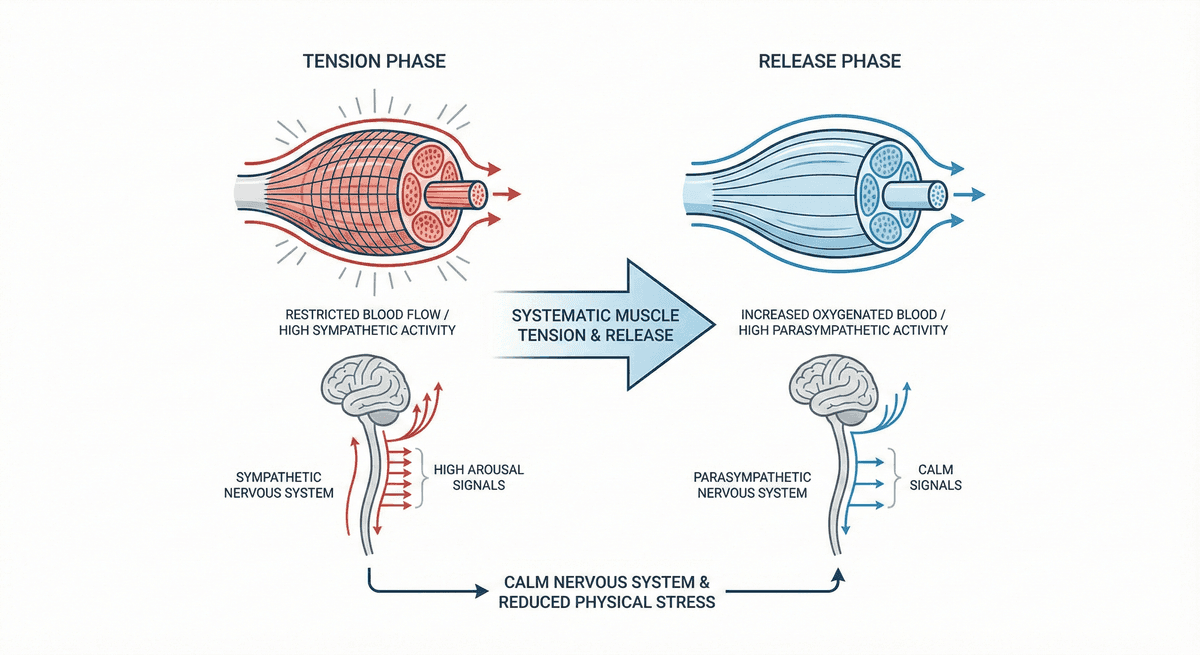
Progressive Muscle Relaxation for Stress Reduction
A systematic muscle group tension and release technique that calms the nervous system and reduces physical stress.
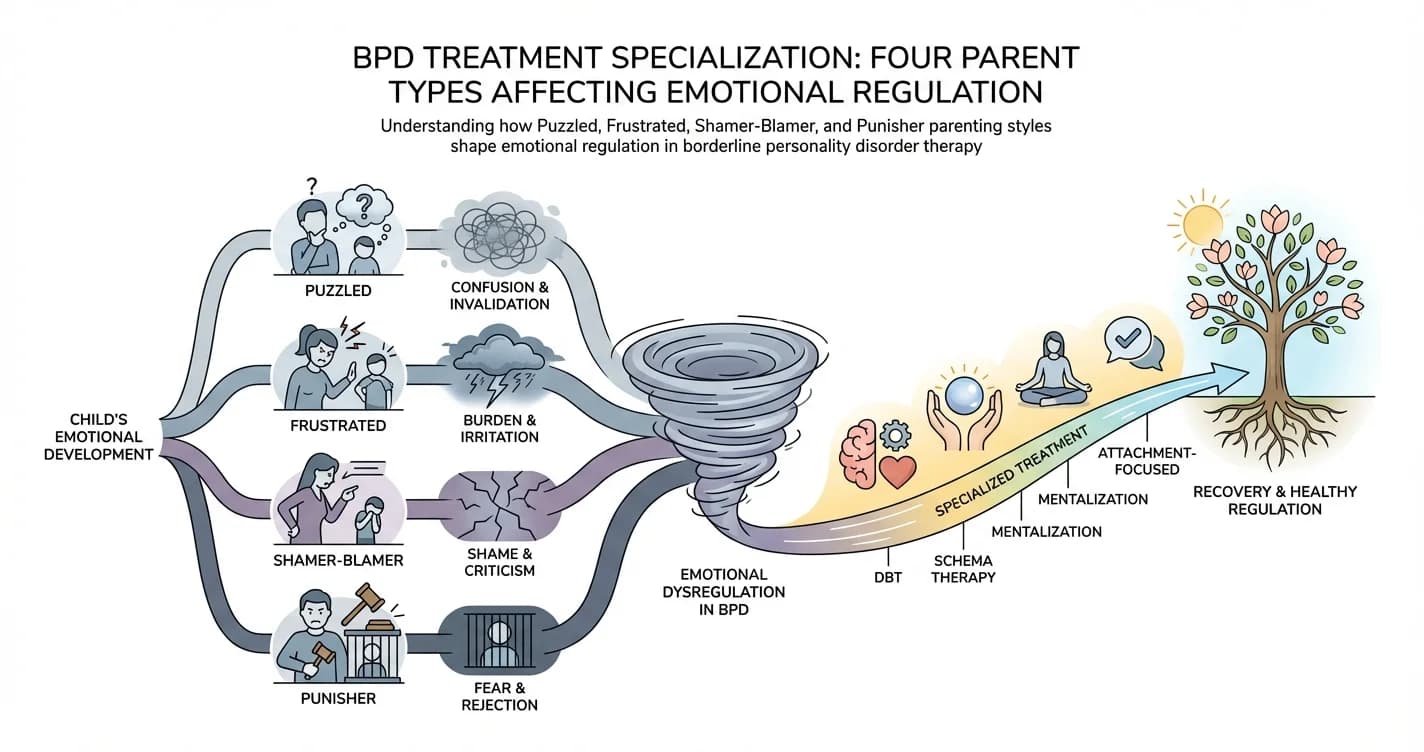
BPD Treatment Specialization: Four Parent Types Affecting Emotional Regulation
For individuals with borderline personality disorder (BPD), emotional regulation difficulties rarely emerge in isolation. Research increasingly suggests that
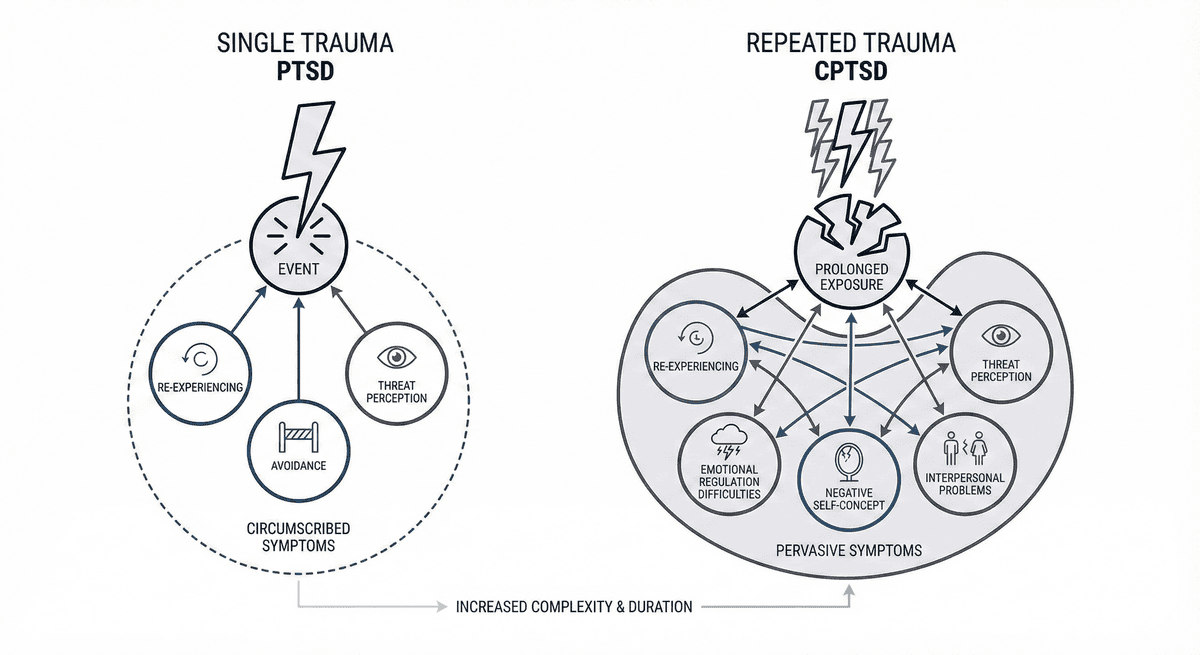
PTSD vs CPTSD: Single Trauma vs Repeated Trauma Symptom Differences
Learn how PTSD from a single traumatic event differs from CPTSD shaped by repeated trauma, including symptom patterns and treatment approaches.
Disclaimer: This article is for informational purposes only and does not constitute medical advice, diagnosis, or treatment. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition. If you are in crisis or think you may have an emergency, call 988 (Suicide & Crisis Lifeline) or go to the nearest emergency room. Outside the US? Find a crisis line in your country.