How to Regulate Nervous System Trauma with Somatic Practices
When trauma lives in the body, words alone often aren't enough to heal it. Traditional talk therapy can provide valuable insights, but many people find...

Key Takeaways
- Feeling your feet on the floor and noticing the support beneath you
- Pressing your hands gently against a wall or surface and noticing the resistance
- Looking around the room and naming objects you see in different colors
- Noticing sounds around you, both near and far
- Feeling the weight of your body in your chair or the texture of clothing against your skin
Introduction
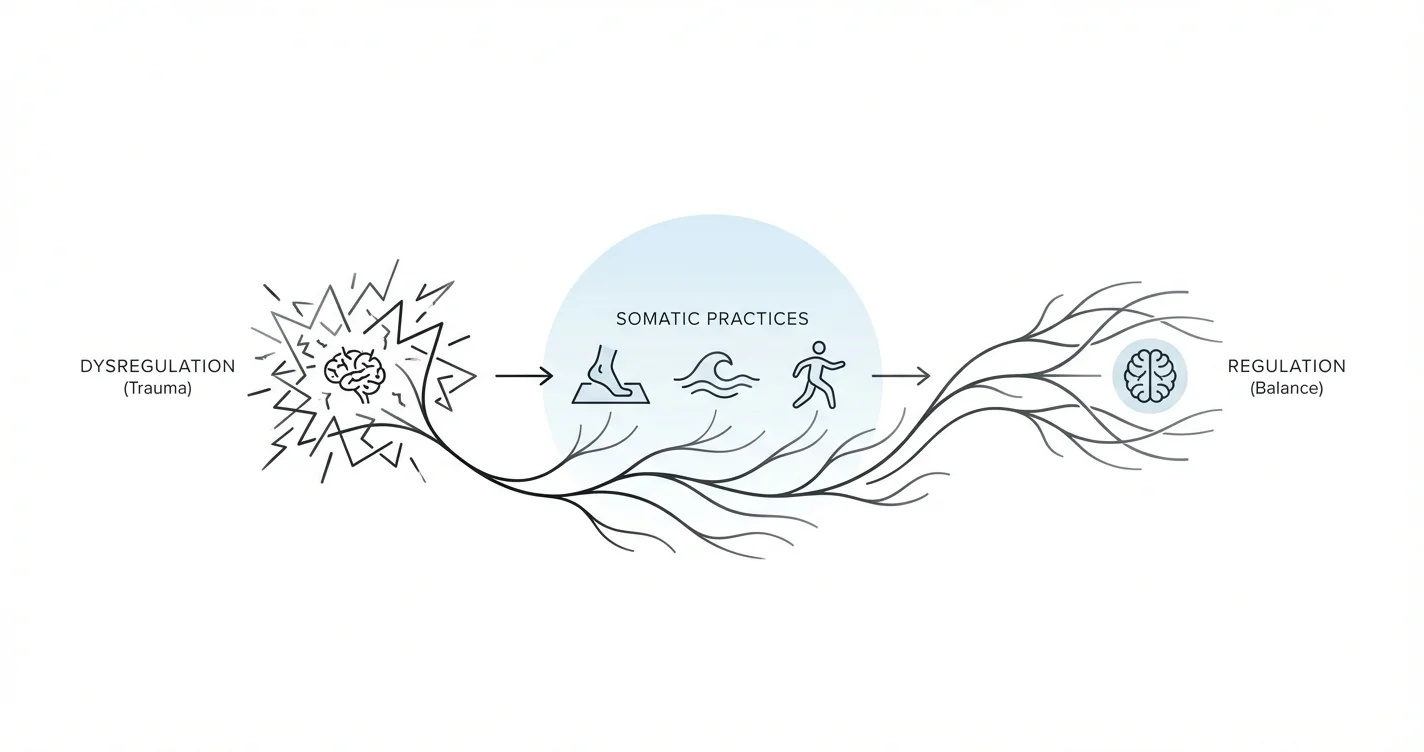
When trauma lives in the body, words alone often aren't enough to heal it. Traditional talk therapy can provide valuable insights, but many people find their nervous systems remain stuck in patterns of hypervigilance, shutdown, or emotional reactivity despite understanding their trauma intellectually. This is where learning how to regulate nervous system trauma through somatic practices becomes essential. These body-based approaches work directly with the physiological imprints of trauma, helping restore a sense of safety and regulation from the inside out.
Somatic practices acknowledge what neuroscience research suggests: that trauma impacts the nervous system at a pre-verbal, bodily level. By working with sensation, movement, breath, and body awareness, these techniques can help release stored trauma responses and build new patterns of regulation. This guide draws on established trauma treatment frameworks and clinical insights to provide practical, actionable approaches you can begin exploring today.
Understanding Somatic Approaches to Nervous System Trauma
Somatic practices for trauma recovery are grounded in the recognition that traumatic experiences become encoded not just in memory, but in the body's nervous system. When you experience trauma, your autonomic nervous system—which governs automatic functions like heart rate, breathing, and stress responses—can become dysregulated. This dysregulation may manifest as chronic tension, hypervigilance, emotional numbness, or difficulty feeling safe even in objectively secure environments.
The term "somatic" comes from the Greek word "soma," meaning body. Somatic approaches work with the principle that by bringing gentle, mindful attention to bodily sensations and supporting the completion of self-protective responses that may have been interrupted during trauma, the nervous system can gradually return to greater flexibility and balance.
Research in trauma treatment suggests that the nervous system operates through distinct states. The ventral vagal state supports social engagement and calm alertness. The sympathetic state activates fight-or-flight responses. The dorsal vagal state can lead to shutdown or immobilization. Trauma survivors often find themselves cycling through these states unpredictably or getting stuck in sympathetic activation or dorsal shutdown. Somatic practices aim to increase your capacity to move more fluidly between these states and spend more time in ventral vagal regulation.
Unlike approaches that focus primarily on changing thoughts or analyzing the past, somatic work emphasizes present-moment awareness of what's happening in your body right now. This bottom-up approach—working from body to mind rather than mind to body—can access healing pathways that cognitive approaches alone may miss.
Core Somatic Practices for Nervous System Regulation
Several body-based techniques have emerged as particularly helpful for trauma recovery and nervous system regulation. Each works slightly differently, but all share the common thread of building capacity to tolerate sensation, track internal experience, and support the nervous system's natural healing processes.
Grounding and Orientation
Grounding techniques help you establish a sense of connection to the present moment and your physical environment. When your nervous system is activated by trauma memories or triggers, grounding can interrupt the cascade of stress responses and remind your system that you're in the present, not the past.
Simple grounding practices include:
- Feeling your feet on the floor and noticing the support beneath you
- Pressing your hands gently against a wall or surface and noticing the resistance
- Looking around the room and naming objects you see in different colors
- Noticing sounds around you, both near and far
- Feeling the weight of your body in your chair or the texture of clothing against your skin
Orientation—deliberately looking around your environment with soft, receptive awareness—helps activate the parts of your nervous system associated with safety and social engagement. This can be as simple as slowly turning your head to take in your surroundings, allowing your eyes to rest on objects or views that feel pleasant or neutral.
Resourcing and Pendulation
Resourcing involves intentionally bringing to mind or noticing experiences, memories, people, places, or sensations that evoke feelings of safety, calm, or positive emotion. This isn't about denying difficult feelings but about ensuring you have access to stabilizing experiences alongside challenging ones.
Pendulation refers to the practice of gently moving attention between areas of activation or discomfort and areas of resource or neutrality. Rather than staying immersed in overwhelming sensations, you learn to "touch into" difficult feelings briefly, then return to something more manageable. This builds tolerance for difficult sensations gradually, without flooding your system.
For example, you might notice tension in your chest related to anxiety, acknowledge it briefly, then shift attention to a part of your body that feels more neutral or comfortable—perhaps your hands or feet. This gentle oscillation helps the nervous system learn it can encounter distress without becoming overwhelmed.
Tracking Sensations and Titration
Somatic tracking involves bringing curiosity and non-judgmental awareness to bodily sensations as they arise and change. You might notice warmth, coolness, tingling, pressure, tightness, spaciousness, or movement. The practice is simply to observe these sensations without trying to change them, allowing your nervous system to process and release held patterns at its own pace.
Titration means working with sensations and emotions in small, manageable doses. Rather than diving into the most overwhelming aspects of trauma, titration involves approaching difficult material gradually, allowing integration to happen in layers. This might mean focusing on a less intense memory first, or noticing just the edge of a difficult sensation rather than its center.
Support tools like Lovon.app can provide on-demand access to guidance through these practices, particularly valuable when you need support processing sensations or emotions as they arise between formal therapy sessions.
Somatic Therapy Techniques vs Traditional Trauma Approaches
Understanding how somatic practices differ from and complement traditional trauma therapy methods can help you make informed choices about your healing journey. Traditional trauma therapy often emphasizes cognitive processing—understanding what happened, challenging distorted beliefs, and developing new narratives about your experiences. These approaches can be profoundly helpful, particularly for making meaning of trauma and addressing cognitive patterns.
Cognitive processing therapies typically work top-down, using thinking and understanding to influence emotional and bodily states. Exposure-based therapies help reduce fear responses by gradually confronting trauma-related memories or situations in safe contexts. These methods have substantial research support for various trauma-related conditions.
Somatic approaches work bottom-up, starting with bodily sensations and using the body as a pathway to processing trauma. Rather than primarily talking about what happened, somatic work emphasizes noticing what's happening in your body right now and supporting the completion of self-protective responses. This can be particularly valuable when trauma occurred pre-verbally, when talking feels unsafe or overwhelming, or when cognitive approaches alone haven't fully resolved physical symptoms.
Many trauma-informed therapists now integrate both approaches, recognizing that comprehensive trauma healing often requires addressing both the cognitive and somatic dimensions of experience. You might work with talk therapy to understand patterns and develop new perspectives while also using somatic practices to release stored tension and build nervous system capacity.
Some key distinctions include:
- Pace: Somatic work often moves more slowly, emphasizing building tolerance and capacity before processing intense material
- Focus: Body sensations and present-moment awareness take priority over narrative or analysis
- Goals: Building nervous system flexibility and embodied self-regulation, not just symptom reduction
- Approach to activation: Rather than avoiding or pushing through arousal, somatic practices teach you to track and work with activation skillfully
When traditional approaches seem to help intellectually but don't shift how you feel in your body, adding somatic practices can bridge that gap. Conversely, somatic work often becomes easier and more effective when combined with cognitive understanding and relational support.
Step-by-Step Guide to Beginning Somatic Nervous System Regulation
If you're new to somatic practices, starting with a structured approach can help you build foundational skills safely and effectively. The following sequence provides a practical pathway for beginners, though remember that healing isn't linear and you may move through these steps at your own pace.
Step 1: Establish Safety and Resources
Before working directly with trauma-related material, build your capacity for regulation and identify resources you can return to when things feel difficult. Spend several sessions or practice periods simply:
- Noticing when you feel relatively calm or neutral
- Identifying places, people, memories, or activities that help you feel safer
- Practicing basic grounding techniques until they become familiar
- Learning to recognize early signs of nervous system activation in your body
This foundation phase isn't skipping ahead to "the real work"—it's creating the container that makes deeper processing possible.
Step 2: Develop Sensation Awareness
Begin noticing bodily sensations throughout your day without trying to change them. Start with neutral or pleasant sensations rather than jumping to areas of pain or tension:
- Notice the sensation of water on your skin during a shower
- Feel the texture and temperature of your morning beverage
- Observe the sensations of breathing without altering your breath
- Track how your body feels during gentle movement or stretching
As this becomes more comfortable, gradually include noticing sensations that are slightly uncomfortable but not overwhelming. Practice describing sensations in simple, descriptive terms (warm, tight, fluttery, heavy) rather than interpretive language (anxious, sad, angry).
Step 3: Practice Pendulation
Once you can track sensations with some ease, begin practicing the gentle oscillation between activation and resource:
- Notice a sensation of tension or discomfort
- Stay with it briefly, observing how it feels
- Before it becomes overwhelming, shift attention to something more comfortable
- Allow yourself to rest in the more comfortable sensation
- When ready, return briefly to the area of tension
This back-and-forth movement teaches your nervous system that it can touch difficult experiences without being consumed by them. Over time, your window of tolerance—the range of activation you can handle without shutting down or becoming overwhelmed—gradually expands.
Step 4: Support Completion of Self-Protective Responses
Trauma often involves situations where natural self-protective responses couldn't complete. Your body may have wanted to run, fight, or cry out but couldn't. Somatic practices can support the gentle completion of these impulses:
- If you notice an impulse to push away, you might press gently against a wall
- If you sense wanting to curl up protectively, allow yourself to hug a pillow or wrap in a blanket
- If you feel impulses in your legs, you might march in place or stomp gently
These actions are done slowly, with full awareness, allowing the nervous system to register that the protective response can now complete. This isn't about cathartic discharge but about gentle, conscious movement that helps the body know the threat has passed.
Step 5: Integrate and Build Resilience
As you develop greater capacity, you'll likely notice increased flexibility in your nervous system responses. Continue practicing:
- Regular check-ins with your body throughout the day
- Using grounding and resourcing when you notice activation beginning
- Celebrating small moments of regulation and self-awareness
- Gradually expanding your window of tolerance
On-demand support tools like Lovon.app can help you process what emerges during practice, work through moments of dysregulation, or simply talk through what you're noticing as you develop these new skills.
When to Seek Professional Help and Advanced Considerations
While many somatic practices can be explored on your own or with supportive resources, working with a trained trauma-informed therapist is important for several situations. If you're experiencing severe symptoms that interfere with daily functioning, have a history of complex trauma, find yourself becoming consistently overwhelmed during self-practice, or have concerns about safety, professional guidance provides essential support and structure.
Therapists trained in somatic approaches—such as Somatic Experiencing, Sensorimotor Psychotherapy, or trauma-informed body-oriented therapies—can help you navigate the process more safely. They can identify when you're moving too quickly, help you develop additional resources, and provide co-regulation (the calming presence of another regulated nervous system) that supports your own regulation.
Several nuances deserve consideration as you deepen your practice. First, healing isn't linear. You may have periods of significant progress followed by times when old patterns resurface. This doesn't mean you've failed or regressed—nervous system healing often involves spiraling back through familiar territory at deeper levels.
Second, what works differs significantly between individuals. Some people find movement-based practices most helpful, while others respond better to stillness and internal awareness. Your own exploration and possibly professional guidance can help you discover what serves your unique nervous system best.
Third, somatic work can sometimes bring up unexpected emotions or memories. This is a normal part of processing, but it underscores the importance of having adequate support and not pushing yourself into overwhelming territory. If something feels like too much, it probably is—backing off and building more resources is always an option.
Fourth, cultural background, identity, and life circumstances all influence how you relate to your body and what practices feel accessible or safe. Approaches that work well in one context may need adaptation in another. Trust your own sense of what feels right and seek practitioners who understand your specific context and needs.
Some people find that certain somatic practices initially feel uncomfortable or even increase distress. This doesn't necessarily mean they're harmful—sometimes discomfort arises because you're beginning to feel sensations that have been numbed or dissociated. However, consistent increases in distress suggest the need to slow down, adjust your approach, or seek professional guidance.
Conclusion
Learning how to regulate nervous system trauma through somatic practices offers a pathway to healing that honors the body's wisdom and capacity for recovery. By working with sensation, movement, breath, and awareness, you can gradually release stored trauma responses and build greater flexibility in your nervous system. The practices outlined here—grounding, resourcing, pendulation, sensation tracking, and supporting completion of self-protective responses—provide a foundation for beginning this journey.
Remember that somatic healing happens at its own pace and requires patience, self-compassion, and often support from others. Whether you explore these practices independently, use support tools like Lovon.app for processing between sessions, or work with a trained trauma-informed therapist, what matters most is finding approaches that resonate with your unique nervous system and circumstances. The path to regulation isn't about forcing change but about creating conditions where your body's innate healing capacities can unfold. As you develop these skills, you may find not just relief from trauma symptoms, but a deeper, more embodied sense of presence and aliveness in your life.
Disclaimer: This is general information, not medical advice or diagnosis. If symptoms are severe, affecting your daily life, or you're having thoughts of self-harm — seek professional help. In the US: call or text 988 (Suicide & Crisis Lifeline). For immediate danger: 911 or local emergency services.
How AI Support Helps You Heal
AI emotional support isn't about replacing human connection — it's about filling the gaps. The moments when you need to talk at 2 AM, when you don't want to burden your friends again, or when you simply need someone to listen without judgment.
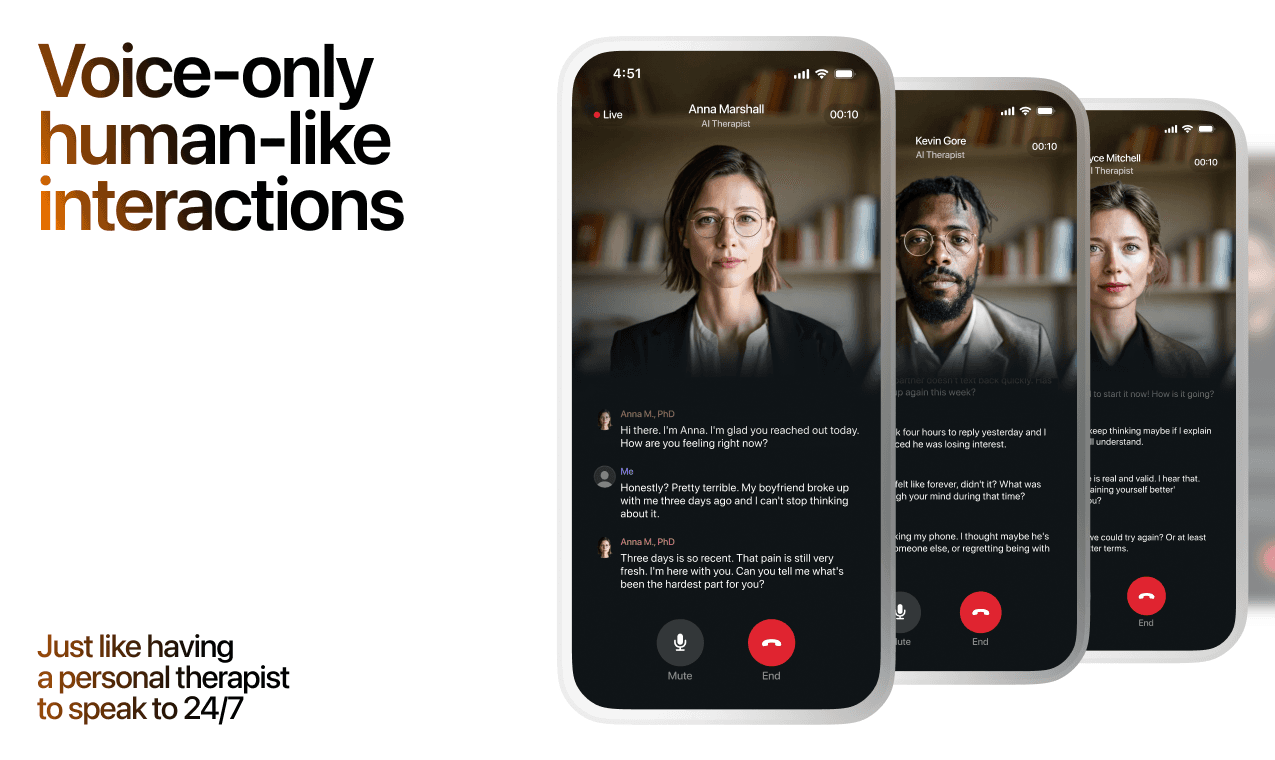
Here's what happens in a typical Lovon session:
You share what's on your mind
There's no script, no intake form, no waiting room. You speak or type whatever you're feeling — in your own words, at your own pace.
Lovon validates and explores
Using frameworks from CBT (Cognitive Behavioral Therapy) and motivational interviewing, Lovon acknowledges your feelings first, then gently helps you explore them. No dismissive "just move on" advice.
You build coping skills together
Lovon doesn't just listen — it actively works with you on evidence-based techniques: thought reframing, urge surfing, behavioral experiments, and more.
What a Session with Lovon Looks Like
When to Seek Professional Help
AI support is a valuable tool, but it's not a replacement for professional care. Please consider reaching out to a licensed therapist if you experience any of the following:
- Persistent thoughts of self-harm or suicide
- Inability to perform daily activities (work, eating, sleeping) for more than 2 weeks
- Turning to alcohol or substances to cope
- Intense anger or desire to harm your ex-partner
- Complete emotional numbness that doesn't improve over time
Crisis Resources (US): If you're in immediate danger, call 988 (Suicide & Crisis Lifeline) or text HOME to 741741 (Crisis Text Line). Available 24/7, free, and confidential.
Outside the US? Find a crisis line in your country
Ready to Start?
Your healing journey can begin right now
1 free conversation. No credit card. No judgment. Just a safe space to process what you're going through.
Frequently Asked Questions
Is AI therapy a replacement for a real therapist?
Is my conversation with Lovon AI private?
How is Lovon different from ChatGPT for emotional support?
Can I use Lovon if I'm already seeing a therapist?
Can I try Lovon for free?
About the Author
The Lovon Editorial Team
Mental Health & Wellness Content Team
The Lovon Editorial Team develops mental health and wellness content designed to make psychological concepts accessible and actionable. Our goal is to bridge the gap between clinical research and everyday life - helping you understand why your mind works the way it does and what you can do about it....
Similar Articles
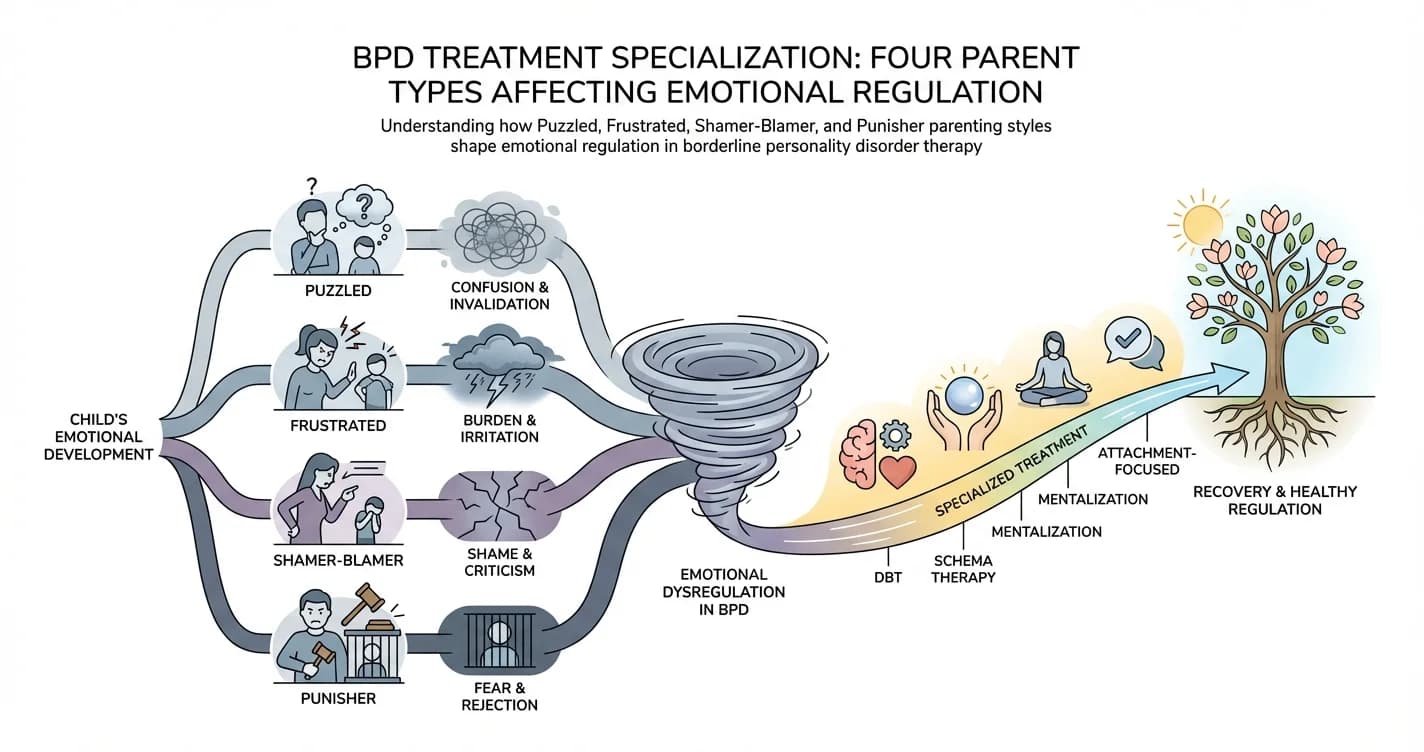
BPD Treatment Specialization: Four Parent Types Affecting Emotional Regulation
For individuals with borderline personality disorder (BPD), emotional regulation difficulties rarely emerge in isolation. Research increasingly suggests that
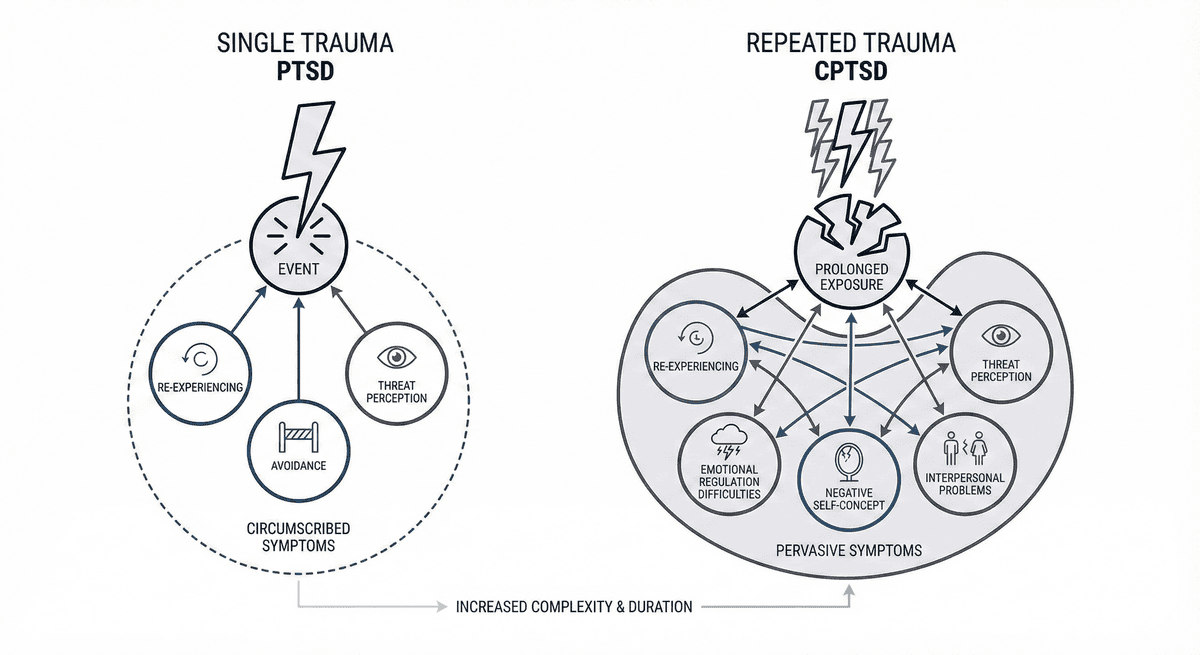
PTSD vs CPTSD: Single Trauma vs Repeated Trauma Symptom Differences
Learn how PTSD from a single traumatic event differs from CPTSD shaped by repeated trauma, including symptom patterns and treatment approaches.
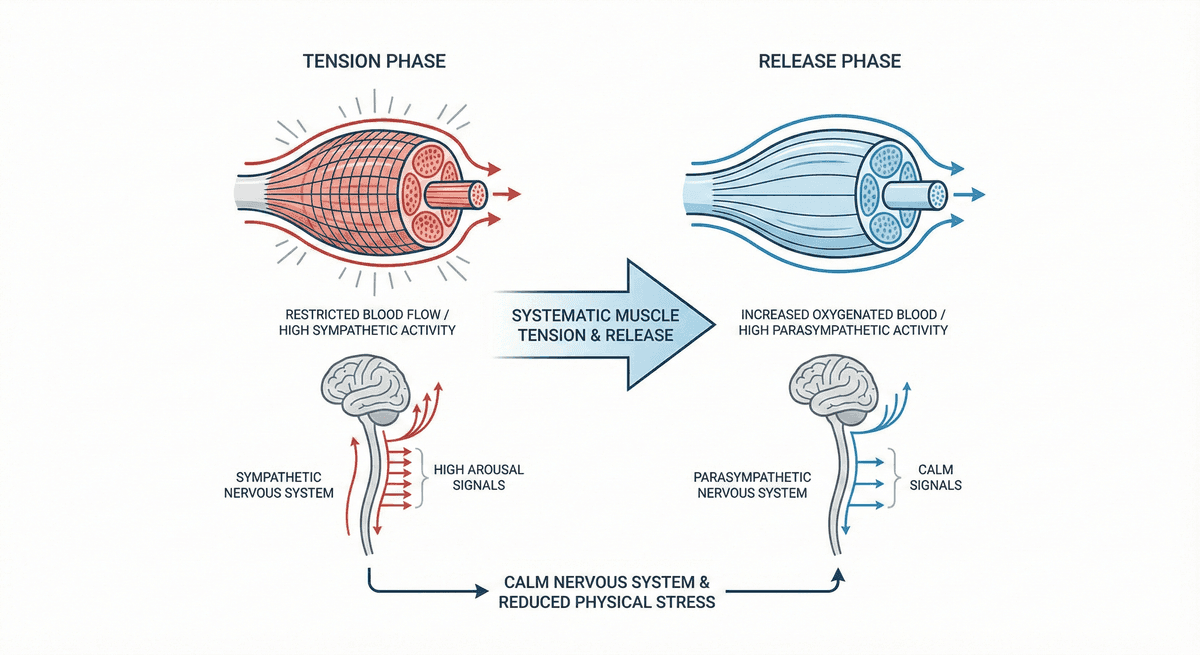
Progressive Muscle Relaxation for Stress Reduction
A systematic muscle group tension and release technique that calms the nervous system and reduces physical stress.
Disclaimer: This article is for informational purposes only and does not constitute medical advice, diagnosis, or treatment. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition. If you are in crisis or think you may have an emergency, call 988 (Suicide & Crisis Lifeline) or go to the nearest emergency room. Outside the US? Find a crisis line in your country.