Intergenerational Trauma & Mental Health: Break the Cycle of Generational Trauma
Some things that happen to people do not stay only with them. A bad experience in one generation can affect the next one.
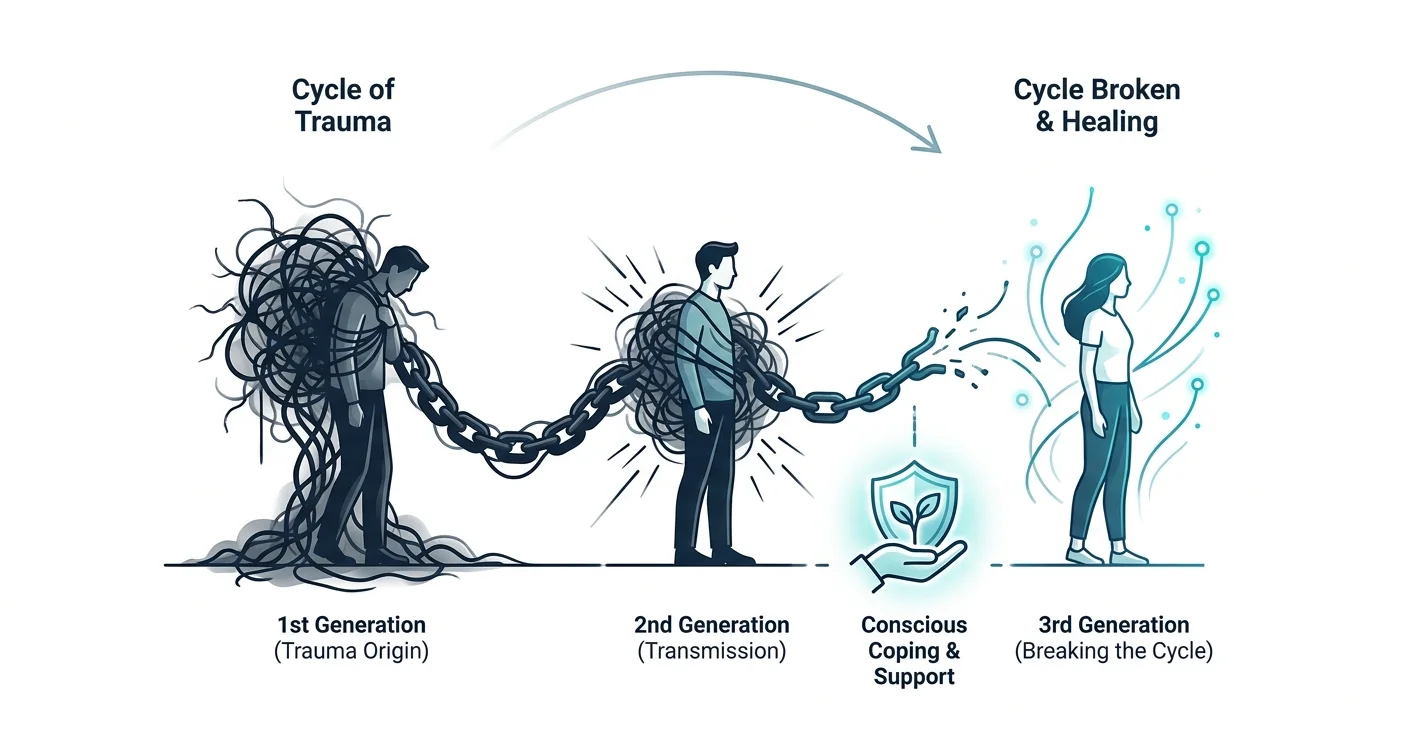
Key Takeaways
- People may carry fear or anxiety that started in the family long before their own life experience
- Generational trauma can affect both mental health and the body
- When families do not talk about trauma, children still feel the stress but do not know why
- You can start to break this cycle with small changes, like better coping or understanding yourself
Introduction
Some things that happen to people do not stay only with them. A bad experience in one generation can affect the next one. It can change how children grow up, what they are afraid of, how their bodies react to stress, and what they pass on to others. This is an important idea in trauma research, and it can help you understand your own behavior and what you can change in the future.
What Is Generational Trauma?
Transgenerational trauma, also called intergenerational trauma or generational trauma, refers to the transmission of trauma across generations, meaning the psychological, behavioral, and in some cases biological effects of a traumatic experience are passed from those who experienced it directly to their children and beyond.
The idea first came from doctors who worked with children of Holocaust survivors in the 1960s and 1970s. Clinicians noticed that the children of Holocaust survivors, who had not themselves experienced the original trauma, were presenting with trauma symptoms including hypervigilance, anxiety and depression, difficulty regulating emotions, and a pervasive but often unnameable sense of dread.
Since then, studies have examined intergenerational effects in survivors of the Armenian genocide, Japanese American internment, Indigenous communities subjected to forced assimilation policies, enslaved people and their descendants, refugees from conflict zones, and communities subjected to sustained racial trauma and systemic violence.
Intergenerational Transmission of Trauma: How Does It Actually Pass Between Generations?
Trauma that isn't directly experienced still produces measurable effects. Here are several mechanisms.
Epigenetic Transmission
The study of how genes work without changing the DNA itself. Life experience, including trauma, can change how genes work, and some of these changes may pass to children.
Studies with children of the Holocaust survivors showed differences in how their bodies react to stress. This means parents’ trauma may affect their children’s stress system. Research by Rachel Yehuda at Icahn School of Medicine at Mount Sinai found real changes in a gene linked to stress in these children.
These changes can change again with new experiences, including therapy. But they help explain why people can feel the effects of trauma even if they did not live through it themselves.
Sociocultural and Structural Transmission
Some trauma does not come from one family. It can come from society. Things like racism, poverty, and unfair systems can affect whole communities for many years.
A clear example is Indian residential schools in North America. Children were taken from their families, could not speak their language, and often faced abuse. This trauma affected not only them but also their children and grandchildren. It led to problems with trust, culture loss, addiction, suicide, and poverty.
Black Americans also carry trauma from history, like slavery and segregation. Many still face racism today. Research shows higher stress and mental health problems in this community, and this cannot be explained only by personal situations.
Psychological and Behavioral Transmission
A parent who had trauma may learn ways to cope. These ways helped before, but now they can cause problems for their children. For example:
- It is hard for them to talk about trauma
- They are always on alert, so the family feels constant anxiety
- They protect too much, so the child feels the world is very dangerous
- They seem distant or numb, so the child does not get enough emotional support
- They use alcohol or other substances to cope
Mental and Physical Health: The Roots of Generational Trauma and What It Does to the Body
Trauma affects both mind and body at the same time. It can also pass from parents to children and affect their health.
The Adverse Childhood Experiences Study showed that more bad childhood experiences lead to more health problems later in life, like heart disease, diabetes, cancer, immune problems, and long-term pain.
Children who grow up in families with trauma often have more of these experiences too, so the cycle can continue.
The mechanisms include:
- Higher rates of substance abuse as a coping mechanism, with its own direct health consequences
- Chronic activation of the stress response system, producing sustained inflammation, hormonal dysregulation, and immune suppression
- Reduced access to health services in communities where historical trauma has produced justified mistrust of medical institutions
- Disrupted sleep, which has cascading effects on physical health across multiple systems
Symptoms of Generational Trauma: Signs of Generational Trauma in Individuals and Families
Generational trauma tends to surface as patterns that feel simply like "how our family is" until something prompts a closer look.
In individuals, symptoms of generational trauma may include:
- Post-traumatic stress disorder or complex trauma symptoms
- Chronic anxiety or generalized anxiety disorder without a clear precipitating cause
- Difficulty regulating emotions, particularly in family or intimate contexts
- Hypervigilance and an exaggerated startle response
- Depression and a persistent sense of hopelessness that does not respond to circumstantial improvement
- Shame that feels structural, not situational, as though it is simply part of who you are
- A sense of carrying something heavy that you cannot fully name or locate
- Difficulty trusting others, particularly authority figures
In family systems, signs of generational trauma often look like:
- Subjects that are never discussed
- Parenting styles that transmit fear, shame, or hypervigilance without the parent being consciously aware of doing so
- Repeated patterns across generations: similar relationship dynamics, similar struggles with addiction, similar patterns of emotional unavailability
- Intense, seemingly disproportionate reactions to specific triggers within the family system
- Family narratives that minimize or erase past experiences
Black Americans, Racial Trauma, and Intergenerational Effects
Racial trauma is different from family trauma and needs care that fits the culture. Research shows that Black Americans have higher levels of PTSD, anxiety, and depression than white Americans, even when income is similar. This is because of history like slavery and segregation, and also racism that still exists today.
Trauma is harder to deal with when society does not talk about it. If the problem is still happening, normal therapy may not help if it ignores culture and history. Better support includes therapy that respects culture, help from the community, and understanding the history behind the trauma.
Complex Trauma and the Family System
Complex trauma means trauma that happens many times or for a long time. It can affect the next generation more strongly. It changes how a person feels and raises children. A parent who had this kind of trauma, especially from people close to them, may not know how to create safe and healthy bonds. It is hard to give children something they did not receive themselves. This helps us understand how trauma passes through families, and how it can be improved with support, therapy, and care.
Effects of Generational Trauma: What It Looks Like Across Generations?
The effects of generational trauma shift somewhat across generations as the original trauma recedes in direct experience but persists in its consequences.
| Generation | Relationship to original trauma | Common presentations | | --- | --- | --- | | First (direct survivors) | Directly experienced the traumatic event | PTSD, grief, survivor guilt, difficulty processing and integrating the experience | | Second (children of survivors) | No direct exposure but raised by those who were directly affected | Anxiety, depression, diffuse shame, difficulty understanding their own distress, absorbing the emotional climate of the household | | Third and beyond | Further removed from the original trauma | May experience symptoms without any family narrative to explain them, higher risk of dismissing the connection between past and present |
Break the Cycle of Trauma
Breaking the cycle of generational trauma is possible. It requires understanding and usually support. Here is what the evidence supports.
Develop Conscious Coping Strategies
Many coping ways come from the past. They helped before, but now they can cause problems. It is important to see which habits you got from your family and which ones you want to keep.
This work can be easier with a therapist, but also with honest self-reflection. Ask yourself: what patterns do I repeat? Why do I feel fear or shame that is stronger than the situation?
Talk About It, Carefully and with Support
One main way trauma passes to children is silence. When families do not talk about trauma, children feel the stress but do not understand it. This does not mean forcing hard talks. It means slowly learning to talk about what happened, with help.
Research on families of the Holocaust survivors and others shows that open communication leads to better mental health. Families who talk about trauma usually do better than families who stay silent.
Therapy Can Help, and Specific Approaches Matter
Not all therapy is equally effective for intergenerational and complex trauma. Approaches with the strongest evidence base include:
- Trauma-focused cognitive behavioral therapy, which addresses the thought patterns and behavioral responses that unresolved trauma installs
- EMDR, or eye movement desensitization and reprocessing, which helps the brain reprocess traumatic memories that have become stuck and are driving ongoing symptoms
- Somatic approaches that work with the body's held trauma rather than relying solely on verbal processing
- Attachment-focused therapy, which specifically addresses the relational disruptions that complex trauma produces and that drive so much of the intergenerational transmission
- Family therapy, which can help make the patterns within the family system visible and begin to shift them at that level rather than only individually
Access Community and Cultural Resources
Individual therapy can help, but it is not always enough for trauma that affects whole communities and comes from history. People also need support from others and understanding of what happened.
For Indigenous communities, reconnecting with culture is very important. This includes language, traditions, ceremonies, and connection to the land. These can improve mental health and sometimes help even more than therapy alone.
Attend to Parenting with Specific Intentionality
Trauma often passes through parenting. If parents understand their own trauma, they can help stop this cycle. They just need to notice when their reactions come from past pain and try to act differently, with support. A parent who can say sorry, stay calm when a child is upset, and admit mistakes is already breaking the cycle.
Multigenerational Legacies of Trauma: What Healing Actually Looks Like?
Healing from trauma does not mean forgetting the past. It means changing how you relate to it. You know what happened, but it does not control your life. For example, it looks like a family that can talk about the past, not to stay in it, but to understand it and move forward.
When to Seek Help?
Consider speaking with a mental health professional if:
- You are a parent who is concerned about patterns you may be transmitting to your children
- You recognize the patterns described in this article in your own life or family
- You experience symptoms of anxiety, depression, PTSD, or complex trauma that feel disconnected from your own experiences
- You are part of a community that has experienced collective or historical trauma and you are struggling with distress
- You are unsure whether what you are carrying is your own or something older
Sources and Further Reading
We used these sources to create this article and help you feel better. You can explore them to get a deeper understanding of the topic:
- Relationship of childhood abuse and household dysfunction to leading causes of death. American Journal of Preventive Medicine. PubMed
- The historical trauma response among Natives and its relationship with substance abuse. Journal of Psychoactive Drugs. PubMed
- Holocaust exposure induced intergenerational effects on FKBP5 methylation. Biological Psychiatry. PubMed
How AI Support Helps You Heal
AI emotional support isn't about replacing human connection — it's about filling the gaps. The moments when you need to talk at 2 AM, when you don't want to burden your friends again, or when you simply need someone to listen without judgment.
Here's what happens in a typical Lovon session:
You share what's on your mind
There's no script, no intake form, no waiting room. You speak or type whatever you're feeling — in your own words, at your own pace.
Lovon validates and explores
Using frameworks from CBT (Cognitive Behavioral Therapy) and motivational interviewing, Lovon acknowledges your feelings first, then gently helps you explore them. No dismissive "just move on" advice.
You build coping skills together
Lovon doesn't just listen — it actively works with you on evidence-based techniques: thought reframing, urge surfing, behavioral experiments, and more.
What a Session with Lovon Looks Like
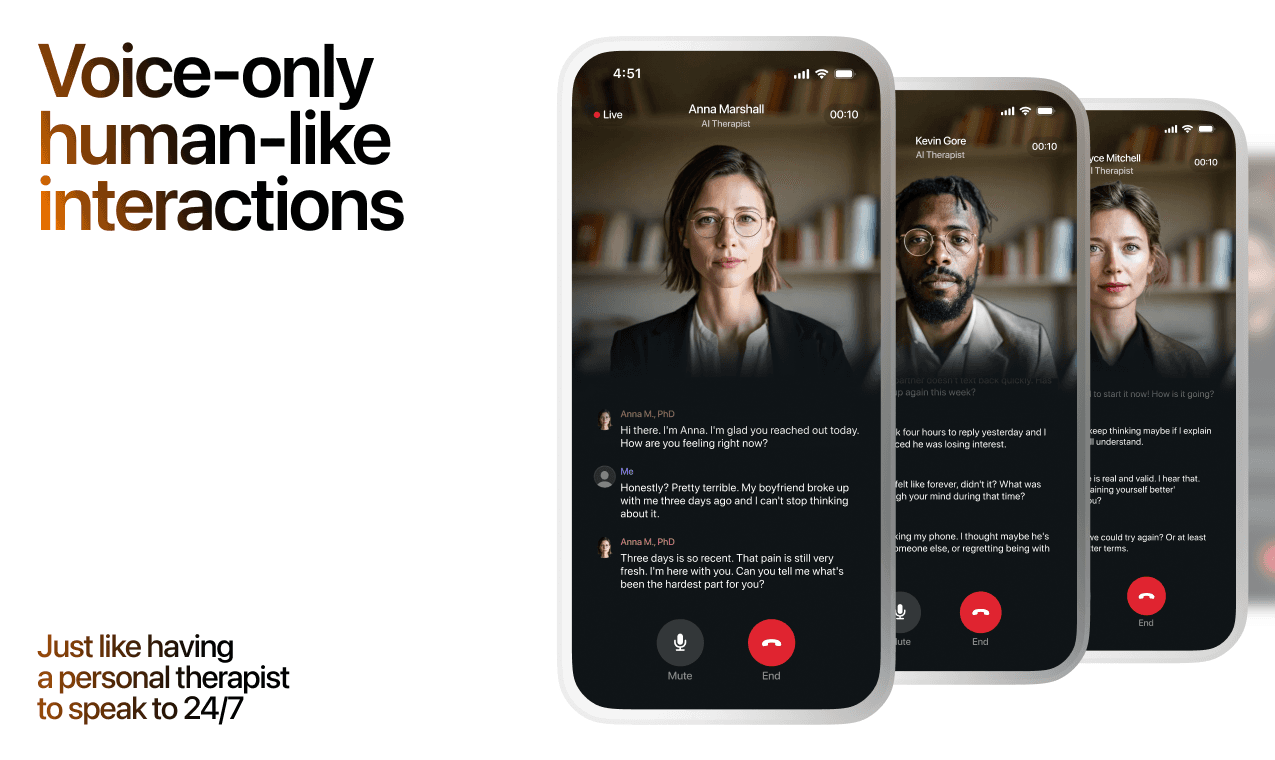
When to Seek Professional Help
AI support is a valuable tool, but it's not a replacement for professional care. Please consider reaching out to a licensed therapist if you experience any of the following:
- Persistent thoughts of self-harm or suicide
- Inability to perform daily activities (work, eating, sleeping) for more than 2 weeks
- Turning to alcohol or substances to cope
- Intense anger or desire to harm your ex-partner
- Complete emotional numbness that doesn't improve over time
Crisis Resources (US): If you're in immediate danger, call 988 (Suicide & Crisis Lifeline) or text HOME to 741741 (Crisis Text Line). Available 24/7, free, and confidential.
Outside the US? Find a crisis line in your country
Ready to Start?
Your healing journey can begin right now
1 free conversation. No credit card. No judgment. Just a safe space to process what you're going through.
Frequently Asked Questions
Q: Is intergenerational trauma scientifically proven?
Q: How do I know if what I am experiencing is intergenerational trauma or my own trauma?
Q: Can epigenetic changes from trauma be reversed?
Q: Does talking about intergenerational trauma risk keeping people stuck in the past?
Q: What if my family refuses to acknowledge or discuss the history?
Q: Are some people more resilient to intergenerational trauma effects than others?
Q: How long does it take to break the cycle of generational trauma?
About the Author
Mireya Tabasa
Mental Health Support Specialist & AI Advisor
Mireya Tabasa is a Mental Health Support Specialist working at the intersection of clinical care and technology. With over 4 years of hands-on experience supporting diverse populations facing mental health challenges in educational and healthcare settings, she brings frontline clinical insight to ev...
Similar Articles
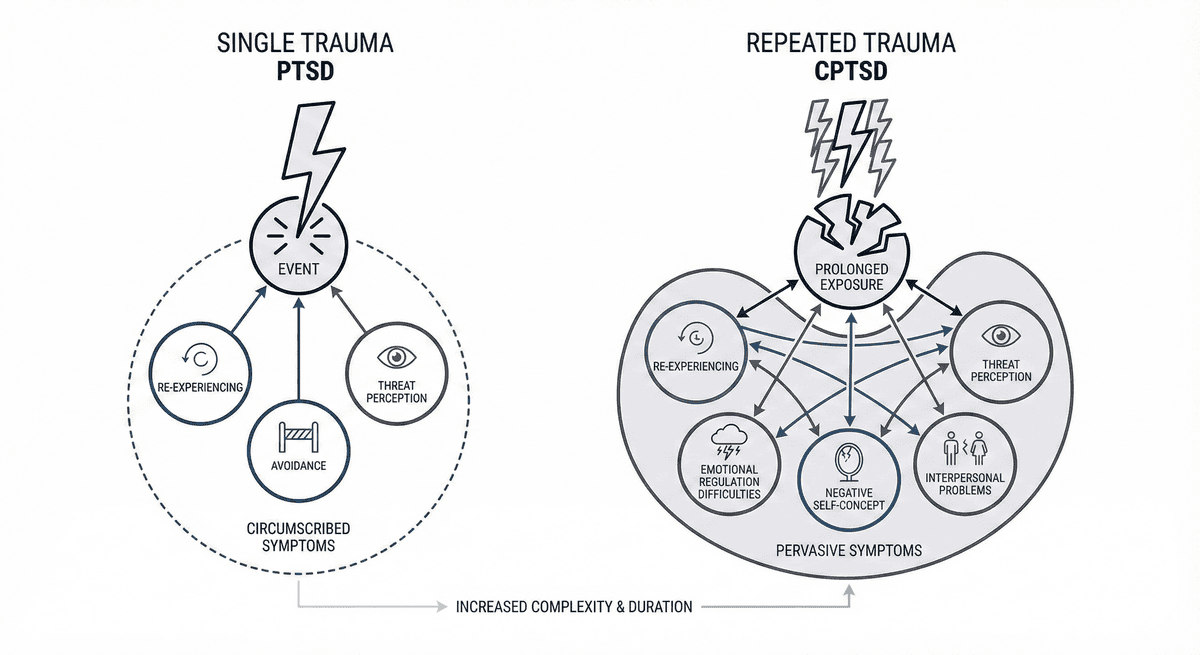
PTSD vs CPTSD: Single Trauma vs Repeated Trauma Symptom Differences
Learn how PTSD from a single traumatic event differs from CPTSD shaped by repeated trauma, including symptom patterns and treatment approaches.
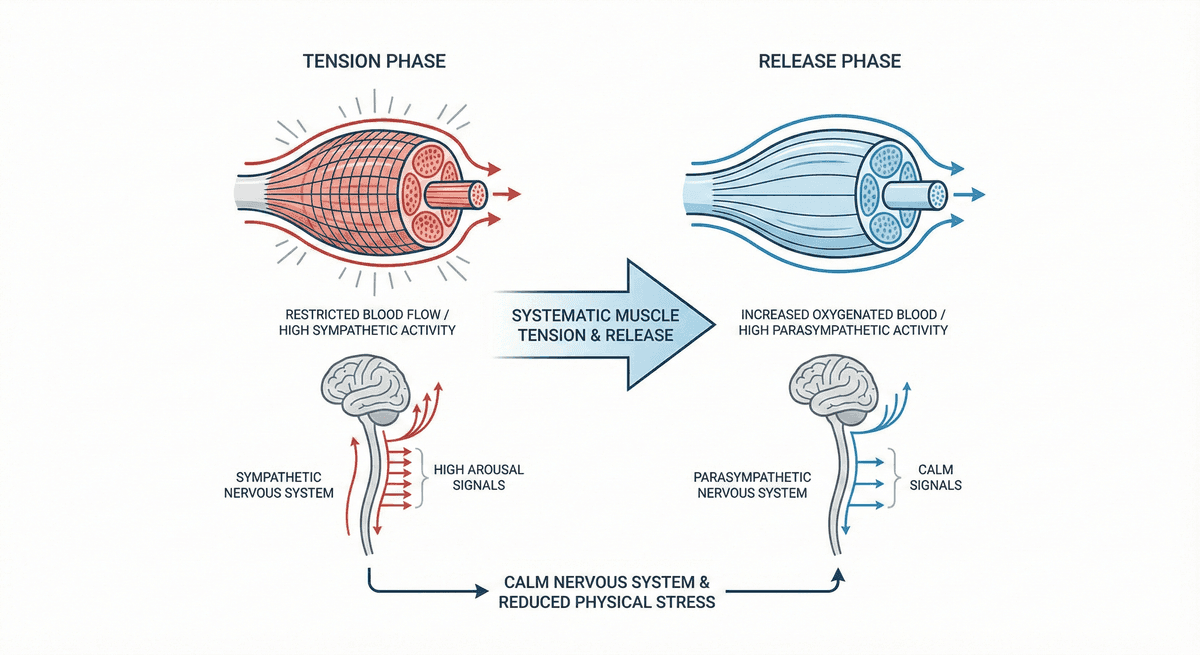
Progressive Muscle Relaxation for Stress Reduction
A systematic muscle group tension and release technique that calms the nervous system and reduces physical stress.
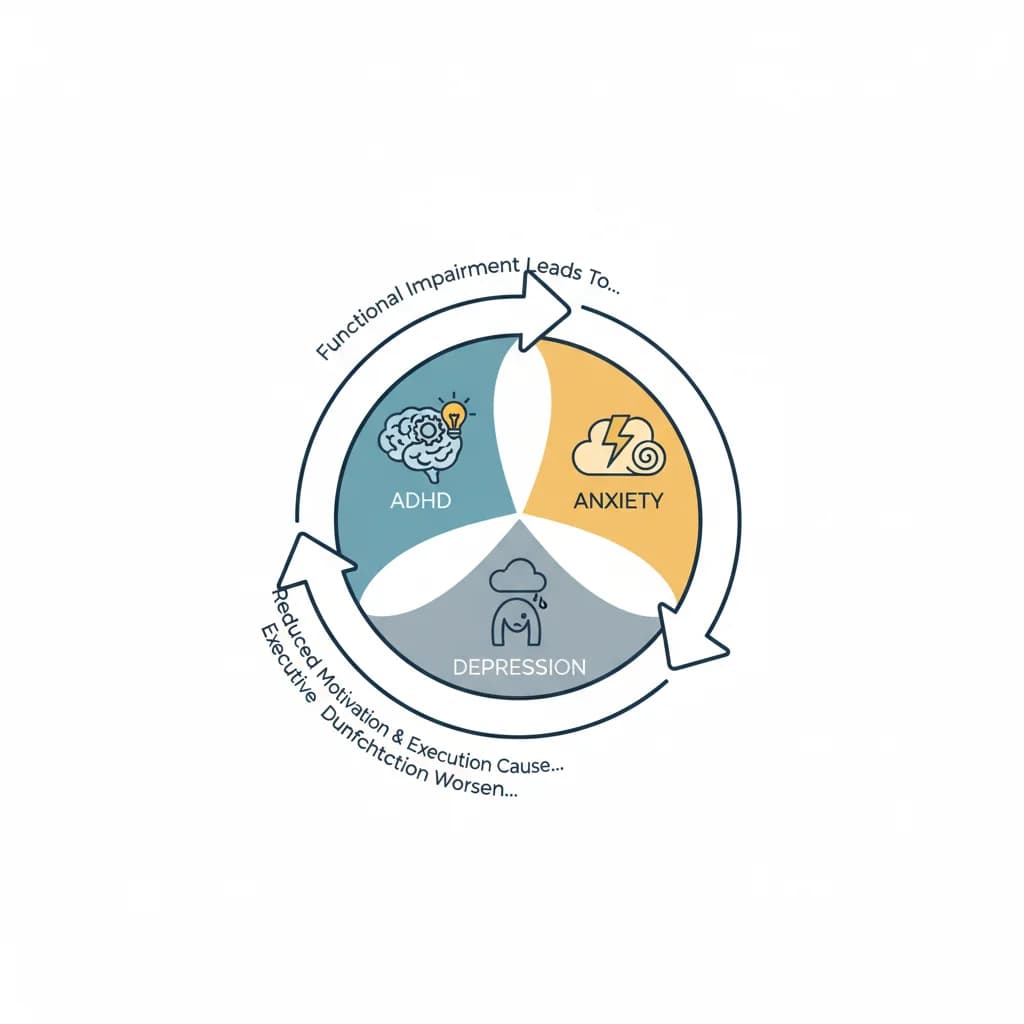
ADHD Comorbidity with Anxiety and Depression Cycles
Understanding the Complex Interplay Between ADHD and Recurring Mental Health Patterns
Disclaimer: This article is for informational purposes only and does not constitute medical advice, diagnosis, or treatment. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition. If you are in crisis or think you may have an emergency, call 988 (Suicide & Crisis Lifeline) or go to the nearest emergency room. Outside the US? Find a crisis line in your country.
