Nervous System Regulation and Disproportionate Emotional Reactions
Have you ever found yourself reacting with overwhelming intensity to something that, logically, shouldn''t warrant such a strong response? Perhaps a minor

Key Takeaways
- Intense anger or defensiveness in response to mild criticism
- Overwhelming anxiety about situations that feel manageable to others
- Frantic efforts to prevent abandonment or rejection
- Compulsive need to fix, control, or manage outcomes
- Feeling devastated when someone doesn't respond to messages promptly
Introduction
Have you ever found yourself reacting with overwhelming intensity to something that, logically, shouldn't warrant such a strong response? Perhaps a minor comment from a partner triggers deep hurt, or a small change in plans sends you into a spiral of anxiety. These disproportionate emotional reactions as trauma activation are not signs of weakness or overreaction—they're your nervous system responding to perceived threats based on past experiences. When the body detects echoes of earlier wounds, it can launch into survival mode even when the present situation is relatively benign. Understanding nervous system regulation and how past trauma creates these amplified responses is essential for anyone experiencing emotional reactivity that feels out of proportion to current circumstances. This article explores the mechanisms behind trauma-triggered emotional intensity and provides evidence-based approaches to working with your nervous system rather than against it.
Understanding Disproportionate Emotional Reactions as Trauma Activation
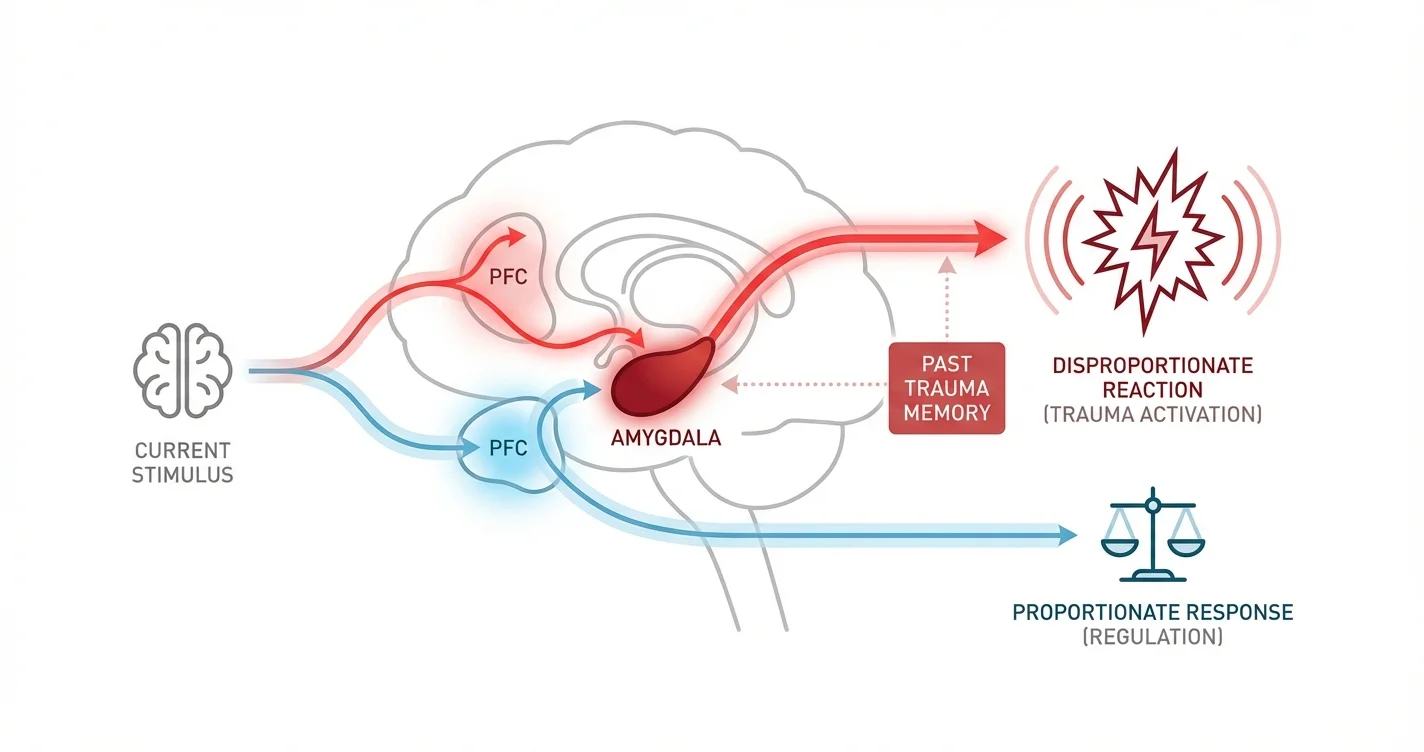
Disproportionate emotional reactions occur when your emotional response significantly exceeds what the current situation would typically warrant. You might feel devastated by a cancelled plan, enraged by a minor inconvenience, or terrified by a manageable challenge. These responses aren't "irrational"—they're your nervous system reacting to what it perceives as a threat based on your personal history.
Research in neuroscience and trauma psychology indicates that the nervous system operates primarily on pattern recognition rather than logical analysis. When present circumstances mirror elements of past traumatic or painful experiences, your body may respond as if the original threat is happening again. This process occurs largely outside conscious awareness, which is why you might feel confused by the intensity of your own emotions.
The body doesn't differentiate between a genuine current threat and a situation that resembles a past threat. Practitioners working with trauma understand that emotional reactions exceeding the apparent cause often signal that something from the past has been activated in the present. Your nervous system essentially opens a doorway to unprocessed experiences, bringing the emotional weight of those earlier events into your current awareness.
This activation involves several interconnected systems. The amygdala, which processes emotional significance and threat detection, may respond to subtle cues that consciously you don't even notice—a tone of voice, a facial expression, a particular context. When these cues match patterns associated with previous distressing experiences, your nervous system can shift into a protective state within fractions of a second, before your conscious mind has time to evaluate the actual level of threat.
The Nervous System's Response to Perceived Threat
Your nervous system operates through distinct states that determine how you respond to your environment. When you feel safe and connected, your system remains in a ventral vagal state characterized by openness, social engagement, and emotional flexibility. However, when your system detects threat—whether real or perceived based on past patterns—it shifts into protective modes.
The sympathetic nervous system activates the fight-or-flight response, flooding your body with stress hormones and preparing you for action. This can manifest as anger, anxiety, panic, or an urgent need to control your circumstances. In the context of disproportionate emotional reactions, this might look like:
- Intense anger or defensiveness in response to mild criticism
- Overwhelming anxiety about situations that feel manageable to others
- Frantic efforts to prevent abandonment or rejection
- Compulsive need to fix, control, or manage outcomes
When fight-or-flight feels ineffective or unsafe, your system may shift into a dorsal vagal state—a shutdown or freeze response characterized by emotional numbness, dissociation, hopelessness, or extreme fatigue. Someone might appear calm externally while feeling completely disconnected internally.
These nervous system states aren't choices you make consciously. According to experts working with nervous system regulation, the body responds not to logic but to its perception of safety versus threat. Your conscious mind might recognize that a situation is objectively safe, but if your nervous system has learned to associate certain cues with danger, it will respond accordingly regardless of what you rationally know.
Understanding this distinction is crucial: regulating your nervous system isn't about commanding yourself to "calm down" or "stop overreacting." Those approaches typically fail because they ignore the underlying activation. Instead, effective regulation involves recognizing when past trauma is being activated in the present moment and responding with approaches that help your body feel safer.
How Trauma Creates Patterns of Emotional Dysregulation
Trauma—particularly relational trauma occurring in early development—shapes how your nervous system interprets and responds to current experiences. When significant relationships weren't consistently safe, predictable, or attuned to your needs, your nervous system adapted by becoming hypervigilant to potential threats and quick to activate protective responses.
Attachment wounds provide a particularly clear example of this pattern. If you experienced relationships where caregivers were unpredictable, dismissive, intrusive, or absent, your developing nervous system learned to associate connection with uncertainty or pain. Clinical research suggests that these early relational patterns create templates that influence how you perceive and respond to relationships throughout life.
When your nervous system carries memories of abandonment, helplessness, or loss, present situations that mirror those experiences—even subtly—can trigger your body into survival mode. Your system desperately seeks control and certainty because the uncertainty feels intolerable, reminiscent of times when unpredictability meant danger or emotional pain.
Common scenarios where disproportionate reactions signal activated attachment wounds include:
- Feeling devastated when someone doesn't respond to messages promptly
- Experiencing intense anxiety about a partner's mood or availability
- Desperately trying to make someone stay or prove your worth
- Feeling rejected by minor signs of disinterest or distance
- Needing constant reassurance about your value in relationships
These patterns often reflect anxious attachment responses—your nervous system learned that relationships weren't reliably safe, so it remains constantly alert to signs of potential rejection or abandonment. The intensity of your reaction reflects not just the present situation but the accumulated weight of all the times your need for secure connection went unmet.
Similarly, individuals who experienced trauma involving helplessness or lack of control may have disproportionate reactions to situations where they feel powerless. A minor schedule change might trigger overwhelming anxiety because your nervous system associates unpredictability with danger. Someone making decisions without consulting you might feel like a profound violation because your body remembers times when your agency was disregarded in damaging ways.
Recognizing Activation Instead of Judging Your Reactions
A fundamental shift in working with disproportionate emotional reactions involves moving from self-judgment to recognition. When you find yourself having an intense emotional response, the instinct might be to criticize yourself: "Why am I being so sensitive? This shouldn't bother me this much. What's wrong with me?"
This self-judgment adds a secondary layer of distress to the original activation. You're now dealing with both the triggered emotional response and the shame or frustration about having that response. Practitioners emphasizing trauma-informed approaches suggest that healing begins when you listen to your reactions rather than judging them.
Your emotional reactions, even when disproportionate to current circumstances, carry important information. They're showing you where old wounds remain unhealed, where your nervous system still perceives threat, and what you needed that you didn't receive in the past. Rather than dismissing or suppressing these reactions, recognizing them as signals from your nervous system creates space for genuine healing.
This recognition process involves developing awareness of your activation patterns:
- Physical signals: Notice what happens in your body when you're activated—tightness in your chest, shallow breathing, tension in your shoulders, a knot in your stomach, feeling hot or cold
- Emotional signatures: Identify the specific emotional quality of your reactions—is it panic, rage, despair, shame, or numbness?
- Situational patterns: Track what types of situations consistently trigger disproportionate responses—conflict, perceived rejection, uncertainty, feeling controlled, or being misunderstood
- Historical connections: Gently explore whether present triggers connect to past experiences without forcing these connections or creating false narratives
Some people find it helpful to work with tools like Lovon.app to process these patterns in real-time, particularly when something has just triggered an intense reaction and you need support in understanding what happened. Having an accessible resource to talk through your emotional responses can help you develop the capacity to recognize activation rather than simply being swept away by it.
Practical Approaches to Nervous System Regulation
Regulating a dysregulated nervous system requires approaches that work with your body's protective responses rather than trying to override them through willpower. Effective regulation helps your nervous system gradually shift from perceiving threat to experiencing safety.
Building Awareness and Grounding
When you notice disproportionate emotional intensity, the first step is grounding yourself in the present moment. Your nervous system is responding as if a past threat is occurring now—grounding techniques help establish that you're in the present, not the past.
Practical grounding strategies include:
- Sensory awareness: Notice five things you can see, four you can hear, three you can touch, two you can smell, one you can taste
- Physical anchoring: Feel your feet on the ground, notice the support of the chair or surface beneath you, press your hands together
- Reality orientation: Remind yourself of the date, your current location, and factual aspects of your present situation
- Controlled breathing: Extend your exhale longer than your inhale to activate the parasympathetic nervous system—try breathing in for a count of four and out for a count of six
These techniques don't eliminate your emotional response, but they can create enough space between the activation and your conscious awareness to prevent immediate reactive behaviors you might regret.
Validation and Self-Compassion
Once you've established some grounding, the next step involves validating your emotional experience rather than dismissing it. Your reaction makes sense given your history, even if it's disproportionate to the present trigger.
Experts emphasize that your body isn't responding to logic—it's responding to patterns of safety and threat established through your experiences. Validating your response might sound like: "Of course this triggered me—it reminds my nervous system of times I felt abandoned/helpless/unseen. My body is trying to protect me based on what it learned was dangerous."
This validation doesn't mean your reaction is objectively proportionate or that others should accommodate it. Rather, it acknowledges that your nervous system's response makes sense within your personal context, which reduces the secondary distress of self-judgment and creates conditions for regulation.
Creating Safety Signals
Your nervous system regulates when it receives consistent signals of safety. These signals can be internal (self-generated) or external (from your environment or relationships).
Internal safety signals include:
- Compassionate self-talk: Speaking to yourself with the kindness you'd offer a scared child
- Bilateral stimulation: Gently tapping alternating sides of your body or using butterfly hugs (crossing arms and tapping shoulders alternately)
- Soothing touch: Placing a hand on your heart or stomach with gentle pressure
- Movement: Gentle stretching, walking, or shaking out tension
External safety signals might involve:
- Trusted relationships: Connecting with someone who can offer calm, non-judgmental presence
- Predictable routines: Establishing consistent patterns that help your nervous system anticipate what comes next
- Safe environments: Creating physical spaces that feel comfortable and under your control
- Professional support: Working with therapists trained in trauma-informed approaches who understand nervous system regulation
For many people, having access to immediate support when activation occurs makes a significant difference. Resources like Lovon.app can provide on-demand space to process what's happening when traditional therapy isn't immediately available—particularly valuable given that trauma activation often occurs outside business hours or in moments when you need to talk through something that just happened.
Exploring the Underlying Wound
Once you've established some regulation in the moment, there's often value in gently exploring what the present trigger connected to from your past. This exploration works best when your nervous system isn't in acute activation—it requires enough safety to reflect without becoming retraumatized.
Questions that can guide this exploration include:
- When have I felt this exact feeling before?
- What did I need in those earlier situations that I didn't receive?
- What was I trying to protect myself from then?
- How is my body trying to protect me now by responding this way?
This work often benefits from professional support, particularly when trauma is significant or complex. Therapists specializing in trauma treatment use approaches like EMDR, somatic experiencing, internal family systems, or attachment-focused therapy to help process underlying wounds in ways that promote genuine nervous system change.
When to Seek Professional Help
While self-regulation strategies can be valuable, some situations warrant professional support. Consider reaching out to a mental health professional if:
- Your emotional reactions consistently interfere with your relationships, work, or daily functioning
- You experience frequent dissociation, numbness, or disconnection from yourself
- You have thoughts of self-harm or suicide
- You struggle with substance use to manage emotional intensity
- Your attempts at self-regulation haven't created meaningful improvement
- You're experiencing symptoms of PTSD, complex trauma, or severe anxiety
Mental health professionals who specialize in trauma—including therapists trained in trauma-focused cognitive behavioral therapy, EMDR, somatic approaches, or attachment-based therapy—can provide structured support for healing nervous system dysregulation at its roots. Psychiatrists or psychiatric nurse practitioners can also evaluate whether medication might help support your nervous system regulation while you engage in therapeutic work.
The strategies discussed in this article complement but don't replace professional treatment when emotional dysregulation is significantly affecting your life. Addressing nervous system regulation with both self-directed strategies and professional guidance often produces the most sustainable results.
Conclusion
Disproportionate emotional reactions as trauma activation aren't signs of personal failure—they're your nervous system responding to perceived threats based on patterns established through your experiences. Understanding nervous system regulation and recognizing when past wounds are activated in present moments creates the foundation for healing rather than perpetuating cycles of self-judgment and shame.
The path toward regulation involves recognizing activation, grounding yourself in the present, validating your experience, and gradually building your nervous system's capacity to distinguish between past threats and present safety. This work takes time and often requires support, whether through trusted relationships, professional therapy, or accessible resources that help you process emotional experiences as they arise.
Your nervous system learned its protective patterns through experience, and it can learn new patterns through repeated experiences of safety, attunement, and effective co-regulation. By approaching your emotional intensity with curiosity rather than criticism, you create conditions for your nervous system to gradually update its threat detection systems and develop more flexible, proportionate responses to present circumstances.
Disclaimer: This is general information, not medical advice or diagnosis. If symptoms are severe, affecting your daily life, or you're having thoughts of self-harm—seek professional help. In the US: call or text 988 (Suicide & Crisis Lifeline). For immediate danger: 911 or local emergency services.
How AI Support Helps You Heal
AI emotional support isn't about replacing human connection — it's about filling the gaps. The moments when you need to talk at 2 AM, when you don't want to burden your friends again, or when you simply need someone to listen without judgment.
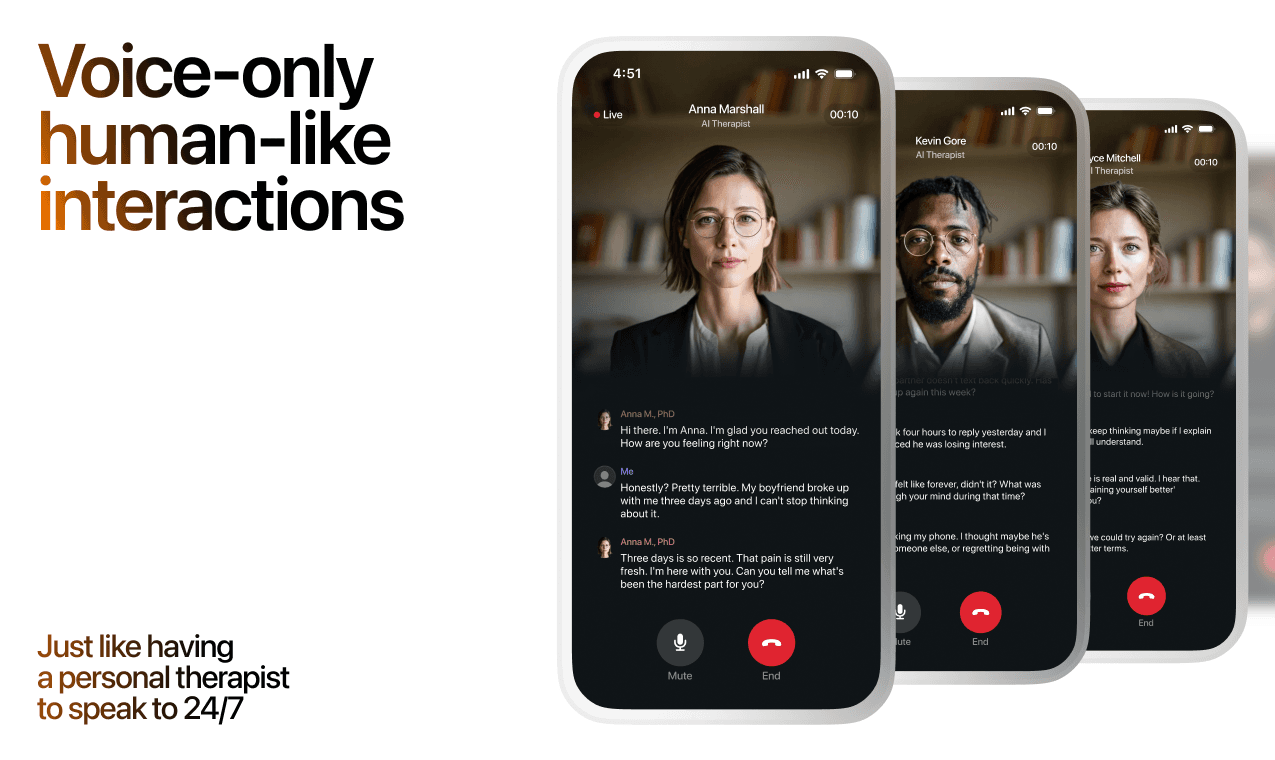
Here's what happens in a typical Lovon session:
You share what's on your mind
There's no script, no intake form, no waiting room. You speak or type whatever you're feeling — in your own words, at your own pace.
Lovon validates and explores
Using frameworks from CBT (Cognitive Behavioral Therapy) and motivational interviewing, Lovon acknowledges your feelings first, then gently helps you explore them. No dismissive "just move on" advice.
You build coping skills together
Lovon doesn't just listen — it actively works with you on evidence-based techniques: thought reframing, urge surfing, behavioral experiments, and more.
What a Session with Lovon Looks Like
When to Seek Professional Help
AI support is a valuable tool, but it's not a replacement for professional care. Please consider reaching out to a licensed therapist if you experience any of the following:
- Persistent thoughts of self-harm or suicide
- Inability to perform daily activities (work, eating, sleeping) for more than 2 weeks
- Turning to alcohol or substances to cope
- Intense anger or desire to harm your ex-partner
- Complete emotional numbness that doesn't improve over time
Crisis Resources (US): If you're in immediate danger, call 988 (Suicide & Crisis Lifeline) or text HOME to 741741 (Crisis Text Line). Available 24/7, free, and confidential.
Outside the US? Find a crisis line in your country
Ready to Start?
Your healing journey can begin right now
1 free conversation. No credit card. No judgment. Just a safe space to process what you're going through.
Frequently Asked Questions
Is AI therapy a replacement for a real therapist?
Is my conversation with Lovon AI private?
How is Lovon different from ChatGPT for emotional support?
Can I use Lovon if I'm already seeing a therapist?
Can I try Lovon for free?
About the Author
The Lovon Editorial Team
Mental Health & Wellness Content Team
The Lovon Editorial Team develops mental health and wellness content designed to make psychological concepts accessible and actionable. Our goal is to bridge the gap between clinical research and everyday life - helping you understand why your mind works the way it does and what you can do about it....
Similar Articles
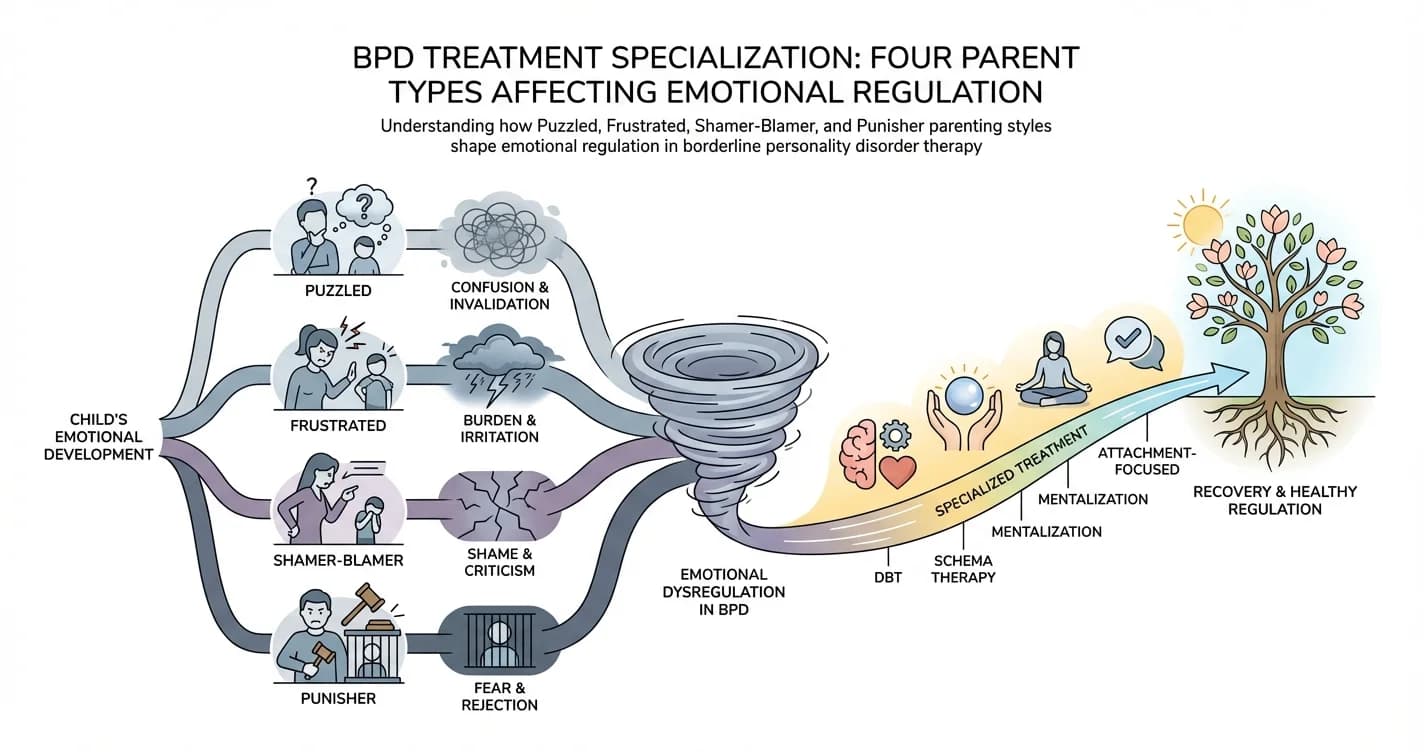
BPD Treatment Specialization: Four Parent Types Affecting Emotional Regulation
For individuals with borderline personality disorder (BPD), emotional regulation difficulties rarely emerge in isolation. Research increasingly suggests that
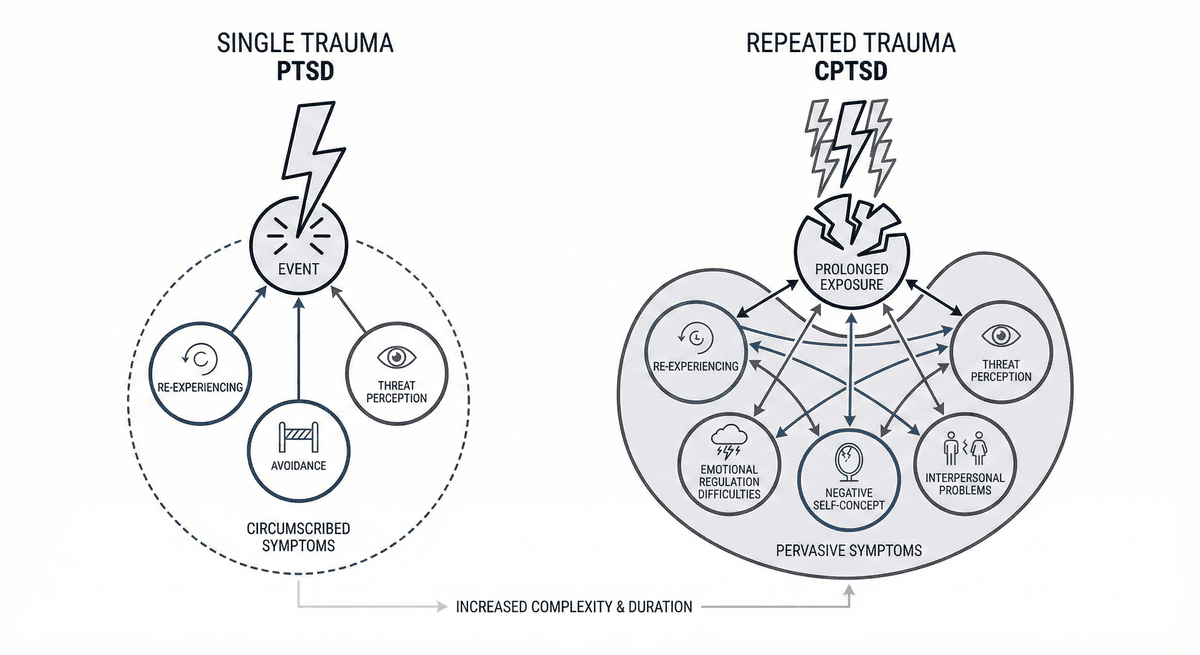
PTSD vs CPTSD: Single Trauma vs Repeated Trauma Symptom Differences
Learn how PTSD from a single traumatic event differs from CPTSD shaped by repeated trauma, including symptom patterns and treatment approaches.
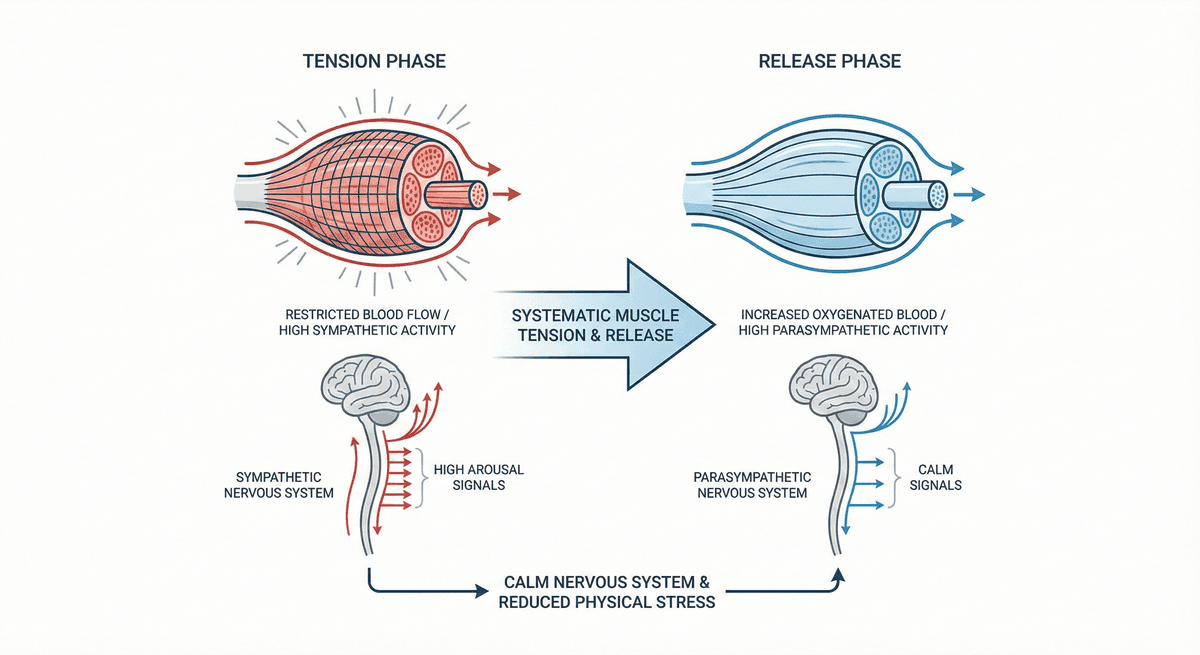
Progressive Muscle Relaxation for Stress Reduction
A systematic muscle group tension and release technique that calms the nervous system and reduces physical stress.
Disclaimer: This article is for informational purposes only and does not constitute medical advice, diagnosis, or treatment. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition. If you are in crisis or think you may have an emergency, call 988 (Suicide & Crisis Lifeline) or go to the nearest emergency room. Outside the US? Find a crisis line in your country.