Relationship PTSD: 7 Signs of Post-traumatic Stress Disorder
Most people think PTSD happens after big disasters, but PTSD from a relationship is more common than many people think.
Key Takeaways
- Someone with PTSD from a relationship may still feel strong trauma symptoms even after it ends
- Complex trauma often develops from long-term emotional or psychological abuse
- Trauma symptoms can lead to serious relationship problems in future connections
- Healing is possible, but someone with PTSD may need support to manage complex trauma and rebuild trust
Introduction
Most people think PTSD happens after big disasters, but PTSD from a relationship is more common than many people think. A close relationship can cause trauma too. This can feel even more confusing, because the person who hurt you was also someone you trusted. If you left a toxic or abusive relationship but still have symptoms, this information can help you.
Can You Actually Get PTSD from a Relationship?
Yes. The Diagnostic and Statistical Manual of Mental Disorders, Fifth Edition says PTSD can happen after real or threatened death, serious injury, or sexual violence. This can happen in abusive relationships, including physical or sexual abuse and threats. Long-term emotional abuse, control, humiliation, and living with an unpredictable partner can also cause trauma and PTSD. Research, including studies in the Journal of Anxiety Disorders, shows that PTSD is much more common in people who experienced partner abuse.
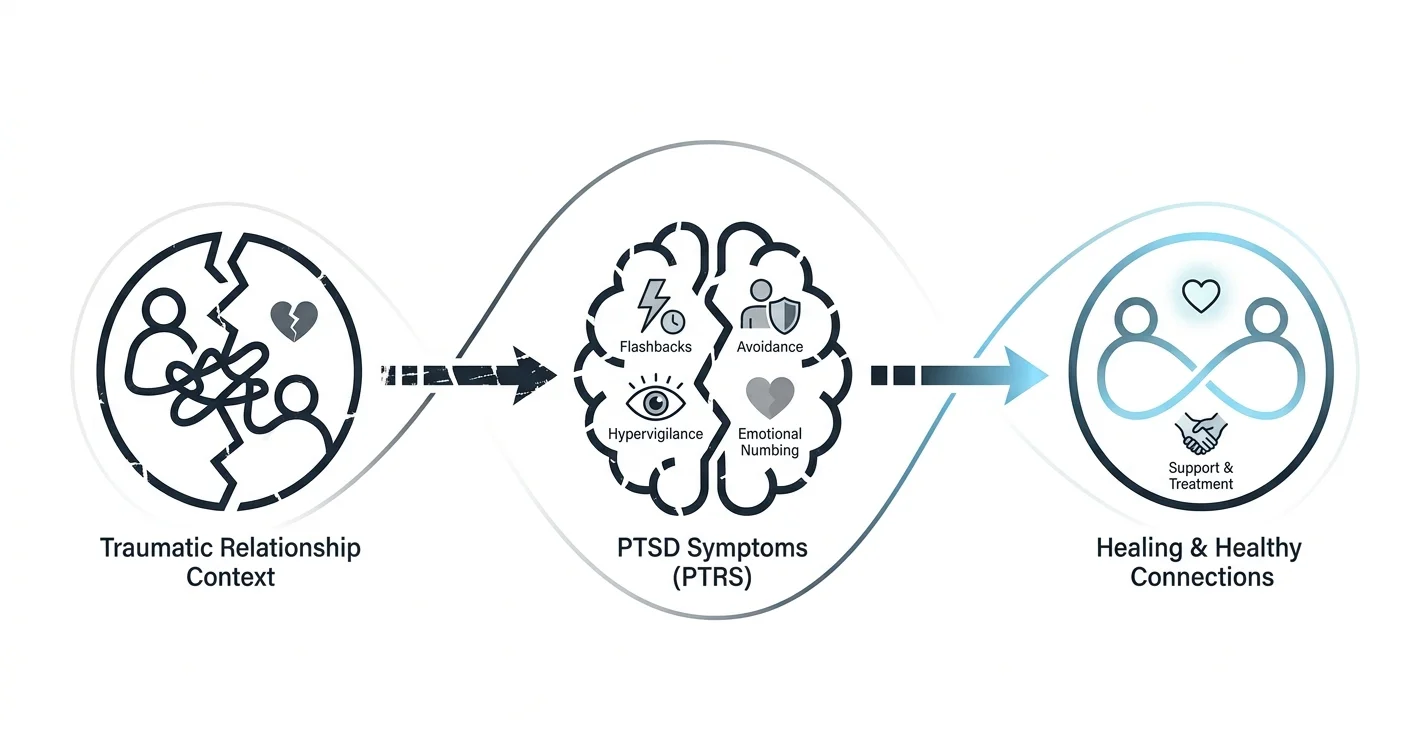
Post-Traumatic Relationship Syndrome: Understanding the Specific Context
Post-traumatic relationship syndrome (PTRS) is a term by Sandra Porterfield. It describes PTSD symptoms that come from an abusive relationship. Trauma in a relationship is different. The person who caused harm was also someone you trusted for safety and care. This can affect self-worth and future relationships more deeply.
Complex PTSD also comes from long-term abuse. It includes PTSD symptoms plus problems with emotions, identity, and relationships. The Diagnostic and Statistical Manual of Mental Disorders, Fifth Edition does not list complex PTSD as a separate diagnosis, but it is included in ICD-11.
7 Signs of Relationship PTSD Symptoms
Relationship trauma can linger and affect how you feel and act in new connections. Here are key signs to watch for.
Flashbacks and Intrusive Trauma Memories
A flashback is a re-experiencing of the traumatic event as though it is happening in the present moment, with the associated emotional and physical sensations intact. Flashbacks may be triggered by sensory cues: a tone of voice, a phrase, a smell, a physical posture that resembles something from the traumatic relationship.
Trauma memories from an abusive relationship are stored differently by the traumatized nervous system: fragmented, context-free, and easily activated by stimuli that bear even partial resemblance to the original experience. This is why individuals with PTSD from past relationships may react intensely to things in a healthy relationship that objectively do not warrant the reaction.
Avoidance of Reminders of the Traumatic Relationship
Avoidance is a key symptom of PTSD. In relationship PTSD, it can mean not going to places linked to the past relationship, not talking about it, pushing away thoughts and feelings, or even avoiding close relationships. This can help in the short term. But over time, it can limit a person’s life and make the fear stronger.
Emotional Numbing and Detachment
Many people with PTSD from past relationships feel emotionally numb. They may not feel positive emotions, feel distant from others, lose interest in things they liked, or feel like they are watching their life from the outside. This numbness is a way to protect themselves. But it also makes close relationships harder, not because they do not want connection, but because their emotions are less active after long-term stress.
Negative Changes in Beliefs About Yourself and Relationships
One key symptom of PTSD is strong negative beliefs about yourself, others, and the future. In relationship trauma, these can include:
- "I am fundamentally unlovable or damaged"
- "I cannot trust my own judgment about people"
- "All relationships end in pain"
- "I deserved what happened to me"
- "I am not safe with other people"
Hypervigilance in Close Relationships
People with PTSD from a traumatic relationship often develop a heightened state of alertness specifically in intimate contexts. This looks like constantly monitoring a new partner's mood, scanning for signs of anger, interpreting neutral behavior as potentially threatening, and finding it genuinely difficult to relax in a romantic relationship even when the current partner is safe and caring. This is the nervous system doing exactly what it learned to do in the abusive relationship: staying one step ahead of potential threats to minimize harm.
Physical Symptoms and Somatic Responses
PTSD symptoms also affect the body. People may have bad sleep, nightmares, feel very tired, have pain, stomach problems, and strong stress reactions that can affect the heart and immune system over time. With relationship PTSD, the body can react in close situations with physical symptoms like fast heartbeat, shallow breathing, muscle tension, or nausea. These reactions can be triggered by touch, situations, or reminders of the past relationship. The body remembers what happened, even when the person is trying to move on.
Difficulties in a Subsequent Healthy Relationship
PTSD can make it hard to be in a new relationship, even if it is safe. Common signs include seeing normal behavior as a threat, feeling emotionally distant, fear of being open, pulling away early, and repeating old conflict patterns with a new partner. Many people feel like they are ruining good relationships. But this is the body and mind reacting based on past trauma.
Relationship PTSD Symptoms vs. Normal Post-Breakup Distress
Not every painful breakup produces PTSD, and distinguishing between normal post-breakup grief and clinical PTSD matters for understanding what kind of support is needed.
| | Normal post-breakup distress | Relationship PTSD | | --- | --- | --- | | Duration | Gradually reduces over weeks to months | Persists or intensifies over time without treatment | | Flashbacks | Memories are painful but feel like memories | Re-experiencing with present-tense emotional and physical intensity | | Functioning | Disrupted initially but recovers | Significantly and persistently impaired | | New relationships | Caution is normal; trust rebuilds gradually | Extreme difficulty; symptoms activate within new relationships | | Physical symptoms | Grief-related fatigue and appetite changes | Chronic hyperarousal, sleep disruption, somatic fear responses | | Self-concept | Sadness and loss without fundamental identity disruption | Pervasive negative beliefs about self and others | | Triggers | Reminders are sad but manageable | Specific triggers produce intense, involuntary stress responses |
Healing and Developing Healthy Relationships After Relationship PTSD
Recovery from relationship PTSD means the past is part of your story, but it does not control you. Some things that can help:
- Slowly reconnect with people, starting with safe and simple relationships
- Build a sense of safety in your body with movement, rest, and self-care
- Be honest with a new partner, so they understand your reactions
- Work on negative beliefs about yourself and others, often with a therapist
Mental Health Treatment for Relationship PTSD
The good news is that PTSD treatment is effective. People with PTSD, including those whose symptoms developed within an intimate relationship, recover with appropriate care. The following approaches have the strongest evidence base.
Cognitive Processing Therapy
Cognitive processing therapy, or CPT, is one of the most extensively researched PTSD treatments available. It focuses specifically on the stuck points, the negative beliefs about self, others, and the world that trauma installs, and works to help the person examine and revise those beliefs in the light of evidence. For relationship PTSD, CPT is particularly useful for addressing the self-blame, shame, and distorted beliefs about one's own worth that emotional and sexual abuse tend to produce.
Prolonged Exposure Therapy
Prolonged exposure therapy works by systematically and safely approaching trauma memories and trauma-related situations that have been avoided, reducing the power of those memories and stimuli over time. Prolonged exposure directly targets the maintenance mechanism.
EMDR
Eye movement desensitization and reprocessing works by facilitating the reprocessing of traumatic memories through bilateral sensory stimulation, reducing the emotional charge associated with those memories without requiring extensive verbal processing. Many people who have not fully responded to talk-based therapy for post-traumatic stress disorder find EMDR useful.
Therapy for Relationship PTSD
A safe, boundaried, and genuinely caring therapeutic relationship is often the first experience of a trustworthy intimate connection that the person has had in some time. This is part of how healing happens.
Medication
SSRIs and SNRIs are the most commonly prescribed medications for PTSD and can reduce PTSD symptom severity, particularly the hyperarousal and mood-related symptoms, while the person engages in trauma-focused therapy. Medication can help reduce symptoms, but it does not fix the problem completely. It should only be taken with a doctor’s prescription, because wrong self-treatment can cause more harm.
Online Therapy
Online therapy for post-traumatic stress disorder symptoms shows comparable outcomes to in-person treatment for many people. Lovon offers private access to licensed professionals who can provide therapy for this problem from wherever you are.
When to Seek Help?
Please consider speaking with a mental health professional if:
- You recognize the signs described in this article in yourself
- The relationship ended but the distress did not, and it has not reduced significantly with time
- You are experiencing flashbacks, nightmares, or intrusive trauma memories related to a past relationship
- You are using dissociation or other avoidance strategies to manage the distress
- Your current relationships are being significantly affected by responses you connect to a previous traumatic relationship
- You have been diagnosed with PTSD or suspect you may meet the criteria
Sources and Further Reading
We used these sources to create this article and help you feel better. You can explore them to get a deeper understanding of the topic:
- Cognitive processing therapy for sexual assault victims. Journal of Consulting and Clinical Psychology. PubMed
- Betrayal Trauma: The Logic of Forgetting Childhood Abuse. Harvard University Press
- Eye Movement Desensitization and Reprocessing (EMDR) Therapy. Guilford Press
- Diagnostic and Statistical Manual of Mental Disorders, Fifth Edition (DSM-5). APA Publishing
How AI Support Helps You Heal
AI emotional support isn't about replacing human connection — it's about filling the gaps. The moments when you need to talk at 2 AM, when you don't want to burden your friends again, or when you simply need someone to listen without judgment.
Here's what happens in a typical Lovon session:
You share what's on your mind
There's no script, no intake form, no waiting room. You speak or type whatever you're feeling — in your own words, at your own pace.
Lovon validates and explores
Using frameworks from CBT (Cognitive Behavioral Therapy) and motivational interviewing, Lovon acknowledges your feelings first, then gently helps you explore them. No dismissive "just move on" advice.
You build coping skills together
Lovon doesn't just listen — it actively works with you on evidence-based techniques: thought reframing, urge surfing, behavioral experiments, and more.
What a Session with Lovon Looks Like
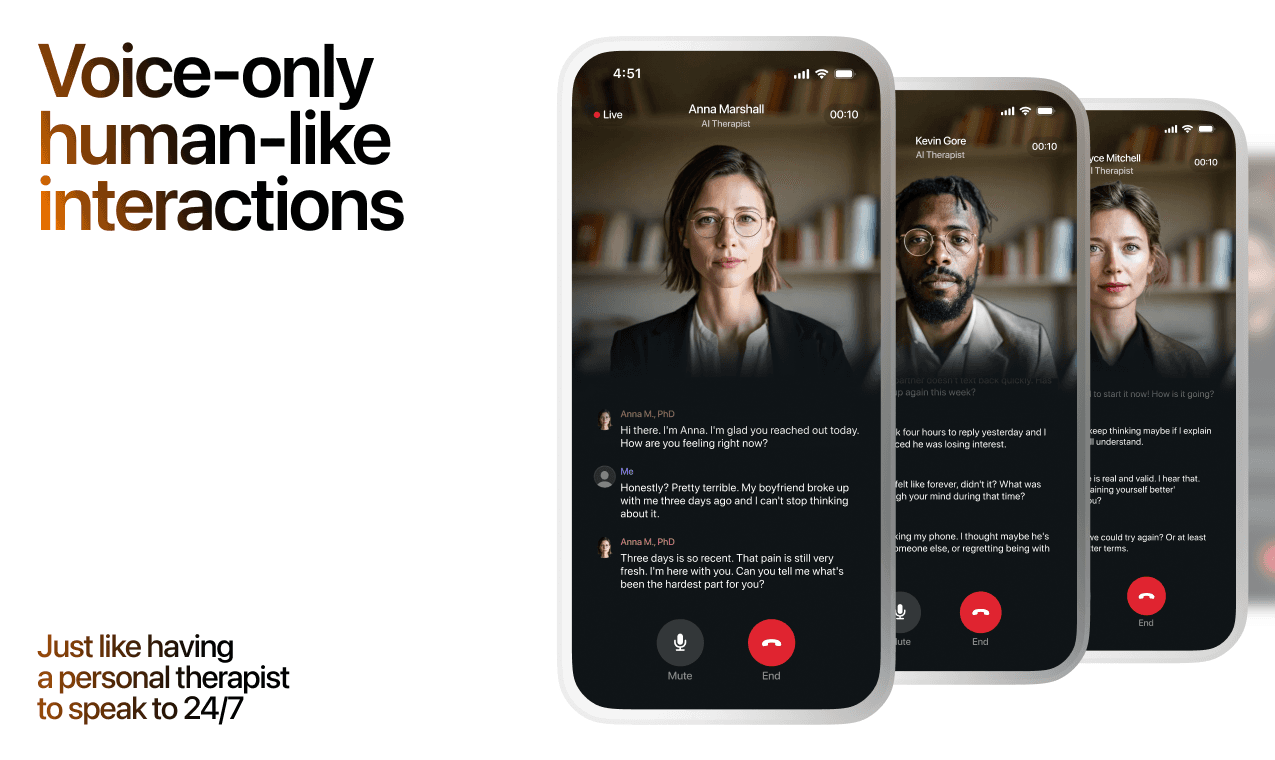
When to Seek Professional Help
AI support is a valuable tool, but it's not a replacement for professional care. Please consider reaching out to a licensed therapist if you experience any of the following:
- Persistent thoughts of self-harm or suicide
- Inability to perform daily activities (work, eating, sleeping) for more than 2 weeks
- Turning to alcohol or substances to cope
- Intense anger or desire to harm your ex-partner
- Complete emotional numbness that doesn't improve over time
Crisis Resources (US): If you're in immediate danger, call 988 (Suicide & Crisis Lifeline) or text HOME to 741741 (Crisis Text Line). Available 24/7, free, and confidential.
Outside the US? Find a crisis line in your country
Ready to Start?
Your healing journey can begin right now
1 free conversation. No credit card. No judgment. Just a safe space to process what you're going through.
Frequently Asked Questions
Q: Is it possible to develop PTSD from a relationship that was not recognized as abusive at the time?
Q: How is relationship PTSD different from complex PTSD?
Q: How do I know if I need therapy for PTSD specifically, rather than general counseling?
Q: Will I be able to trust people again after a traumatic relationship?
Q: Can veterans with PTSD from combat also experience relationship PTSD simultaneously?
Q: How long does PTSD from a relationship typically last without treatment?
Q: Can a breakup cause PTSD even if the relationship was not physically abusive?
About the Author
Mireya Tabasa
Mental Health Support Specialist & AI Advisor
Mireya Tabasa is a Mental Health Support Specialist working at the intersection of clinical care and technology. With over 4 years of hands-on experience supporting diverse populations facing mental health challenges in educational and healthcare settings, she brings frontline clinical insight to ev...
Similar Articles
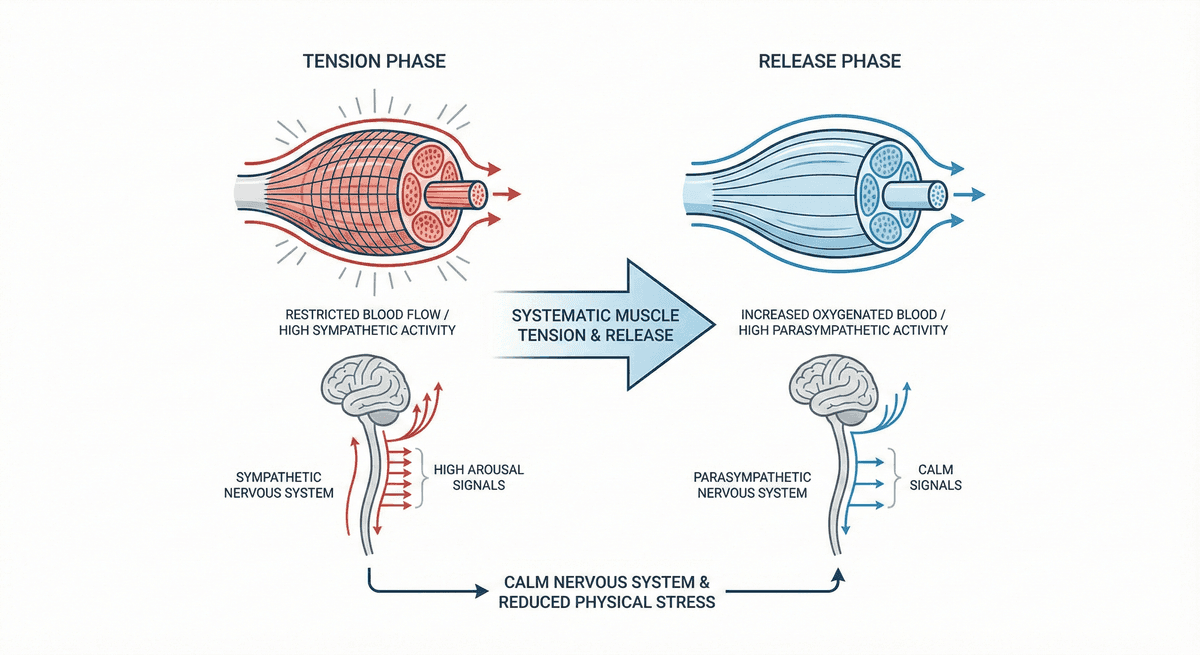
Progressive Muscle Relaxation for Stress Reduction
A systematic muscle group tension and release technique that calms the nervous system and reduces physical stress.
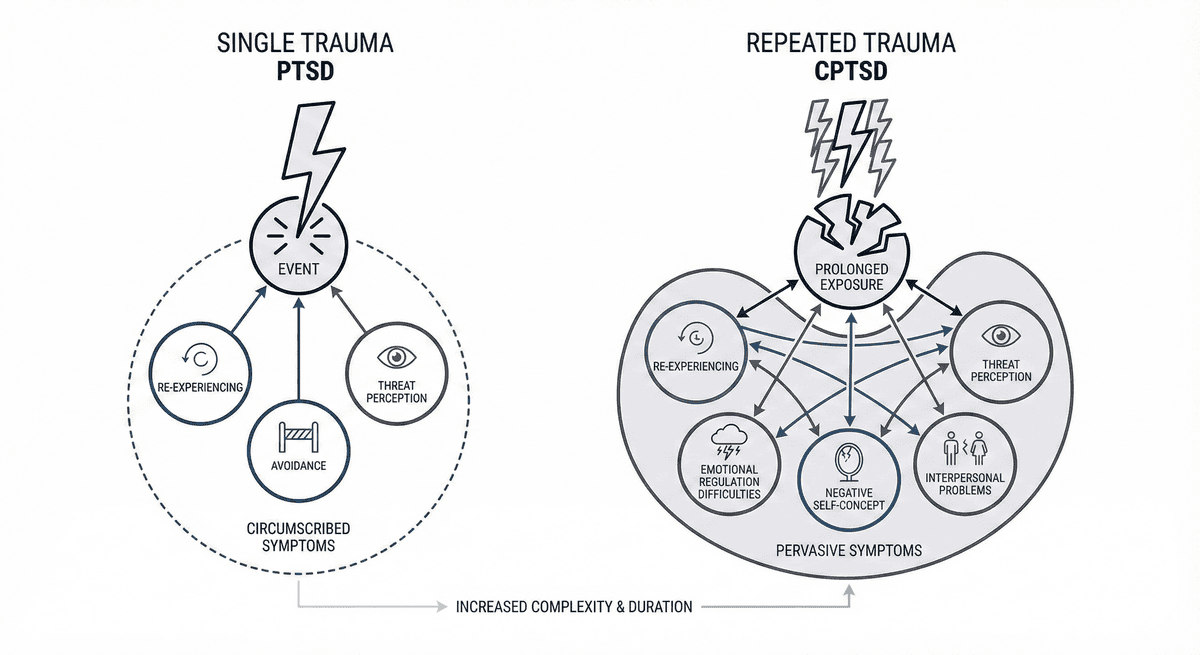
PTSD vs CPTSD: Single Trauma vs Repeated Trauma Symptom Differences
Learn how PTSD from a single traumatic event differs from CPTSD shaped by repeated trauma, including symptom patterns and treatment approaches.
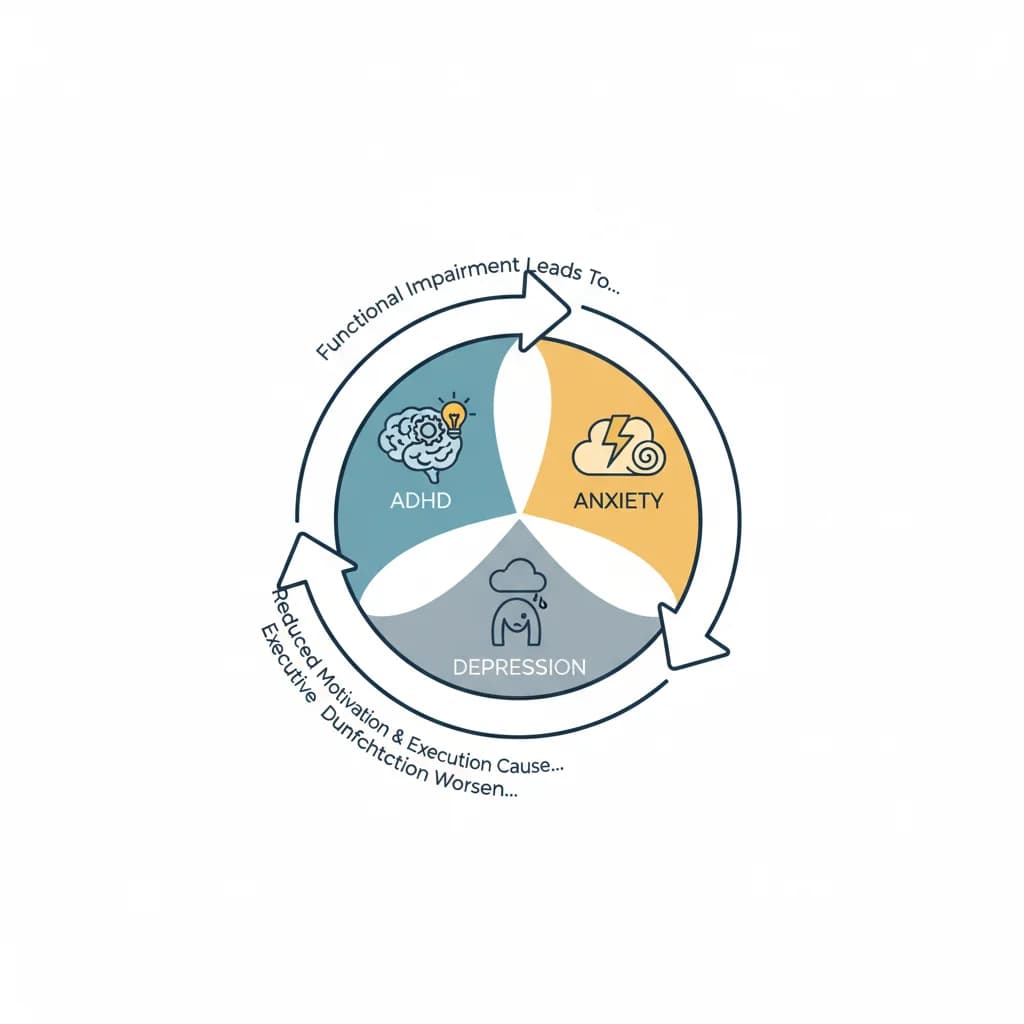
ADHD Comorbidity with Anxiety and Depression Cycles
Understanding the Complex Interplay Between ADHD and Recurring Mental Health Patterns
Disclaimer: This article is for informational purposes only and does not constitute medical advice, diagnosis, or treatment. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition. If you are in crisis or think you may have an emergency, call 988 (Suicide & Crisis Lifeline) or go to the nearest emergency room. Outside the US? Find a crisis line in your country.
