Understanding CPTSD Symptom Expansion and How It Affects Recovery
When people begin addressing their Complex PTSD, many encounter an unexpected and disorienting phenomenon: their symptoms seem to get worse before they...

Key Takeaways
- When people begin addressing their Complex PTSD, many encounter an unexpected and disorienting phenomenon: their
- This experience, often referred to as CPTSD symptom expansion, describes the temporary intensification or
- Rather than indicating failure or regression, symptom expansion often reflects the nervous system's initial response
Introduction
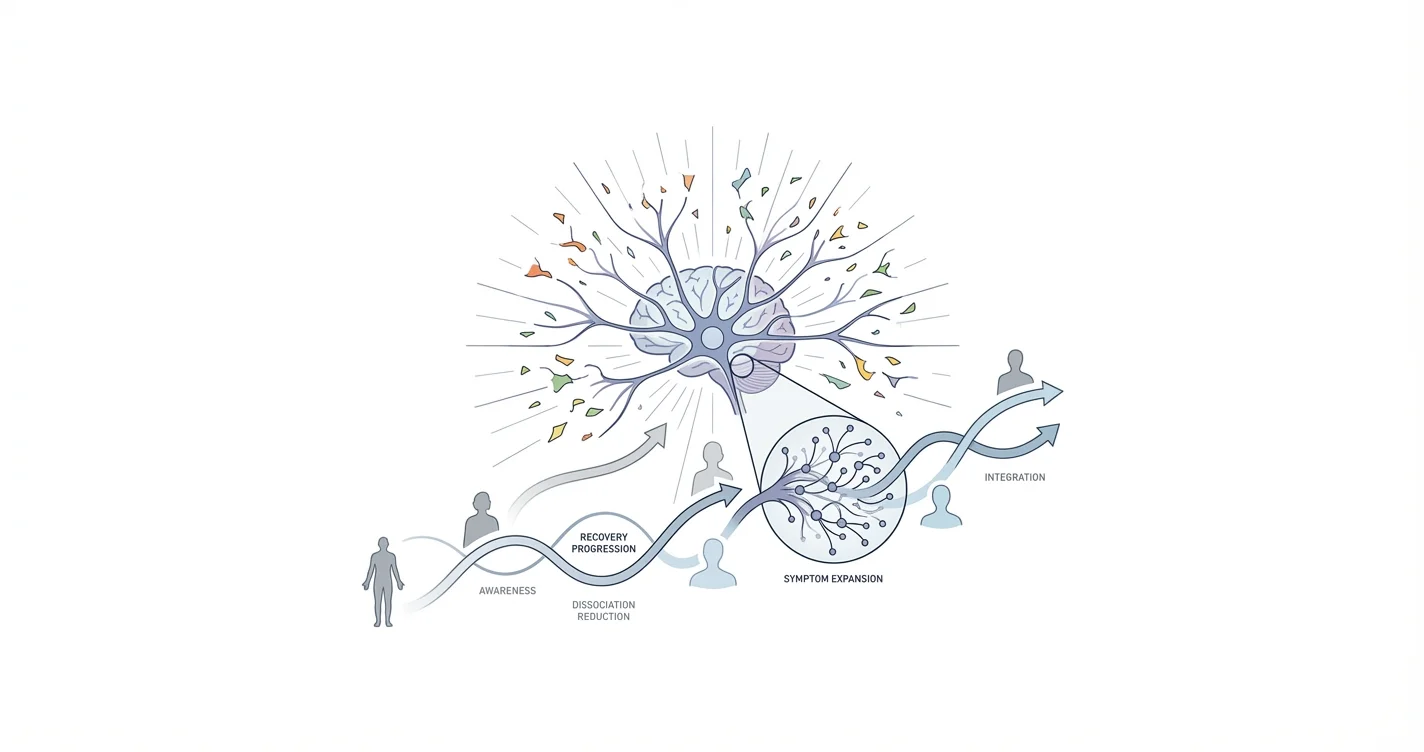
When people begin addressing their Complex PTSD, many encounter an unexpected and disorienting phenomenon: their symptoms seem to get worse before they get better. This experience, often referred to as CPTSD symptom expansion, describes the temporary intensification or multiplication of trauma-related symptoms that can occur when survivors start therapy, practice new coping skills, or simply become more aware of their emotional patterns. Rather than indicating failure or regression, symptom expansion often reflects the nervous system's initial response to change and the conscious mind's growing awareness of previously suppressed experiences. Understanding this process can help survivors recognize it as a potentially normal—though challenging—phase of recovery rather than evidence that healing isn't working.
What CPTSD Symptom Expansion Actually Means
CPTSD symptom expansion refers to the phenomenon where survivors of complex trauma notice an increase in symptom frequency, intensity, or variety as they begin recovery work. Research on trauma processing suggests that when defensive mechanisms start to relax—through therapy, safety, or conscious attention—previously compartmentalized emotional material may surface more readily. This can manifest as heightened emotional reactivity, more frequent flashbacks, increased hypervigilance, or the emergence of symptoms that seemed less prominent before treatment began.
The term "expansion" captures how symptoms may feel like they're spreading into more areas of life or becoming harder to ignore. A person who previously experienced emotional numbness might suddenly feel overwhelmed by intense emotions. Someone whose hypervigilance was manageable in controlled environments might notice it activating in situations that previously felt safe. Clinical observations indicate this often occurs during the early stages of trauma-focused therapy or when survivors make significant life changes that challenge old coping patterns.
Importantly, symptom expansion differs from genuine deterioration. While both involve increased distress, expansion typically occurs in the context of active healing work and often includes moments of insight, emotional release, or new awareness alongside the discomfort. Survivors may notice they're feeling more but also understanding more about why they respond the way they do.
Why Complex PTSD Symptoms Can Intensify During Healing
Several interconnected mechanisms appear to contribute to symptom expansion in Complex PTSD recovery:
Decreased dissociation and increased awareness. Many CPTSD survivors develop sophisticated dissociative defenses that keep traumatic material out of conscious awareness. As therapy or healing practices reduce dissociation, previously blocked emotions, memories, and body sensations can surface more readily. This increased awareness means symptoms that were always present but hidden become consciously noticeable—creating the experience of symptoms expanding even though the underlying trauma response hasn't necessarily worsened.
Nervous system recalibration. The autonomic nervous system in complex trauma survivors often operates with heightened baseline activation. When therapeutic interventions begin to shift these patterns, the nervous system may initially respond with increased instability as it searches for new equilibrium. Studies on trauma neurobiology suggest the nervous system doesn't immediately "know" the difference between genuine threat and the vulnerable feelings that arise during healing—both can trigger protective responses.
Relaxation-induced anxiety. Paradoxically, as survivors begin to feel safer, their defenses may temporarily lower, allowing suppressed fear and vulnerability to emerge. Clinical experience shows that people with complex trauma often unconsciously maintain high levels of tension and control to manage their internal state. When these defenses relax even slightly—through therapeutic relationship, medication, or life stability—the emotional material they were containing can flood forward.
Attachment activation in therapy. For many complex trauma survivors, the therapeutic relationship itself can trigger attachment-related symptoms. As trust develops and emotional connection deepens, old relational wounds may activate, bringing forward feelings of fear, shame, or need that were suppressed in earlier unsafe relationships. This activation is often necessary for healing but can temporarily intensify symptoms related to abandonment fears, emotional dysregulation, and interpersonal sensitivity.
Recognizing CPTSD Symptom Expansion in Your Recovery
Understanding what symptom expansion actually looks like can help you distinguish it from other experiences during recovery. Common manifestations include:
Emotional intensity changes. You might notice emotions feel more raw, overwhelming, or difficult to regulate than before you started addressing trauma. Feelings you could previously suppress or ignore may demand attention. Some people describe this as "feeling everything" after years of feeling numb, or experiencing emotional reactions that seem disproportionate to current circumstances.
Physical symptom activation. Somatic symptoms—tension, pain, digestive issues, fatigue, or activation in specific body areas—may increase as the body begins processing stored trauma. You might become more aware of how your body holds stress or notice physical sensations connected to emotional states that you previously didn't recognize.
Memory and flashback changes. Rather than memories fading, they might become more vivid, frequent, or emotionally charged. This doesn't mean you're getting worse—emerging research suggests that memory reprocessing often involves initial intensification before integration occurs. You might also recall details or experiences you hadn't thought about in years.
Increased sensitivity to triggers. Situations, relationships, or environments that you managed reasonably well might suddenly feel overwhelming. Your window of tolerance—the zone in which you can process emotion without becoming dysregulated—may temporarily narrow as your system recalibrates.
It's worth noting that symptom expansion doesn't happen to everyone, and its presence or absence doesn't indicate whether healing is occurring. Some people experience gradual, steady improvement without significant intensification periods, while others move through multiple waves of expansion and integration throughout their recovery journey.
How to Navigate CPTSD Symptom Expansion
When you recognize you're experiencing symptom expansion, several approaches can help you move through this phase while maintaining stability:
Maintain therapeutic support and communication. If you're working with a therapist, counselor, or psychiatrist, communicate openly about symptom changes. Professionals experienced in complex trauma expect this phenomenon and can adjust treatment pacing, introduce additional stabilization techniques, or provide reassurance that what you're experiencing fits within normal recovery patterns. If symptoms expand to the point of significantly impacting functioning or safety, your treatment team can help determine whether adjustments are needed.
Prioritize regulation and stabilization practices. During periods of symptom expansion, the priority shifts from processing and exploring trauma to maintaining regulation and safety. This might mean temporarily focusing more on grounding techniques, breathwork, movement practices, or activities that support nervous system calming. Resources like bilateral stimulation exercises, progressive muscle relaxation, or even brief check-ins with support tools like Lovon.app can help you process emotional intensity and identify patterns as they emerge.
Adjust expectations and pace. Recognizing that expansion often precedes integration can help you maintain perspective. This doesn't mean you should push through overwhelming distress, but rather that temporary intensification doesn't necessarily indicate you're moving backward. Some people find it helpful to consciously slow the pace of trauma processing work during expansion phases, focusing instead on building internal and external resources.
Strengthen external supports and structure. Maintaining regular routines, sleep schedules, and connection with safe people provides a containing structure when internal experience feels chaotic. This is also a time when practical support matters—if possible, reduce external stressors, ask for help with daily responsibilities, and build in additional time for rest and self-care.
Track patterns without judgment. Keeping a simple record of symptom intensity, triggers, and what helps can reveal patterns over time. Many people notice that expansion phases, while difficult, are typically time-limited and eventually give way to periods of greater stability and integration. This tracking also helps you and any professionals you work with identify what interventions are actually helpful for you specifically.
When CPTSD Symptom Expansion Requires Additional Support
While symptom expansion can be a normal part of trauma recovery, certain signs indicate the need for increased professional support:
Functional impairment. If symptoms prevent you from maintaining basic self-care, attending work or school, or caring for dependents, this indicates a need for additional stabilization and support. Temporary increase in symptoms shouldn't render you unable to function in essential areas of life for extended periods.
Safety concerns. Thoughts of self-harm, suicidal ideation, or urges to engage in dangerous behaviors require immediate professional attention. Symptom expansion should not include active risk to yourself or others—if it does, this indicates the need for a higher level of care or treatment adjustment.
Sustained distress without relief. While expansion involves increased symptoms, you should still have periods of relative calm, moments of insight or progress, and some response to regulation practices. If distress is unrelenting for weeks without any moments of relief, this may indicate that treatment pacing needs adjustment or that additional interventions would be helpful.
Relationship or life crisis. If symptom expansion is contributing to job loss, relationship ruptures, or other significant life problems, professional support can help you develop strategies to maintain important areas of life while continuing healing work at an appropriate pace.
The Integration Phase: What Comes After Symptom Expansion
For many people who experience CPTSD symptom expansion, this phase eventually transitions into a period of integration where the intensified symptoms begin to settle into new patterns. Integration doesn't necessarily mean symptoms disappear, but rather that they become more manageable, less overwhelming, and more connected to conscious understanding.
During integration, people often report feeling more "in their body," having greater emotional range without being overwhelmed, and noticing that triggers that previously caused intense reactions produce more moderate responses. The insights and awareness that emerged during the expansion phase become incorporated into a more coherent sense of self and history.
This process isn't linear—many survivors move through multiple cycles of expansion and integration throughout recovery. Each cycle may address different layers of experience or activate in response to new life circumstances, deeper therapeutic work, or changing relationships. Understanding this cyclical nature can reduce the disappointment that sometimes comes when symptoms intensify again after a period of relative stability.
Approaches that support integration include continued therapy with attention to meaning-making and narrative development, practices that connect emotional awareness with cognitive understanding, and gradual increases in life engagement as capacity allows. Some people find that on-demand resources like Lovon.app help them process emerging patterns between therapy sessions and prepare for deeper therapeutic work by organizing their thoughts and emotional responses.
Conclusion
CPTSD symptom expansion—the temporary intensification or multiplication of complex trauma symptoms during recovery—represents one of the more challenging yet often normal phases of healing. Rather than indicating failure, this phenomenon frequently reflects the nervous system's response to change, decreased dissociation, and the emergence of previously suppressed emotional material as safety increases. Recognizing symptom expansion for what it is can help survivors maintain perspective during difficult periods and trust the process even when progress feels counterintuitive. By prioritizing stabilization, maintaining professional support, and understanding that intensification often precedes integration, you can navigate this phase while continuing to move toward greater healing. If you're experiencing symptom changes that concern you, discussing them openly with a trauma-informed therapist or counselor can help determine whether what you're experiencing fits within expected patterns or requires treatment adjustment.
Disclaimer: This is general information, not medical advice or diagnosis. If symptoms are severe, affecting your daily life, or you're having thoughts of self-harm — seek professional help. In the US: call or text 988 (Suicide & Crisis Lifeline). For immediate danger: 911 or local emergency services.
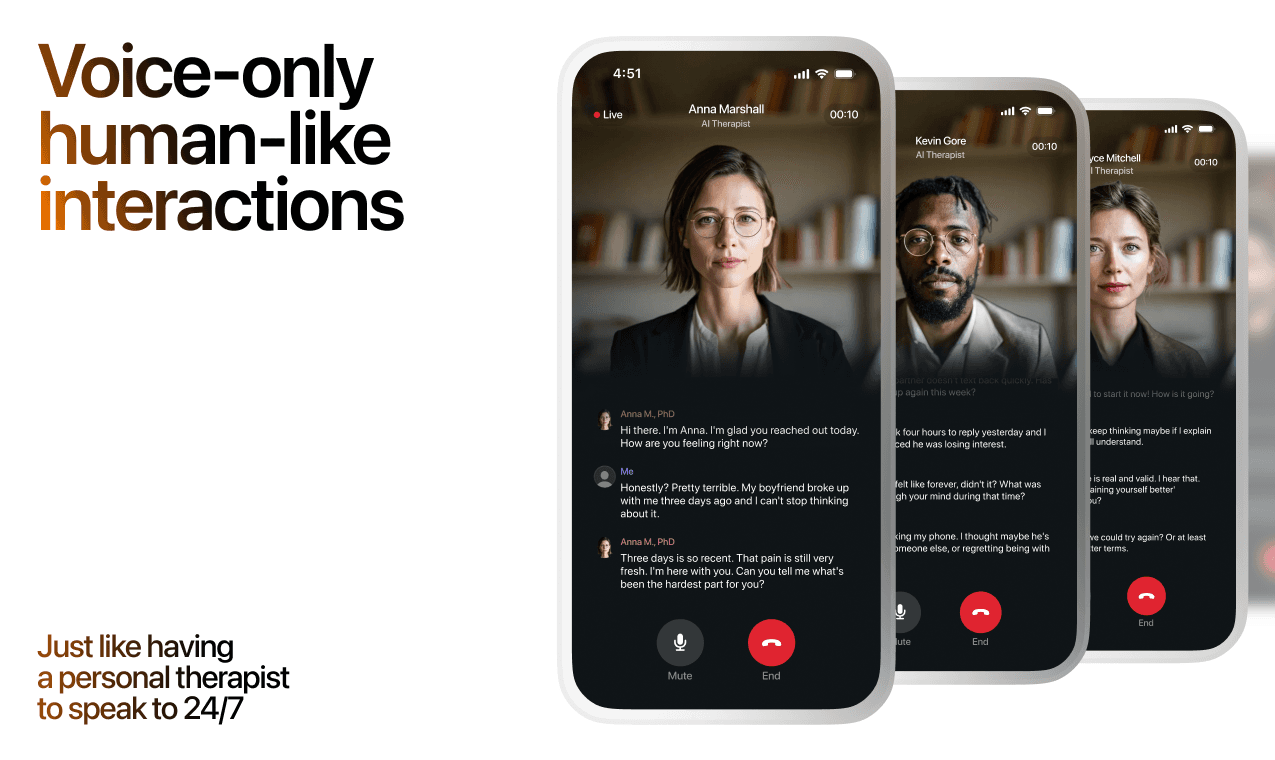
How AI Support Helps You Heal
AI emotional support isn't about replacing human connection — it's about filling the gaps. The moments when you need to talk at 2 AM, when you don't want to burden your friends again, or when you simply need someone to listen without judgment.
Here's what happens in a typical Lovon session:
You share what's on your mind
There's no script, no intake form, no waiting room. You speak or type whatever you're feeling — in your own words, at your own pace.
Lovon validates and explores
Using frameworks from CBT (Cognitive Behavioral Therapy) and motivational interviewing, Lovon acknowledges your feelings first, then gently helps you explore them. No dismissive "just move on" advice.
You build coping skills together
Lovon doesn't just listen — it actively works with you on evidence-based techniques: thought reframing, urge surfing, behavioral experiments, and more.
What a Session with Lovon Looks Like
When to Seek Professional Help
AI support is a valuable tool, but it's not a replacement for professional care. Please consider reaching out to a licensed therapist if you experience any of the following:
- Persistent thoughts of self-harm or suicide
- Inability to perform daily activities (work, eating, sleeping) for more than 2 weeks
- Turning to alcohol or substances to cope
- Intense anger or desire to harm your ex-partner
- Complete emotional numbness that doesn't improve over time
Crisis Resources (US): If you're in immediate danger, call 988 (Suicide & Crisis Lifeline) or text HOME to 741741 (Crisis Text Line). Available 24/7, free, and confidential.
Outside the US? Find a crisis line in your country
Ready to Start?
Your healing journey can begin right now
1 free conversation. No credit card. No judgment. Just a safe space to process what you're going through.
Frequently Asked Questions
Is AI therapy a replacement for a real therapist?
Is my conversation with Lovon AI private?
How is Lovon different from ChatGPT for emotional support?
Can I use Lovon if I'm already seeing a therapist?
Can I try Lovon for free?
About the Author
The Lovon Editorial Team
Mental Health & Wellness Content Team
The Lovon Editorial Team develops mental health and wellness content designed to make psychological concepts accessible and actionable. Our goal is to bridge the gap between clinical research and everyday life - helping you understand why your mind works the way it does and what you can do about it....
Similar Articles
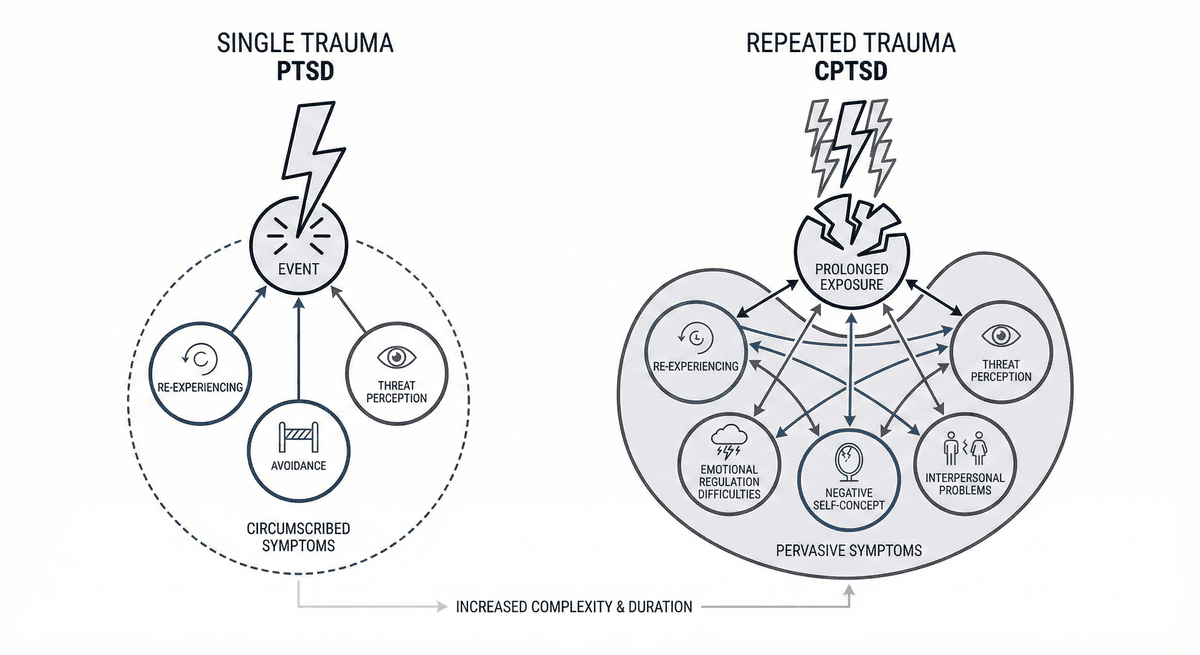
PTSD vs CPTSD: Single Trauma vs Repeated Trauma Symptom Differences
Learn how PTSD from a single traumatic event differs from CPTSD shaped by repeated trauma, including symptom patterns and treatment approaches.
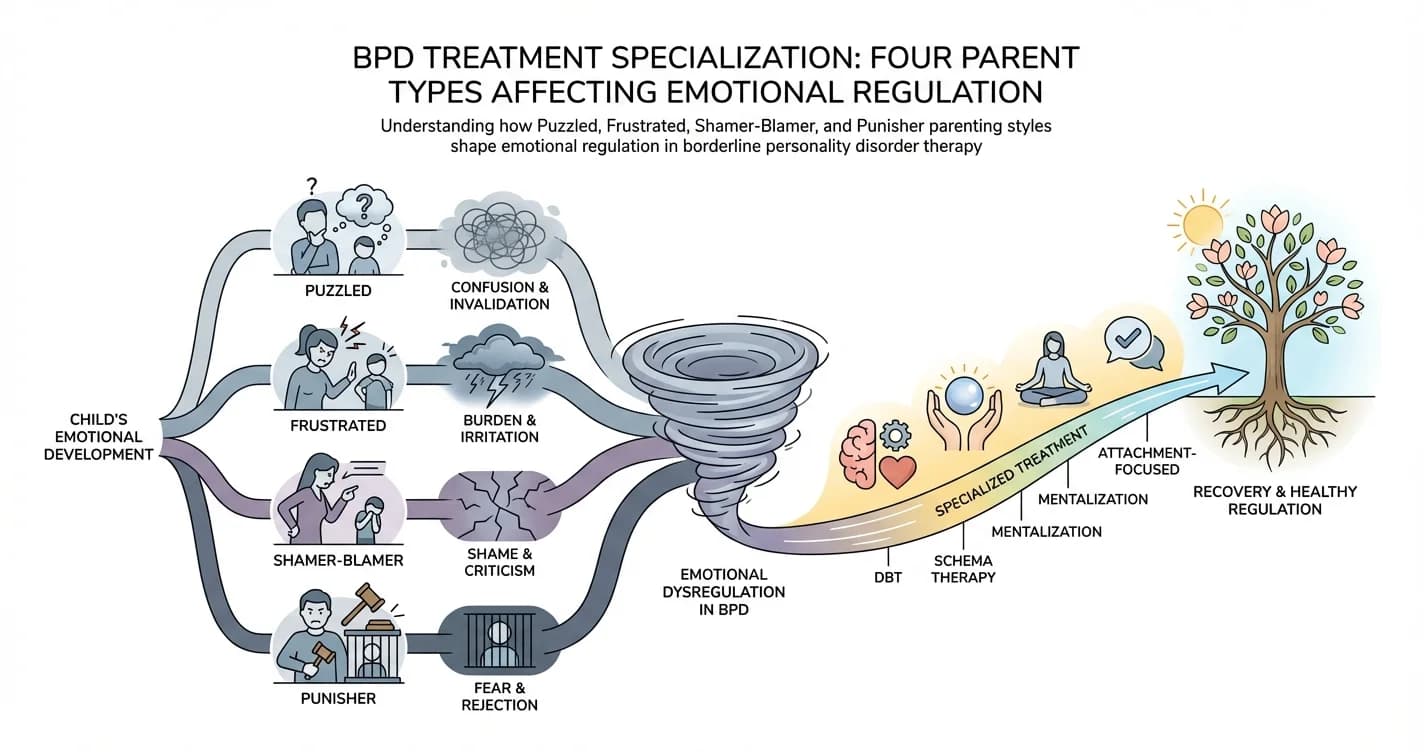
BPD Treatment Specialization: Four Parent Types Affecting Emotional Regulation
For individuals with borderline personality disorder (BPD), emotional regulation difficulties rarely emerge in isolation. Research increasingly suggests that
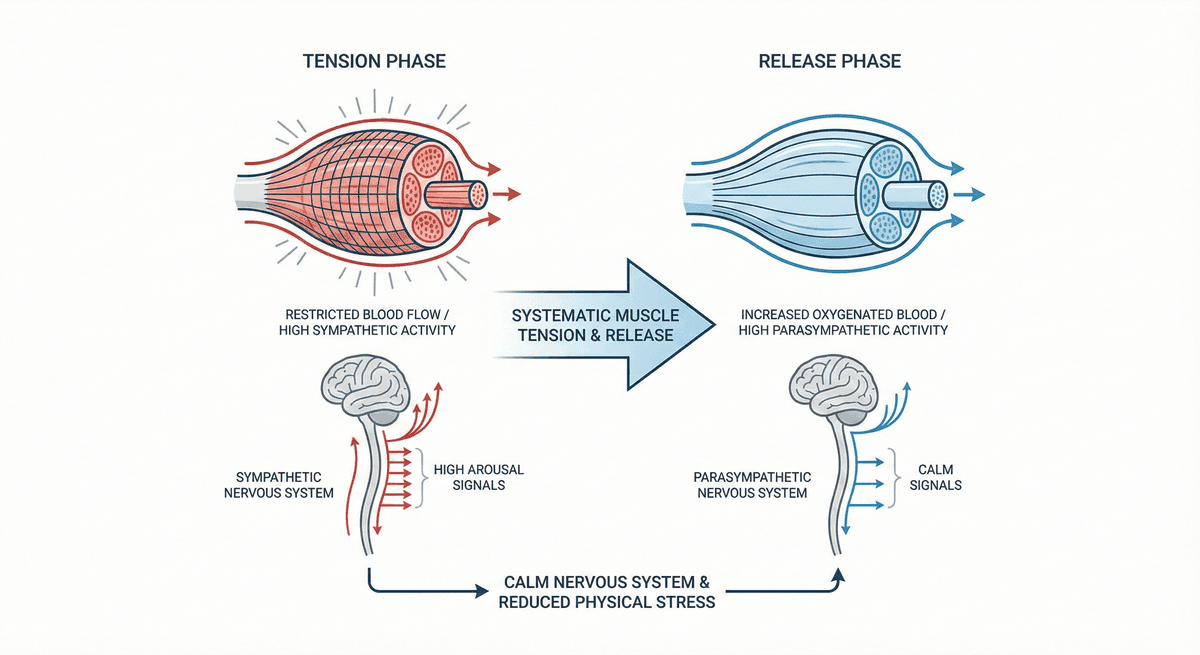
Progressive Muscle Relaxation for Stress Reduction
A systematic muscle group tension and release technique that calms the nervous system and reduces physical stress.
Disclaimer: This article is for informational purposes only and does not constitute medical advice, diagnosis, or treatment. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition. If you are in crisis or think you may have an emergency, call 988 (Suicide & Crisis Lifeline) or go to the nearest emergency room. Outside the US? Find a crisis line in your country.