What is CPTSD from Inconsistent Parenting and How to Heal
Complex Post-Traumatic Stress Disorder (CPTSD) from inconsistent parenting represents a profound psychological injury that develops not from a single...

Key Takeaways
- Emotional dysregulation and difficulty identifying or managing feelings
- Persistent negative self-concept and internalized shame
- Relationship difficulties including fear of abandonment and difficulty trusting
- Hypervigilance to others' emotions and reactions
- Difficulty maintaining consistent sense of self across situations
Introduction
Complex Post-Traumatic Stress Disorder (CPTSD) from inconsistent parenting represents a profound psychological injury that develops not from a single traumatic event, but from chronic exposure to unpredictable caregiving environments. Unlike PTSD stemming from discrete incidents, CPTSD emerges when children grow up never knowing which version of their parent they'll encounter—the loving caregiver one moment, the critical or absent figure the next. This developmental trauma disrupts the formation of core psychological capacities including emotional regulation, stable self-concept, and the ability to form secure relationships. Understanding what CPTSD from inconsistent parenting involves and the pathways toward healing has become increasingly important as mental health professionals recognize how common these patterns are and how treatable they can be with appropriate support.
Understanding CPTSD from Inconsistent Parenting
Complex PTSD from inconsistent parenting develops when children experience ongoing unpredictability in their primary attachment relationships. While genetic factors and individual temperament also contribute to how these patterns develop, the relational environment plays a significant role. The defining feature isn't necessarily overt abuse or severe neglect—it's the chronic uncertainty that prevents children from developing a coherent internal working model of relationships and themselves.
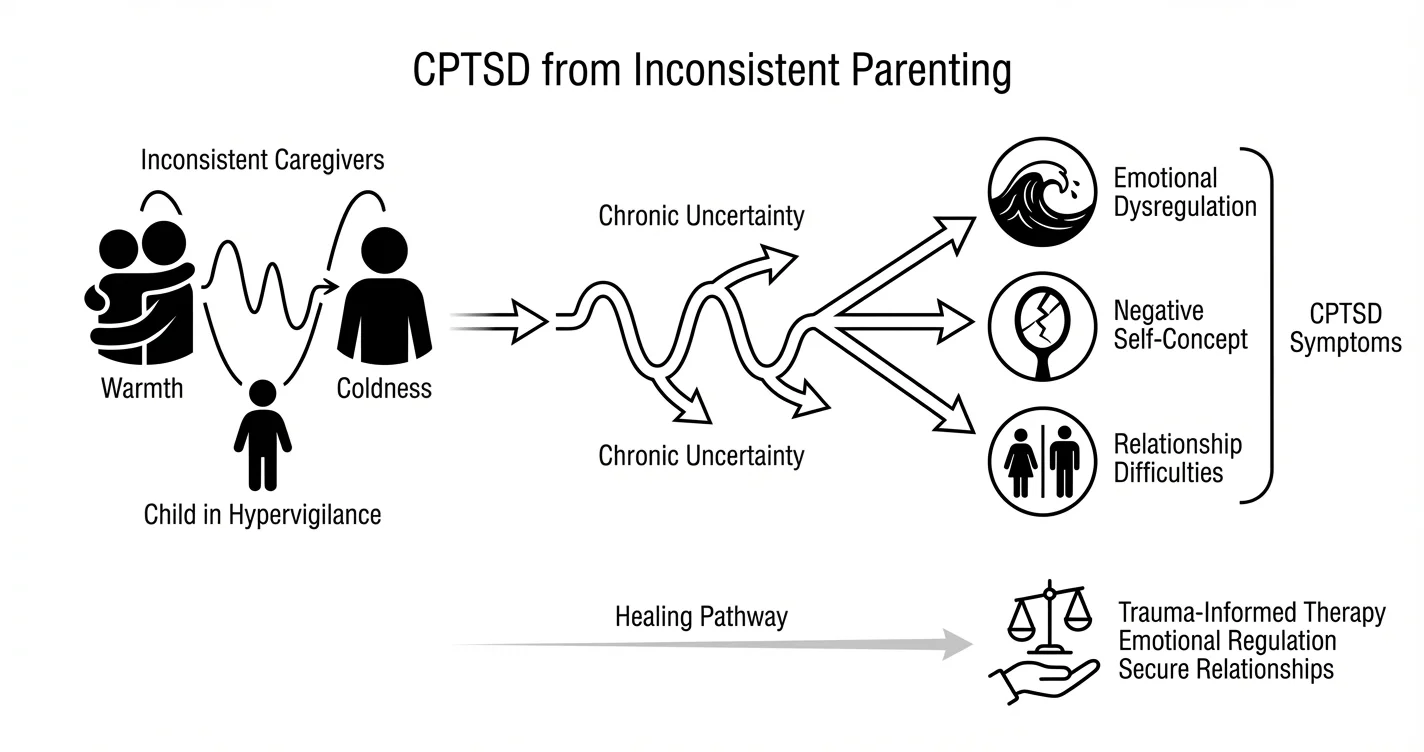
When caregivers oscillate unpredictably between emotional availability and withdrawal, warmth and coldness, or reasonable expectations and unrealistic demands, children remain in a state of hypervigilance. The developing brain adapts to this environment by staying constantly alert to subtle shifts in mood and behavior, trying to predict and prevent negative outcomes. Research suggests this chronic activation of stress response systems during critical developmental periods may alter how the brain processes emotional information and regulates stress throughout life.
The symptoms of CPTSD from inconsistent parenting typically include:
- Emotional dysregulation and difficulty identifying or managing feelings
- Persistent negative self-concept and internalized shame
- Relationship difficulties including fear of abandonment and difficulty trusting
- Hypervigilance to others' emotions and reactions
- Difficulty maintaining consistent sense of self across situations
- Physical symptoms including chronic tension, fatigue, or pain
- Dissociation or feeling disconnected from experiences
CPTSD from Emotional Neglect Versus Childhood Abuse
Understanding the differences between CPTSD from emotional neglect and more overt forms of childhood abuse helps clarify treatment approaches and validates experiences that may have been dismissed as "not that bad." Both can result in complex trauma, but the pathways differ in important ways.
Emotional neglect and inconsistent parenting often fly under the radar because they involve what didn't happen rather than what did. Children may have had their physical needs met while their emotional world went unacknowledged. They learned their feelings were inconvenient, confusing, or unimportant. This creates a particular kind of injury—a void where emotional attunement and consistent validation should have been.
In contrast, CPTSD from overt abuse typically involves experiences that are easier to identify as harmful—physical punishment, verbal attacks, or clear boundary violations. The child knows something wrong is happening, even if they can't escape it. With inconsistent parenting and emotional neglect, children often blame themselves, assuming they're somehow defective rather than recognizing the inadequacy of care they received.
Clinically, CPTSD from inconsistent parenting may present with:
- More difficulty identifying the source of distress ("nothing really bad happened")
- Minimization of their experiences and difficulty claiming their feelings matter
- Confusion about what constitutes healthy relationships
- Particular sensitivity to perceived criticism or emotional withdrawal
- Strong tendency toward self-blame rather than recognizing patterns in caregiving
Both forms of complex trauma respond to similar therapeutic approaches, though individuals from emotionally neglectful or inconsistent backgrounds may need specific help learning to identify their needs and feelings as legitimate.
Why Inconsistent Parenting Causes Complex PTSD
The question of why inconsistent parenting causes complex post-traumatic stress disorder relates to fundamental aspects of human development and nervous system functioning. While genetic predispositions and temperament influence individual responses, understanding these mechanisms helps explain the symptoms and points toward healing.
During early development, children require consistent, predictable responses from caregivers to develop secure attachment and emotional regulation capacities. When caregivers respond inconsistently—sometimes attuned and responsive, other times dismissive or intrusive—children cannot develop reliable mental models of relationships or effective strategies for managing distress.
This unpredictability may be more distressing to the developing nervous system than consistent harshness because it prevents adaptation. With consistent negative treatment, children develop (maladaptive but coherent) coping strategies. With inconsistency, no strategy reliably works, creating chronic uncertainty and helplessness.
The brain may respond similarly to ongoing unpredictability as it does to more obvious threats. When children cannot predict whether expressing needs will result in comfort or rejection, approach or withdrawal, the stress response systems remain chronically activated. Studies indicate that prolonged activation during development may influence how these systems function into adulthood, contributing to emotional reactivity, difficulty relaxing, and heightened threat perception.
Additionally, inconsistent parenting disrupts the development of mentalization—the capacity to understand one's own and others' mental states. Children need caregivers to reflect their experiences accurately and consistently to develop this capacity. When reflections are inconsistent or distorted, children may struggle throughout life to trust their perceptions and understand their emotional experiences.
Healing Complex Trauma from Unstable Childhood
Recovery from complex PTSD caused by unpredictable parenting follows different pathways than treatment for single-incident trauma. The most effective approaches focus on building capacities that inconsistent parenting prevented from developing, rather than solely processing specific memories.
Trauma-Informed Therapy Approaches
Several therapeutic modalities show promise for healing complex trauma from unstable childhood environments. These typically involve longer-term work than PTSD treatment because they address developmental wounds rather than discrete events.
Trauma-focused cognitive behavioral therapy adapted for complex trauma helps individuals identify and modify patterns developed in response to inconsistent caregiving. This might involve recognizing how hypervigilance to others' moods served a protective function but now creates relationship difficulties.
EMDR (Eye Movement Desensitization and Reprocessing) for complex trauma targets not just specific memories but the core negative beliefs developed through repeated experiences. Someone who grew up with inconsistent parenting might work on beliefs like "I'm too much" or "I can never do anything right."
Internal Family Systems therapy helps individuals recognize and work with different parts of themselves that developed in response to unpredictable environments—the hypervigilant protector, the part that learned to minimize needs, the exiled feelings that weren't safe to express.
Building Emotional Regulation Capacities
Since inconsistent parenting often disrupts the development of emotional regulation, healing requires building these capacities in adulthood. This involves:
- Learning to identify and name emotional experiences with increasing specificity
- Developing tolerance for uncomfortable feelings without immediate reactivity
- Understanding emotions as information rather than threats
- Practicing self-soothing strategies that replace early co-regulation experiences
- Building awareness of the connection between thoughts, feelings, and bodily sensations
Resources like Lovon.app can provide on-demand support for processing emotions as they arise, offering a consistent reflection that helps build these capacities between therapy sessions. The ability to talk through feelings late at night or immediately after a triggering situation provides practice in articulating experiences and receiving attuned responses.
Establishing Secure Relationships
Healing from complex trauma from unstable childhood fundamentally involves new relational experiences. While genetic factors and temperament influence relationship patterns, repeated experiences of consistency and attunement can gradually shift expectations and responses.
This happens primarily in therapy but also in carefully chosen relationships where individuals practice:
- Communicating needs directly rather than through indirect signals
- Tolerating moments of disconnection without catastrophizing
- Trusting that repair is possible after conflict
- Recognizing that others' moods aren't always about them
- Allowing themselves to be known rather than constantly adapting
Professional Treatment Options and Step-by-Step Recovery
Approaching recovery from CPTSD symptoms from unreliable caregivers benefits from a structured, phased approach rather than rushing directly into trauma processing. Mental health professionals specializing in complex trauma typically recommend the following progression.
Phase One: Safety and Stabilization
Before addressing traumatic material, establishing current safety and basic coping skills is essential. This phase involves:
- Creating safety in current living situation and relationships
- Developing crisis management strategies for overwhelming emotions
- Building basic self-care routines and identifying support resources
- Learning grounding techniques for managing dissociation or flashbacks
- Addressing any immediate concerns like substance use or self-harm
During this phase, working with a therapist who specializes in complex trauma provides the consistent, predictable relationship that begins to challenge expectations formed in childhood. Some people also find tools like Lovon.app helpful during this phase for processing day-to-day stressors and practicing emotional articulation in a low-stakes environment.
Phase Two: Processing and Mourning
Once stabilization is achieved, the work of processing traumatic experiences and grieving what was lost can begin. This is often the longest and most challenging phase, involving:
- Making sense of childhood experiences and their impact
- Processing specific memories or patterns that cause distress
- Grieving the childhood and parenting that should have been
- Challenging internalized beliefs formed through inconsistent caregiving
- Understanding how survival strategies that once helped now create difficulties
This phase requires patience. The instinct to rush through or minimize these experiences reflects the very patterns being addressed—the sense that feelings are inconvenient or shouldn't matter.
Phase Three: Integration and Reconnection
The final phase involves consolidating gains and building a life aligned with values rather than survival strategies:
- Experimenting with new behaviors in relationships and situations
- Building identity beyond trauma history
- Developing meaningful connections and pursuing valued activities
- Practicing self-compassion and realistic self-appraisal
- Planning for ongoing maintenance of gains
Recovery isn't linear—individuals may move between phases or need to return to earlier work when new challenges arise. This is normal and doesn't indicate failure.
When to Seek Professional Help
While self-help strategies and peer support provide valuable resources, professional treatment is important when CPTSD symptoms significantly impact daily functioning. Consider seeking help from a therapist specializing in complex trauma or attachment issues if you experience:
- Persistent difficulty managing emotions that interferes with work or relationships
- Frequent dissociation, numbness, or feeling disconnected from your life
- Self-harm urges or behaviors
- Substance use to manage emotions
- Inability to maintain relationships due to fear or reactivity
- Intrusive memories, nightmares, or flashbacks
- Severe self-criticism or feelings of worthlessness affecting your ability to function
Licensed therapists, particularly those trained in trauma-focused modalities like EMDR, DBT, or Internal Family Systems, can provide the specialized support needed for healing complex trauma. Psychiatrists can evaluate whether medication might help manage specific symptoms while you engage in therapy. Many people benefit from a combination of medication management and psychotherapy.
If you're experiencing thoughts of self-harm or suicide, immediate professional intervention is necessary rather than attempting to manage these symptoms independently.
Conclusion
Understanding what CPTSD from inconsistent parenting involves—and recognizing it as a legitimate response to chronic relational unpredictability—represents the first step toward healing. Complex trauma from unstable childhood doesn't require dramatic abuse to be valid; the ongoing uncertainty and lack of emotional attunement create genuine psychological injury. Recovery is possible through trauma-informed therapy, building emotional regulation capacities that inconsistent parenting prevented from developing, and gradually experiencing the consistent, attuned relationships that reshape expectations. The healing journey requires patience and often professional support, but thousands of people successfully navigate this path toward more secure relationships with themselves and others. If you're struggling with symptoms of complex PTSD caused by unpredictable parenting, reaching out to a trauma-informed therapist or utilizing resources like Lovon.app for emotional processing support can provide the consistent reflection needed to begin building new patterns.
Disclaimer: This is general information, not medical advice or diagnosis. If symptoms are severe, affecting your daily life, or you're having thoughts of self-harm—seek professional help. In the US: call or text 988 (Suicide & Crisis Lifeline). For immediate danger: 911 or local emergency services.
How AI Support Helps You Heal
AI emotional support isn't about replacing human connection — it's about filling the gaps. The moments when you need to talk at 2 AM, when you don't want to burden your friends again, or when you simply need someone to listen without judgment.
Here's what happens in a typical Lovon session:
You share what's on your mind
There's no script, no intake form, no waiting room. You speak or type whatever you're feeling — in your own words, at your own pace.
Lovon validates and explores
Using frameworks from CBT (Cognitive Behavioral Therapy) and motivational interviewing, Lovon acknowledges your feelings first, then gently helps you explore them. No dismissive "just move on" advice.
You build coping skills together
Lovon doesn't just listen — it actively works with you on evidence-based techniques: thought reframing, urge surfing, behavioral experiments, and more.
What a Session with Lovon Looks Like
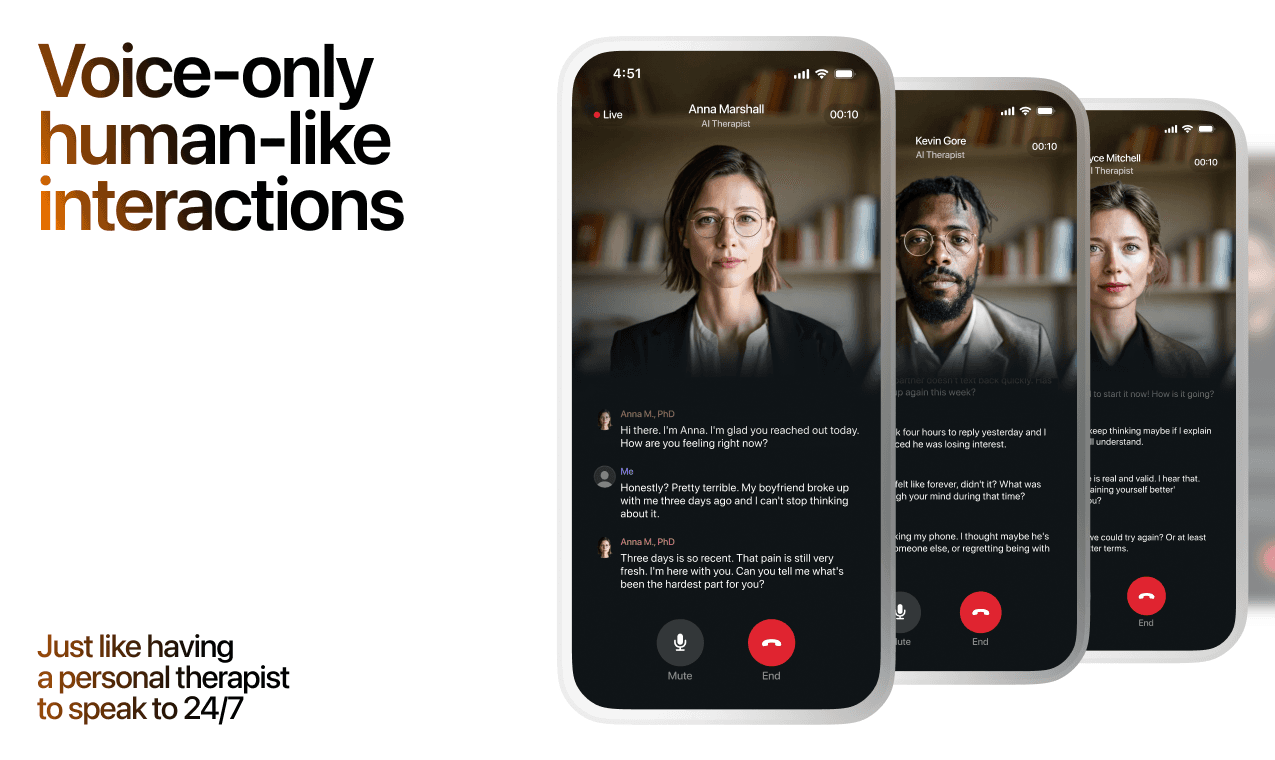
When to Seek Professional Help
AI support is a valuable tool, but it's not a replacement for professional care. Please consider reaching out to a licensed therapist if you experience any of the following:
- Persistent thoughts of self-harm or suicide
- Inability to perform daily activities (work, eating, sleeping) for more than 2 weeks
- Turning to alcohol or substances to cope
- Intense anger or desire to harm your ex-partner
- Complete emotional numbness that doesn't improve over time
Crisis Resources (US): If you're in immediate danger, call 988 (Suicide & Crisis Lifeline) or text HOME to 741741 (Crisis Text Line). Available 24/7, free, and confidential.
Outside the US? Find a crisis line in your country
Ready to Start?
Your healing journey can begin right now
1 free conversation. No credit card. No judgment. Just a safe space to process what you're going through.
Frequently Asked Questions
Is AI therapy a replacement for a real therapist?
Is my conversation with Lovon AI private?
How is Lovon different from ChatGPT for emotional support?
Can I use Lovon if I'm already seeing a therapist?
Can I try Lovon for free?
About the Author
The Lovon Editorial Team
Mental Health & Wellness Content Team
The Lovon Editorial Team develops mental health and wellness content designed to make psychological concepts accessible and actionable. Our goal is to bridge the gap between clinical research and everyday life - helping you understand why your mind works the way it does and what you can do about it....
Similar Articles
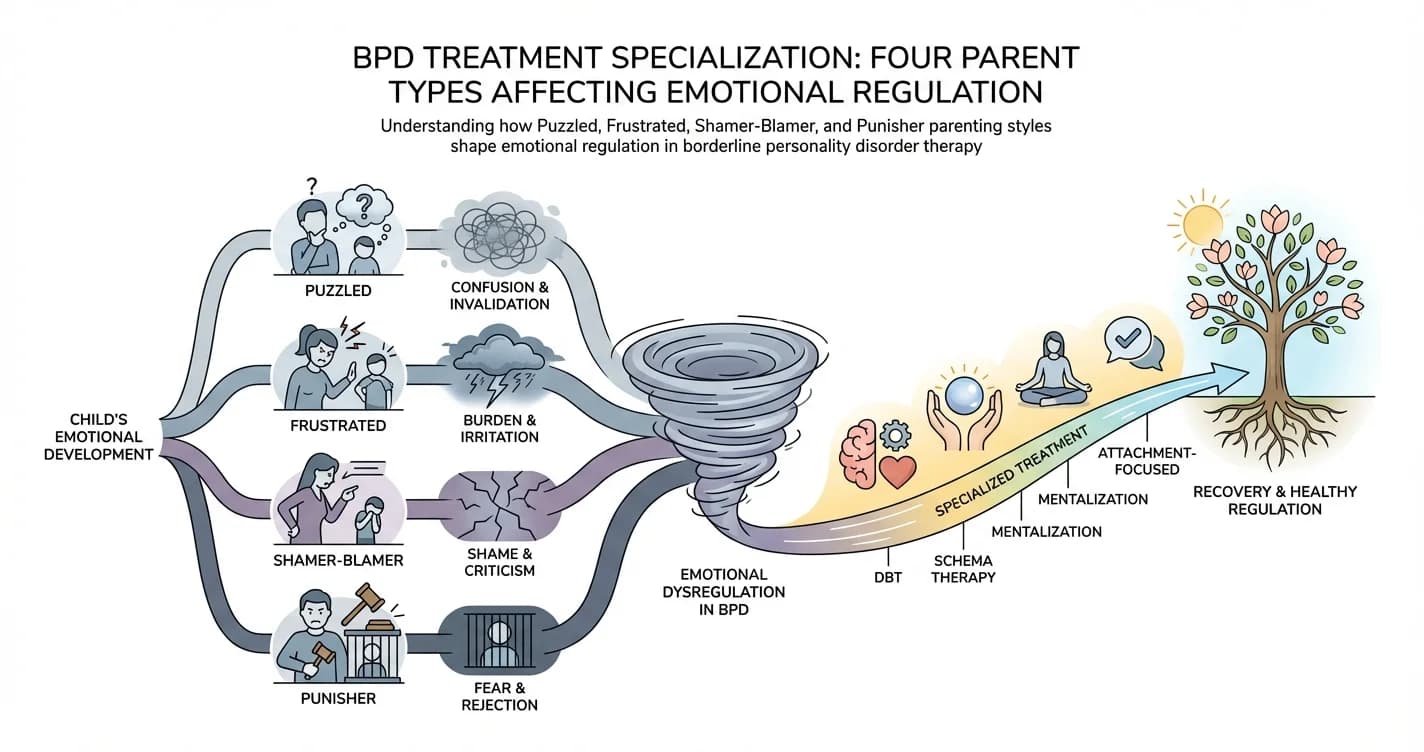
BPD Treatment Specialization: Four Parent Types Affecting Emotional Regulation
For individuals with borderline personality disorder (BPD), emotional regulation difficulties rarely emerge in isolation. Research increasingly suggests that
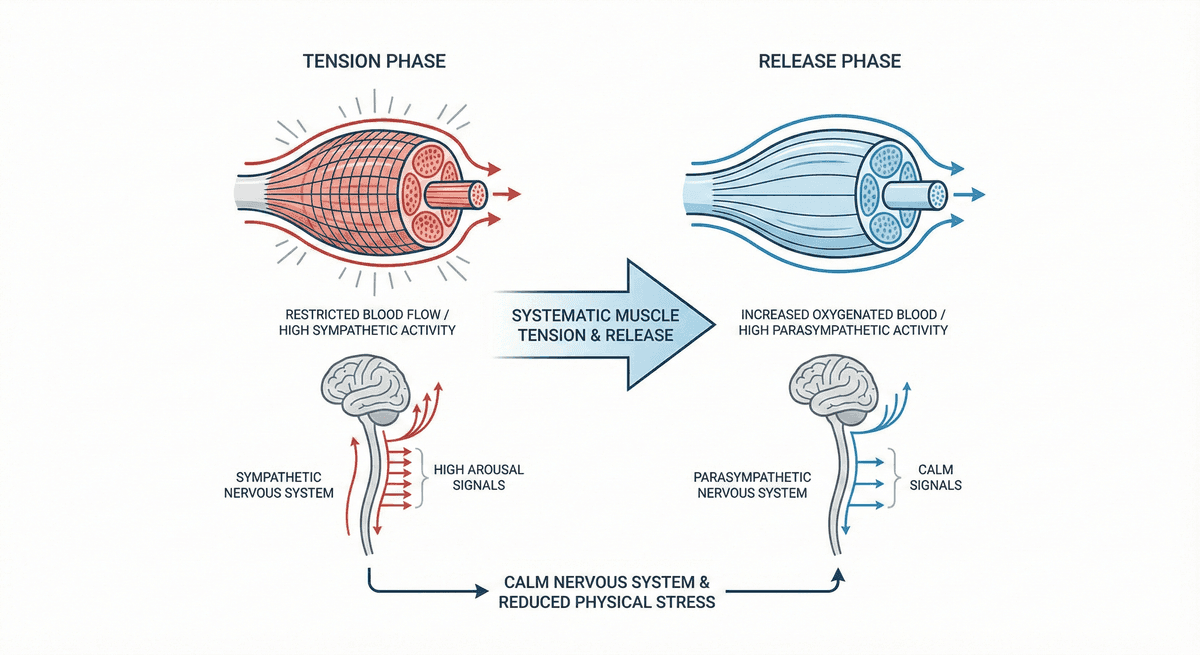
Progressive Muscle Relaxation for Stress Reduction
A systematic muscle group tension and release technique that calms the nervous system and reduces physical stress.
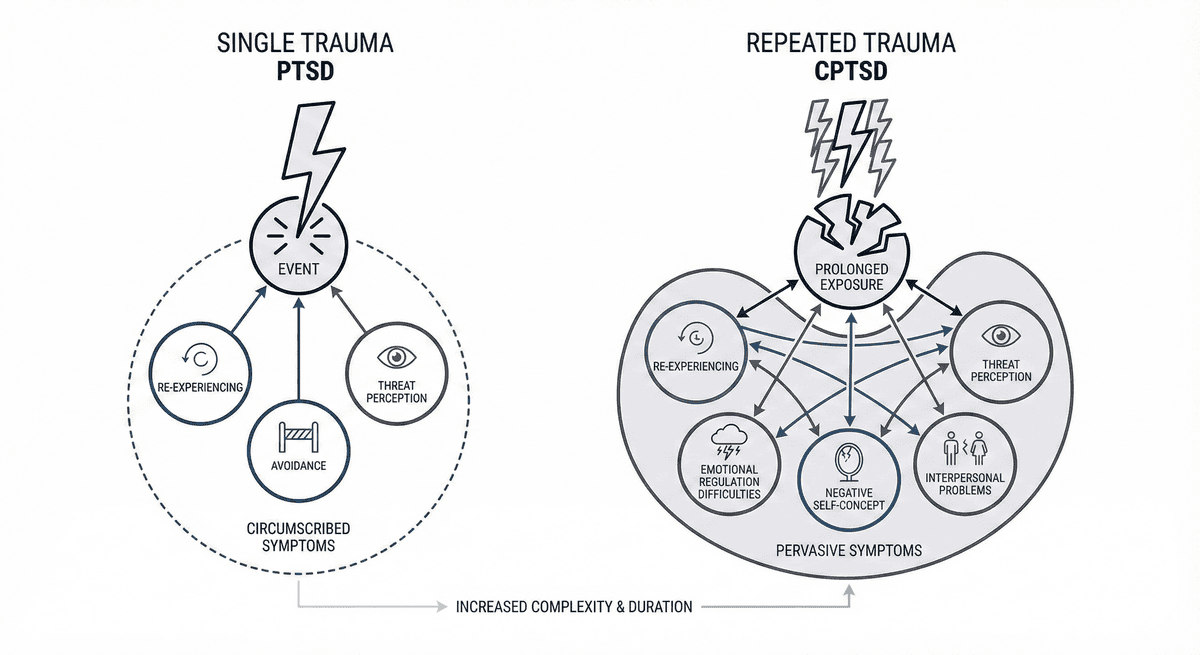
PTSD vs CPTSD: Single Trauma vs Repeated Trauma Symptom Differences
Learn how PTSD from a single traumatic event differs from CPTSD shaped by repeated trauma, including symptom patterns and treatment approaches.
Disclaimer: This article is for informational purposes only and does not constitute medical advice, diagnosis, or treatment. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition. If you are in crisis or think you may have an emergency, call 988 (Suicide & Crisis Lifeline) or go to the nearest emergency room. Outside the US? Find a crisis line in your country.